Author Interviews, CDC, Emergency Care, JAMA / 06.10.2021
Number of Emergency Room Visits for Medication Harms Increases with Age
MedicalResearch.com Interview with:
[caption id="attachment_58203" align="alignleft" width="200"] Dr. Budnitz[/caption]
Dr. Daniel S. Budnitz MD MPH CAPT, USPHS
Division of Healthcare Quality Promotion
Director, Centers for Disease Control and Prevention’s Medication Safety Program
Atlanta, Georgia
MedicalResearch.com: What is the background for this study?
Response: Medications are generally safe when used as prescribed or as directed on the label, but there can be risks in taking any medication. Adverse drug events are harms resulting from the use of medication.
The risk of adverse drug events is highest among older adults and very young children. Older adults have higher risks because they typically take more medications and are more likely to have underlying medical conditions. Very young children have higher risks because they often find and ingest medications meant for others.
Previous studies of medication safety have focused on harm from medications when taken for therapeutic reasons. Separate studies have focused on harm from specific types of non-therapeutic use (taking medications for recreational use or self-harm). This study examined the number of emergency department (ED) visits that resulted when people who took medications for any reason – as directed by a clinician or for other reasons, including recreational use or intentional self-harm.
Dr. Budnitz[/caption]
Dr. Daniel S. Budnitz MD MPH CAPT, USPHS
Division of Healthcare Quality Promotion
Director, Centers for Disease Control and Prevention’s Medication Safety Program
Atlanta, Georgia
MedicalResearch.com: What is the background for this study?
Response: Medications are generally safe when used as prescribed or as directed on the label, but there can be risks in taking any medication. Adverse drug events are harms resulting from the use of medication.
The risk of adverse drug events is highest among older adults and very young children. Older adults have higher risks because they typically take more medications and are more likely to have underlying medical conditions. Very young children have higher risks because they often find and ingest medications meant for others.
Previous studies of medication safety have focused on harm from medications when taken for therapeutic reasons. Separate studies have focused on harm from specific types of non-therapeutic use (taking medications for recreational use or self-harm). This study examined the number of emergency department (ED) visits that resulted when people who took medications for any reason – as directed by a clinician or for other reasons, including recreational use or intentional self-harm.
 Dr. Budnitz[/caption]
Dr. Daniel S. Budnitz MD MPH CAPT, USPHS
Division of Healthcare Quality Promotion
Director, Centers for Disease Control and Prevention’s Medication Safety Program
Atlanta, Georgia
MedicalResearch.com: What is the background for this study?
Response: Medications are generally safe when used as prescribed or as directed on the label, but there can be risks in taking any medication. Adverse drug events are harms resulting from the use of medication.
The risk of adverse drug events is highest among older adults and very young children. Older adults have higher risks because they typically take more medications and are more likely to have underlying medical conditions. Very young children have higher risks because they often find and ingest medications meant for others.
Previous studies of medication safety have focused on harm from medications when taken for therapeutic reasons. Separate studies have focused on harm from specific types of non-therapeutic use (taking medications for recreational use or self-harm). This study examined the number of emergency department (ED) visits that resulted when people who took medications for any reason – as directed by a clinician or for other reasons, including recreational use or intentional self-harm.
Dr. Budnitz[/caption]
Dr. Daniel S. Budnitz MD MPH CAPT, USPHS
Division of Healthcare Quality Promotion
Director, Centers for Disease Control and Prevention’s Medication Safety Program
Atlanta, Georgia
MedicalResearch.com: What is the background for this study?
Response: Medications are generally safe when used as prescribed or as directed on the label, but there can be risks in taking any medication. Adverse drug events are harms resulting from the use of medication.
The risk of adverse drug events is highest among older adults and very young children. Older adults have higher risks because they typically take more medications and are more likely to have underlying medical conditions. Very young children have higher risks because they often find and ingest medications meant for others.
Previous studies of medication safety have focused on harm from medications when taken for therapeutic reasons. Separate studies have focused on harm from specific types of non-therapeutic use (taking medications for recreational use or self-harm). This study examined the number of emergency department (ED) visits that resulted when people who took medications for any reason – as directed by a clinician or for other reasons, including recreational use or intentional self-harm.



