Accidents & Violence, Author Interviews, Dermatology / 06.02.2019
Skin Care Products Make Cotton Fabrics More Flammable
MedicalResearch.com Interview with:
[caption id="attachment_47346" align="alignleft" width="200"] Dr. Hall[/caption]
Dr Sarah Hall PhD
Senior Lecturer in Forensic Science
Anglia Ruskin University
MedicalResearch.com: What is the background for this study?
Response: We initially started the study in collaboration with Essex Fire and Rescue Services, as we were already doing some research on the recovery of evidence from fire scenes. During a visit to their cold fire scene facility, they described a tragic fatality with extensive fire damage, which didn’t link with the main fuel in the room. Therefore they questioned if a skin cream, regularly used by the victim, could have contributed as a fuel or ignited to initiate the fire and asked if we would do some initial research. Now we are also working with West Yorkshire and Cambridgeshire Fire and Rescue Service, the London Fire Brigade, St Andrews Centre for Plastic Surgery and Burns and the National Fire Chiefs Council.
We initially started the study in collaboration with Essex Fire and Rescue Services, as we were already doing some research on the recovery of evidence from fire scenes. During a visit to their cold fire scene facility, they described a tragic fatality with extensive fire damage, which didn’t link with the main fuel in the room. Therefore they questioned if a skin cream, regularly used by the victim, could have contributed as a fuel or ignited to initiate the fire and asked if we would do some initial research. Now we are also working with West Yorkshire and Cambridgeshire Fire and Rescue Service, the London Fire Brigade, St Andrews Centre for Plastic Surgery and Burns and the National Fire Chiefs Council.
Dr. Hall[/caption]
Dr Sarah Hall PhD
Senior Lecturer in Forensic Science
Anglia Ruskin University
MedicalResearch.com: What is the background for this study?
Response: We initially started the study in collaboration with Essex Fire and Rescue Services, as we were already doing some research on the recovery of evidence from fire scenes. During a visit to their cold fire scene facility, they described a tragic fatality with extensive fire damage, which didn’t link with the main fuel in the room. Therefore they questioned if a skin cream, regularly used by the victim, could have contributed as a fuel or ignited to initiate the fire and asked if we would do some initial research. Now we are also working with West Yorkshire and Cambridgeshire Fire and Rescue Service, the London Fire Brigade, St Andrews Centre for Plastic Surgery and Burns and the National Fire Chiefs Council.
We initially started the study in collaboration with Essex Fire and Rescue Services, as we were already doing some research on the recovery of evidence from fire scenes. During a visit to their cold fire scene facility, they described a tragic fatality with extensive fire damage, which didn’t link with the main fuel in the room. Therefore they questioned if a skin cream, regularly used by the victim, could have contributed as a fuel or ignited to initiate the fire and asked if we would do some initial research. Now we are also working with West Yorkshire and Cambridgeshire Fire and Rescue Service, the London Fire Brigade, St Andrews Centre for Plastic Surgery and Burns and the National Fire Chiefs Council.
 Dr. Hall[/caption]
Dr Sarah Hall PhD
Senior Lecturer in Forensic Science
Anglia Ruskin University
MedicalResearch.com: What is the background for this study?
Response: We initially started the study in collaboration with Essex Fire and Rescue Services, as we were already doing some research on the recovery of evidence from fire scenes. During a visit to their cold fire scene facility, they described a tragic fatality with extensive fire damage, which didn’t link with the main fuel in the room. Therefore they questioned if a skin cream, regularly used by the victim, could have contributed as a fuel or ignited to initiate the fire and asked if we would do some initial research. Now we are also working with West Yorkshire and Cambridgeshire Fire and Rescue Service, the London Fire Brigade, St Andrews Centre for Plastic Surgery and Burns and the National Fire Chiefs Council.
We initially started the study in collaboration with Essex Fire and Rescue Services, as we were already doing some research on the recovery of evidence from fire scenes. During a visit to their cold fire scene facility, they described a tragic fatality with extensive fire damage, which didn’t link with the main fuel in the room. Therefore they questioned if a skin cream, regularly used by the victim, could have contributed as a fuel or ignited to initiate the fire and asked if we would do some initial research. Now we are also working with West Yorkshire and Cambridgeshire Fire and Rescue Service, the London Fire Brigade, St Andrews Centre for Plastic Surgery and Burns and the National Fire Chiefs Council.
Dr. Hall[/caption]
Dr Sarah Hall PhD
Senior Lecturer in Forensic Science
Anglia Ruskin University
MedicalResearch.com: What is the background for this study?
Response: We initially started the study in collaboration with Essex Fire and Rescue Services, as we were already doing some research on the recovery of evidence from fire scenes. During a visit to their cold fire scene facility, they described a tragic fatality with extensive fire damage, which didn’t link with the main fuel in the room. Therefore they questioned if a skin cream, regularly used by the victim, could have contributed as a fuel or ignited to initiate the fire and asked if we would do some initial research. Now we are also working with West Yorkshire and Cambridgeshire Fire and Rescue Service, the London Fire Brigade, St Andrews Centre for Plastic Surgery and Burns and the National Fire Chiefs Council.
We initially started the study in collaboration with Essex Fire and Rescue Services, as we were already doing some research on the recovery of evidence from fire scenes. During a visit to their cold fire scene facility, they described a tragic fatality with extensive fire damage, which didn’t link with the main fuel in the room. Therefore they questioned if a skin cream, regularly used by the victim, could have contributed as a fuel or ignited to initiate the fire and asked if we would do some initial research. Now we are also working with West Yorkshire and Cambridgeshire Fire and Rescue Service, the London Fire Brigade, St Andrews Centre for Plastic Surgery and Burns and the National Fire Chiefs Council.






