Author Interviews, BMJ, Obstructive Sleep Apnea, Pediatrics, Sleep Disorders, Surgical Research / 09.11.2018
Tonsillectomy Often Done When Not Indicated (and vice versa!)
MedicalResearch.com Interview with:
[caption id="attachment_45826" align="alignleft" width="200"]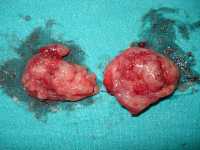 A pair of tonsils after surgical removal
A pair of tonsils after surgical removal
Wikipedia image[/caption] Tom Marshall, MSc, PhD, MRCGP, FFPH Professor of public health and primary care Institute of Applied Health Research University of Birmingham, Birmingham, UK MedicalResearch.com: What is the background for this study? Response: Tonsillectomy is one of the most common childhood surgical procedures. There are two main indications: recurrent sore throat and sleep-related breathing problems (including obstructive sleep apnoea). Jack Paradise’s 1984 study made clear tonsillectomy is modestly effective in children with frequent, severe sore throats: seven in one year, or five yearly in two successive years, or three yearly in three successive years. Sore throats must have symptoms: fever, pus seen on tonsils, lymphadenopathy or confirmed Streptococcal infection. With surgery, children average two sore throats in the next year, without surgery, three. Two years later there is no difference. Further research shows the benefits are too tiny to justify surgery in children with less frequent, less severe or undocumented sore throats. Subsequent randomised controlled trials have not changed the evidence. There isn’t enough good evidence to support surgery in children with obstructive sleep apnoea or sleep related breathing problems. Tonsillectomy is not a trivial procedure, about 2% are readmitted with haemorrhage and about 1 in 40,000 dies. Childhood tonsillectomy is linked to risk of adult autoimmune diseases. It is important to be sure tonsillectomy is only undertaken in children where there are evidence-based indications.
 A pair of tonsils after surgical removal
A pair of tonsils after surgical removalWikipedia image[/caption] Tom Marshall, MSc, PhD, MRCGP, FFPH Professor of public health and primary care Institute of Applied Health Research University of Birmingham, Birmingham, UK MedicalResearch.com: What is the background for this study? Response: Tonsillectomy is one of the most common childhood surgical procedures. There are two main indications: recurrent sore throat and sleep-related breathing problems (including obstructive sleep apnoea). Jack Paradise’s 1984 study made clear tonsillectomy is modestly effective in children with frequent, severe sore throats: seven in one year, or five yearly in two successive years, or three yearly in three successive years. Sore throats must have symptoms: fever, pus seen on tonsils, lymphadenopathy or confirmed Streptococcal infection. With surgery, children average two sore throats in the next year, without surgery, three. Two years later there is no difference. Further research shows the benefits are too tiny to justify surgery in children with less frequent, less severe or undocumented sore throats. Subsequent randomised controlled trials have not changed the evidence. There isn’t enough good evidence to support surgery in children with obstructive sleep apnoea or sleep related breathing problems. Tonsillectomy is not a trivial procedure, about 2% are readmitted with haemorrhage and about 1 in 40,000 dies. Childhood tonsillectomy is linked to risk of adult autoimmune diseases. It is important to be sure tonsillectomy is only undertaken in children where there are evidence-based indications.



 Nicholas Reed AuD[/caption]
Nicholas S. Reed, AuD
Assistant Professor | Department of Otolaryngology-Head/Neck Surgery
Core Faculty | Cochlear Center for Hearing and Public Health
Johns Hopkins University School of Medicine
Johns Hopkins University Bloomberg School of Public Health
MedicalResearch.com: What is the background for this study?
Response: This study was a true team effort. It was funded by AARP and AARP Services, INC and the research was a collaboration of representatives from Johns Hopkins University, OptumLabs, University of California – San Francisco, and AARP Services, INC. Given all of the resent research on downstream effects of hearing loss on important health outcomes such as cognitive decline, falls, and dementia, the aim was to explore how persons with hearing loss interacted with the healthcare system in terms of cost and utilization.
MedicalResearch.com: What are the main findings?