 Dr. Singer[/caption]
Daniel E. Singer, MD
Professor of Medicine, Harvard Medical School
Professor in the Department of Epidemiology
Harvard T.H. Chan School of Public Health
Division of General Internal Medicine
Massachusetts General Hospital
Boston, MA, 02114
MedicalResearch.com: What is the background for this study?
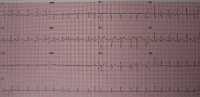
Response: Atrial fibrillation (AF) raises the risk of ischemic stroke 4-5-fold and this risk is largely reversible by oral anticoagulants (OAC). These facts are part of the core knowledge of internal medicine and the basis of multiple guidelines. They are based on studies of patients with persistent or predominantly “heavy burden” paroxysmal AF completed in the 1990s.
More recent studies using cardiac implantable devices (CIEDs: implantable defibrillators, pacemakers, etc) which have the capacity to monitor heart rhythm continuously have found that many older patients have brief, often undiagnosed, episodes of AF. Several of these studies have found that strokes occur during periods of sinus rhythm temporally distant from a preceding episode of AF. This has led to a widespread suspicion that AF is not a direct causal risk factor but a risk “marker” indicating the presence of other truly causal features like a diseased left atrium (atrial myopathy). If the risk marker hypothesis is correct, then long-term anticoagulation is needed even for brief and rare episodes of AF (assuming the patient’ s CHA2DS2-VASc score is high enough). The key problem with prior prospective studies using CIEDs was that only a small number of strokes were observed leading to inadequate statistical power.
Our study addressed this power problem by linking the very large Optum electronic health record database which could identify ischemic strokes with the Medtronic CareLink database of long-term, continuous heart rhythm records of patients with CIEDs. We ended up studying 891 individuals who had an ischemic stroke and had 120 days of continuous heart monitoring prior to the stroke.
Dr. Singer[/caption]
Daniel E. Singer, MD
Professor of Medicine, Harvard Medical School
Professor in the Department of Epidemiology
Harvard T.H. Chan School of Public Health
Division of General Internal Medicine
Massachusetts General Hospital
Boston, MA, 02114
MedicalResearch.com: What is the background for this study?
Response: Atrial fibrillation (AF) raises the risk of ischemic stroke 4-5-fold and this risk is largely reversible by oral anticoagulants (OAC). These facts are part of the core knowledge of internal medicine and the basis of multiple guidelines. They are based on studies of patients with persistent or predominantly “heavy burden” paroxysmal AF completed in the 1990s.
More recent studies using cardiac implantable devices (CIEDs: implantable defibrillators, pacemakers, etc) which have the capacity to monitor heart rhythm continuously have found that many older patients have brief, often undiagnosed, episodes of AF. Several of these studies have found that strokes occur during periods of sinus rhythm temporally distant from a preceding episode of AF. This has led to a widespread suspicion that AF is not a direct causal risk factor but a risk “marker” indicating the presence of other truly causal features like a diseased left atrium (atrial myopathy). If the risk marker hypothesis is correct, then long-term anticoagulation is needed even for brief and rare episodes of AF (assuming the patient’ s CHA2DS2-VASc score is high enough). The key problem with prior prospective studies using CIEDs was that only a small number of strokes were observed leading to inadequate statistical power.
Our study addressed this power problem by linking the very large Optum electronic health record database which could identify ischemic strokes with the Medtronic CareLink database of long-term, continuous heart rhythm records of patients with CIEDs. We ended up studying 891 individuals who had an ischemic stroke and had 120 days of continuous heart monitoring prior to the stroke.





 Helen Trottier Ph.D
Assistant Professor, Department of Social and Preventive Medicine,
Researcher, CHU Sainte-Justine Research Center
Université de Montréal
Montréal, Québec, Canada
MedicalResearch.com: What is the background for this study?
Response: We know that HPV infection can have serious consequences such as the development of cancerous lesions in the cervix. HPV infection is also very prevalent in young women of childbearing age but the possible consequences of HPV in pregnancy have been poorly studied. Some population registers around the world have shown a reduction in the risk of preterm birth with HPV mass vaccination, but we must be careful with this kind of ecological correlation.
