Author Interviews, Heart Disease, JAMA, Lifestyle & Health, USPSTF / 03.12.2020
USPSTF: Behavioral Counseling Recommended For Patients at Risk of Cardiovascular Disease
MedicalResearch.com Interview with:
[caption id="attachment_56105" align="alignleft" width="133"] Dr. Epling[/caption]
Dr. John Epling, M.D., M.S.Ed
Professor of family and community medicine
Virginia Tech Carilion School of Medicine in Roanoke, VA.
Medical director of research for family and community medicine
Medical director of employee health and wellness for the Carilion Clinic
Dr. Epling joined the U.S. Preventive Services Task Force in January 2016.
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Cardiovascular disease, which includes heart disease and stroke, is one of the leading causes of death in the United States. Nearly half of all adults have at least one risk factor for cardiovascular disease. Evidence shows that counseling aimed at helping people improve their diet and increase their physical activity can help prevent cardiovascular disease. This typically involves a trained counselor who provides education, helps people set goals, shares strategies, and stays in regular contact.
The Task Force recommends behavioral counseling interventions that promote a healthy diet and physical activity to help people at risk for cardiovascular disease stay healthy.
Dr. Epling[/caption]
Dr. John Epling, M.D., M.S.Ed
Professor of family and community medicine
Virginia Tech Carilion School of Medicine in Roanoke, VA.
Medical director of research for family and community medicine
Medical director of employee health and wellness for the Carilion Clinic
Dr. Epling joined the U.S. Preventive Services Task Force in January 2016.
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Cardiovascular disease, which includes heart disease and stroke, is one of the leading causes of death in the United States. Nearly half of all adults have at least one risk factor for cardiovascular disease. Evidence shows that counseling aimed at helping people improve their diet and increase their physical activity can help prevent cardiovascular disease. This typically involves a trained counselor who provides education, helps people set goals, shares strategies, and stays in regular contact.
The Task Force recommends behavioral counseling interventions that promote a healthy diet and physical activity to help people at risk for cardiovascular disease stay healthy.
 Dr. Epling[/caption]
Dr. John Epling, M.D., M.S.Ed
Professor of family and community medicine
Virginia Tech Carilion School of Medicine in Roanoke, VA.
Medical director of research for family and community medicine
Medical director of employee health and wellness for the Carilion Clinic
Dr. Epling joined the U.S. Preventive Services Task Force in January 2016.
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Cardiovascular disease, which includes heart disease and stroke, is one of the leading causes of death in the United States. Nearly half of all adults have at least one risk factor for cardiovascular disease. Evidence shows that counseling aimed at helping people improve their diet and increase their physical activity can help prevent cardiovascular disease. This typically involves a trained counselor who provides education, helps people set goals, shares strategies, and stays in regular contact.
The Task Force recommends behavioral counseling interventions that promote a healthy diet and physical activity to help people at risk for cardiovascular disease stay healthy.
Dr. Epling[/caption]
Dr. John Epling, M.D., M.S.Ed
Professor of family and community medicine
Virginia Tech Carilion School of Medicine in Roanoke, VA.
Medical director of research for family and community medicine
Medical director of employee health and wellness for the Carilion Clinic
Dr. Epling joined the U.S. Preventive Services Task Force in January 2016.
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Cardiovascular disease, which includes heart disease and stroke, is one of the leading causes of death in the United States. Nearly half of all adults have at least one risk factor for cardiovascular disease. Evidence shows that counseling aimed at helping people improve their diet and increase their physical activity can help prevent cardiovascular disease. This typically involves a trained counselor who provides education, helps people set goals, shares strategies, and stays in regular contact.
The Task Force recommends behavioral counseling interventions that promote a healthy diet and physical activity to help people at risk for cardiovascular disease stay healthy.





 Dr. Flaherty[/caption]
Michael R. Flaherty, DO
Attending, Pediatric Critical Care Medicine
Co-Director, Trauma and Injury Prevention Outreach Program, MGH
Instructor in Pediatrics,
Harvard Medical School
Boston, MA 02114
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: This study was a joint collaboration between Massachusetts General Hospital and Boston Children’s Hospital. The Consumer Product Safety Commission (CPSC) found an increasing incidence of rare earth magnet ingestions by children causing serious injury; Injuries are particularly serious when a child ingests two of these small magnets, or a magnet with another metal object – this can lead to bowel walls becoming attached and kinked, leading to catastrophic bowel injury and/or death.
