Author Interviews, COVID -19 Coronavirus, Occupational Health / 16.11.2020
Nurses Particularly Hard Hit By COVID-19 Infections
MedicalResearch.com Interview with:
[caption id="attachment_55952" align="alignleft" width="200"] Dr. Barrett[/caption]
Emily Barrett, PhD
Associate Professor
Department of Biostatistics and Epidemiology
Rutgers School of Public Health
MedicalResearch.com: What is the background for this study?
Response: We started this study in the very early stages of the pandemic to look at SARS-CoV-2 viral transmission and disease severity in health care workers as compared to non-health care workers. There was a tremendous amount of fear and uncertainty about the virus and the early anecdotal reports coming out of China and Italy highlighted the plight of many frontline health care workers who had been infected on the job. We knew that our U.S. health care workers would soon be facing this tremendous challenge. We started this study to examine risks of infection in our vulnerable frontline health care workers and a comparison group of non-health care workers. Our results are from the early stages of the U.S. pandemic in March-April 2020.
Dr. Barrett[/caption]
Emily Barrett, PhD
Associate Professor
Department of Biostatistics and Epidemiology
Rutgers School of Public Health
MedicalResearch.com: What is the background for this study?
Response: We started this study in the very early stages of the pandemic to look at SARS-CoV-2 viral transmission and disease severity in health care workers as compared to non-health care workers. There was a tremendous amount of fear and uncertainty about the virus and the early anecdotal reports coming out of China and Italy highlighted the plight of many frontline health care workers who had been infected on the job. We knew that our U.S. health care workers would soon be facing this tremendous challenge. We started this study to examine risks of infection in our vulnerable frontline health care workers and a comparison group of non-health care workers. Our results are from the early stages of the U.S. pandemic in March-April 2020.
 Dr. Barrett[/caption]
Emily Barrett, PhD
Associate Professor
Department of Biostatistics and Epidemiology
Rutgers School of Public Health
MedicalResearch.com: What is the background for this study?
Response: We started this study in the very early stages of the pandemic to look at SARS-CoV-2 viral transmission and disease severity in health care workers as compared to non-health care workers. There was a tremendous amount of fear and uncertainty about the virus and the early anecdotal reports coming out of China and Italy highlighted the plight of many frontline health care workers who had been infected on the job. We knew that our U.S. health care workers would soon be facing this tremendous challenge. We started this study to examine risks of infection in our vulnerable frontline health care workers and a comparison group of non-health care workers. Our results are from the early stages of the U.S. pandemic in March-April 2020.
Dr. Barrett[/caption]
Emily Barrett, PhD
Associate Professor
Department of Biostatistics and Epidemiology
Rutgers School of Public Health
MedicalResearch.com: What is the background for this study?
Response: We started this study in the very early stages of the pandemic to look at SARS-CoV-2 viral transmission and disease severity in health care workers as compared to non-health care workers. There was a tremendous amount of fear and uncertainty about the virus and the early anecdotal reports coming out of China and Italy highlighted the plight of many frontline health care workers who had been infected on the job. We knew that our U.S. health care workers would soon be facing this tremendous challenge. We started this study to examine risks of infection in our vulnerable frontline health care workers and a comparison group of non-health care workers. Our results are from the early stages of the U.S. pandemic in March-April 2020.



