Author Interviews, Biomarkers, Infections, JAMA, Stanford / 29.10.2018
Gene Signature Blood Test Can Diagnose TB and Treatment Response
MedicalResearch.com Interview with:
 Purvesh Khatri, Ph.D.
Associate Professor
Stanford Institute for Immunity, Transplantation and Infection (ITI)
Stanford Center for Biomedical Informatics Research (BMIR)
Department of Medicine
Stanford University
Stanford, CA 94305
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: We have previously described a 3-gene signature for distinguishing patients with active tuberculosis (ATB) from those with other diseases, latent mycobacterium tuberculosis (LTB) infection, and healthy controls (Sweeney et al. Lancet Respir Med 2016).
The current study in JAMA Network Open is a follow up study to validate the 3-gene signature in 3 additional independent cohorts that were prospectively collected.
Using these 3 cohorts we have now showed that the 3-gene signature
(1) can identify patients with LTB that will progress to ATB about 6 months prior to diagnosis of active tuberculosis.
(2) can identify patients with ATB in active screening, and
(3) can identify patients with ATB at diagnosis that have higher likelihood of persistent lung inflammation due to subclinical ATB at the end of treatment.
Purvesh Khatri, Ph.D.
Associate Professor
Stanford Institute for Immunity, Transplantation and Infection (ITI)
Stanford Center for Biomedical Informatics Research (BMIR)
Department of Medicine
Stanford University
Stanford, CA 94305
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: We have previously described a 3-gene signature for distinguishing patients with active tuberculosis (ATB) from those with other diseases, latent mycobacterium tuberculosis (LTB) infection, and healthy controls (Sweeney et al. Lancet Respir Med 2016).
The current study in JAMA Network Open is a follow up study to validate the 3-gene signature in 3 additional independent cohorts that were prospectively collected.
Using these 3 cohorts we have now showed that the 3-gene signature
(1) can identify patients with LTB that will progress to ATB about 6 months prior to diagnosis of active tuberculosis.
(2) can identify patients with ATB in active screening, and
(3) can identify patients with ATB at diagnosis that have higher likelihood of persistent lung inflammation due to subclinical ATB at the end of treatment.
 Purvesh Khatri, Ph.D.
Associate Professor
Stanford Institute for Immunity, Transplantation and Infection (ITI)
Stanford Center for Biomedical Informatics Research (BMIR)
Department of Medicine
Stanford University
Stanford, CA 94305
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: We have previously described a 3-gene signature for distinguishing patients with active tuberculosis (ATB) from those with other diseases, latent mycobacterium tuberculosis (LTB) infection, and healthy controls (Sweeney et al. Lancet Respir Med 2016).
The current study in JAMA Network Open is a follow up study to validate the 3-gene signature in 3 additional independent cohorts that were prospectively collected.
Using these 3 cohorts we have now showed that the 3-gene signature
(1) can identify patients with LTB that will progress to ATB about 6 months prior to diagnosis of active tuberculosis.
(2) can identify patients with ATB in active screening, and
(3) can identify patients with ATB at diagnosis that have higher likelihood of persistent lung inflammation due to subclinical ATB at the end of treatment.
Purvesh Khatri, Ph.D.
Associate Professor
Stanford Institute for Immunity, Transplantation and Infection (ITI)
Stanford Center for Biomedical Informatics Research (BMIR)
Department of Medicine
Stanford University
Stanford, CA 94305
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: We have previously described a 3-gene signature for distinguishing patients with active tuberculosis (ATB) from those with other diseases, latent mycobacterium tuberculosis (LTB) infection, and healthy controls (Sweeney et al. Lancet Respir Med 2016).
The current study in JAMA Network Open is a follow up study to validate the 3-gene signature in 3 additional independent cohorts that were prospectively collected.
Using these 3 cohorts we have now showed that the 3-gene signature
(1) can identify patients with LTB that will progress to ATB about 6 months prior to diagnosis of active tuberculosis.
(2) can identify patients with ATB in active screening, and
(3) can identify patients with ATB at diagnosis that have higher likelihood of persistent lung inflammation due to subclinical ATB at the end of treatment. 

 Dipender Gill[/caption]
Dipender Gill
Imperial College Healthcare NHS Trust
London, United Kingdon
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Iron status has previously been associated with risk of various types of cardiovascular disease, including stroke. However, the observational research methodologies that identified these associations can be affected by confounding from environmental factors and reverse causation.
We used randomly allocated genetic variants that affect iron status to investigate its effect on risk of different types of ischemic stroke, and found evidence to support that higher iron status increases risk of cardioembolic stroke.
Dipender Gill[/caption]
Dipender Gill
Imperial College Healthcare NHS Trust
London, United Kingdon
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Iron status has previously been associated with risk of various types of cardiovascular disease, including stroke. However, the observational research methodologies that identified these associations can be affected by confounding from environmental factors and reverse causation.
We used randomly allocated genetic variants that affect iron status to investigate its effect on risk of different types of ischemic stroke, and found evidence to support that higher iron status increases risk of cardioembolic stroke.