The Consumer Product Safety Commission initiated campaigns to limit sales in 2012 with voluntary recalls and safety standards, as well as public awareness campaigns, legislative advocacy, and lawsuits. In October 2014, the CPSC published their final rule, “Safety Standard for Magnet Sets,” which prohibited the sale of magnets based on a pre-specified size and power scale, essentially eliminating the ability to sell SREMs. This rule was appealed by largest manufacturer of these magnets, Zen Magnets, LLC., and in November 2016 this rule was legally reversed by the U.S. Court of Appeals Tenth Circuit resulting in a resurgence of these magnets on the market.
Dr. Flaherty[/caption]
Michael R. Flaherty, DO
Attending, Pediatric Critical Care Medicine
Co-Director, Trauma and Injury Prevention Outreach Program, MGH
Instructor in Pediatrics,
Harvard Medical School
Boston, MA 02114
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: This study was a joint collaboration between Massachusetts General Hospital and Boston Children’s Hospital. The Consumer Product Safety Commission (CPSC) found an increasing incidence of rare earth magnet ingestions by children causing serious injury; Injuries are particularly serious when a child ingests two of these small magnets, or a magnet with another metal object – this can lead to bowel walls becoming attached and kinked, leading to catastrophic bowel injury and/or death.
The Consumer Product Safety Commission initiated campaigns to limit sales in 2012 with voluntary recalls and safety standards, as well as public awareness campaigns, legislative advocacy, and lawsuits. In October 2014, the CPSC published their final rule, “Safety Standard for Magnet Sets,” which prohibited the sale of magnets based on a pre-specified size and power scale, essentially eliminating the ability to sell SREMs. This rule was appealed by largest manufacturer of these magnets, Zen Magnets, LLC., and in November 2016 this rule was legally reversed by the U.S. Court of Appeals Tenth Circuit resulting in a resurgence of these magnets on the market.






 Prof. Pottel[/caption]
Prof. Dr. Hans Pottel PhD
Professeur Invité (titre honorifique)
Faculté de Médecine
Université de Liège
KULeuven-KULAK, Kortrijk, Belgium
MedicalResearch.com: What is the background for this study? Why do we need a new GFR?
Response: The currently recommended equations have flaws, mainly because there is one equation (CKiD) recommended for children, and one recommended (CKD-EPI) for adults (by KDIGO). When transitioning from pediatric nephrology care to adult nephrology care, the switch from CKiD to CKD-EPI causes implausible jumps (of more than 50%), mainly because CKD-EPI largely overestimates GFR in young adults (18-30 years). The new equation overcomes this problem as it applies for all ages (for children and adults) and overcomes the known flaws of the currently most used equations. The new equation is less biased and more precise across the full age spectrum and for the full range of serum creatinine concentrations.
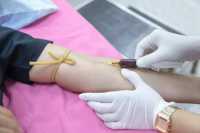
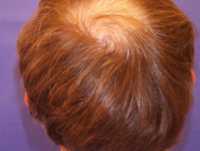
The equation was developed in 11 251 participants from 7 cohorts (development and internal validation datasets) and validated in 8 378 participants from 6 cohorts (external validation dataset). Data were coming from European and American nephrology centers. No patients of African-American ancestry were included. Actually, the previously published FAS-equation served as the basic mathematical form for the equation, but we adjusted the power coefficients for serum creatinine (very much like it was done in the CKD-EPI equation). You could say that we used properties of both the FAS and CKD-EPI equation to come to an improved equation to estimate GFR.
Prof. Pottel[/caption]
Prof. Dr. Hans Pottel PhD
Professeur Invité (titre honorifique)
Faculté de Médecine
Université de Liège
KULeuven-KULAK, Kortrijk, Belgium
MedicalResearch.com: What is the background for this study? Why do we need a new GFR?
Response: The currently recommended equations have flaws, mainly because there is one equation (CKiD) recommended for children, and one recommended (CKD-EPI) for adults (by KDIGO). When transitioning from pediatric nephrology care to adult nephrology care, the switch from CKiD to CKD-EPI causes implausible jumps (of more than 50%), mainly because CKD-EPI largely overestimates GFR in young adults (18-30 years). The new equation overcomes this problem as it applies for all ages (for children and adults) and overcomes the known flaws of the currently most used equations. The new equation is less biased and more precise across the full age spectrum and for the full range of serum creatinine concentrations.
