Author Interviews, Breast Cancer, Cancer Research, JAMA, Leukemia / 21.01.2019
Breast Cancer Survivors More Likely To Develop Subsequent Blood Cancers
MedicalResearch.com Interview with:
 Dr. Marie Joelle Jabagi, PharmD, MPH
University of Paris Sud, Paris-Saclay University, Paris
Health Product Epidemiology Department
French National Agency for Medicines and Health Products Safety
Saint-Denis, France
MedicalResearch.com: What is the background for this study?
Response: Secondary hematologic malignant neoplasms that develop months or years after the diagnosis of breast cancer may be a consequence of genetic predisposition, environmental factors, previous cancer treatments or a combination of all those factors. These secondary malignant neoplasms are increasingly becoming a concern given that the population of breast cancer survivors is growing substantially. However, their frequency in real life has been poorly investigated to date.
The aims of our research were to estimate the frequency of various types of hematologic malignant neoplasm following a diagnosis of primary breast cancer among women aged 20 to 85 years in France during the past decade, and to compare it to the corresponding frequency in women of the French general population.
Dr. Marie Joelle Jabagi, PharmD, MPH
University of Paris Sud, Paris-Saclay University, Paris
Health Product Epidemiology Department
French National Agency for Medicines and Health Products Safety
Saint-Denis, France
MedicalResearch.com: What is the background for this study?
Response: Secondary hematologic malignant neoplasms that develop months or years after the diagnosis of breast cancer may be a consequence of genetic predisposition, environmental factors, previous cancer treatments or a combination of all those factors. These secondary malignant neoplasms are increasingly becoming a concern given that the population of breast cancer survivors is growing substantially. However, their frequency in real life has been poorly investigated to date.
The aims of our research were to estimate the frequency of various types of hematologic malignant neoplasm following a diagnosis of primary breast cancer among women aged 20 to 85 years in France during the past decade, and to compare it to the corresponding frequency in women of the French general population.
 Dr. Marie Joelle Jabagi, PharmD, MPH
University of Paris Sud, Paris-Saclay University, Paris
Health Product Epidemiology Department
French National Agency for Medicines and Health Products Safety
Saint-Denis, France
MedicalResearch.com: What is the background for this study?
Response: Secondary hematologic malignant neoplasms that develop months or years after the diagnosis of breast cancer may be a consequence of genetic predisposition, environmental factors, previous cancer treatments or a combination of all those factors. These secondary malignant neoplasms are increasingly becoming a concern given that the population of breast cancer survivors is growing substantially. However, their frequency in real life has been poorly investigated to date.
The aims of our research were to estimate the frequency of various types of hematologic malignant neoplasm following a diagnosis of primary breast cancer among women aged 20 to 85 years in France during the past decade, and to compare it to the corresponding frequency in women of the French general population.
Dr. Marie Joelle Jabagi, PharmD, MPH
University of Paris Sud, Paris-Saclay University, Paris
Health Product Epidemiology Department
French National Agency for Medicines and Health Products Safety
Saint-Denis, France
MedicalResearch.com: What is the background for this study?
Response: Secondary hematologic malignant neoplasms that develop months or years after the diagnosis of breast cancer may be a consequence of genetic predisposition, environmental factors, previous cancer treatments or a combination of all those factors. These secondary malignant neoplasms are increasingly becoming a concern given that the population of breast cancer survivors is growing substantially. However, their frequency in real life has been poorly investigated to date.
The aims of our research were to estimate the frequency of various types of hematologic malignant neoplasm following a diagnosis of primary breast cancer among women aged 20 to 85 years in France during the past decade, and to compare it to the corresponding frequency in women of the French general population.