We have set up a large cohort study in pregnant women to study the association between HPV in pregnancy and preterm birth by targeting certain HPV genotypes and the duration of the infection.
Helen Trottier Ph.D
Assistant Professor, Department of Social and Preventive Medicine,
Researcher, CHU Sainte-Justine Research Center
Université de Montréal
Montréal, Québec, Canada
MedicalResearch.com: What is the background for this study?
Response: We know that HPV infection can have serious consequences such as the development of cancerous lesions in the cervix. HPV infection is also very prevalent in young women of childbearing age but the possible consequences of HPV in pregnancy have been poorly studied. Some population registers around the world have shown a reduction in the risk of preterm birth with HPV mass vaccination, but we must be careful with this kind of ecological correlation.
We have set up a large cohort study in pregnant women to study the association between HPV in pregnancy and preterm birth by targeting certain HPV genotypes and the duration of the infection.


 Dr. Cole[/caption]
Megan B. Cole, PhD, MPH
Assistant Professor | Dept. of Health Law, Policy, & Management
Co-Director | BU Medicaid Policy Lab
Boston University School of Public Health
Boston, MA 02118
MedicalResearch.com: What is the background for this study?
Response: Under the Affordable Care Act, states were given the option to expand Medicaid eligibility to nonelderly adults with incomes up to 138% of the federal poverty level, where in January 2014, 25 states plus Washington, DC expanded eligibility, with 13 additional states expanding thereafter. State Medicaid expansion decisions were particularly consequential for federally qualified health centers (FQHCs), which serve nearly 30 million low-income, disproportionately uninsured patients across the US.
We know from earlier work that in the shorter-term, Medicaid expansion was associated with improvements in quality of care process measures and FQHC service capacity. However, we conducted the first known nationally representative study to examine how Medicaid expansion impacted key chronic disease outcome measures at FQHCs over the longer-term by looking at changes five years after implementation, including changes by race/ethnicity.
Dr. Cole[/caption]
Megan B. Cole, PhD, MPH
Assistant Professor | Dept. of Health Law, Policy, & Management
Co-Director | BU Medicaid Policy Lab
Boston University School of Public Health
Boston, MA 02118
MedicalResearch.com: What is the background for this study?
Response: Under the Affordable Care Act, states were given the option to expand Medicaid eligibility to nonelderly adults with incomes up to 138% of the federal poverty level, where in January 2014, 25 states plus Washington, DC expanded eligibility, with 13 additional states expanding thereafter. State Medicaid expansion decisions were particularly consequential for federally qualified health centers (FQHCs), which serve nearly 30 million low-income, disproportionately uninsured patients across the US.
We know from earlier work that in the shorter-term, Medicaid expansion was associated with improvements in quality of care process measures and FQHC service capacity. However, we conducted the first known nationally representative study to examine how Medicaid expansion impacted key chronic disease outcome measures at FQHCs over the longer-term by looking at changes five years after implementation, including changes by race/ethnicity.




 Amanda Paluch, PhD
Assistant Professor
University of Massachusetts Amherst
Department of Kinesiology
Institute for Applied Life Sciences
Life Science Laboratories
Amherst, MA 01003
MedicalResearch.com: What is the background for this study?
Response: We wanted to understand the association of total steps per day with premature mortality among middle-aged, Black and White women and men. This study included 2110 adults; age 38-50 years old at the start of this study. These adults wore a step counting device for one week and then followed for death from any cause over the next 10 years.
Amanda Paluch, PhD
Assistant Professor
University of Massachusetts Amherst
Department of Kinesiology
Institute for Applied Life Sciences
Life Science Laboratories
Amherst, MA 01003
MedicalResearch.com: What is the background for this study?
Response: We wanted to understand the association of total steps per day with premature mortality among middle-aged, Black and White women and men. This study included 2110 adults; age 38-50 years old at the start of this study. These adults wore a step counting device for one week and then followed for death from any cause over the next 10 years.







