Author Interviews, Brigham & Women's - Harvard, Heart Disease, JAMA, Mediterranean Diet, Women's Heart Health / 10.12.2018
Mediterranean Diet Linked to Lower Long-Term Cardiovascular Events in Women
MedicalResearch.com Interview with:
[caption id="attachment_46414" align="alignleft" width="117"] Dr. Mora[/caption]
Samia Mora, MD, MHS
Associate Professor of Medicine
Harvard Medical School
Director, Center for Lipid Metabolomics
Brigham and Women’s Hospital
Boston, MA
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The Mediterranean diet is rich in plants (nuts, seeds, fruits, vegetables, whole grains, legumes) and olive oil, and includes moderate intake of fish, poultry, dairy, and eggs, and alcohol, and rare use of meats and sweets.The Mediterranean diet has been associated with lower risk of cardiovascular disease (CVD) events but the precise mechanisms through which Mediterranean diet intake may reduce long-term risk of CVD are not well understood. We aimed to investigate the biological mechanisms that may mediate this cardiovascular benefit.
Using a prospective study of 25,994 initially healthy women enrolled in the Women’s Health Study who were followed up to 12-years, we evaluated potential mediating effects of a panel of biomarkers (in total 40 biomarkers) that represent different CVD pathways and clinical factors.
Higher baseline intake of a Mediterranean-type diet was associated with approximately one quarter lower risk of CVD events during the 12 year follow up. For the MED-CVD risk reduction, biomarkers of inflammation, glucose-metabolism/insulin-resistance, and adiposity contributed most to explaining the association, with additional contributions from pathways related to blood pressure, lipids – in particular HDL or triglyceride-rich lipoprotein metabolism, and to a lesser extent LDL cholesterol, branched chain amino acids, and small molecule metabolites.
Dr. Mora[/caption]
Samia Mora, MD, MHS
Associate Professor of Medicine
Harvard Medical School
Director, Center for Lipid Metabolomics
Brigham and Women’s Hospital
Boston, MA
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The Mediterranean diet is rich in plants (nuts, seeds, fruits, vegetables, whole grains, legumes) and olive oil, and includes moderate intake of fish, poultry, dairy, and eggs, and alcohol, and rare use of meats and sweets.The Mediterranean diet has been associated with lower risk of cardiovascular disease (CVD) events but the precise mechanisms through which Mediterranean diet intake may reduce long-term risk of CVD are not well understood. We aimed to investigate the biological mechanisms that may mediate this cardiovascular benefit.
Using a prospective study of 25,994 initially healthy women enrolled in the Women’s Health Study who were followed up to 12-years, we evaluated potential mediating effects of a panel of biomarkers (in total 40 biomarkers) that represent different CVD pathways and clinical factors.
Higher baseline intake of a Mediterranean-type diet was associated with approximately one quarter lower risk of CVD events during the 12 year follow up. For the MED-CVD risk reduction, biomarkers of inflammation, glucose-metabolism/insulin-resistance, and adiposity contributed most to explaining the association, with additional contributions from pathways related to blood pressure, lipids – in particular HDL or triglyceride-rich lipoprotein metabolism, and to a lesser extent LDL cholesterol, branched chain amino acids, and small molecule metabolites.
 Dr. Mora[/caption]
Samia Mora, MD, MHS
Associate Professor of Medicine
Harvard Medical School
Director, Center for Lipid Metabolomics
Brigham and Women’s Hospital
Boston, MA
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The Mediterranean diet is rich in plants (nuts, seeds, fruits, vegetables, whole grains, legumes) and olive oil, and includes moderate intake of fish, poultry, dairy, and eggs, and alcohol, and rare use of meats and sweets.The Mediterranean diet has been associated with lower risk of cardiovascular disease (CVD) events but the precise mechanisms through which Mediterranean diet intake may reduce long-term risk of CVD are not well understood. We aimed to investigate the biological mechanisms that may mediate this cardiovascular benefit.
Using a prospective study of 25,994 initially healthy women enrolled in the Women’s Health Study who were followed up to 12-years, we evaluated potential mediating effects of a panel of biomarkers (in total 40 biomarkers) that represent different CVD pathways and clinical factors.
