MedicalResearch.com Interview with:
[caption id="attachment_59713" align="alignleft" width="136"]

Dr. Shan[/caption]
Zhilei Shan, MD, PhD
Postdoctoral fellow on Nutritional Epidemiology
Harvard T.H. Chan School of Public Health
MedicalResearch.com: What is the background for this study?
Response: Unhealthy sleep behaviors and sleep disturbances are associated with higher risk of multiple diseases and mortality. The current profiles of sleep habits and disturbances, particularly the differences between workdays and free days, are unknown in the contemporary US.
MedicalResearch.com: What are the main findings?
Response: In this nationally representative cross-sectional analysis with 9004 adults aged 20 years or older, differences in sleep patterns between workdays and free days were observed. The mean sleep duration was 7.59 hours on workdays and 8.24 hours on free days (difference, 0.65 hour). The mean sleep and wake times were at 11:02 PM and 6:41 AM, respectively, on workdays and 11:25 PM and 7:41 AM, respectively, on free days (differences, 0.23 hour for sleep time and 1.00 hour for wake time). With regard to sleep disturbances, 30.5% of adults experienced 1 hour or more of sleep debt,46.5% experienced 1 hour or more of social jet lag, 29.8% had trouble sleeping, and 27.2% experienced daytime sleepiness.
 Dr. Kubik[/caption]
Martha Kubik, Ph.D., R.N.
Professor, School of Nursing
College of Health and Human Services
George Mason University
Member, U.S. Preventive Services Task Force
MedicalResearch.com: What is the background for this study?
Response: Obstructive sleep apnea is a health condition in which part or all of a person’s airway gets blocked during sleep, causing their breathing to stop and restart many times. Untreated sleep apnea is associated with heart disease, stroke, and diabetes. However, there is currently very limited evidence on screening people who don’t have signs or symptoms like snoring and excessive daytime sleepiness.
Dr. Kubik[/caption]
Martha Kubik, Ph.D., R.N.
Professor, School of Nursing
College of Health and Human Services
George Mason University
Member, U.S. Preventive Services Task Force
MedicalResearch.com: What is the background for this study?
Response: Obstructive sleep apnea is a health condition in which part or all of a person’s airway gets blocked during sleep, causing their breathing to stop and restart many times. Untreated sleep apnea is associated with heart disease, stroke, and diabetes. However, there is currently very limited evidence on screening people who don’t have signs or symptoms like snoring and excessive daytime sleepiness.




 Dr. Dai[/caption]
Dr. Hongying Daisy Dai, PhD
Professor and Associate Dean of Research
The College of Public Health
University of Nebraska Medical Center.
MedicalResearch.com: What is the background for this study?
Response: Tobacco use landscape has been changing in the United States with fewer combustible cigarette smokers and more e-cigarette and other emerging tobacco users. Nicotine concentration level is a key product characteristic of modern e-cigarette products and high-nicotine vaping devices have recently become available. This study seeks to examine whether biomarkers of exposure to tobacco-related toxicants have changed since 2013 among adult nicotine e-cigarette users, non-nicotine e-cigarette users, and cigarette smokers.
Dr. Dai[/caption]
Dr. Hongying Daisy Dai, PhD
Professor and Associate Dean of Research
The College of Public Health
University of Nebraska Medical Center.
MedicalResearch.com: What is the background for this study?
Response: Tobacco use landscape has been changing in the United States with fewer combustible cigarette smokers and more e-cigarette and other emerging tobacco users. Nicotine concentration level is a key product characteristic of modern e-cigarette products and high-nicotine vaping devices have recently become available. This study seeks to examine whether biomarkers of exposure to tobacco-related toxicants have changed since 2013 among adult nicotine e-cigarette users, non-nicotine e-cigarette users, and cigarette smokers.

