Aging, Author Interviews, Environmental Risks, Nature / 30.07.2022
Avoidance of Blue Light Might Be A Good Anti-Aging Strategy
MedicalResearch.com Interview with:
[caption id="attachment_59381" align="alignleft" width="150"] Dr. Giebultowicz[/caption]
Dr. Jaga Giebultowicz
Professor Emeritus,
Department of Integrative Biology
Oregon State University
Corvallis, OR 97331
MedicalResearch.com: What is the background for this study? Where is blue light commonly found?
Response: Our study in short-lived model organism Drosophila revealed that cumulative, long-term exposure to blue light impacts brain function, accelerates the aging process and significantly shortens lifespan compared to flies maintained in constant darkness or in white light with blue wavelengths blocked.
Blue light is predominantly produced by the light-emitting diodes (LEDs); it appears white due to the addition of yellow fluorescent powder which is activated by blue light. LEDs has become a main source of display screens (phones, laptops, desktops, TV), and ambient lights. Indeed, humans have become awash in LEDs for most of their waking hours.
Dr. Giebultowicz[/caption]
Dr. Jaga Giebultowicz
Professor Emeritus,
Department of Integrative Biology
Oregon State University
Corvallis, OR 97331
MedicalResearch.com: What is the background for this study? Where is blue light commonly found?
Response: Our study in short-lived model organism Drosophila revealed that cumulative, long-term exposure to blue light impacts brain function, accelerates the aging process and significantly shortens lifespan compared to flies maintained in constant darkness or in white light with blue wavelengths blocked.
Blue light is predominantly produced by the light-emitting diodes (LEDs); it appears white due to the addition of yellow fluorescent powder which is activated by blue light. LEDs has become a main source of display screens (phones, laptops, desktops, TV), and ambient lights. Indeed, humans have become awash in LEDs for most of their waking hours.
 Dr. Giebultowicz[/caption]
Dr. Jaga Giebultowicz
Professor Emeritus,
Department of Integrative Biology
Oregon State University
Corvallis, OR 97331
MedicalResearch.com: What is the background for this study? Where is blue light commonly found?
Response: Our study in short-lived model organism Drosophila revealed that cumulative, long-term exposure to blue light impacts brain function, accelerates the aging process and significantly shortens lifespan compared to flies maintained in constant darkness or in white light with blue wavelengths blocked.
Blue light is predominantly produced by the light-emitting diodes (LEDs); it appears white due to the addition of yellow fluorescent powder which is activated by blue light. LEDs has become a main source of display screens (phones, laptops, desktops, TV), and ambient lights. Indeed, humans have become awash in LEDs for most of their waking hours.
Dr. Giebultowicz[/caption]
Dr. Jaga Giebultowicz
Professor Emeritus,
Department of Integrative Biology
Oregon State University
Corvallis, OR 97331
MedicalResearch.com: What is the background for this study? Where is blue light commonly found?
Response: Our study in short-lived model organism Drosophila revealed that cumulative, long-term exposure to blue light impacts brain function, accelerates the aging process and significantly shortens lifespan compared to flies maintained in constant darkness or in white light with blue wavelengths blocked.
Blue light is predominantly produced by the light-emitting diodes (LEDs); it appears white due to the addition of yellow fluorescent powder which is activated by blue light. LEDs has become a main source of display screens (phones, laptops, desktops, TV), and ambient lights. Indeed, humans have become awash in LEDs for most of their waking hours.




 Clare Jensen[/caption]
Clare Jensen
O’Haire Research Team
Center for the Human-Animal Bond
Purdue University College of Veterinary Medicine
MedicalResearch.com: What is the background for this study?
Response: Service dogs for PTSD are becoming more common and the evidence shows they can help improve mental health and quality of life for many veterans with PTSD. However, some veterans benefit more than others. Our research goal was to ask for the very first time: Why?
Clare Jensen[/caption]
Clare Jensen
O’Haire Research Team
Center for the Human-Animal Bond
Purdue University College of Veterinary Medicine
MedicalResearch.com: What is the background for this study?
Response: Service dogs for PTSD are becoming more common and the evidence shows they can help improve mental health and quality of life for many veterans with PTSD. However, some veterans benefit more than others. Our research goal was to ask for the very first time: Why?