Response: Over a 10 year period, untreated hearing loss (hearing aid users were excluded from this study as they are difficult to capture in the claims database) was associated with higher healthcare spending and utilization. Specifically, over 10 years, persons with untreated hearing loss spent 46.5% more, on average, on healthcare (to the tune of approximately $22000 more) than those without evidence of hearing loss. Furthermore, persons with untreated hearing loss had 44% and 17% higher risk for 30-day readmission and emergency department visit, respectively.
Similar relationships were seen across other measures where persons with untreated hearing loss were more likely to be hospitalized and spent longer in the hospital compared to those without evidence of hearing loss.
Nicholas Reed AuD[/caption]
Nicholas S. Reed, AuD
Assistant Professor | Department of Otolaryngology-Head/Neck Surgery
Core Faculty | Cochlear Center for Hearing and Public Health
Johns Hopkins University School of Medicine
Johns Hopkins University Bloomberg School of Public Health
MedicalResearch.com: What is the background for this study?
Response: This study was a true team effort. It was funded by AARP and AARP Services, INC and the research was a collaboration of representatives from Johns Hopkins University, OptumLabs, University of California – San Francisco, and AARP Services, INC. Given all of the resent research on downstream effects of hearing loss on important health outcomes such as cognitive decline, falls, and dementia, the aim was to explore how persons with hearing loss interacted with the healthcare system in terms of cost and utilization.
MedicalResearch.com: What are the main findings?
Response: Over a 10 year period, untreated hearing loss (hearing aid users were excluded from this study as they are difficult to capture in the claims database) was associated with higher healthcare spending and utilization. Specifically, over 10 years, persons with untreated hearing loss spent 46.5% more, on average, on healthcare (to the tune of approximately $22000 more) than those without evidence of hearing loss. Furthermore, persons with untreated hearing loss had 44% and 17% higher risk for 30-day readmission and emergency department visit, respectively.
Similar relationships were seen across other measures where persons with untreated hearing loss were more likely to be hospitalized and spent longer in the hospital compared to those without evidence of hearing loss. 




 Dr. Yano[/caption]
Yuichiro Yano MD PhD
Assistant Professor in Community and Family Medicine
Duke University
MedicalResearch.com: What is the background for this study?
Response: New blood pressure guidelines, issued in 2017 in the US, lowered the blood pressure thresholds for hypertension from systolic blood pressure/diastolic ≥140/90 mm Hg to systolic/diastolic ≥130/80 mm Hg. This change increased the prevalence of hypertension two- to three-fold among young adults. The guidelines also newly defined elevated blood pressure as, 120-129 mmHg systolic blood pressure over 80 mmHg diastolic or less. However, no study investigated that high blood pressure, as defined by the new criteria, is something that younger people should be concerned about as a potential precursor to serious problems.
Our study is among the first to report that people younger than age 40 who have elevated blood pressure or hypertension are at increased risk of heart failure, strokes and blood vessel blockages as they age.
Dr. Yano[/caption]
Yuichiro Yano MD PhD
Assistant Professor in Community and Family Medicine
Duke University
MedicalResearch.com: What is the background for this study?
Response: New blood pressure guidelines, issued in 2017 in the US, lowered the blood pressure thresholds for hypertension from systolic blood pressure/diastolic ≥140/90 mm Hg to systolic/diastolic ≥130/80 mm Hg. This change increased the prevalence of hypertension two- to three-fold among young adults. The guidelines also newly defined elevated blood pressure as, 120-129 mmHg systolic blood pressure over 80 mmHg diastolic or less. However, no study investigated that high blood pressure, as defined by the new criteria, is something that younger people should be concerned about as a potential precursor to serious problems.
Our study is among the first to report that people younger than age 40 who have elevated blood pressure or hypertension are at increased risk of heart failure, strokes and blood vessel blockages as they age.










 Dr. Wanpen Vongpatanasin, M.D.
Professor of Medicine
Program Director, Hypertension Fellowship Program
UT Southwestern Medical Center in Dallas
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The new US hypertension guideline places a greater emphasis on out-of-office blood pressure measurement, and maintains that a clinic BP of 130/80 mm Hg is equivalent to the same reading for home BP monitoring or daytime ambulatory BP monitoring. That is based, however, on data from non-US cohorts, primarily from Japanese cohorts and some European populations. None has been studied in the US population until now.