 Dr. Epling[/caption]
John W. Epling, Jr., M.D., M.S.Ed
Professor of Family and Community Medicine
Virginia Tech Carilion School of Medicine
Roanoke, VA
USPSTF Task Force Member
MedicalResearch.com: What is the background for this study?
Response: Intimate partner violence, often known as domestic violence, can have devastating consequences to one’s health and wellbeing. It can lead to mental illness, substance abuse, unintended pregnancy, and even death. This is a serious public health issue in America: one in three men—and even more women—experience it in their lifetimes. Because this is such an important topic, and the last time we made a recommendation on it was in 2013, the U.S. Preventive Services Task Force reviewed the most recent evidence to determine how clinicians can help prevent the negative health effects of intimate partner violence.
Dr. Epling[/caption]
John W. Epling, Jr., M.D., M.S.Ed
Professor of Family and Community Medicine
Virginia Tech Carilion School of Medicine
Roanoke, VA
USPSTF Task Force Member
MedicalResearch.com: What is the background for this study?
Response: Intimate partner violence, often known as domestic violence, can have devastating consequences to one’s health and wellbeing. It can lead to mental illness, substance abuse, unintended pregnancy, and even death. This is a serious public health issue in America: one in three men—and even more women—experience it in their lifetimes. Because this is such an important topic, and the last time we made a recommendation on it was in 2013, the U.S. Preventive Services Task Force reviewed the most recent evidence to determine how clinicians can help prevent the negative health effects of intimate partner violence.


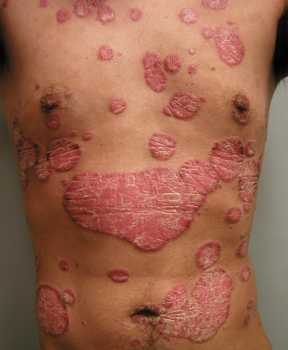
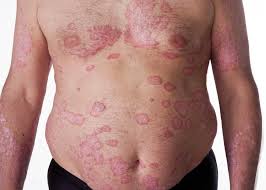 Psoriasis[/caption]
Prof Ching-Chi Chi, MD, MMS, DPhil
Department of Dermatology
Chang Gung Memorial Hospital, Linkou
Guishan Dist, Taoyuan
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Previous studies have shown common genotypes, clinical course, and immunological features shared by psoriasis and inflammatory bowel disease.
However, the relationship between psoriasis and inflammatory bowel disease was largely unclear.
In this study, we found when compared to the general population, psoriatic patients are more likely to have concomitant inflammatory bowel disease.
Psoriasis[/caption]
Prof Ching-Chi Chi, MD, MMS, DPhil
Department of Dermatology
Chang Gung Memorial Hospital, Linkou
Guishan Dist, Taoyuan
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Previous studies have shown common genotypes, clinical course, and immunological features shared by psoriasis and inflammatory bowel disease.
However, the relationship between psoriasis and inflammatory bowel disease was largely unclear.
In this study, we found when compared to the general population, psoriatic patients are more likely to have concomitant inflammatory bowel disease. 








 Dr. Shlipak[/caption]
Michael G. Shlipak, MD, MPH
Scientific Director , Kidney Health Research Collaborative (
Dr. Shlipak[/caption]
Michael G. Shlipak, MD, MPH
Scientific Director , Kidney Health Research Collaborative (










 Dr. Nicole Karcher, PhD
Post-doctoral scholar with the NIMH Training in Clinical Sciences fellowship
Department of Psychiatry
Washington University School of Medicine
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: For over fifteen years, researchers have debated the role that cannabis use plays in the development of both psychotic disorders as well as subthreshold psychotic symptoms, such as psychotic-like experiences (PLEs). There is still a lack of consensus regarding the nature of the association between cannabis use and psychosis risk, with some research finding evidence for genetic overlap, while other research finds evidence for potentially causal pathways.
The current study examined data from twins and siblings from two different samples, the U.S.-based Human Connectome Project and the Australian Twin Registry, with a total of 4,674 participants. Overall, psychotic-like experiences were associated with three separate cannabis use variables [frequent (≥100 times) use, a Cannabis Use Disorder diagnosis, and current cannabis use]. Furthermore, the current research found evidence for both shared genetic and individual-specific contributions to the association between PLEs and these three cannabis use variables. More specifically, while the association between cannabis use and psychotic-like experiences was largely attributable to shared genetic factors, cannabis users were more likely to endorse PLEs in comparison to the relative who used cannabis less.
Dr. Nicole Karcher, PhD
Post-doctoral scholar with the NIMH Training in Clinical Sciences fellowship
Department of Psychiatry
Washington University School of Medicine
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: For over fifteen years, researchers have debated the role that cannabis use plays in the development of both psychotic disorders as well as subthreshold psychotic symptoms, such as psychotic-like experiences (PLEs). There is still a lack of consensus regarding the nature of the association between cannabis use and psychosis risk, with some research finding evidence for genetic overlap, while other research finds evidence for potentially causal pathways.
The current study examined data from twins and siblings from two different samples, the U.S.-based Human Connectome Project and the Australian Twin Registry, with a total of 4,674 participants. Overall, psychotic-like experiences were associated with three separate cannabis use variables [frequent (≥100 times) use, a Cannabis Use Disorder diagnosis, and current cannabis use]. Furthermore, the current research found evidence for both shared genetic and individual-specific contributions to the association between PLEs and these three cannabis use variables. More specifically, while the association between cannabis use and psychotic-like experiences was largely attributable to shared genetic factors, cannabis users were more likely to endorse PLEs in comparison to the relative who used cannabis less.