![MedicalResearch.com Interview with: Jeffrey D. Kent, M.D., FACG, FACP Executive Vice President, Medical Affairs and Outcomes Research Horizon MedicalResearch.com: What is the background for this study? What is the marker for reduced immunogenicity with Pegloticase? Response: Pegloticase is a recombinant, pegylated uricase that is used for treatment of chronic gout in patients who fail oral urate lowering therapy (uncontrolled gout) and has a demonstrated impact on the serum uric acid (sUA) level. As with other biologics, in some people the body’s immune system develops anti-drug antibodies and reduces the effectiveness of the biologic therapy. Recent case series and open-label trials have suggested that using an immunomodulator with pegloticase has the potential to increase the durability of response so patients can receive a full course of therapy. Researchers in the RECIPE trial sought to examine whether the co-administration of disease-modifying antirheumatic drugs (DMARDs), specifically mycophenolate mofetil, may mitigate this loss of efficacy and increase in response rates for people living with uncontrolled gout MedicalResearch.com: Are symptoms of gout improved as well as reduced infusion reactions? Response Results from this trial indicated that short-term concomitant use of mycophenolate mofetil with pegloticase was generally well tolerated. It was also associated with a statistically significant and clinically meaningful impact on the proportion of patients achieving and maintaining an sUA ≤6 mg/dL at 24 weeks. No infusion reactions were reported in the pegloticase/mycophenolate mofetil arm (0 or 22 patients) compared to 30 percent (3 of 10) of patients reporting infusion reactions in the pegloticase/placebo arm. It’s been well established that in patients receiving pegloticase with persistent urate lowering, they experience relatively rapid resolution of tophi indicating significant reductions in their urate burden. MedicalResearch.com: What are the main findings? Response: This is the first randomized controlled trial evaluating pegloticase co-prescribed with an immunomodulator compared to pegloticase with placebo. Data showed that 86.4 percent of patients (19 of 22) receiving co-therapy of pegloticase with mycophenolate mofetil achieved an sUA ≤ 6 mg/dL through Month 3, the primary study endpoint, compared to 40.0 percent of patients (4 of 10) receiving pegloticase monotherapy. After Month 3, all patients received pegloticase only and at Month 6 a sustained response was shown in 68.2 percent (15 of 22) of patients who had received pegloticase with mycophenolate mofetil versus 30.0 percent (3 of 10) of patients who received pegloticase and placebo. This data adds to the growing body of evidence on the concomitant use of pegloticase with an immunomodulator to ultimately help more patients receive a full course of therapy and improve outcomes and may help shift the treatment paradigm in uncontrolled gout. MedicalResearch.com: What should readers take away from your report? Response: While rheumatologists are familiar with and may use DMARDs for other autoimmune conditions to minimize the development of anti-drug antibodies and increase response to therapies, data shows that the use of an immunomodulating therapy in patients with uncontrolled gout can improve response rates. MedicalResearch.com: What recommendations do you have for future research as a result of this work? Response: There is a consistent pattern demonstrating that the concomitant use of pegloticase and an immunomodulator can improve patient outcomes without introducing additional toxicities. As clinicians we understand the immense burden gout places on our patients. Future research should continue exploring options to maximize the benefit of effective treatments to improve patient outcomes. MedicalResearch.com: Is there anything else you would like to add? Response: Uncontrolled gout is a chronic, systemic inflammatory condition and we continue to see data linking it to many comorbid conditions. Horizon is evaluating the use of methotrexate to improve response rates for pegloticase. We are committed to exploring various immunotherapy co-treatment options to allow both patients and clinicians to address elevated sUA levels to minimize urate burden and avoid lasting damage to the body. RECIPE is an investigator-initiated trial led by Puja Khanna, M.D., M.P.H. and Kenneth Saag, M.D., M.Sc. Citation: Khanna P, Khanna D, Cutter G, Foster J, Melnick J, Jaafar S, Biggers S, Rahman A, Kuo H, Feese M, Saag K. Reducing Immunogenicity of Pegloticase (RECIPE) with Concomitant Use of Mycophenolate Mofetil in Patients with Refractory Gout—a Phase II Double Blind Randomized Controlled Trial [abstract]. Arthritis Rheumatol. 2020; 72 (suppl 10). https://acrabstracts.org/abstract/reducing-immunogenicity-of-pegloticase-recipe-with-concomitant-use-of-mycophenolate-mofetil-in-patients-with-refractory-gout-a-phase-ii-double-blind-randomized-controlled-trial/. Accessed November 12, 2020. [subscribe] Last Modified: [last-modified] The information on MedicalResearch.com is provided for educational purposes only, and is in no way intended to diagnose, cure, or treat any medical or other condition. Always seek the advice of your physician or other qualified health and ask your doctor any questions you may have regarding a medical condition. In addition to all other limitations and disclaimers in this agreement, service provider and its third party providers disclaim any liability or loss in connection with the content provided on this website.](https://medicalresearch.com/wp-content/uploads/2020/11/Dr-Jeffrey-Kent.jpg)


 Prof. Pottel[/caption]
Prof. Dr. Hans Pottel PhD
Professeur Invité (titre honorifique)
Faculté de Médecine
Université de Liège
KULeuven-KULAK, Kortrijk, Belgium
MedicalResearch.com: What is the background for this study? Why do we need a new GFR?