 Dr. Shan[/caption]
Zhilei Shan, MD, PhD
Postdoctoral fellow on Nutritional Epidemiology
Harvard T.H. Chan School of Public Health
MedicalResearch.com: What is the background for this study?
Response: Unhealthy sleep behaviors and sleep disturbances are associated with higher risk of multiple diseases and mortality. The current profiles of sleep habits and disturbances, particularly the differences between workdays and free days, are unknown in the contemporary US.
MedicalResearch.com: What are the main findings?
Response: In this nationally representative cross-sectional analysis with 9004 adults aged 20 years or older, differences in sleep patterns between workdays and free days were observed. The mean sleep duration was 7.59 hours on workdays and 8.24 hours on free days (difference, 0.65 hour). The mean sleep and wake times were at 11:02 PM and 6:41 AM, respectively, on workdays and 11:25 PM and 7:41 AM, respectively, on free days (differences, 0.23 hour for sleep time and 1.00 hour for wake time). With regard to sleep disturbances, 30.5% of adults experienced 1 hour or more of sleep debt,46.5% experienced 1 hour or more of social jet lag, 29.8% had trouble sleeping, and 27.2% experienced daytime sleepiness.
Dr. Shan[/caption]
Zhilei Shan, MD, PhD
Postdoctoral fellow on Nutritional Epidemiology
Harvard T.H. Chan School of Public Health
MedicalResearch.com: What is the background for this study?
Response: Unhealthy sleep behaviors and sleep disturbances are associated with higher risk of multiple diseases and mortality. The current profiles of sleep habits and disturbances, particularly the differences between workdays and free days, are unknown in the contemporary US.
MedicalResearch.com: What are the main findings?
Response: In this nationally representative cross-sectional analysis with 9004 adults aged 20 years or older, differences in sleep patterns between workdays and free days were observed. The mean sleep duration was 7.59 hours on workdays and 8.24 hours on free days (difference, 0.65 hour). The mean sleep and wake times were at 11:02 PM and 6:41 AM, respectively, on workdays and 11:25 PM and 7:41 AM, respectively, on free days (differences, 0.23 hour for sleep time and 1.00 hour for wake time). With regard to sleep disturbances, 30.5% of adults experienced 1 hour or more of sleep debt,46.5% experienced 1 hour or more of social jet lag, 29.8% had trouble sleeping, and 27.2% experienced daytime sleepiness.


 Dr. Wong[/caption]
Mitchell Wong, MD PhD
Professor of Medicine
Executive Vice Chair for Research Training
Department of Medicine
Executive Co-Director, Specialty Training and Advanced Research (STAR) Program
Director, UCLA CTSI KL2 Program
UCLA Division of General Internal Medicine and Health Services Research Los Angeles, CA 90024
MedicalResearch.com: What is the background for this study?
Response: It is estimated that social factors like poverty, education, and housing have a large impact on health. Yet, there are few interventions that exist to directly address those issues. Schools are a promising solution since society already invests heavily in education and schools are an everyday part of most children’s lives.
Dr. Wong[/caption]
Mitchell Wong, MD PhD
Professor of Medicine
Executive Vice Chair for Research Training
Department of Medicine
Executive Co-Director, Specialty Training and Advanced Research (STAR) Program
Director, UCLA CTSI KL2 Program
UCLA Division of General Internal Medicine and Health Services Research Los Angeles, CA 90024
MedicalResearch.com: What is the background for this study?
Response: It is estimated that social factors like poverty, education, and housing have a large impact on health. Yet, there are few interventions that exist to directly address those issues. Schools are a promising solution since society already invests heavily in education and schools are an everyday part of most children’s lives.
 Dr. Ogedegbe[/caption]
Gbenga Ogedegbe, MD, MPH
Dr. Adolph & Margaret Berger Professor of Population Health
Director, Division of Health & Behavior
Director Center for Healthful Behavior Change
Department of Population Health
NYU Langone Health
NYU School of Medicine
Member of the U.S. Preventive Services Task Force
MedicalResearch.com: What is the background for this study?
Response: Syphilis has become more common over the past 20 years, after reaching a record low in 2000. The Task Force found that screening people who are at increased risk for syphilis can identify the infection early so it can be treated before problems develop. For that reason, the Task Force recommends screening people who are at increased risk for syphilis infection.
Dr. Ogedegbe[/caption]
Gbenga Ogedegbe, MD, MPH
Dr. Adolph & Margaret Berger Professor of Population Health
Director, Division of Health & Behavior
Director Center for Healthful Behavior Change
Department of Population Health
NYU Langone Health
NYU School of Medicine
Member of the U.S. Preventive Services Task Force
MedicalResearch.com: What is the background for this study?
Response: Syphilis has become more common over the past 20 years, after reaching a record low in 2000. The Task Force found that screening people who are at increased risk for syphilis can identify the infection early so it can be treated before problems develop. For that reason, the Task Force recommends screening people who are at increased risk for syphilis infection.

