Author Interviews, NEJM, Neurology, Pain Research / 18.08.2021
Episodic Migraine: Atogepant Effective At Reducing Migraine Days
MedicalResearch.com Interview with:
[caption id="attachment_57964" align="alignleft" width="200"] Dr. Ailani[/caption]
Jessica Ailani M.D. FAHS FAAN FANA
Director Medstar Georgetown Headache Center
Vice Co-Chair of Strategic Planning for MedStar Neurology
Professor of Clinical Neurology
MedStar Georgetown University Hospital
MedicalResearch.com: What is the background for this study?
Response: Migraine is a common neurological disease that causes disabling attacks that can be frequent. Preventive treatments can help reduce the frequency of attacks and improve patient function, reducing disease burden.
Dr. Ailani[/caption]
Jessica Ailani M.D. FAHS FAAN FANA
Director Medstar Georgetown Headache Center
Vice Co-Chair of Strategic Planning for MedStar Neurology
Professor of Clinical Neurology
MedStar Georgetown University Hospital
MedicalResearch.com: What is the background for this study?
Response: Migraine is a common neurological disease that causes disabling attacks that can be frequent. Preventive treatments can help reduce the frequency of attacks and improve patient function, reducing disease burden.
 Dr. Ailani[/caption]
Jessica Ailani M.D. FAHS FAAN FANA
Director Medstar Georgetown Headache Center
Vice Co-Chair of Strategic Planning for MedStar Neurology
Professor of Clinical Neurology
MedStar Georgetown University Hospital
MedicalResearch.com: What is the background for this study?
Response: Migraine is a common neurological disease that causes disabling attacks that can be frequent. Preventive treatments can help reduce the frequency of attacks and improve patient function, reducing disease burden.
Dr. Ailani[/caption]
Jessica Ailani M.D. FAHS FAAN FANA
Director Medstar Georgetown Headache Center
Vice Co-Chair of Strategic Planning for MedStar Neurology
Professor of Clinical Neurology
MedStar Georgetown University Hospital
MedicalResearch.com: What is the background for this study?
Response: Migraine is a common neurological disease that causes disabling attacks that can be frequent. Preventive treatments can help reduce the frequency of attacks and improve patient function, reducing disease burden.


 Dr. Anderson[/caption]
Dr. Weston B Anderson PhD
Postdoctoral Reasearch Scientist
International Research Institute for Climate and Society
The Earth Institute
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: We find that while drought continues to be a consistent trigger of food crises in Sub-Saharan Africa, protracted conflict has become relatively more important over the last decade.
We furthermore find that pastoral livelihoods have taken longer to return to food secure conditions following droughts as compared to agricultural livelihoods.
Dr. Anderson[/caption]
Dr. Weston B Anderson PhD
Postdoctoral Reasearch Scientist
International Research Institute for Climate and Society
The Earth Institute
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: We find that while drought continues to be a consistent trigger of food crises in Sub-Saharan Africa, protracted conflict has become relatively more important over the last decade.
We furthermore find that pastoral livelihoods have taken longer to return to food secure conditions following droughts as compared to agricultural livelihoods.
 Dr. Albrecht[/caption]
Joerg Albrecht, MD, PhD
Dermatologist, Internist, Clinical Pharmacologist
Division of Dermatology, Department of Medicine
Attending Dermatologist, Chair Division of Dermatology
Chair system-wide Pharmacy & Therapeutics Committee
Cook County Health
Chicago, IL 60612
MedicalResearch.com: What is the background for this study?
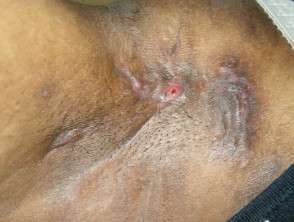
Response: The study was stimulated by data that suggested that an unusually large proportion of inpatient with Hidradenitis suppurativa (HS) were African American. HS is an underdiagnosed disease and the total numbers of inpatients with HS in the year we looked at initially seemed small. So we wanted to test whether this finding held up when the period of observation was extended. Point estimates can be unreliable and we had followed another finding in the data that did not hold up when we looked at other years, so we felt one year was not enough to confirm a trend
Dr. Albrecht[/caption]
Joerg Albrecht, MD, PhD
Dermatologist, Internist, Clinical Pharmacologist
Division of Dermatology, Department of Medicine
Attending Dermatologist, Chair Division of Dermatology
Chair system-wide Pharmacy & Therapeutics Committee
Cook County Health
Chicago, IL 60612
MedicalResearch.com: What is the background for this study?
Response: The study was stimulated by data that suggested that an unusually large proportion of inpatient with Hidradenitis suppurativa (HS) were African American. HS is an underdiagnosed disease and the total numbers of inpatients with HS in the year we looked at initially seemed small. So we wanted to test whether this finding held up when the period of observation was extended. Point estimates can be unreliable and we had followed another finding in the data that did not hold up when we looked at other years, so we felt one year was not enough to confirm a trend