Response: The currently recommended equations have flaws, mainly because there is one equation (CKiD) recommended for children, and one recommended (CKD-EPI) for adults (by KDIGO). When transitioning from pediatric nephrology care to adult nephrology care, the switch from CKiD to CKD-EPI causes implausible jumps (of more than 50%), mainly because CKD-EPI largely overestimates GFR in young adults (18-30 years). The new equation overcomes this problem as it applies for all ages (for children and adults) and overcomes the known flaws of the currently most used equations. The new equation is less biased and more precise across the full age spectrum and for the full range of serum creatinine concentrations.
The equation was developed in 11 251 participants from 7 cohorts (development and internal validation datasets) and validated in 8 378 participants from 6 cohorts (external validation dataset). Data were coming from European and American nephrology centers. No patients of African-American ancestry were included. Actually, the previously published FAS-equation served as the basic mathematical form for the equation, but we adjusted the power coefficients for serum creatinine (very much like it was done in the CKD-EPI equation). You could say that we used properties of both the FAS and CKD-EPI equation to come to an improved equation to estimate GFR.
Prof. Pottel[/caption]
Prof. Dr. Hans Pottel PhD
Professeur Invité (titre honorifique)
Faculté de Médecine
Université de Liège
KULeuven-KULAK, Kortrijk, Belgium
MedicalResearch.com: What is the background for this study? Why do we need a new GFR?
Response: The currently recommended equations have flaws, mainly because there is one equation (CKiD) recommended for children, and one recommended (CKD-EPI) for adults (by KDIGO). When transitioning from pediatric nephrology care to adult nephrology care, the switch from CKiD to CKD-EPI causes implausible jumps (of more than 50%), mainly because CKD-EPI largely overestimates GFR in young adults (18-30 years). The new equation overcomes this problem as it applies for all ages (for children and adults) and overcomes the known flaws of the currently most used equations. The new equation is less biased and more precise across the full age spectrum and for the full range of serum creatinine concentrations.
The equation was developed in 11 251 participants from 7 cohorts (development and internal validation datasets) and validated in 8 378 participants from 6 cohorts (external validation dataset). Data were coming from European and American nephrology centers. No patients of African-American ancestry were included. Actually, the previously published FAS-equation served as the basic mathematical form for the equation, but we adjusted the power coefficients for serum creatinine (very much like it was done in the CKD-EPI equation). You could say that we used properties of both the FAS and CKD-EPI equation to come to an improved equation to estimate GFR. Dr. Ganson[/caption]
Kyle T. Ganson, PhD, MSW
Assistant Professor, Factor-Inwentash Faculty of Social Work
University of Toronto
Toronto, Canada
[caption id="attachment_55902" align="alignleft" width="132"]
Dr. Ganson[/caption]
Kyle T. Ganson, PhD, MSW
Assistant Professor, Factor-Inwentash Faculty of Social Work
University of Toronto
Toronto, Canada
[caption id="attachment_55902" align="alignleft" width="132"] Dr. Nagata[/caption]
Jason Nagata, MD, MSc
Assistant Professor of Pediatrics
University of California, San Francisco
San Francisco, California, USA
MedicalResearch.com: What is the background for this study?
Response: A quarter of young adults in the US have reported being unemployed during the COVID-19 pandemic. Young adults may be especially affected by employment loss as they often work in industries most adversely affected by social distancing.
MedicalResearch.com: What are the main findings?
