Author Interviews, Dermatology, Environmental Risks, JAMA, Melanoma / 15.09.2018
Clothing Patterns of Boys Compared to Girls May Explain Differences in Patterns of Mole Development
MedicalResearch.com Interview with:
[caption id="attachment_44531" align="alignleft" width="133"] Dr. Crane[/caption]
Lori A. Crane, PhD
Department of Community and Behavioral Health
Colorado School of Public Health
University of Colorado Anschutz Medical Campus,
Aurora CO
MedicalResearch.com: What is the background for this study? What are the main findings?
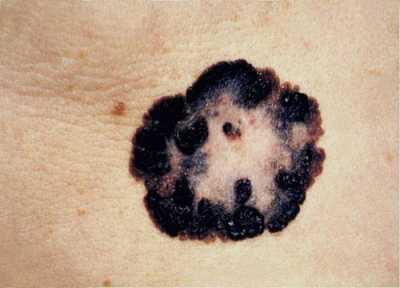
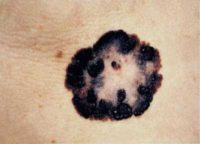
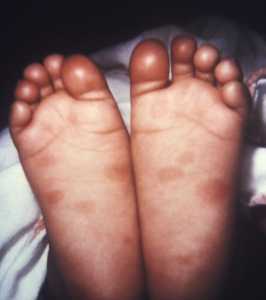
Response: Nevi, which are commonly called “moles”, are brown or black spots on the skin that are usually raised. Moles are the number one risk factor for malignant melanoma, the most dangerous kind of skin cancer. About 9,000 people die of melanoma each year in the U.S. The more moles a person has, the higher their risk for melanoma. Sun exposure is a major factor in the development of moles, and in order to prevent melanoma, it is important to better understand how moles are formed on the skin.
Most moles are formed during childhood and adolescence. We studied non-Hispanic and Hispanic white children age 3-16 and found that non-Hispanic children developed many more moles than Hispanic children. Overall, boys developed more moles than girls, but there were some important differences. For parts of the skin that are often covered by clothing but sometimes exposed to the sun, such as the chest and back, upper arms and upper legs, girls developed more moles than boys, especially among Hispanic children. In contrast, for parts of the skin that are usually exposed to the sun, such as the face, boys developed many more moles than girls. The development of moles leveled off by age 16 for parts of the skin usually exposed to the sun, while for the less often exposed skin, children continued to develop moles to age 16.
Dr. Crane[/caption]
Lori A. Crane, PhD
Department of Community and Behavioral Health
Colorado School of Public Health
University of Colorado Anschutz Medical Campus,
Aurora CO
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Nevi, which are commonly called “moles”, are brown or black spots on the skin that are usually raised. Moles are the number one risk factor for malignant melanoma, the most dangerous kind of skin cancer. About 9,000 people die of melanoma each year in the U.S. The more moles a person has, the higher their risk for melanoma. Sun exposure is a major factor in the development of moles, and in order to prevent melanoma, it is important to better understand how moles are formed on the skin.
Most moles are formed during childhood and adolescence. We studied non-Hispanic and Hispanic white children age 3-16 and found that non-Hispanic children developed many more moles than Hispanic children. Overall, boys developed more moles than girls, but there were some important differences. For parts of the skin that are often covered by clothing but sometimes exposed to the sun, such as the chest and back, upper arms and upper legs, girls developed more moles than boys, especially among Hispanic children. In contrast, for parts of the skin that are usually exposed to the sun, such as the face, boys developed many more moles than girls. The development of moles leveled off by age 16 for parts of the skin usually exposed to the sun, while for the less often exposed skin, children continued to develop moles to age 16.
 Dr. Crane[/caption]
Lori A. Crane, PhD
Department of Community and Behavioral Health
Colorado School of Public Health
University of Colorado Anschutz Medical Campus,
Aurora CO
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Nevi, which are commonly called “moles”, are brown or black spots on the skin that are usually raised. Moles are the number one risk factor for malignant melanoma, the most dangerous kind of skin cancer. About 9,000 people die of melanoma each year in the U.S. The more moles a person has, the higher their risk for melanoma. Sun exposure is a major factor in the development of moles, and in order to prevent melanoma, it is important to better understand how moles are formed on the skin.
Most moles are formed during childhood and adolescence. We studied non-Hispanic and Hispanic white children age 3-16 and found that non-Hispanic children developed many more moles than Hispanic children. Overall, boys developed more moles than girls, but there were some important differences. For parts of the skin that are often covered by clothing but sometimes exposed to the sun, such as the chest and back, upper arms and upper legs, girls developed more moles than boys, especially among Hispanic children. In contrast, for parts of the skin that are usually exposed to the sun, such as the face, boys developed many more moles than girls. The development of moles leveled off by age 16 for parts of the skin usually exposed to the sun, while for the less often exposed skin, children continued to develop moles to age 16.
Dr. Crane[/caption]
Lori A. Crane, PhD
Department of Community and Behavioral Health
Colorado School of Public Health
University of Colorado Anschutz Medical Campus,
Aurora CO
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Nevi, which are commonly called “moles”, are brown or black spots on the skin that are usually raised. Moles are the number one risk factor for malignant melanoma, the most dangerous kind of skin cancer. About 9,000 people die of melanoma each year in the U.S. The more moles a person has, the higher their risk for melanoma. Sun exposure is a major factor in the development of moles, and in order to prevent melanoma, it is important to better understand how moles are formed on the skin.
Most moles are formed during childhood and adolescence. We studied non-Hispanic and Hispanic white children age 3-16 and found that non-Hispanic children developed many more moles than Hispanic children. Overall, boys developed more moles than girls, but there were some important differences. For parts of the skin that are often covered by clothing but sometimes exposed to the sun, such as the chest and back, upper arms and upper legs, girls developed more moles than boys, especially among Hispanic children. In contrast, for parts of the skin that are usually exposed to the sun, such as the face, boys developed many more moles than girls. The development of moles leveled off by age 16 for parts of the skin usually exposed to the sun, while for the less often exposed skin, children continued to develop moles to age 16.