Author Interviews, JAMA, Mental Health Research / 28.02.2020
Antipsychotic Medication Linked to Brain Cortex Thinning in People in Remission from Psychotic Depression
MedicalResearch.com Interview with:
[caption id="attachment_53338" align="alignleft" width="190"] Dr. Voineskos[/caption]
Dr. Aristotle Voineskos MD, PhD, FRCPC
Director, Slaight Family Centre for Youth in Transition and Head,
Kimel Family Translational Imaging-Genetics Laboratory
Campbell Family Mental Health Research Institute
CAMH
University of Toronto
MedicalResearch.com: What is the background for this study?
Response: Uncontrolled studies in humans have shown conflicting results regarding effects of antipsychotic medications on brain structure. Recent studies in animals (e.g. rats and non-human primates) show that these medications may be associated with brain volume loss. To date, our knowledge of the effects of antipsychotic medications on brain structure in humans have been limited by the lack of a double-blind, randomized, placebo-controlled trial with brain imaging. Ours is the first such study. It is considered unethical to do such a study in people with schizophrenia, because of the life-saving benefits of these medications in this illness. However, in people with depression also experiencing psychosis, it was possible to do such a study once people experienced remission from their illness.
Dr. Voineskos[/caption]
Dr. Aristotle Voineskos MD, PhD, FRCPC
Director, Slaight Family Centre for Youth in Transition and Head,
Kimel Family Translational Imaging-Genetics Laboratory
Campbell Family Mental Health Research Institute
CAMH
University of Toronto
MedicalResearch.com: What is the background for this study?
Response: Uncontrolled studies in humans have shown conflicting results regarding effects of antipsychotic medications on brain structure. Recent studies in animals (e.g. rats and non-human primates) show that these medications may be associated with brain volume loss. To date, our knowledge of the effects of antipsychotic medications on brain structure in humans have been limited by the lack of a double-blind, randomized, placebo-controlled trial with brain imaging. Ours is the first such study. It is considered unethical to do such a study in people with schizophrenia, because of the life-saving benefits of these medications in this illness. However, in people with depression also experiencing psychosis, it was possible to do such a study once people experienced remission from their illness.
 Dr. Voineskos[/caption]
Dr. Aristotle Voineskos MD, PhD, FRCPC
Director, Slaight Family Centre for Youth in Transition and Head,
Kimel Family Translational Imaging-Genetics Laboratory
Campbell Family Mental Health Research Institute
CAMH
University of Toronto
MedicalResearch.com: What is the background for this study?
Response: Uncontrolled studies in humans have shown conflicting results regarding effects of antipsychotic medications on brain structure. Recent studies in animals (e.g. rats and non-human primates) show that these medications may be associated with brain volume loss. To date, our knowledge of the effects of antipsychotic medications on brain structure in humans have been limited by the lack of a double-blind, randomized, placebo-controlled trial with brain imaging. Ours is the first such study. It is considered unethical to do such a study in people with schizophrenia, because of the life-saving benefits of these medications in this illness. However, in people with depression also experiencing psychosis, it was possible to do such a study once people experienced remission from their illness.
Dr. Voineskos[/caption]
Dr. Aristotle Voineskos MD, PhD, FRCPC
Director, Slaight Family Centre for Youth in Transition and Head,
Kimel Family Translational Imaging-Genetics Laboratory
Campbell Family Mental Health Research Institute
CAMH
University of Toronto
MedicalResearch.com: What is the background for this study?
Response: Uncontrolled studies in humans have shown conflicting results regarding effects of antipsychotic medications on brain structure. Recent studies in animals (e.g. rats and non-human primates) show that these medications may be associated with brain volume loss. To date, our knowledge of the effects of antipsychotic medications on brain structure in humans have been limited by the lack of a double-blind, randomized, placebo-controlled trial with brain imaging. Ours is the first such study. It is considered unethical to do such a study in people with schizophrenia, because of the life-saving benefits of these medications in this illness. However, in people with depression also experiencing psychosis, it was possible to do such a study once people experienced remission from their illness.




