Response: Among a sample of nearly 5,000 young adults age 18 to 26 in the US, we found that since March 2020, young adults who lost their job or were part of a household that experienced employment loss were more likely than those with secure employment to experience four common symptoms of anxiety and depression. This was also true of young adults who expected an employment loss in the next four weeks. The study also found that symptoms of anxiety and depression were common among the sample of young adults. In the seven days prior to the survey, 75% reported being nervous, anxious or on edge, 68% reported not being able to stop or control worrying, 67% reported having little interest or pleasure in doing things, and 64% reported feeling down, depressed, or hopeless.
Dr. Nagata[/caption]
Jason Nagata, MD, MSc
Assistant Professor of Pediatrics
University of California, San Francisco
San Francisco, California, USA
MedicalResearch.com: What is the background for this study?
Response: A quarter of young adults in the US have reported being unemployed during the COVID-19 pandemic. Young adults may be especially affected by employment loss as they often work in industries most adversely affected by social distancing.
MedicalResearch.com: What are the main findings?
Response: Among a sample of nearly 5,000 young adults age 18 to 26 in the US, we found that since March 2020, young adults who lost their job or were part of a household that experienced employment loss were more likely than those with secure employment to experience four common symptoms of anxiety and depression. This was also true of young adults who expected an employment loss in the next four weeks. The study also found that symptoms of anxiety and depression were common among the sample of young adults. In the seven days prior to the survey, 75% reported being nervous, anxious or on edge, 68% reported not being able to stop or control worrying, 67% reported having little interest or pleasure in doing things, and 64% reported feeling down, depressed, or hopeless.

 Dr. Al Rifai[/caption]
Mahmoud Al Rifai, MD, MPH
Cardiovascular Disease Fellow
Baylor College of Medicine Houston, TX
[caption id="attachment_55680" align="alignleft" width="150"]
Dr. Al Rifai[/caption]
Mahmoud Al Rifai, MD, MPH
Cardiovascular Disease Fellow
Baylor College of Medicine Houston, TX
[caption id="attachment_55680" align="alignleft" width="150"] Dr. Virani[/caption]
Salim S. Virani, MD, PhD, FACC, FAHA, FASPC
Professor, Section of Cardiovascular Research
Director, Cardiology Fellowship Training Program
Baylor College of Medicine
Staff Cardiologist, Michael E. DeBakey Veterans Affairs Medical Center
Co-Director, VA Advanced Fellowship in Health Services Research & Development at the Michael E. DeBakey VA Medical Center
Investigator, Health Policy, Quality and Informatics Program
Michael E. DeBakey Veterans Affairs Medical Center HSR&D Center of Innovation Houston, TX
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: E-cigarettes have gained popularity since their introduction in the U.S. market nearly 20 years ago and their use has increased especially among younger adults. On the other hand, public health efforts aimed at curbing tobacco use over the past few decades have resulted in a decrease in cigarette use. However, state-specific laws and regional cultural differences with regards to perception of these products may result in variability in tobacco use patterns. We therefore evaluate temporal changes in e-cigarette and cigarette use in each U.S. state between the years 2016 to 2018.
Dr. Virani[/caption]
Salim S. Virani, MD, PhD, FACC, FAHA, FASPC
Professor, Section of Cardiovascular Research
Director, Cardiology Fellowship Training Program
Baylor College of Medicine
Staff Cardiologist, Michael E. DeBakey Veterans Affairs Medical Center
Co-Director, VA Advanced Fellowship in Health Services Research & Development at the Michael E. DeBakey VA Medical Center
Investigator, Health Policy, Quality and Informatics Program
Michael E. DeBakey Veterans Affairs Medical Center HSR&D Center of Innovation Houston, TX
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: E-cigarettes have gained popularity since their introduction in the U.S. market nearly 20 years ago and their use has increased especially among younger adults. On the other hand, public health efforts aimed at curbing tobacco use over the past few decades have resulted in a decrease in cigarette use. However, state-specific laws and regional cultural differences with regards to perception of these products may result in variability in tobacco use patterns. We therefore evaluate temporal changes in e-cigarette and cigarette use in each U.S. state between the years 2016 to 2018.