 Dr. Albrecht[/caption]
Joerg Albrecht, MD, PhD
Dermatologist, Internist, Clinical Pharmacologist
Division of Dermatology, Department of Medicine
Attending Dermatologist, Chair Division of Dermatology
Chair system-wide Pharmacy & Therapeutics Committee
Cook County Health
Chicago, IL 60612
MedicalResearch.com: What is the background for this study?
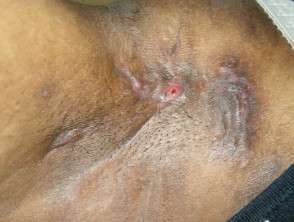
Response: The study was stimulated by data that suggested that an unusually large proportion of inpatient with Hidradenitis suppurativa (HS) were African American. HS is an underdiagnosed disease and the total numbers of inpatients with HS in the year we looked at initially seemed small. So we wanted to test whether this finding held up when the period of observation was extended. Point estimates can be unreliable and we had followed another finding in the data that did not hold up when we looked at other years, so we felt one year was not enough to confirm a trend
Dr. Albrecht[/caption]
Joerg Albrecht, MD, PhD
Dermatologist, Internist, Clinical Pharmacologist
Division of Dermatology, Department of Medicine
Attending Dermatologist, Chair Division of Dermatology
Chair system-wide Pharmacy & Therapeutics Committee
Cook County Health
Chicago, IL 60612
MedicalResearch.com: What is the background for this study?
Response: The study was stimulated by data that suggested that an unusually large proportion of inpatient with Hidradenitis suppurativa (HS) were African American. HS is an underdiagnosed disease and the total numbers of inpatients with HS in the year we looked at initially seemed small. So we wanted to test whether this finding held up when the period of observation was extended. Point estimates can be unreliable and we had followed another finding in the data that did not hold up when we looked at other years, so we felt one year was not enough to confirm a trend


 Dr. Ribeiro[/caption]
Fernando Ribeiro PhD
School of Health Sciences
Institute of Biomedicine - iBiMED
University of Aveiro
Aveiro, Portugal
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Resistant hypertension is a puzzling problem without a clear solution. The available treatment options to lower blood pressure, namely medication and renal denervation, have had limited success, making nonpharmacological strategies good candidates to optimize the treatment of this condition.
Exercise training is consistently recommended as adjuvant therapy for patients with hypertension, yet, it is with a great delay that the efficacy of exercise training is being tested in patients with resistant hypertension.
Having that in mind, the EnRicH trial was designed to address whether the benefits of an exercise intervention with proven results in hypertensive individuals are extended to patients with resistant hypertension, a clinical population with low responsiveness to drug therapy. Exercise training was safe and associated with a significant and clinically relevant reduction in 24-hour, daytime ambulatory, and office blood pressure compared with control (usual care).
Dr. Ribeiro[/caption]
Fernando Ribeiro PhD
School of Health Sciences
Institute of Biomedicine - iBiMED
University of Aveiro
Aveiro, Portugal
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Resistant hypertension is a puzzling problem without a clear solution. The available treatment options to lower blood pressure, namely medication and renal denervation, have had limited success, making nonpharmacological strategies good candidates to optimize the treatment of this condition.
Exercise training is consistently recommended as adjuvant therapy for patients with hypertension, yet, it is with a great delay that the efficacy of exercise training is being tested in patients with resistant hypertension.
Having that in mind, the EnRicH trial was designed to address whether the benefits of an exercise intervention with proven results in hypertensive individuals are extended to patients with resistant hypertension, a clinical population with low responsiveness to drug therapy. Exercise training was safe and associated with a significant and clinically relevant reduction in 24-hour, daytime ambulatory, and office blood pressure compared with control (usual care).
 Dr. Pierce[/caption]
John Pierce, PhD
Professor Emeritus
Department of Family Medicine and Public Health
Moores Cancer Center Director for Population Sciences
Co-leader of the Cancer Prevention program
UC San Diego
MedicalResearch.com: What is the background for this study? What are the main findings?