 Dr. Ribeiro[/caption]
Fernando Ribeiro PhD
School of Health Sciences
Institute of Biomedicine - iBiMED
University of Aveiro
Aveiro, Portugal
MedicalResearch.com: What is the background for this study? What are the main findings?
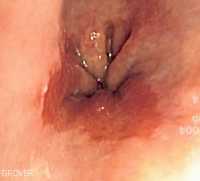
Response: Resistant hypertension is a puzzling problem without a clear solution. The available treatment options to lower blood pressure, namely medication and renal denervation, have had limited success, making nonpharmacological strategies good candidates to optimize the treatment of this condition.
Exercise training is consistently recommended as adjuvant therapy for patients with hypertension, yet, it is with a great delay that the efficacy of exercise training is being tested in patients with resistant hypertension.
Having that in mind, the EnRicH trial was designed to address whether the benefits of an exercise intervention with proven results in hypertensive individuals are extended to patients with resistant hypertension, a clinical population with low responsiveness to drug therapy. Exercise training was safe and associated with a significant and clinically relevant reduction in 24-hour, daytime ambulatory, and office blood pressure compared with control (usual care).
Dr. Ribeiro[/caption]
Fernando Ribeiro PhD
School of Health Sciences
Institute of Biomedicine - iBiMED
University of Aveiro
Aveiro, Portugal
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Resistant hypertension is a puzzling problem without a clear solution. The available treatment options to lower blood pressure, namely medication and renal denervation, have had limited success, making nonpharmacological strategies good candidates to optimize the treatment of this condition.
Exercise training is consistently recommended as adjuvant therapy for patients with hypertension, yet, it is with a great delay that the efficacy of exercise training is being tested in patients with resistant hypertension.
Having that in mind, the EnRicH trial was designed to address whether the benefits of an exercise intervention with proven results in hypertensive individuals are extended to patients with resistant hypertension, a clinical population with low responsiveness to drug therapy. Exercise training was safe and associated with a significant and clinically relevant reduction in 24-hour, daytime ambulatory, and office blood pressure compared with control (usual care).
 Dr. Pierce[/caption]
John Pierce, PhD
Professor Emeritus
Department of Family Medicine and Public Health
Moores Cancer Center Director for Population Sciences
Co-leader of the Cancer Prevention program
UC San Diego
MedicalResearch.com: What is the background for this study? What are the main findings?
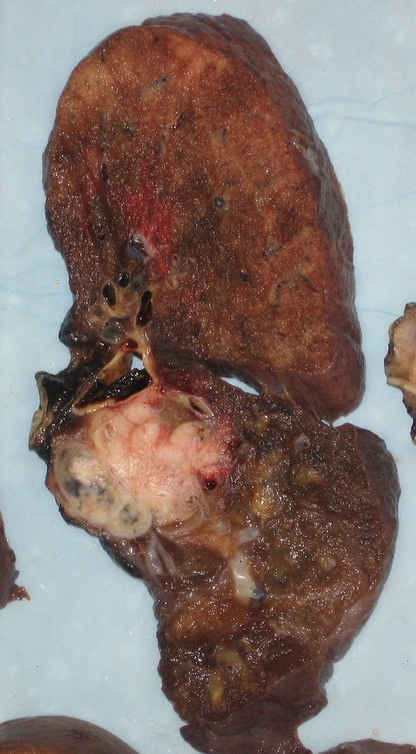
Response: Graphic Warning Labels are to be implemented in the US in July 2022, depending on litigation. This will be about 10 years after they were first proposed. Meanwhile, 120 other countries have implemented them already.
The FDA states that their purpose for the warnings is to provide a constant reminder to smokers about the health consequences of smoking, not to force them to quit.
In our study, 3 months of having cigarettes repackaged into graphic warning packs was associated with smokers thinking more about quitting and not getting as much pleasure out of their cigarettes. However, thinking about quitting is only the first step to conquering a nicotine addiction.
Dr. Pierce[/caption]
John Pierce, PhD
Professor Emeritus
Department of Family Medicine and Public Health
Moores Cancer Center Director for Population Sciences
Co-leader of the Cancer Prevention program
UC San Diego
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Graphic Warning Labels are to be implemented in the US in July 2022, depending on litigation. This will be about 10 years after they were first proposed. Meanwhile, 120 other countries have implemented them already.
The FDA states that their purpose for the warnings is to provide a constant reminder to smokers about the health consequences of smoking, not to force them to quit.
In our study, 3 months of having cigarettes repackaged into graphic warning packs was associated with smokers thinking more about quitting and not getting as much pleasure out of their cigarettes. However, thinking about quitting is only the first step to conquering a nicotine addiction.
 Dr. Lopez[/caption]
Maria Luisa S. Sequeira Lopez, MD, FAHA
Harrison Distinguished Professor in Pediatrics and Biology
University of Virginia
Charlottesville, VA 22908
MedicalResearch.com: What is the background for this study?
Response: The renin-angiotensin system (RAS) is crucial in the regulation of the blood pressure (BP). Synthesis and secretion of renin is the key regulated event in the operation of the RAS.
One of the main mechanisms that control renin synthesis and release is the baroreceptor mechanism whereby a decrease in blood pressure results in increased release of renin by juxtaglomerular (JG) cells.
In spite of its enormous importance, the nature and location of the renal baroreceptor was still unknown. This was due in great part to the lack of appropriate in vitro and in vivo models to confidently allow tracking of the fate and isolation of renin cells, and the lack of tools to study the chromatin in scarce cells.
Dr. Lopez[/caption]
Maria Luisa S. Sequeira Lopez, MD, FAHA
Harrison Distinguished Professor in Pediatrics and Biology
University of Virginia
Charlottesville, VA 22908
MedicalResearch.com: What is the background for this study?
Response: The renin-angiotensin system (RAS) is crucial in the regulation of the blood pressure (BP). Synthesis and secretion of renin is the key regulated event in the operation of the RAS.
One of the main mechanisms that control renin synthesis and release is the baroreceptor mechanism whereby a decrease in blood pressure results in increased release of renin by juxtaglomerular (JG) cells.
In spite of its enormous importance, the nature and location of the renal baroreceptor was still unknown. This was due in great part to the lack of appropriate in vitro and in vivo models to confidently allow tracking of the fate and isolation of renin cells, and the lack of tools to study the chromatin in scarce cells.