To find out, we analyzed large multi-ethnic studies of primarily young and middle-aged adults in Dallas, Texas, and Durham, N.C., that compared home blood pressure to clinic measurements, using the regression correlation (i.e. regression approach). To confirm the findings, we use another approach called “outcome approach” by determining risks of stroke, MI, and death associated with a clinic systolic blood pressure reading of 130 mmHg from the 3,132 participants in the Dallas study during an 11-year follow up.
Then, we determined the home blood pressure levels that carried the same heart disease risk and stroke risk as the clinic systolic 130 mm Hg reading.
We found that the level of home blood pressure of 130/80 mm Hg actually best correlates with blood pressure taken at the doctor’s office of 130/80 mmHg. This is true for whites, blacks and Hispanic patients in both treated and untreated population.
Dr. Wanpen Vongpatanasin, M.D.
Professor of Medicine
Program Director, Hypertension Fellowship Program
UT Southwestern Medical Center in Dallas
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The new US hypertension guideline places a greater emphasis on out-of-office blood pressure measurement, and maintains that a clinic BP of 130/80 mm Hg is equivalent to the same reading for home BP monitoring or daytime ambulatory BP monitoring. That is based, however, on data from non-US cohorts, primarily from Japanese cohorts and some European populations. None has been studied in the US population until now.
To find out, we analyzed large multi-ethnic studies of primarily young and middle-aged adults in Dallas, Texas, and Durham, N.C., that compared home blood pressure to clinic measurements, using the regression correlation (i.e. regression approach). To confirm the findings, we use another approach called “outcome approach” by determining risks of stroke, MI, and death associated with a clinic systolic blood pressure reading of 130 mmHg from the 3,132 participants in the Dallas study during an 11-year follow up.
Then, we determined the home blood pressure levels that carried the same heart disease risk and stroke risk as the clinic systolic 130 mm Hg reading.
We found that the level of home blood pressure of 130/80 mm Hg actually best correlates with blood pressure taken at the doctor’s office of 130/80 mmHg. This is true for whites, blacks and Hispanic patients in both treated and untreated population. 






 Faiz Gani, PhD
Postdoctoral research fellow
Department of Surgery
Johns Hopkins University School of Medicine
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Firearm related injuries are a leading cause of injury and death in the United States, yet, due to combination of factors, limited data exist that evaluate these injuries, particularly among younger patients (patients younger than 18 years).
The objective of this study was to describe emergency department utilization for firearm related injuries and to quantitate the financial burden associated with these injuries.
In our study of over 75,000 emergency department visits, we observed that each year, over 8,300 children and adolescents present to the emergency department for the treatment / management of a gunshot injury. Within this sub-population of patients, we observed that these injuries are most frequent among patients aged 15-17 years and while these injuries decreased over time initially, were observed to increase again towards the end of the time period studied.
In addition to describing the clinical burden of these injuries, we also sought to describe the financial burden associated with these injuries. For patients discharged from the emergency department, the average (median) charge associated with their care was $2,445, while for patients admitted as inpatients for further care, the average (median) charge was $44,966.
Collectively these injuries resulted in $2.5 billion in emergency department and hospital charges over the time period studied. This translates to an annual financial burden of approximately $270 million.
Faiz Gani, PhD
Postdoctoral research fellow
Department of Surgery
Johns Hopkins University School of Medicine
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Firearm related injuries are a leading cause of injury and death in the United States, yet, due to combination of factors, limited data exist that evaluate these injuries, particularly among younger patients (patients younger than 18 years).
The objective of this study was to describe emergency department utilization for firearm related injuries and to quantitate the financial burden associated with these injuries.
In our study of over 75,000 emergency department visits, we observed that each year, over 8,300 children and adolescents present to the emergency department for the treatment / management of a gunshot injury. Within this sub-population of patients, we observed that these injuries are most frequent among patients aged 15-17 years and while these injuries decreased over time initially, were observed to increase again towards the end of the time period studied.
In addition to describing the clinical burden of these injuries, we also sought to describe the financial burden associated with these injuries. For patients discharged from the emergency department, the average (median) charge associated with their care was $2,445, while for patients admitted as inpatients for further care, the average (median) charge was $44,966.
Collectively these injuries resulted in $2.5 billion in emergency department and hospital charges over the time period studied. This translates to an annual financial burden of approximately $270 million.