 Dr. Vallerand[/caption]
Isabelle Vallerand, PhD
Epidemiologist, MD Student
Department of Community Health Sciences
Cumming School of Medicine
University of Calgary
MedicalResearch.com: What is the background for this study? What are the main findings?
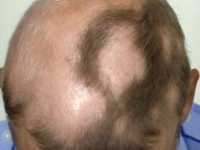
Response: It is well known that patients with alopecia areata, a form of autoimmune hair loss, are at a higher risk of suffering from depression than the general population. But in practice, we often hear patients tell us that they believe their hair loss developed as a result of stress or problems with mental health – certainly the phrase “so stressed your hair is falling out” is something most people have heard of. Despite this, there has actually been very little research investigating the role that mental health may have on development of alopecia areata.
Interestingly, depression has recently been associated with increased systemic inflammatory markers, so there is biologic plausibility that depression could increase the risk of alopecia areata. Our group was interested in addressing this question, and used a large population-level health records database with up to 26 years of follow-up to study it. We ultimately found that not only does depression increase one’s risk of alopecia areata, but that it increases their risk by nearly 90% compared to people who have never had depression. We also found that using antidepressants can significantly decrease the risk of developing alopecia areata in patients with depression. So there appears to be an important link between mental health and development of hair loss from alopecia areata.
Dr. Vallerand[/caption]
Isabelle Vallerand, PhD
Epidemiologist, MD Student
Department of Community Health Sciences
Cumming School of Medicine
University of Calgary
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: It is well known that patients with alopecia areata, a form of autoimmune hair loss, are at a higher risk of suffering from depression than the general population. But in practice, we often hear patients tell us that they believe their hair loss developed as a result of stress or problems with mental health – certainly the phrase “so stressed your hair is falling out” is something most people have heard of. Despite this, there has actually been very little research investigating the role that mental health may have on development of alopecia areata.
Interestingly, depression has recently been associated with increased systemic inflammatory markers, so there is biologic plausibility that depression could increase the risk of alopecia areata. Our group was interested in addressing this question, and used a large population-level health records database with up to 26 years of follow-up to study it. We ultimately found that not only does depression increase one’s risk of alopecia areata, but that it increases their risk by nearly 90% compared to people who have never had depression. We also found that using antidepressants can significantly decrease the risk of developing alopecia areata in patients with depression. So there appears to be an important link between mental health and development of hair loss from alopecia areata.




 Dr. Shenoy[/caption]
ESS= Erica S. Shenoy, MD, PhD
Harvard Medical School
Division of Infectious Diseases, Department of Medicine
Massachusetts General Hospital, Boston
[caption id="attachment_47011" align="alignleft" width="150"]
Dr. Shenoy[/caption]
ESS= Erica S. Shenoy, MD, PhD
Harvard Medical School
Division of Infectious Diseases, Department of Medicine
Massachusetts General Hospital, Boston
[caption id="attachment_47011" align="alignleft" width="150"] Dr. Blumenthal[/caption]
KGB= Kimberly G. Blumenthal MD, MSc
Division of Rheumatology, Allergy and Immunology
Department of Medicine, Massachusetts General Hospital,Boston
[caption id="attachment_47012" align="alignleft" width="100"]
Dr. Blumenthal[/caption]
KGB= Kimberly G. Blumenthal MD, MSc
Division of Rheumatology, Allergy and Immunology
Department of Medicine, Massachusetts General Hospital,Boston
[caption id="attachment_47012" align="alignleft" width="100"] Dr. Macy[/caption]
EMM= Eric M. Macy MD, MS
Department of Allergy
Southern California Permanente Medical Group
San Diego Medical Center
[caption id="attachment_47013" align="alignleft" width="150"]
Dr. Macy[/caption]
EMM= Eric M. Macy MD, MS
Department of Allergy
Southern California Permanente Medical Group
San Diego Medical Center
[caption id="attachment_47013" align="alignleft" width="150"] Dr. Rowe[/caption]
TR= Theresa Rowe, DO, MS
General Internal Medicine and Geriatrics
Feinberg School of Medicine
Northwestern University, Chicago, Illinois
MedicalResearch.com: What is the background for this review?
ESS: A key component of reducing antimicrobial resistance is improving how antimicrobials are prescribed—both reducing inappropriate use (i.e., not prescribing when not needed) and favoring the use of narrow-spectrum agents that are less likely to contribute to the development of antimicrobial resistance.
KGB: Because unverified penicillin allergy labels are so prevalent with greater than 32 million Americans affected, and these labels lead to the use of alternative antibiotics that are often more broad-spectrum, we now know that penicillin allergy evaluations are an emerging important component of antibiotic stewardship. When patients with a reported penicillin allergy are tested, more than 95% of them are not allergic, and thus could (and should) receive penicillins, and often related drugs, when appropriate.
Dr. Rowe[/caption]
TR= Theresa Rowe, DO, MS
General Internal Medicine and Geriatrics
Feinberg School of Medicine
Northwestern University, Chicago, Illinois
MedicalResearch.com: What is the background for this review?
ESS: A key component of reducing antimicrobial resistance is improving how antimicrobials are prescribed—both reducing inappropriate use (i.e., not prescribing when not needed) and favoring the use of narrow-spectrum agents that are less likely to contribute to the development of antimicrobial resistance.
KGB: Because unverified penicillin allergy labels are so prevalent with greater than 32 million Americans affected, and these labels lead to the use of alternative antibiotics that are often more broad-spectrum, we now know that penicillin allergy evaluations are an emerging important component of antibiotic stewardship. When patients with a reported penicillin allergy are tested, more than 95% of them are not allergic, and thus could (and should) receive penicillins, and often related drugs, when appropriate.