 Prof Jeffrey S Tobias, Prof Jayant S Vaidya, Prof Max Bulsara. and Prof Michael Baum[/caption]
Response: The findings of the large international randomised trial (TARGIT-A trial), published in the British Medical Journal (
Prof Jeffrey S Tobias, Prof Jayant S Vaidya, Prof Max Bulsara. and Prof Michael Baum[/caption]
Response: The findings of the large international randomised trial (TARGIT-A trial), published in the British Medical Journal (




 Dr. Spann[/caption]
Marisa N. Spann, PhD, MPH
Columbia University Irving Medical Center
New York, New York
MedicalResearch.com: What is the background for this study?
Response: Prior research has demonstrated that higher maternal pre-pregnancy body mass index is associated with adverse long-term outcomes for offspring including obesity, poorer cognitive and social abilities, and increased risk of psychiatric disorders.
MedicalResearch.com: What are the main findings?
Response: In this study, we investigated the association of maternal pre-pregnancy body mass index with fetal growth and neonatal functional connectivity and found that maternal pre-pregnancy BMI has a significant positive correlation with fetal weight and with greater thalamic connectivity of the brain.
Dr. Spann[/caption]
Marisa N. Spann, PhD, MPH
Columbia University Irving Medical Center
New York, New York
MedicalResearch.com: What is the background for this study?
Response: Prior research has demonstrated that higher maternal pre-pregnancy body mass index is associated with adverse long-term outcomes for offspring including obesity, poorer cognitive and social abilities, and increased risk of psychiatric disorders.
MedicalResearch.com: What are the main findings?
Response: In this study, we investigated the association of maternal pre-pregnancy body mass index with fetal growth and neonatal functional connectivity and found that maternal pre-pregnancy BMI has a significant positive correlation with fetal weight and with greater thalamic connectivity of the brain. 




 Dr. Sachdev[/caption]
Darpun D. Sachdev, M.D.
Case investigation and Contact tracing Branch Chief
SFDPH Covid Command Center
San Francisco Department of Public Health
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The ultimate goal of contact tracing is to rapidly identify and isolate contacts who are COVID-19 positive before they have time to transmit to others. As mentioned in the published research letter by SFDPH, through JAMA, during early shelter-in-place (from April to June 2020), our contact tracing program successfully reached greater than 80% of cases and contacts within a median timeframe of 6 days from the onset of their case’s symptoms. Approximately 10% of named contacts were newly diagnosed with COVID-19 (compared to 2% positivity during this time period). Household contacts made up approximately 80% of all identified contacts, but 90% of contacts who tested positive lived in the same household as the case. Secondary cases (contacts who were found to be newly diagnosed with COVID-19) were traced and quarantined within 6 days of the case’s symptom onset.
With that said, the 6-day time difference between symptom onset and contact notification raises concern regarding the overall effectiveness of tracing in preventing onward transmission by infected contacts. We are working with community-based organizations to scale up access to testing and culturally competent tracing and wraparound services. Currently, we have now decreased the time difference to 5 days. Moreover, given that the majority of contacts resided in the same household, transmission could have occurred presymptomatically such that by the time infected contacts were identified, they might have already transmitted the virus. Hence, why SFDPH, on May 5, 2020, implemented the recommendation of universal testing for COVID-19 contacts, regardless of symptoms.
We recommend that testing should be offered to all contacts regardless of symptoms and encourage local health departments to adopt novel ways of increasing testing access for contacts.
Dr. Sachdev[/caption]
Darpun D. Sachdev, M.D.
Case investigation and Contact tracing Branch Chief
SFDPH Covid Command Center
San Francisco Department of Public Health
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The ultimate goal of contact tracing is to rapidly identify and isolate contacts who are COVID-19 positive before they have time to transmit to others. As mentioned in the published research letter by SFDPH, through JAMA, during early shelter-in-place (from April to June 2020), our contact tracing program successfully reached greater than 80% of cases and contacts within a median timeframe of 6 days from the onset of their case’s symptoms. Approximately 10% of named contacts were newly diagnosed with COVID-19 (compared to 2% positivity during this time period). Household contacts made up approximately 80% of all identified contacts, but 90% of contacts who tested positive lived in the same household as the case. Secondary cases (contacts who were found to be newly diagnosed with COVID-19) were traced and quarantined within 6 days of the case’s symptom onset.