 Dr. Blumenthal[/caption]
Kimberly G. Blumenthal, MD, MSc
Massachusetts General Hospital
The Mongan Institute
Boston, MA 02114
[caption id="attachment_57828" align="alignleft" width="100"]
Dr. Blumenthal[/caption]
Kimberly G. Blumenthal, MD, MSc
Massachusetts General Hospital
The Mongan Institute
Boston, MA 02114
[caption id="attachment_57828" align="alignleft" width="100"] Dr. Krantz[/caption]
Matthew S. Krantz, MD
Division of Allergy, Pulmonary and Critical Care Medicine
Department of Medicine,
Vanderbilt University Medical Center,
Nashville, Tennessee
MedicalResearch.com: What is the background for this study?
Response: During the initial COVID-19 vaccine campaign with healthcare workers in December 2020, there was an unexpected higher than anticipated rate of immediate allergic reactions after Pfizer and Moderna mRNA vaccines. This prompted both patient and provider concerns, particularly in those with underlying allergic histories, on the associated risks for immediate allergic reactions with the mRNA vaccines.
Because of the significantly improved effectiveness of two doses of an mRNA vaccine compared to one dose, it was important to determine if those who experienced immediate allergic reaction symptoms after their first dose could go on to tolerate a second dose safely.
Dr. Krantz[/caption]
Matthew S. Krantz, MD
Division of Allergy, Pulmonary and Critical Care Medicine
Department of Medicine,
Vanderbilt University Medical Center,
Nashville, Tennessee
MedicalResearch.com: What is the background for this study?
Response: During the initial COVID-19 vaccine campaign with healthcare workers in December 2020, there was an unexpected higher than anticipated rate of immediate allergic reactions after Pfizer and Moderna mRNA vaccines. This prompted both patient and provider concerns, particularly in those with underlying allergic histories, on the associated risks for immediate allergic reactions with the mRNA vaccines.
Because of the significantly improved effectiveness of two doses of an mRNA vaccine compared to one dose, it was important to determine if those who experienced immediate allergic reaction symptoms after their first dose could go on to tolerate a second dose safely. 