 Dr. Coupet[/caption]
Edouard Coupet Jr, MD, MS
Assistant Professor
Department of Emergency Medicine
Yale School of Medicine
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: For many individuals with nonfatal firearm injuries, their only point of contact with the healthcare system may be the emergency department. Both hospital-based violence intervention programs and counseling and safe firearm storage have shown promise in reducing the burden of firearm injury.
In this study, one third of individuals with firearm injuries presented to non-trauma centers. Only 1 out of 5 firearm injuries were assault injuries that led to admission to trauma centers, the population most likely to receive interventions to reduce re-injury.
Dr. Coupet[/caption]
Edouard Coupet Jr, MD, MS
Assistant Professor
Department of Emergency Medicine
Yale School of Medicine
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: For many individuals with nonfatal firearm injuries, their only point of contact with the healthcare system may be the emergency department. Both hospital-based violence intervention programs and counseling and safe firearm storage have shown promise in reducing the burden of firearm injury.
In this study, one third of individuals with firearm injuries presented to non-trauma centers. Only 1 out of 5 firearm injuries were assault injuries that led to admission to trauma centers, the population most likely to receive interventions to reduce re-injury.






 Dr. Leas[/caption]
Eric Leas PhD, MPH
Stanford Prevention Research Center
University of California, San Diego
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Recent research has demonstrated the importance that neighborhood context has on life opportunity, health and well-being that can perpetuate across generations. A strongly defining factor that leads to differences in health outcomes across neighborhoods, such as differences in chronic disease, is the concurrent-uneven distribution of modifiable risk factors for chronic disease.
The main goal of our study was to characterize inequities in smoking, the leading risk factor for chronic disease, between neighborhoods in America's 500 largest cities. To accomplish this aim we used first-of-its-kind data generated from the 500 Cities Project—a collaboration between Robert Wood Johnson Foundation and the US Centers for Disease Control and Prevention—representing the largest effort to provide small-area estimates of modifiable risk factors for chronic disease.
We found that inequities in smoking prevalence are greater within cities than between cities, are highest in the nation’s capital, and are linked to inequities in chronic disease outcomes. We also found that inequities in smoking were associated to inequities in neighborhood characteristics, including race, median household income and the number of tobacco retailers.
Dr. Leas[/caption]
Eric Leas PhD, MPH
Stanford Prevention Research Center
University of California, San Diego
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Recent research has demonstrated the importance that neighborhood context has on life opportunity, health and well-being that can perpetuate across generations. A strongly defining factor that leads to differences in health outcomes across neighborhoods, such as differences in chronic disease, is the concurrent-uneven distribution of modifiable risk factors for chronic disease.
The main goal of our study was to characterize inequities in smoking, the leading risk factor for chronic disease, between neighborhoods in America's 500 largest cities. To accomplish this aim we used first-of-its-kind data generated from the 500 Cities Project—a collaboration between Robert Wood Johnson Foundation and the US Centers for Disease Control and Prevention—representing the largest effort to provide small-area estimates of modifiable risk factors for chronic disease.
We found that inequities in smoking prevalence are greater within cities than between cities, are highest in the nation’s capital, and are linked to inequities in chronic disease outcomes. We also found that inequities in smoking were associated to inequities in neighborhood characteristics, including race, median household income and the number of tobacco retailers.