 Dr. Orkaby[/caption]
Ariela Orkaby, MD, MPH
Geriatrics & Preventive Cardiology
Associate Epidemiologist
Division of Aging, Brigham and Women's Hospital
Assistant Professor of Medicine, Harvard Medical School
MedicalResearch.com: What is the background for this study?
Response: As the population is living longer, there is increased risk of frailty and vulnerability. Frailty is defined as reduced physiological reserve and decreased ability to cope with even an acute stress. Up to half of adults over the age of 85 are living with frailty and preventative measures are greatly needed. We tested the effect of vitamin D and marine omega-3 fatty acid supplementation on the risk of developing frailty in healthy older adults in the US enrolled in the VITamin D and OmegA-3 TriaL (VITAL) trial.
Dr. Orkaby[/caption]
Ariela Orkaby, MD, MPH
Geriatrics & Preventive Cardiology
Associate Epidemiologist
Division of Aging, Brigham and Women's Hospital
Assistant Professor of Medicine, Harvard Medical School
MedicalResearch.com: What is the background for this study?
Response: As the population is living longer, there is increased risk of frailty and vulnerability. Frailty is defined as reduced physiological reserve and decreased ability to cope with even an acute stress. Up to half of adults over the age of 85 are living with frailty and preventative measures are greatly needed. We tested the effect of vitamin D and marine omega-3 fatty acid supplementation on the risk of developing frailty in healthy older adults in the US enrolled in the VITamin D and OmegA-3 TriaL (VITAL) trial.

 Dr. Orkaby[/caption]
Ariela Orkaby, MD, MPH
Geriatrics & Preventive Cardiology
Associate Epidemiologist
Division of Aging, Brigham and Women's Hospital
Assistant Professor of Medicine, Harvard Medical School
MedicalResearch.com: What is the background for this study?
Response: As the population is living longer, there is increased risk of frailty and vulnerability. Frailty is defined as reduced physiological reserve and decreased ability to cope with even an acute stress. Up to half of adults over the age of 85 are living with frailty and preventative measures are greatly needed. We tested the effect of vitamin D and marine omega-3 fatty acid supplementation on the risk of developing frailty in healthy older adults in the US enrolled in the VITamin D and OmegA-3 TriaL (VITAL) trial.
Dr. Orkaby[/caption]
Ariela Orkaby, MD, MPH
Geriatrics & Preventive Cardiology
Associate Epidemiologist
Division of Aging, Brigham and Women's Hospital
Assistant Professor of Medicine, Harvard Medical School
MedicalResearch.com: What is the background for this study?
Response: As the population is living longer, there is increased risk of frailty and vulnerability. Frailty is defined as reduced physiological reserve and decreased ability to cope with even an acute stress. Up to half of adults over the age of 85 are living with frailty and preventative measures are greatly needed. We tested the effect of vitamin D and marine omega-3 fatty acid supplementation on the risk of developing frailty in healthy older adults in the US enrolled in the VITamin D and OmegA-3 TriaL (VITAL) trial.

 Dr. Jing Li[/caption]
Jing Li, PhD
Assistant Professor of Health Economics
The Comparative Health Outcomes, Policy and Economics (CHOICE) Institute
University of Washington School of Pharmacy
MedicalResearch.com: What is the background for this study?
Response: Dementia and other cognitive impairment are highly prevalent among older adults in the U.S. and globally, and have been linked to deficiencies in decision-making, especially financial decision-making. However, little is known about the extent to which older adults with cognitive impairment manage their own finances and the characteristics of the assets they manage.
Dr. Jing Li[/caption]
Jing Li, PhD
Assistant Professor of Health Economics
The Comparative Health Outcomes, Policy and Economics (CHOICE) Institute
University of Washington School of Pharmacy
MedicalResearch.com: What is the background for this study?
Response: Dementia and other cognitive impairment are highly prevalent among older adults in the U.S. and globally, and have been linked to deficiencies in decision-making, especially financial decision-making. However, little is known about the extent to which older adults with cognitive impairment manage their own finances and the characteristics of the assets they manage.