With that said, the 6-day time difference between symptom onset and contact notification raises concern regarding the overall effectiveness of tracing in preventing onward transmission by infected contacts. We are working with community-based organizations to scale up access to testing and culturally competent tracing and wraparound services. Currently, we have now decreased the time difference to 5 days. Moreover, given that the majority of contacts resided in the same household, transmission could have occurred presymptomatically such that by the time infected contacts were identified, they might have already transmitted the virus. Hence, why SFDPH, on May 5, 2020, implemented the recommendation of universal testing for COVID-19 contacts, regardless of symptoms.
We recommend that testing should be offered to all contacts regardless of symptoms and encourage local health departments to adopt novel ways of increasing testing access for contacts.
 Dr. Adnan[/caption]
Darbaz Adnan, MBChB
Lab Research Assistant
Department of Internal Medicine - Section of Gastroenterology
Rush University Medical Center
Chicago, Illinois 60612
MedicalResearch.com: What is the background for this study?
Response: - We have conducted a large study of over 1000 patients at a major COVID-19 response center in Chicago at Rush University Medical Center, to assess for the frequency of initial GI symptoms (diarrhea, vomiting, abdominal pain) and evaluate whether these symptoms in adult COVID-19 positive could predict the disease course. Overall, 22.4% of our patients reported at least one GI symptom at the onset of their infection, with nausea/vomiting being the most common complaint. GI symptoms in COVID-19 patients were associated with worse outcomes.
Dr. Adnan[/caption]
Darbaz Adnan, MBChB
Lab Research Assistant
Department of Internal Medicine - Section of Gastroenterology
Rush University Medical Center
Chicago, Illinois 60612
MedicalResearch.com: What is the background for this study?
Response: - We have conducted a large study of over 1000 patients at a major COVID-19 response center in Chicago at Rush University Medical Center, to assess for the frequency of initial GI symptoms (diarrhea, vomiting, abdominal pain) and evaluate whether these symptoms in adult COVID-19 positive could predict the disease course. Overall, 22.4% of our patients reported at least one GI symptom at the onset of their infection, with nausea/vomiting being the most common complaint. GI symptoms in COVID-19 patients were associated with worse outcomes.
 Dr. Curtis J. Donskey[/caption]
Curtis J. Donskey, MD
Professor of Medicine
Case Western Reserve University
Staff Physician, Infectious Diseases Section,
Louis Stokes Cleveland VA Medical Center
MedicalResearch.com: What is the background for this study?
Response: The goal of the study was to obtain a better understanding of how healthcare-associated pathogens are transmitted. Infection control efforts tend to emphasize hand hygiene and cleaning of high-touch surfaces in patient rooms. However, there is evidence that portable equipment and floors could be underappreciated sources of transmission.
We previously found that a nonpathogenic virus inoculated onto floors in patient rooms spread rapidly to the hands of patients and to surfaces in the room and throughout the ward. This raised concern that pathogens could spread by the same route.
Dr. Curtis J. Donskey[/caption]
Curtis J. Donskey, MD
Professor of Medicine
Case Western Reserve University
Staff Physician, Infectious Diseases Section,
Louis Stokes Cleveland VA Medical Center
MedicalResearch.com: What is the background for this study?
Response: The goal of the study was to obtain a better understanding of how healthcare-associated pathogens are transmitted. Infection control efforts tend to emphasize hand hygiene and cleaning of high-touch surfaces in patient rooms. However, there is evidence that portable equipment and floors could be underappreciated sources of transmission.
We previously found that a nonpathogenic virus inoculated onto floors in patient rooms spread rapidly to the hands of patients and to surfaces in the room and throughout the ward. This raised concern that pathogens could spread by the same route.