Higher baseline intake of a Mediterranean-type diet was associated with approximately one quarter lower risk of CVD events during the 12 year follow up. For the MED-CVD risk reduction, biomarkers of inflammation, glucose-metabolism/insulin-resistance, and adiposity contributed most to explaining the association, with additional contributions from pathways related to blood pressure, lipids – in particular HDL or triglyceride-rich lipoprotein metabolism, and to a lesser extent LDL cholesterol, branched chain amino acids, and small molecule metabolites.
Dr. Mora[/caption]
Samia Mora, MD, MHS
Associate Professor of Medicine
Harvard Medical School
Director, Center for Lipid Metabolomics
Brigham and Women’s Hospital
Boston, MA
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The Mediterranean diet is rich in plants (nuts, seeds, fruits, vegetables, whole grains, legumes) and olive oil, and includes moderate intake of fish, poultry, dairy, and eggs, and alcohol, and rare use of meats and sweets.The Mediterranean diet has been associated with lower risk of cardiovascular disease (CVD) events but the precise mechanisms through which Mediterranean diet intake may reduce long-term risk of CVD are not well understood. We aimed to investigate the biological mechanisms that may mediate this cardiovascular benefit.
Using a prospective study of 25,994 initially healthy women enrolled in the Women’s Health Study who were followed up to 12-years, we evaluated potential mediating effects of a panel of biomarkers (in total 40 biomarkers) that represent different CVD pathways and clinical factors.
Higher baseline intake of a Mediterranean-type diet was associated with approximately one quarter lower risk of CVD events during the 12 year follow up. For the MED-CVD risk reduction, biomarkers of inflammation, glucose-metabolism/insulin-resistance, and adiposity contributed most to explaining the association, with additional contributions from pathways related to blood pressure, lipids – in particular HDL or triglyceride-rich lipoprotein metabolism, and to a lesser extent LDL cholesterol, branched chain amino acids, and small molecule metabolites. 










 Prof. Ye[/caption]
Dr. Weimin Ye, MD MSC, PhD
Department of Medical Epidemiology and Biostatistics
Karolinska Institue
MedicalResearch.com: What is the background for this study? What are the main findings?
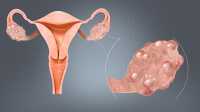
Response: Polycystic ovary syndrome (PCOS) is the most common endocrine disorder affecting 5-10% of women of reproductive age. Characterized by hyperandrogenism and metabolic abnormalities, PCOS is known to be related to various long-term health consequences, including diabetes, cardiovascular disease and endometrial cancer. Besides, inconsistent results have been reported for the associations between PCOS and the risk of ovarian and breast cancer. Studies addressing the risks of other cancers are scarce. Thus, we conducted a large, population-based cohort study with a long follow-up and rather sufficient confounding adjustment to explore the full picture of associations between PCOS and the risks of various cancer types.
We found that PCOS is a risk factor for certain types of cancer, including cancers of the endometrium, ovary, endocrine gland, pancreas, kidney and skeletal & hematopoietic system.
Prof. Ye[/caption]
Dr. Weimin Ye, MD MSC, PhD
Department of Medical Epidemiology and Biostatistics
Karolinska Institue
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Polycystic ovary syndrome (PCOS) is the most common endocrine disorder affecting 5-10% of women of reproductive age. Characterized by hyperandrogenism and metabolic abnormalities, PCOS is known to be related to various long-term health consequences, including diabetes, cardiovascular disease and endometrial cancer. Besides, inconsistent results have been reported for the associations between PCOS and the risk of ovarian and breast cancer. Studies addressing the risks of other cancers are scarce. Thus, we conducted a large, population-based cohort study with a long follow-up and rather sufficient confounding adjustment to explore the full picture of associations between PCOS and the risks of various cancer types.
We found that PCOS is a risk factor for certain types of cancer, including cancers of the endometrium, ovary, endocrine gland, pancreas, kidney and skeletal & hematopoietic system.