 Joanna Jiang, PhD
Agency for Healthcare Research and Quality
Rockville, Maryland
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Over the last decade we have seen two trends occurring to rural hospitals – closures and mergers. A hospital in financial distress could likely face closure. But if the hospital affiliates with a multihospital system, it may have access to resources from the system that help shelter the hospital from closure.
That is exactly what we found in this study. System affiliation was associated with a lower risk of closure for financially distressed hospitals. However, among hospitals that were financially stable, system affiliation was associated with a higher risk of closure. This is somewhat puzzling and needs further study to better understand the reason for closure.
Joanna Jiang, PhD
Agency for Healthcare Research and Quality
Rockville, Maryland
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Over the last decade we have seen two trends occurring to rural hospitals – closures and mergers. A hospital in financial distress could likely face closure. But if the hospital affiliates with a multihospital system, it may have access to resources from the system that help shelter the hospital from closure.
That is exactly what we found in this study. System affiliation was associated with a lower risk of closure for financially distressed hospitals. However, among hospitals that were financially stable, system affiliation was associated with a higher risk of closure. This is somewhat puzzling and needs further study to better understand the reason for closure.

 Dr. Midya[/caption]
Dania Valvi, MD MPH PhD
Assistant Professor
Department of Environmental Medicine and Public Health
Co-Director, MS in Epidemiology
Icahn School of Medicine at Mount Sinai
Email: dania.valvi@mssm.edu
MedicalResearch.com: What is the background for this study?
Response: Non-alcoholic fatty liver disease (NAFLD) is the most common liver disease in children in the U.S., Europe and other world regions, currently affecting 1 in every 10 children, and 1 in every 3 children with obesity in the U.S. The rate of pediatric NAFLD has more than doubled in recent decades following the epidemic rates also noted for childhood obesity. There is increasing interest in the role that environmental chemical exposures may play in NAFLD etiology, since several animal studies have shown that prenatal exposures to endocrine-disrupting chemicals (EDCs) cause liver injury and damage; but, until now, the potential effects of prenatal EDC mixture exposures in pediatric NAFLD had not been studied.
Dr. Midya[/caption]
Dania Valvi, MD MPH PhD
Assistant Professor
Department of Environmental Medicine and Public Health
Co-Director, MS in Epidemiology
Icahn School of Medicine at Mount Sinai
Email: dania.valvi@mssm.edu
MedicalResearch.com: What is the background for this study?
Response: Non-alcoholic fatty liver disease (NAFLD) is the most common liver disease in children in the U.S., Europe and other world regions, currently affecting 1 in every 10 children, and 1 in every 3 children with obesity in the U.S. The rate of pediatric NAFLD has more than doubled in recent decades following the epidemic rates also noted for childhood obesity. There is increasing interest in the role that environmental chemical exposures may play in NAFLD etiology, since several animal studies have shown that prenatal exposures to endocrine-disrupting chemicals (EDCs) cause liver injury and damage; but, until now, the potential effects of prenatal EDC mixture exposures in pediatric NAFLD had not been studied.
 SooYoung VanDeMar[/caption]
SooYoung VanDeMark, MBS
Geisinger Commonwealth School of Medicine
Scranton, Pennsylvania
MedicalResearch.com: What is the background for this study?
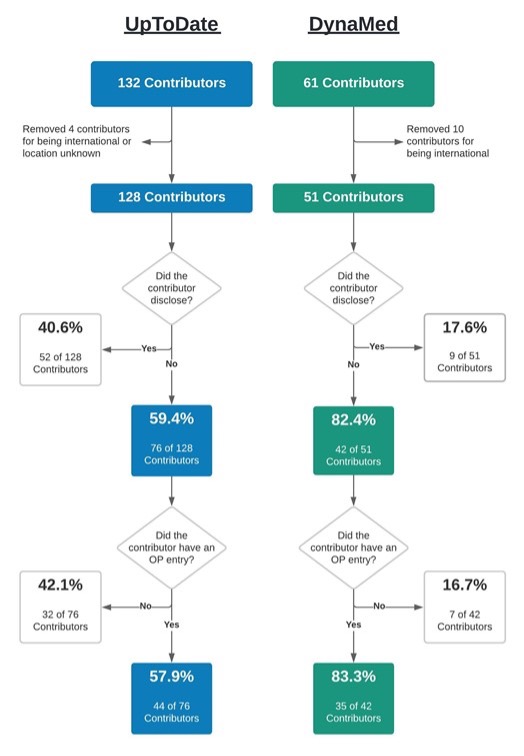
Response: Health care providers utilize subscription-based, point-of-care databases such as DynaMed and UpToDate to provide clinical care guidance and remain current on the latest evidence-based findings. Both of these websites maintain this content through a cadre of physician contributors who write and edit articles for these sites. These physician contributors are required to self-report any conflicts of interest (COI) as outlined by the respective policies on each website. However, prior COI research into similarly self-regulated areas, such as medical and pharmacology textbooks, and clinical practice guidelines, has found both appreciable potential COI and inconsistencies between self-reported and industry mandated disclosures (1-3).
This study (4) explored the accuracy of physician contributors to DynaMed and UpToDate by comparing their self-reported disclosure status with the financial remunerations they received from the healthcare industry (e.g., pharmaceutical companies) as reported to the U.S. Centers for Medicare and Medicaid Services’ Open Payments database. Physician contributors who reported “nothing to disclose” on their respective article topic but had an entry on Open Payments for having received money from industry, were classified as discordant and, thus, as having the potential for a COI. Additionally, total remuneration, gender, and payment category were investigated more in depth for each database.
SooYoung VanDeMar[/caption]
SooYoung VanDeMark, MBS
Geisinger Commonwealth School of Medicine
Scranton, Pennsylvania
MedicalResearch.com: What is the background for this study?
Response: Health care providers utilize subscription-based, point-of-care databases such as DynaMed and UpToDate to provide clinical care guidance and remain current on the latest evidence-based findings. Both of these websites maintain this content through a cadre of physician contributors who write and edit articles for these sites. These physician contributors are required to self-report any conflicts of interest (COI) as outlined by the respective policies on each website. However, prior COI research into similarly self-regulated areas, such as medical and pharmacology textbooks, and clinical practice guidelines, has found both appreciable potential COI and inconsistencies between self-reported and industry mandated disclosures (1-3).
This study (4) explored the accuracy of physician contributors to DynaMed and UpToDate by comparing their self-reported disclosure status with the financial remunerations they received from the healthcare industry (e.g., pharmaceutical companies) as reported to the U.S. Centers for Medicare and Medicaid Services’ Open Payments database. Physician contributors who reported “nothing to disclose” on their respective article topic but had an entry on Open Payments for having received money from industry, were classified as discordant and, thus, as having the potential for a COI. Additionally, total remuneration, gender, and payment category were investigated more in depth for each database.