 Dr. Thompson[/caption]
Rebecca R. Thompson, Ph.D.
Postdoctoral Scholar
Department of Psychological Science
University of California, Irvine
MedicalResearch.com: What is the background for this study?
Response: Our research team has been interested in how people respond to the repeated threat of disaster exposure for many years. We recently published a review of the literature on evacuation from natural disasters, and one of our main findings was that there have been no studies that include assessments of individuals’ intentions, perceptions, and psychological states assessed prior to an approaching storm’s landfall – all prior research has been retrospective, and recall is undoubtedly biased and unreliable. Our goal in undertaking this study was to fill this hole in the literature. We sought to assess individuals' responses to Hurricane Irma in the days leading up to and immediately after its landfall in the State of Florida.
Dr. Thompson[/caption]
Rebecca R. Thompson, Ph.D.
Postdoctoral Scholar
Department of Psychological Science
University of California, Irvine
MedicalResearch.com: What is the background for this study?
Response: Our research team has been interested in how people respond to the repeated threat of disaster exposure for many years. We recently published a review of the literature on evacuation from natural disasters, and one of our main findings was that there have been no studies that include assessments of individuals’ intentions, perceptions, and psychological states assessed prior to an approaching storm’s landfall – all prior research has been retrospective, and recall is undoubtedly biased and unreliable. Our goal in undertaking this study was to fill this hole in the literature. We sought to assess individuals' responses to Hurricane Irma in the days leading up to and immediately after its landfall in the State of Florida.




 Dr. Rebholz[/caption]
Casey M. Rebholz, PhD, MS, MNSP, MPH, FAHA
Assistant Professor, Department of Epidemiology
Johns Hopkins Bloomberg School of Public Health
Core Faculty, Welch Center for Prevention, Epidemiology, and Clinical Research
Baltimore, MD 21287
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Individual beverages have been previously shown to influence risk of a wide range of cardiometabolic diseases. Less is known about beverage consumption and kidney disease risk.
In this study population, we found that one such beverage pattern consisted of soda, sugar-sweetened beverages, and water, and that higher adherence to the sugar-sweetened beverage pattern was associated with greater odds of developing incident kidney disease, even after accounting for demographic characteristics and established risk factors.
Dr. Rebholz[/caption]
Casey M. Rebholz, PhD, MS, MNSP, MPH, FAHA
Assistant Professor, Department of Epidemiology
Johns Hopkins Bloomberg School of Public Health
Core Faculty, Welch Center for Prevention, Epidemiology, and Clinical Research
Baltimore, MD 21287
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Individual beverages have been previously shown to influence risk of a wide range of cardiometabolic diseases. Less is known about beverage consumption and kidney disease risk.
In this study population, we found that one such beverage pattern consisted of soda, sugar-sweetened beverages, and water, and that higher adherence to the sugar-sweetened beverage pattern was associated with greater odds of developing incident kidney disease, even after accounting for demographic characteristics and established risk factors. 





 Sarah Hartz, MD PhD
Assistant Professor
Department of Psychiatry
Washington University School of Medicine in St. Louis
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: This study is the first to show that daily drinking is dangerous. Specifically, drinking four or more times weekly, even if it’s only 1-2 drinks at a time, increases risk of mortality. This is in line with recent studies published in the Lancet, but we were able to break down their lowest drinking categories (up to 12.5 drinks weekly in one and up to 5.6 drinks weekly in the other) and found that the frequency is important, not just the average number of drinks per week. It looks like the increased mortality is predominantly due to cancer-related deaths.
Sarah Hartz, MD PhD
Assistant Professor
Department of Psychiatry
Washington University School of Medicine in St. Louis
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: This study is the first to show that daily drinking is dangerous. Specifically, drinking four or more times weekly, even if it’s only 1-2 drinks at a time, increases risk of mortality. This is in line with recent studies published in the Lancet, but we were able to break down their lowest drinking categories (up to 12.5 drinks weekly in one and up to 5.6 drinks weekly in the other) and found that the frequency is important, not just the average number of drinks per week. It looks like the increased mortality is predominantly due to cancer-related deaths.