 Dr. LeBoff[/caption]
Meryl S. LeBoff, MD
Dr. LeBoff[/caption]
Meryl S. LeBoff, MD
 Dr. Manson[/caption]
JoAnn E. Manson, MD, DrPH
Professor, Epidemiology, Harvard T.H. Chan School Of Public Health
Michael and Lee Bell Professor of Women's Health, Medicine, Harvard Medical School
Chief, Preventive Medicine, Brigham And Women's Hospital
Co-Director, Womens Health, Brigham And Women's Hospital
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Osteoporosis is a major public health problem. Although supplemental vitamin D has been widely used to reduce the risk of fractures in the general population, studies of the effects of vitamin D on fractures, the most important bone health outcome, have been conflicting.
Randomized controlled trials, the highest quality studies, from around the world have shown benefit, no effect, or even harm of supplemental vitamin D on risk of fractures. Some of the trials used bolus dosing, had small samples sizes or short study duration, and co-administered calcium. No large RCTS of this scale tested whether daily supplemental vitamin D (without co-administration with calcium) prevented fractures in the US population.
To fill these knowledge gaps, we tested the hypothesis in this ancillary study to VITAL, whether daily supplemental vitamin D3 reduced the risk of incident total, non-spine and hip fractures in women and men in the US.
Dr. Manson[/caption]
JoAnn E. Manson, MD, DrPH
Professor, Epidemiology, Harvard T.H. Chan School Of Public Health
Michael and Lee Bell Professor of Women's Health, Medicine, Harvard Medical School
Chief, Preventive Medicine, Brigham And Women's Hospital
Co-Director, Womens Health, Brigham And Women's Hospital
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Osteoporosis is a major public health problem. Although supplemental vitamin D has been widely used to reduce the risk of fractures in the general population, studies of the effects of vitamin D on fractures, the most important bone health outcome, have been conflicting.
Randomized controlled trials, the highest quality studies, from around the world have shown benefit, no effect, or even harm of supplemental vitamin D on risk of fractures. Some of the trials used bolus dosing, had small samples sizes or short study duration, and co-administered calcium. No large RCTS of this scale tested whether daily supplemental vitamin D (without co-administration with calcium) prevented fractures in the US population.
To fill these knowledge gaps, we tested the hypothesis in this ancillary study to VITAL, whether daily supplemental vitamin D3 reduced the risk of incident total, non-spine and hip fractures in women and men in the US.


 Joanna Jiang, PhD
Agency for Healthcare Research and Quality
Rockville, Maryland
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Over the last decade we have seen two trends occurring to rural hospitals – closures and mergers. A hospital in financial distress could likely face closure. But if the hospital affiliates with a multihospital system, it may have access to resources from the system that help shelter the hospital from closure.
That is exactly what we found in this study. System affiliation was associated with a lower risk of closure for financially distressed hospitals. However, among hospitals that were financially stable, system affiliation was associated with a higher risk of closure. This is somewhat puzzling and needs further study to better understand the reason for closure.
Joanna Jiang, PhD
Agency for Healthcare Research and Quality
Rockville, Maryland
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Over the last decade we have seen two trends occurring to rural hospitals – closures and mergers. A hospital in financial distress could likely face closure. But if the hospital affiliates with a multihospital system, it may have access to resources from the system that help shelter the hospital from closure.
That is exactly what we found in this study. System affiliation was associated with a lower risk of closure for financially distressed hospitals. However, among hospitals that were financially stable, system affiliation was associated with a higher risk of closure. This is somewhat puzzling and needs further study to better understand the reason for closure.