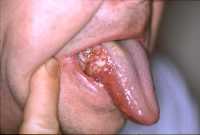
![MedicalResearch.com Interview with: Selin Tokez, PhD Student Department of Dermatology Erasmus MC, Rotterdam MedicalResearch.com: What is the background for this study? Response: Cutaneous squamous cell carcinoma (cSCC) is the second most common skin cancer worldwide with still increasing incidence rates. Given these high incidence rates together with the associated health costs and possibility of fatal progression, it is extremely important to have accurate and complete data on the epidemiology of this disease. Nevertheless, national cancer registries in many countries do not routinely record cSCC cases and therefore currently known numbers are mainly based on incomplete data sources. Additionally, if cSCC cases are registered, this usually only concerns the first cSCC per patient while we know that, contrary to many other malignant neoplasms, patients may develop numerous cSCCs over time. MedicalResearch.com: What are the main findings? Response: In the present study, we analyzed Dutch nationwide data comprising about 145,000 patients with a first invasive cSCC diagnosis between the years 1989 and 2017. We found that the incidence rates of a first cSCC per patient almost tripled in male patients and increased about fivefold in female patients in this 30-year time period. Also, we had data on all cSCCs per patient for the year 2017 and could therefore compare this with the data on only the first cSCC per patient: incidence rates increased by 58% for men and 35% for women when multiple cSCCs were considered. In absolute numbers, this resulted in an increase of 45% in cSCC diagnoses in 2017. Lastly, we extended our analyses by predicting future cSCC incidence rates up to 2027. Given that no substantially effective measures are undertaken in the near future, current cSCC incidence rates will increase with 23% in males and 29% in females in the next decade. MedicalResearch.com: What should readers take away from your report? Response: We could summarize our main message in two points: while people generally know that cSCC is a very common disease with increasing incidence rates, it is not taken into account that these numbers are often based on incomplete data registries and that the real numbers are even higher. In this paper, we provided these numbers for a period of 30 years based on highly accurate data from the Netherlands Cancer Registry. On top of that, as a second main finding, we showed that the real burden caused by cSCC is approximately 50% higher (taken males and females together) when all cSCC diagnoses in 1 year are registered instead of only the first tumor per patient. Together with our prediction analyses that showed an on average 26% further increase for the coming decade, this will have enormous implications for the dermato-oncological health care planning and cost management. Our results urgently call for revision of skin cancer health policies to be able to cope with this rising burden of cSCC management. Ultimately, primary prevention will remain the key strategy to halt the increasing trend in cSCC incidence and the occurrence of multiple cSCCs per patient, which we hope to further stimulate with our paper as well. MedicalResearch.com: What recommendations do you have for future research as a result of this work? Response: As we had data on multiple cSCCs for only one year, we would suggest to perform trend analyses for multiple cSCCs per patient as well when a longer follow-up duration has been reached. Furthermore, it would be very relevant to identify high-risk cSCCs or patients at risk for multiple cSCCs in order to be able to establish efficient follow-up regimens and take these high risk groups into account when revising skin cancer health policies. MedicalResearch.com: Is there anything else you would like to add? Response: The authors of this study have no conflicts of interest that are relevant to this article. Citation: Tokez S, Hollestein L, Louwman M, Nijsten T, Wakkee M. Incidence of Multiple vs First Cutaneous Squamous Cell Carcinoma on a Nationwide Scale and Estimation of Future Incidences of Cutaneous Squamous Cell Carcinoma. JAMA Dermatol. Published online October 28, 2020. doi:10.1001/jamadermatol.2020.3677 [subscribe] Last Modified: [last-modified] The information on MedicalResearch.com is provided for educational purposes only, and is in no way intended to diagnose, cure, or treat any medical or other condition. Always seek the advice of your physician or other qualified health and ask your doctor any questions you may have regarding a medical condition. In addition to all other limitations and disclaimers in this agreement, service provider and its third party providers disclaim any liability or loss in connection with the content provided on this website.](https://medicalresearch.com/wp-content/uploads/2020/10/squamous-cell-cancer-dermnetnz-image.jpg)