The equation was developed in 11 251 participants from 7 cohorts (development and internal validation datasets) and validated in 8 378 participants from 6 cohorts (external validation dataset). Data were coming from European and American nephrology centers. No patients of African-American ancestry were included. Actually, the previously published FAS-equation served as the basic mathematical form for the equation, but we adjusted the power coefficients for serum creatinine (very much like it was done in the CKD-EPI equation). You could say that we used properties of both the FAS and CKD-EPI equation to come to an improved equation to estimate GFR.

 Prof Jeffrey S Tobias, Prof Jayant S Vaidya, Prof Max Bulsara. and Prof Michael Baum[/caption]
Response: The findings of the large international randomised trial (TARGIT-A trial), published in the British Medical Journal (
Prof Jeffrey S Tobias, Prof Jayant S Vaidya, Prof Max Bulsara. and Prof Michael Baum[/caption]
Response: The findings of the large international randomised trial (TARGIT-A trial), published in the British Medical Journal (
 Dr. Spann[/caption]
Marisa N. Spann, PhD, MPH
Columbia University Irving Medical Center
New York, New York
MedicalResearch.com: What is the background for this study?
Response: Prior research has demonstrated that higher maternal pre-pregnancy body mass index is associated with adverse long-term outcomes for offspring including obesity, poorer cognitive and social abilities, and increased risk of psychiatric disorders.
MedicalResearch.com: What are the main findings?
Response: In this study, we investigated the association of maternal pre-pregnancy body mass index with fetal growth and neonatal functional connectivity and found that maternal pre-pregnancy BMI has a significant positive correlation with fetal weight and with greater thalamic connectivity of the brain.
Dr. Spann[/caption]
Marisa N. Spann, PhD, MPH
Columbia University Irving Medical Center
New York, New York
MedicalResearch.com: What is the background for this study?
Response: Prior research has demonstrated that higher maternal pre-pregnancy body mass index is associated with adverse long-term outcomes for offspring including obesity, poorer cognitive and social abilities, and increased risk of psychiatric disorders.
MedicalResearch.com: What are the main findings?
Response: In this study, we investigated the association of maternal pre-pregnancy body mass index with fetal growth and neonatal functional connectivity and found that maternal pre-pregnancy BMI has a significant positive correlation with fetal weight and with greater thalamic connectivity of the brain. 

 Dr. Sachdev[/caption]
Darpun D. Sachdev, M.D.
Case investigation and Contact tracing Branch Chief
SFDPH Covid Command Center
San Francisco Department of Public Health
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The ultimate goal of contact tracing is to rapidly identify and isolate contacts who are COVID-19 positive before they have time to transmit to others. As mentioned in the published research letter by SFDPH, through JAMA, during early shelter-in-place (from April to June 2020), our contact tracing program successfully reached greater than 80% of cases and contacts within a median timeframe of 6 days from the onset of their case’s symptoms. Approximately 10% of named contacts were newly diagnosed with COVID-19 (compared to 2% positivity during this time period). Household contacts made up approximately 80% of all identified contacts, but 90% of contacts who tested positive lived in the same household as the case. Secondary cases (contacts who were found to be newly diagnosed with COVID-19) were traced and quarantined within 6 days of the case’s symptom onset.
With that said, the 6-day time difference between symptom onset and contact notification raises concern regarding the overall effectiveness of tracing in preventing onward transmission by infected contacts. We are working with community-based organizations to scale up access to testing and culturally competent tracing and wraparound services. Currently, we have now decreased the time difference to 5 days. Moreover, given that the majority of contacts resided in the same household, transmission could have occurred presymptomatically such that by the time infected contacts were identified, they might have already transmitted the virus. Hence, why SFDPH, on May 5, 2020, implemented the recommendation of universal testing for COVID-19 contacts, regardless of symptoms.
We recommend that testing should be offered to all contacts regardless of symptoms and encourage local health departments to adopt novel ways of increasing testing access for contacts.
Dr. Sachdev[/caption]
Darpun D. Sachdev, M.D.
Case investigation and Contact tracing Branch Chief
SFDPH Covid Command Center
San Francisco Department of Public Health
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The ultimate goal of contact tracing is to rapidly identify and isolate contacts who are COVID-19 positive before they have time to transmit to others. As mentioned in the published research letter by SFDPH, through JAMA, during early shelter-in-place (from April to June 2020), our contact tracing program successfully reached greater than 80% of cases and contacts within a median timeframe of 6 days from the onset of their case’s symptoms. Approximately 10% of named contacts were newly diagnosed with COVID-19 (compared to 2% positivity during this time period). Household contacts made up approximately 80% of all identified contacts, but 90% of contacts who tested positive lived in the same household as the case. Secondary cases (contacts who were found to be newly diagnosed with COVID-19) were traced and quarantined within 6 days of the case’s symptom onset.