 Dr. Elgendy[/caption]
Akram Elgendy MD
Division of Cardiovascular Medicine
University of Florida
MedicalResearch.com: What is the background for this study?
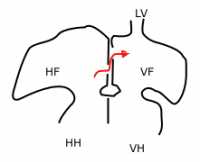
Response: Recent clinical trials have demonstrated that percutaneous patent foramen ovale closure is associated with lower risk of stroke recurrence in cryptogenic stroke patients. However, new-onset atrial fibrillation (AF) has been reported as a safety concern. To better understand the risk of new-onset AF, we performed a meta-analysis of PFO closure trials in patients with cryptogenic stroke and migraine.
Dr. Elgendy[/caption]
Akram Elgendy MD
Division of Cardiovascular Medicine
University of Florida
MedicalResearch.com: What is the background for this study?
Response: Recent clinical trials have demonstrated that percutaneous patent foramen ovale closure is associated with lower risk of stroke recurrence in cryptogenic stroke patients. However, new-onset atrial fibrillation (AF) has been reported as a safety concern. To better understand the risk of new-onset AF, we performed a meta-analysis of PFO closure trials in patients with cryptogenic stroke and migraine.



 Prof. Kleiman[/caption]
Prof. Mark A. R. Kleiman PhD
Affiliated Faculty, NYU Wagner; Professor of Public Policy
NYU Marron Institute of Urban Management
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: As state after state legalizes the sale of cannabis, the question of cannabis-impaired driving is getting more attention. There is evidence that the practice has become more common, both because cannabis use - and especially heavy, frequent use - has increased and because a distressingly large fraction of cannabis users believe, falsely, that stoned driving is safe.
The natural response to the problem is to treat cannabis on a par with alcohol: fairly severe criminal penalties for impaired driving, with impairment defined by a specific level of the drug in the body. The paper argues that this would be a mistake, for four independent reasons:
- While cannabis makes driving riskier, it does so by about a factor of two, with no strongly observed dependency on dosage. Alcohol, by contrast, has a steep dose-effect curve. At the legal limit of 0.08% blood alcohol content by weight, the relative risk of drunk driving is at least eight; at 0.15%, which is fairly common, the relative risk has been estimated at 30-50. So there is no justification for punishing stoned driving as severely as we punish drunk driving.
- The lack of evidence of a strong dose-effect relationship suggests that a legal standard based on the content of cannabinoids in blood may not be appropriate.
- Even if a blood standard were valid, the lack of a breath test would make enforcing that standard nearly impossible as a practical matter.
- The long and unpredictable course of cannabis metabolism means that frequent users will be at risk of failing a drug test even when they are neither subjectively intoxicated nor objectively impaired. Worse, they would have no way of judging in advance whether or not driving would be legal. The result would be a re-criminalization of cannabis use through the back door.
Prof. Kleiman[/caption]
Prof. Mark A. R. Kleiman PhD
Affiliated Faculty, NYU Wagner; Professor of Public Policy
NYU Marron Institute of Urban Management
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: As state after state legalizes the sale of cannabis, the question of cannabis-impaired driving is getting more attention. There is evidence that the practice has become more common, both because cannabis use - and especially heavy, frequent use - has increased and because a distressingly large fraction of cannabis users believe, falsely, that stoned driving is safe.
The natural response to the problem is to treat cannabis on a par with alcohol: fairly severe criminal penalties for impaired driving, with impairment defined by a specific level of the drug in the body. The paper argues that this would be a mistake, for four independent reasons:
- While cannabis makes driving riskier, it does so by about a factor of two, with no strongly observed dependency on dosage. Alcohol, by contrast, has a steep dose-effect curve. At the legal limit of 0.08% blood alcohol content by weight, the relative risk of drunk driving is at least eight; at 0.15%, which is fairly common, the relative risk has been estimated at 30-50. So there is no justification for punishing stoned driving as severely as we punish drunk driving.
- The lack of evidence of a strong dose-effect relationship suggests that a legal standard based on the content of cannabinoids in blood may not be appropriate.
- Even if a blood standard were valid, the lack of a breath test would make enforcing that standard nearly impossible as a practical matter.
- The long and unpredictable course of cannabis metabolism means that frequent users will be at risk of failing a drug test even when they are neither subjectively intoxicated nor objectively impaired. Worse, they would have no way of judging in advance whether or not driving would be legal. The result would be a re-criminalization of cannabis use through the back door.