 Dr. Hongying (Daisy) Dai[/caption]
Hongying (Daisy) Dai, PhD
Associate Professor
Department of Biostatistics | College of Public Health
University of Nebraska Medical Center
Omaha, NE
MedicalResearch.com: What is the background for this study?
Response: E-cigarette use increased dramatically from 11.7% to 27.5% for high school students and from 3.3% to 10.5% for middle school students during the periods of 2017 - 2019. In September 2018, the Food and Drug Administration (FDA) warned that youth e-cigarette use is reaching an epidemic proportion.
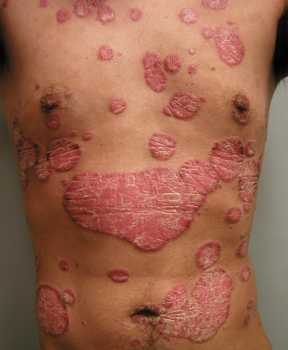
Exposure to secondhand aerosol (SHA) from e-cigarettes is not harmless as e-cigarettes aerosol contains nicotine and potentially harmful substances, including carbonyl compounds, TSNAs, heavy metals, and glycols. This study analyzed the 2015-2018 National Youth Tobacco Survey (NYTS) and the main findings are:
Dr. Hongying (Daisy) Dai[/caption]
Hongying (Daisy) Dai, PhD
Associate Professor
Department of Biostatistics | College of Public Health
University of Nebraska Medical Center
Omaha, NE
MedicalResearch.com: What is the background for this study?
Response: E-cigarette use increased dramatically from 11.7% to 27.5% for high school students and from 3.3% to 10.5% for middle school students during the periods of 2017 - 2019. In September 2018, the Food and Drug Administration (FDA) warned that youth e-cigarette use is reaching an epidemic proportion.
Exposure to secondhand aerosol (SHA) from e-cigarettes is not harmless as e-cigarettes aerosol contains nicotine and potentially harmful substances, including carbonyl compounds, TSNAs, heavy metals, and glycols. This study analyzed the 2015-2018 National Youth Tobacco Survey (NYTS) and the main findings are:

 Prof. Woloshin[/caption]
Steven Woloshin, MD, MS
Professor of Medicine and Community and Family Medicine
Professor, The Dartmouth Institute for Health Policy and Clinical Practice
MedicalResearch.com: What is the background for this study?
Response: Industry spends more on detailing visits and free samples than any other form of prescription drug marketing. There is good evidence that these activities can lead to more use of expensive new drugs over equally effective cheaper options. Given these concerns there have been efforts by some hospitalls and practices to restrict these forms of marketing.
We asked physicians in group practices delivering primary care about how often pharmaceutical reps visit their practice and whether they have a free sample closet.
Prof. Woloshin[/caption]
Steven Woloshin, MD, MS
Professor of Medicine and Community and Family Medicine
Professor, The Dartmouth Institute for Health Policy and Clinical Practice
MedicalResearch.com: What is the background for this study?
Response: Industry spends more on detailing visits and free samples than any other form of prescription drug marketing. There is good evidence that these activities can lead to more use of expensive new drugs over equally effective cheaper options. Given these concerns there have been efforts by some hospitalls and practices to restrict these forms of marketing.
We asked physicians in group practices delivering primary care about how often pharmaceutical reps visit their practice and whether they have a free sample closet. 
 Dr. Liao[/caption]
Joshua M. Liao, MD, MSc, FACP
Assistant Professor, Department of Medicine
Director, UW Medicine Value and Systems Science Lab
Medical Director of Payment Strategy, UW Medicine
University of Washington
Dr. Liao[/caption]
Joshua M. Liao, MD, MSc, FACP
Assistant Professor, Department of Medicine
Director, UW Medicine Value and Systems Science Lab
Medical Director of Payment Strategy, UW Medicine
University of Washington

 MedicalResearch.com: What is the background for this study?
Response: A prior pilot
MedicalResearch.com: What is the background for this study?
Response: A prior pilot 