With that said, the 6-day time difference between symptom onset and contact notification raises concern regarding the overall effectiveness of tracing in preventing onward transmission by infected contacts. We are working with community-based organizations to scale up access to testing and culturally competent tracing and wraparound services. Currently, we have now decreased the time difference to 5 days. Moreover, given that the majority of contacts resided in the same household, transmission could have occurred presymptomatically such that by the time infected contacts were identified, they might have already transmitted the virus. Hence, why SFDPH, on May 5, 2020, implemented the recommendation of universal testing for COVID-19 contacts, regardless of symptoms.
We recommend that testing should be offered to all contacts regardless of symptoms and encourage local health departments to adopt novel ways of increasing testing access for contacts.
![MedicalResearch.com Interview with: Selin Tokez, PhD Student Department of Dermatology Erasmus MC, Rotterdam MedicalResearch.com: What is the background for this study? Response: Cutaneous squamous cell carcinoma (cSCC) is the second most common skin cancer worldwide with still increasing incidence rates. Given these high incidence rates together with the associated health costs and possibility of fatal progression, it is extremely important to have accurate and complete data on the epidemiology of this disease. Nevertheless, national cancer registries in many countries do not routinely record cSCC cases and therefore currently known numbers are mainly based on incomplete data sources. Additionally, if cSCC cases are registered, this usually only concerns the first cSCC per patient while we know that, contrary to many other malignant neoplasms, patients may develop numerous cSCCs over time. MedicalResearch.com: What are the main findings? Response: In the present study, we analyzed Dutch nationwide data comprising about 145,000 patients with a first invasive cSCC diagnosis between the years 1989 and 2017. We found that the incidence rates of a first cSCC per patient almost tripled in male patients and increased about fivefold in female patients in this 30-year time period. Also, we had data on all cSCCs per patient for the year 2017 and could therefore compare this with the data on only the first cSCC per patient: incidence rates increased by 58% for men and 35% for women when multiple cSCCs were considered. In absolute numbers, this resulted in an increase of 45% in cSCC diagnoses in 2017. Lastly, we extended our analyses by predicting future cSCC incidence rates up to 2027. Given that no substantially effective measures are undertaken in the near future, current cSCC incidence rates will increase with 23% in males and 29% in females in the next decade. MedicalResearch.com: What should readers take away from your report? Response: We could summarize our main message in two points: while people generally know that cSCC is a very common disease with increasing incidence rates, it is not taken into account that these numbers are often based on incomplete data registries and that the real numbers are even higher. In this paper, we provided these numbers for a period of 30 years based on highly accurate data from the Netherlands Cancer Registry. On top of that, as a second main finding, we showed that the real burden caused by cSCC is approximately 50% higher (taken males and females together) when all cSCC diagnoses in 1 year are registered instead of only the first tumor per patient. Together with our prediction analyses that showed an on average 26% further increase for the coming decade, this will have enormous implications for the dermato-oncological health care planning and cost management. Our results urgently call for revision of skin cancer health policies to be able to cope with this rising burden of cSCC management. Ultimately, primary prevention will remain the key strategy to halt the increasing trend in cSCC incidence and the occurrence of multiple cSCCs per patient, which we hope to further stimulate with our paper as well. MedicalResearch.com: What recommendations do you have for future research as a result of this work? Response: As we had data on multiple cSCCs for only one year, we would suggest to perform trend analyses for multiple cSCCs per patient as well when a longer follow-up duration has been reached. Furthermore, it would be very relevant to identify high-risk cSCCs or patients at risk for multiple cSCCs in order to be able to establish efficient follow-up regimens and take these high risk groups into account when revising skin cancer health policies. MedicalResearch.com: Is there anything else you would like to add? Response: The authors of this study have no conflicts of interest that are relevant to this article. Citation: Tokez S, Hollestein L, Louwman M, Nijsten T, Wakkee M. Incidence of Multiple vs First Cutaneous Squamous Cell Carcinoma on a Nationwide Scale and Estimation of Future Incidences of Cutaneous Squamous Cell Carcinoma. JAMA Dermatol. Published online October 28, 2020. doi:10.1001/jamadermatol.2020.3677 [subscribe] Last Modified: [last-modified] The information on MedicalResearch.com is provided for educational purposes only, and is in no way intended to diagnose, cure, or treat any medical or other condition. Always seek the advice of your physician or other qualified health and ask your doctor any questions you may have regarding a medical condition. In addition to all other limitations and disclaimers in this agreement, service provider and its third party providers disclaim any liability or loss in connection with the content provided on this website.](https://medicalresearch.com/wp-content/uploads/2020/10/squamous-cell-cancer-dermnetnz-image.jpg)



 Dr. Bayes-Genis[/caption]
Antoni Bayes-Genis, MD, PhD, FESC, FHFA
Head, Heart Institute. Hospital Universitari Germans Trias i Pujol
Full Professor, Autonomous University Barcelona
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Omega-3 fatty acids are incorporated into the phospholipids of cellular membranes, including cardiac contractile cells, and have a wide range of demonstrated physiological effects. Several potential mechanisms have been investigated, including antiarrhythmic, anti-inflammatory, and endothelial.