 Dr. Correa[/caption]
Andres F. Correa, MD
Assistant Professor
Department of Surgical Oncology, and
[caption id="attachment_57815" align="alignleft" width="150"]
Dr. Correa[/caption]
Andres F. Correa, MD
Assistant Professor
Department of Surgical Oncology, and
[caption id="attachment_57815" align="alignleft" width="150"] Dr. Bernstein[/caption]
Adrien Bernstein, MD
Second Year Urologic Oncology Fellow
Fox Chase Cancer Center
MedicalResearch.com: What is the background for this study?
Response: Unfortunately, it has been well-established that historically Black Americans experience increased cancer specific mortality compared to white patients. In prostate cancer specifically studies have shown that when access to care is equitable this gap resolves. This suggests that biological factors are not driving these differences but rather the result of the complex interplay of social determinants and systemic inequities in our healthcare system.
Early in the pandemic, multiple studies demonstrated that minority communities disproportionately shouldered poor COVID-19 outcomes. On March 13th 2020, the American College of Surgeons recommended against elective procedures; however, the definition of an elective oncologic case was left to the discretion of the provider. As prostate cancer treatment can be safely deferred up to a year follow diagnosis, management of prostate cancer during the initial lockdown period of the COVID-19 Pandemic provided a useful analysis of the differential restrictions placed on non-emergent health care during the Pandemic.
Dr. Bernstein[/caption]
Adrien Bernstein, MD
Second Year Urologic Oncology Fellow
Fox Chase Cancer Center
MedicalResearch.com: What is the background for this study?
Response: Unfortunately, it has been well-established that historically Black Americans experience increased cancer specific mortality compared to white patients. In prostate cancer specifically studies have shown that when access to care is equitable this gap resolves. This suggests that biological factors are not driving these differences but rather the result of the complex interplay of social determinants and systemic inequities in our healthcare system.
Early in the pandemic, multiple studies demonstrated that minority communities disproportionately shouldered poor COVID-19 outcomes. On March 13th 2020, the American College of Surgeons recommended against elective procedures; however, the definition of an elective oncologic case was left to the discretion of the provider. As prostate cancer treatment can be safely deferred up to a year follow diagnosis, management of prostate cancer during the initial lockdown period of the COVID-19 Pandemic provided a useful analysis of the differential restrictions placed on non-emergent health care during the Pandemic.








 Dr. Nation[/caption]
Daniel A. Nation, Ph.D.,
Associate Professor of Psychological Science
Institute for Memory Impairments and Neurological Disorders
University of California, Irvin
MedicalResearch.com: What is the background for this study?
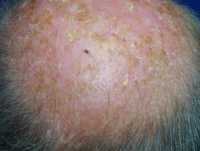
Response: Hypertension is a risk factor for cognitive decline and dementia, and treatment of hypertension has been linked to decreased risk for cognitive impairment.
Prior studies have attempted to identify which specific type of antihypertensive treatment conveys the most benefit for cognition, but findings have been mixed regarding this question. We hypothesized that antihypertensive drugs acting on the brain angiotensin system may convey the greatest benefit since they affect the brain angiotensin system that has been implicated in memory function.
Dr. Nation[/caption]
Daniel A. Nation, Ph.D.,
Associate Professor of Psychological Science
Institute for Memory Impairments and Neurological Disorders
University of California, Irvin
MedicalResearch.com: What is the background for this study?
Response: Hypertension is a risk factor for cognitive decline and dementia, and treatment of hypertension has been linked to decreased risk for cognitive impairment.
Prior studies have attempted to identify which specific type of antihypertensive treatment conveys the most benefit for cognition, but findings have been mixed regarding this question. We hypothesized that antihypertensive drugs acting on the brain angiotensin system may convey the greatest benefit since they affect the brain angiotensin system that has been implicated in memory function.

 Dr. Seifi[/caption]
Ali Seifi, MD, FACP, FNCS, FCCM
Associate Professor
Director of Neuro Critical Care,
Fellowship Director, CAST Neurosurgery Critical Care
Department of Neurosurgery, Neurology, Anesthesiology and Medicine
The University of Texas Health Science Center at San Antonio
MedicalResearch.com: What is the background for this study?
Dr. Seifi[/caption]
Ali Seifi, MD, FACP, FNCS, FCCM
Associate Professor
Director of Neuro Critical Care,
Fellowship Director, CAST Neurosurgery Critical Care
Department of Neurosurgery, Neurology, Anesthesiology and Medicine
The University of Texas Health Science Center at San Antonio
MedicalResearch.com: What is the background for this study?


 Dr. Conner[/caption]
Christopher Conner, MD, PhD
Neurosurgery resident
McGovern Medical School
The University of Texas Health Science Center at Houston
MedicalResearch.com: What is the background for this study?
Response: There has been a growing understanding in medicine that the incidence of motor vehicle trauma is changing. We have watched as Friday and Saturday night emergencies have declined without a good explanation. Several other studies have investigated this, but the results were not conclusive.
We think that is due to a lack of data from the rideshare companies and hospitals directly
Dr. Conner[/caption]
Christopher Conner, MD, PhD
Neurosurgery resident
McGovern Medical School
The University of Texas Health Science Center at Houston
MedicalResearch.com: What is the background for this study?
Response: There has been a growing understanding in medicine that the incidence of motor vehicle trauma is changing. We have watched as Friday and Saturday night emergencies have declined without a good explanation. Several other studies have investigated this, but the results were not conclusive.
We think that is due to a lack of data from the rideshare companies and hospitals directly