 Dr. Soriano[/caption]
Victoria Soriano PhD
Research Assistant/Officer, Population Allergy
University of Melbourne
MedicalResearch.com: What is the background for this study?
Response: Peanut allergy is one of the most common childhood food allergies, and children rarely grow out of it. The only proven way to prevent peanut allergy is to give infants age-appropriate peanut products in the first year of life.
We previously showed there was a dramatic increase in peanut introduction from 2007-11 to 2018-19, following changes to infant feeding guidelines. We wanted to know if earlier peanut introduction would reduce peanut allergy in the general population (in Melbourne, Australia).
Dr. Soriano[/caption]
Victoria Soriano PhD
Research Assistant/Officer, Population Allergy
University of Melbourne
MedicalResearch.com: What is the background for this study?
Response: Peanut allergy is one of the most common childhood food allergies, and children rarely grow out of it. The only proven way to prevent peanut allergy is to give infants age-appropriate peanut products in the first year of life.
We previously showed there was a dramatic increase in peanut introduction from 2007-11 to 2018-19, following changes to infant feeding guidelines. We wanted to know if earlier peanut introduction would reduce peanut allergy in the general population (in Melbourne, Australia).
 Dr. Barry[/caption]
Michael J. Barry, M.D
Director of the Informed Medical Decisions Program
Health Decision Sciences Center
Massachusetts General Hospital.
Professor of medicine at Harvard Medical School
Dr. Barry was appointed as Vice Chair of USPSTF in March 2021.
He previously served as a member from January 2017 through December 2020.
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The Task Force looked at the use of vitamin and mineral supplementation specifically for the prevention of heart disease, stroke, and cancer. We found that there is not enough evidence to recommend for or against taking multivitamin supplements, nor the use of single or paired nutrient supplements, to prevent these conditions.
However, we do know that you should not take vitamin E or beta-carotene for this purpose.
Dr. Barry[/caption]
Michael J. Barry, M.D
Director of the Informed Medical Decisions Program
Health Decision Sciences Center
Massachusetts General Hospital.
Professor of medicine at Harvard Medical School
Dr. Barry was appointed as Vice Chair of USPSTF in March 2021.
He previously served as a member from January 2017 through December 2020.
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The Task Force looked at the use of vitamin and mineral supplementation specifically for the prevention of heart disease, stroke, and cancer. We found that there is not enough evidence to recommend for or against taking multivitamin supplements, nor the use of single or paired nutrient supplements, to prevent these conditions.
However, we do know that you should not take vitamin E or beta-carotene for this purpose.