Omega-3 fatty acids lower heart rate and improve heart rate variability, both associated with lower sudden cardiac death risk, one of the complications that may occur after a myocardial infarction.
Increased omega-3 fatty acids also enhance arterial elasticity by increasing endothelium-derived vasodilators, which is associated with blood pressure–lowering effects.
They also have a cardioprotective effect on platelet-monocyte aggregation, and lower triglyceride levels.
Dr. Bayes-Genis[/caption]
Antoni Bayes-Genis, MD, PhD, FESC, FHFA
Head, Heart Institute. Hospital Universitari Germans Trias i Pujol
Full Professor, Autonomous University Barcelona
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Omega-3 fatty acids are incorporated into the phospholipids of cellular membranes, including cardiac contractile cells, and have a wide range of demonstrated physiological effects. Several potential mechanisms have been investigated, including antiarrhythmic, anti-inflammatory, and endothelial.
Omega-3 fatty acids lower heart rate and improve heart rate variability, both associated with lower sudden cardiac death risk, one of the complications that may occur after a myocardial infarction.
Increased omega-3 fatty acids also enhance arterial elasticity by increasing endothelium-derived vasodilators, which is associated with blood pressure–lowering effects.
They also have a cardioprotective effect on platelet-monocyte aggregation, and lower triglyceride levels.
 Dr. Bragg[/caption]
Marie Bragg, PhD
Assistant Professor, Department of Population Health on Health Choice
NYU College of Global Public Health
MedicalResearch.com: What is the background for this study?
Response: We know from previous research that children who see food advertisements eat significantly more calories than children who see non-food advertisements. Those studies led the World Health Organization and National Academy of Medicine to issue reports declaring that exposure to food advertising is a major driver of childhood obesity.
What we don’t know is how frequently unhealthy food and beverage brands are appearing in YouTube videos posted by Kid Influencers. Kid influences are children whose parents film videos of the child playing with toys, unwrapping presents, eating food, or engaging in other family-friendly activities. The parents then post the videos to YouTube for other children and parents to view for entertainment.
Dr. Bragg[/caption]
Marie Bragg, PhD
Assistant Professor, Department of Population Health on Health Choice
NYU College of Global Public Health
MedicalResearch.com: What is the background for this study?
Response: We know from previous research that children who see food advertisements eat significantly more calories than children who see non-food advertisements. Those studies led the World Health Organization and National Academy of Medicine to issue reports declaring that exposure to food advertising is a major driver of childhood obesity.
What we don’t know is how frequently unhealthy food and beverage brands are appearing in YouTube videos posted by Kid Influencers. Kid influences are children whose parents film videos of the child playing with toys, unwrapping presents, eating food, or engaging in other family-friendly activities. The parents then post the videos to YouTube for other children and parents to view for entertainment. 


 Christos V. Chalitsios[/caption]
Christos Chalitsios B.Sc, M.Sc PhD student
Funded by British Medical Association (BMA)
School of Medicine
Division of Respiratory Medicine
University of Nottingham
City Hospital,Nottingham
MedicalResearch.com: What is the background for this study?
Response: Inhaled (ICS) and oral (OCS) corticosteroids play a crucial role in the control of airway inflammation in asthma. Given that the use of ICS in asthma is likely to increase with the recent change in GINA guidance recommending combined long-acting-β2-agonists with ICS at step 1 and the upward trend in prescribing of OCS, we sought to clarify the link between steroids, osteoporosis and FF in patients with asthma, stratifying the risk by dose, number of courses and type of steroids. The prevalence of patients receiving at least one bisphosphonate was also calculated.