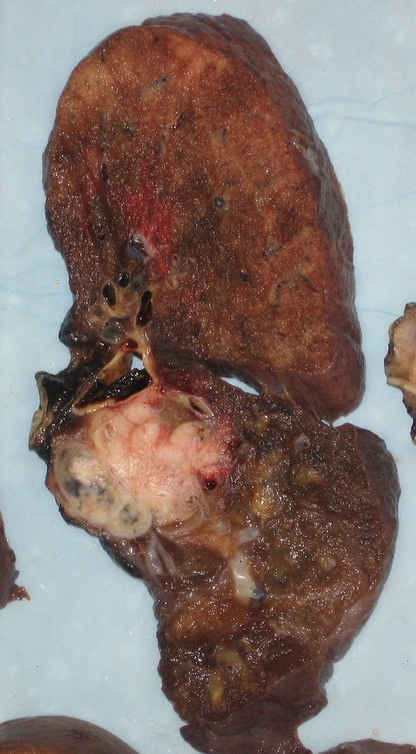
Response: Graphic Warning Labels are to be implemented in the US in July 2022, depending on litigation. This will be about 10 years after they were first proposed. Meanwhile, 120 other countries have implemented them already.
The FDA states that their purpose for the warnings is to provide a constant reminder to smokers about the health consequences of smoking, not to force them to quit.
In our study, 3 months of having cigarettes repackaged into graphic warning packs was associated with smokers thinking more about quitting and not getting as much pleasure out of their cigarettes. However, thinking about quitting is only the first step to conquering a nicotine addiction.
Dr. Pierce[/caption]
John Pierce, PhD
Professor Emeritus
Department of Family Medicine and Public Health
Moores Cancer Center Director for Population Sciences
Co-leader of the Cancer Prevention program
UC San Diego
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Graphic Warning Labels are to be implemented in the US in July 2022, depending on litigation. This will be about 10 years after they were first proposed. Meanwhile, 120 other countries have implemented them already.
The FDA states that their purpose for the warnings is to provide a constant reminder to smokers about the health consequences of smoking, not to force them to quit.
In our study, 3 months of having cigarettes repackaged into graphic warning packs was associated with smokers thinking more about quitting and not getting as much pleasure out of their cigarettes. However, thinking about quitting is only the first step to conquering a nicotine addiction.

 Dr. Blumenthal[/caption]
Kimberly G. Blumenthal, MD, MSc
Massachusetts General Hospital
The Mongan Institute
Boston, MA 02114
[caption id="attachment_57828" align="alignleft" width="100"]
Dr. Blumenthal[/caption]
Kimberly G. Blumenthal, MD, MSc
Massachusetts General Hospital
The Mongan Institute
Boston, MA 02114
[caption id="attachment_57828" align="alignleft" width="100"] Dr. Krantz[/caption]
Matthew S. Krantz, MD
Division of Allergy, Pulmonary and Critical Care Medicine
Department of Medicine,
Vanderbilt University Medical Center,
Nashville, Tennessee
MedicalResearch.com: What is the background for this study?
Response: During the initial COVID-19 vaccine campaign with healthcare workers in December 2020, there was an unexpected higher than anticipated rate of immediate allergic reactions after Pfizer and Moderna mRNA vaccines. This prompted both patient and provider concerns, particularly in those with underlying allergic histories, on the associated risks for immediate allergic reactions with the mRNA vaccines.
Because of the significantly improved effectiveness of two doses of an mRNA vaccine compared to one dose, it was important to determine if those who experienced immediate allergic reaction symptoms after their first dose could go on to tolerate a second dose safely.
Dr. Krantz[/caption]
Matthew S. Krantz, MD
Division of Allergy, Pulmonary and Critical Care Medicine
Department of Medicine,
Vanderbilt University Medical Center,
Nashville, Tennessee
MedicalResearch.com: What is the background for this study?
Response: During the initial COVID-19 vaccine campaign with healthcare workers in December 2020, there was an unexpected higher than anticipated rate of immediate allergic reactions after Pfizer and Moderna mRNA vaccines. This prompted both patient and provider concerns, particularly in those with underlying allergic histories, on the associated risks for immediate allergic reactions with the mRNA vaccines.
Because of the significantly improved effectiveness of two doses of an mRNA vaccine compared to one dose, it was important to determine if those who experienced immediate allergic reaction symptoms after their first dose could go on to tolerate a second dose safely.