 Dr. Sehested[/caption]
Thomas S. G. Sehested MD
Department of Cardiology
Copenhagen University Hospital Gentofte
[caption id="attachment_46991" align="alignleft" width="150"]
Dr. Sehested[/caption]
Thomas S. G. Sehested MD
Department of Cardiology
Copenhagen University Hospital Gentofte
[caption id="attachment_46991" align="alignleft" width="150"]






 Dr. Longo[/caption]
Valter Longo, PhD
Edna M. Jones Professor of Gerontology
Professor of Biological Sciences
Leonard Davis School of Gerontology
Director of the USC Longevity Institute
USC
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The use of a low calorie diet that mimics fasting for 4 days twice a month starting at middle age can extend lifespan and rejuvenate mice.
In humans a similar diet once a month causes improvements in cholesterol, blood pressure , inflammation, fasting glucose etc consistent with rejuvenation
Dr. Longo[/caption]
Valter Longo, PhD
Edna M. Jones Professor of Gerontology
Professor of Biological Sciences
Leonard Davis School of Gerontology
Director of the USC Longevity Institute
USC
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The use of a low calorie diet that mimics fasting for 4 days twice a month starting at middle age can extend lifespan and rejuvenate mice.
In humans a similar diet once a month causes improvements in cholesterol, blood pressure , inflammation, fasting glucose etc consistent with rejuvenation








 Dr. Leas[/caption]
Eric Leas PhD, MPH
Stanford Prevention Research Center
University of California, San Diego
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Recent research has demonstrated the importance that neighborhood context has on life opportunity, health and well-being that can perpetuate across generations. A strongly defining factor that leads to differences in health outcomes across neighborhoods, such as differences in chronic disease, is the concurrent-uneven distribution of modifiable risk factors for chronic disease.
The main goal of our study was to characterize inequities in smoking, the leading risk factor for chronic disease, between neighborhoods in America's 500 largest cities. To accomplish this aim we used first-of-its-kind data generated from the 500 Cities Project—a collaboration between Robert Wood Johnson Foundation and the US Centers for Disease Control and Prevention—representing the largest effort to provide small-area estimates of modifiable risk factors for chronic disease.
We found that inequities in smoking prevalence are greater within cities than between cities, are highest in the nation’s capital, and are linked to inequities in chronic disease outcomes. We also found that inequities in smoking were associated to inequities in neighborhood characteristics, including race, median household income and the number of tobacco retailers.
Dr. Leas[/caption]
Eric Leas PhD, MPH
Stanford Prevention Research Center
University of California, San Diego
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Recent research has demonstrated the importance that neighborhood context has on life opportunity, health and well-being that can perpetuate across generations. A strongly defining factor that leads to differences in health outcomes across neighborhoods, such as differences in chronic disease, is the concurrent-uneven distribution of modifiable risk factors for chronic disease.
The main goal of our study was to characterize inequities in smoking, the leading risk factor for chronic disease, between neighborhoods in America's 500 largest cities. To accomplish this aim we used first-of-its-kind data generated from the 500 Cities Project—a collaboration between Robert Wood Johnson Foundation and the US Centers for Disease Control and Prevention—representing the largest effort to provide small-area estimates of modifiable risk factors for chronic disease.
We found that inequities in smoking prevalence are greater within cities than between cities, are highest in the nation’s capital, and are linked to inequities in chronic disease outcomes. We also found that inequities in smoking were associated to inequities in neighborhood characteristics, including race, median household income and the number of tobacco retailers.