Christos V. Chalitsios[/caption]
Christos Chalitsios B.Sc, M.Sc PhD student
Funded by British Medical Association (BMA)
School of Medicine
Division of Respiratory Medicine
University of Nottingham
City Hospital,Nottingham
MedicalResearch.com: What is the background for this study?
Response: Inhaled (ICS) and oral (OCS) corticosteroids play a crucial role in the control of airway inflammation in asthma. Given that the use of ICS in asthma is likely to increase with the recent change in GINA guidance recommending combined long-acting-β2-agonists with ICS at step 1 and the upward trend in prescribing of OCS, we sought to clarify the link between steroids, osteoporosis and FF in patients with asthma, stratifying the risk by dose, number of courses and type of steroids. The prevalence of patients receiving at least one bisphosphonate was also calculated.

 Dr. Etkin[/caption]
Amit Etkin, MD, PhD
Department of Psychiatry and Behavioral Sciences
Wu Tsai Neurosciences Institute, Stanford Universitu
Stanford, CA
MedicalResearch.com: What is the mission of Cohen Veterans Bioscience - CVB?
Dr. Etkin[/caption]
Amit Etkin, MD, PhD
Department of Psychiatry and Behavioral Sciences
Wu Tsai Neurosciences Institute, Stanford Universitu
Stanford, CA
MedicalResearch.com: What is the mission of Cohen Veterans Bioscience - CVB?
 Response: Cohen Veterans Bioscience (CVB) is a non-profit 501(c)(3) research biotech dedicated to fast-tracking the development of diagnostic tests and personalized therapeutics for the millions of Veterans and civilians who suffer the devastating effects of trauma-related and other brain disorders.
MedicalResearch.com: How can patients with PTSD or MDD benefit from this information?
Response: With the discovery of this new brain imaging biomarker, patients who suffer from PTSD or MDD may be guided towards the most effective treatment without waiting months and months to find a treatment that may work for them.
MedicalResearch.com: What is the background for this study?
Response: This study, which was supported with a grant from Cohen Veterans Bioscience, grants from the National Institute of Mental Health (NIMH and other supporters, derives from our work over the past few years which has pointed to the critical importance of understanding how patients with a variety of psychiatric disorders differ biologically. The shortcomings of our current diagnostic system have become very clear over the past 1-2 decades, but the availability of tools for transcending these limitations on the back of objective biological tests has not kept pace with the need for those tools.
In prior work, we have used a variety of methods, including different types of brain imaging, to identify brain signals that underpin key biological differences within and across traditional psychiatric diagnoses. We have also developed specialized AI tools for decoding complex patterns of brain activity in order to understand and quantify biological heterogeneity in individual patients. These developments have then, in turn, converged with the completion of a number of large brain imaging-coupled clinical trials, which have provided a scale of these types of data not previously available in the field.
Response: Cohen Veterans Bioscience (CVB) is a non-profit 501(c)(3) research biotech dedicated to fast-tracking the development of diagnostic tests and personalized therapeutics for the millions of Veterans and civilians who suffer the devastating effects of trauma-related and other brain disorders.
MedicalResearch.com: How can patients with PTSD or MDD benefit from this information?
Response: With the discovery of this new brain imaging biomarker, patients who suffer from PTSD or MDD may be guided towards the most effective treatment without waiting months and months to find a treatment that may work for them.
MedicalResearch.com: What is the background for this study?
Response: This study, which was supported with a grant from Cohen Veterans Bioscience, grants from the National Institute of Mental Health (NIMH and other supporters, derives from our work over the past few years which has pointed to the critical importance of understanding how patients with a variety of psychiatric disorders differ biologically. The shortcomings of our current diagnostic system have become very clear over the past 1-2 decades, but the availability of tools for transcending these limitations on the back of objective biological tests has not kept pace with the need for those tools.
In prior work, we have used a variety of methods, including different types of brain imaging, to identify brain signals that underpin key biological differences within and across traditional psychiatric diagnoses. We have also developed specialized AI tools for decoding complex patterns of brain activity in order to understand and quantify biological heterogeneity in individual patients. These developments have then, in turn, converged with the completion of a number of large brain imaging-coupled clinical trials, which have provided a scale of these types of data not previously available in the field.