 Dr. Midya[/caption]
Dania Valvi, MD MPH PhD
Assistant Professor
Department of Environmental Medicine and Public Health
Co-Director, MS in Epidemiology
Icahn School of Medicine at Mount Sinai
Email: dania.valvi@mssm.edu
MedicalResearch.com: What is the background for this study?
Response: Non-alcoholic fatty liver disease (NAFLD) is the most common liver disease in children in the U.S., Europe and other world regions, currently affecting 1 in every 10 children, and 1 in every 3 children with obesity in the U.S. The rate of pediatric NAFLD has more than doubled in recent decades following the epidemic rates also noted for childhood obesity. There is increasing interest in the role that environmental chemical exposures may play in NAFLD etiology, since several animal studies have shown that prenatal exposures to endocrine-disrupting chemicals (EDCs) cause liver injury and damage; but, until now, the potential effects of prenatal EDC mixture exposures in pediatric NAFLD had not been studied.
Dr. Midya[/caption]
Dania Valvi, MD MPH PhD
Assistant Professor
Department of Environmental Medicine and Public Health
Co-Director, MS in Epidemiology
Icahn School of Medicine at Mount Sinai
Email: dania.valvi@mssm.edu
MedicalResearch.com: What is the background for this study?
Response: Non-alcoholic fatty liver disease (NAFLD) is the most common liver disease in children in the U.S., Europe and other world regions, currently affecting 1 in every 10 children, and 1 in every 3 children with obesity in the U.S. The rate of pediatric NAFLD has more than doubled in recent decades following the epidemic rates also noted for childhood obesity. There is increasing interest in the role that environmental chemical exposures may play in NAFLD etiology, since several animal studies have shown that prenatal exposures to endocrine-disrupting chemicals (EDCs) cause liver injury and damage; but, until now, the potential effects of prenatal EDC mixture exposures in pediatric NAFLD had not been studied.
 SooYoung VanDeMar[/caption]
SooYoung VanDeMark, MBS
Geisinger Commonwealth School of Medicine
Scranton, Pennsylvania
MedicalResearch.com: What is the background for this study?
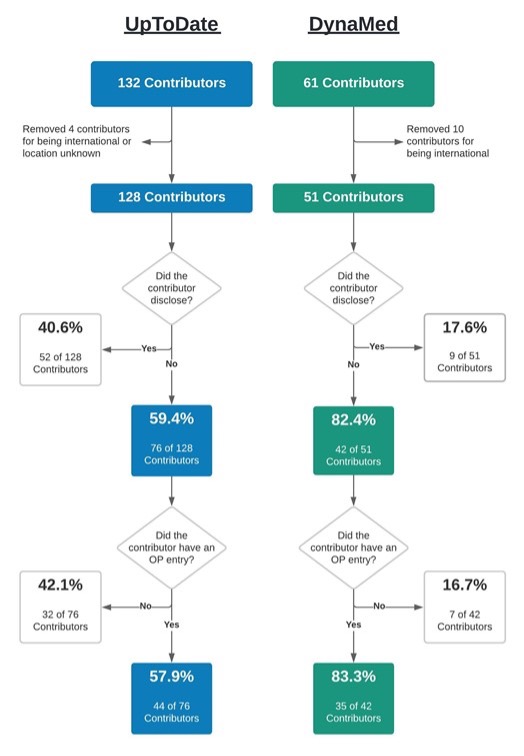
Response: Health care providers utilize subscription-based, point-of-care databases such as DynaMed and UpToDate to provide clinical care guidance and remain current on the latest evidence-based findings. Both of these websites maintain this content through a cadre of physician contributors who write and edit articles for these sites. These physician contributors are required to self-report any conflicts of interest (COI) as outlined by the respective policies on each website. However, prior COI research into similarly self-regulated areas, such as medical and pharmacology textbooks, and clinical practice guidelines, has found both appreciable potential COI and inconsistencies between self-reported and industry mandated disclosures (1-3).
This study (4) explored the accuracy of physician contributors to DynaMed and UpToDate by comparing their self-reported disclosure status with the financial remunerations they received from the healthcare industry (e.g., pharmaceutical companies) as reported to the U.S. Centers for Medicare and Medicaid Services’ Open Payments database. Physician contributors who reported “nothing to disclose” on their respective article topic but had an entry on Open Payments for having received money from industry, were classified as discordant and, thus, as having the potential for a COI. Additionally, total remuneration, gender, and payment category were investigated more in depth for each database.
SooYoung VanDeMar[/caption]
SooYoung VanDeMark, MBS
Geisinger Commonwealth School of Medicine
Scranton, Pennsylvania
MedicalResearch.com: What is the background for this study?
Response: Health care providers utilize subscription-based, point-of-care databases such as DynaMed and UpToDate to provide clinical care guidance and remain current on the latest evidence-based findings. Both of these websites maintain this content through a cadre of physician contributors who write and edit articles for these sites. These physician contributors are required to self-report any conflicts of interest (COI) as outlined by the respective policies on each website. However, prior COI research into similarly self-regulated areas, such as medical and pharmacology textbooks, and clinical practice guidelines, has found both appreciable potential COI and inconsistencies between self-reported and industry mandated disclosures (1-3).
This study (4) explored the accuracy of physician contributors to DynaMed and UpToDate by comparing their self-reported disclosure status with the financial remunerations they received from the healthcare industry (e.g., pharmaceutical companies) as reported to the U.S. Centers for Medicare and Medicaid Services’ Open Payments database. Physician contributors who reported “nothing to disclose” on their respective article topic but had an entry on Open Payments for having received money from industry, were classified as discordant and, thus, as having the potential for a COI. Additionally, total remuneration, gender, and payment category were investigated more in depth for each database.

 Dr. Soriano[/caption]
Victoria Soriano PhD
Research Assistant/Officer, Population Allergy
University of Melbourne
MedicalResearch.com: What is the background for this study?
Response: Peanut allergy is one of the most common childhood food allergies, and children rarely grow out of it. The only proven way to prevent peanut allergy is to give infants age-appropriate peanut products in the first year of life.
We previously showed there was a dramatic increase in peanut introduction from 2007-11 to 2018-19, following changes to infant feeding guidelines. We wanted to know if earlier peanut introduction would reduce peanut allergy in the general population (in Melbourne, Australia).
Dr. Soriano[/caption]
Victoria Soriano PhD
Research Assistant/Officer, Population Allergy
University of Melbourne
MedicalResearch.com: What is the background for this study?
Response: Peanut allergy is one of the most common childhood food allergies, and children rarely grow out of it. The only proven way to prevent peanut allergy is to give infants age-appropriate peanut products in the first year of life.
We previously showed there was a dramatic increase in peanut introduction from 2007-11 to 2018-19, following changes to infant feeding guidelines. We wanted to know if earlier peanut introduction would reduce peanut allergy in the general population (in Melbourne, Australia).

 Dr. Barry[/caption]
Michael J. Barry, M.D
Director of the Informed Medical Decisions Program
Health Decision Sciences Center
Massachusetts General Hospital.
Professor of medicine at Harvard Medical School
Dr. Barry was appointed as Vice Chair of USPSTF in March 2021.
He previously served as a member from January 2017 through December 2020.
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The Task Force looked at the use of vitamin and mineral supplementation specifically for the prevention of heart disease, stroke, and cancer. We found that there is not enough evidence to recommend for or against taking multivitamin supplements, nor the use of single or paired nutrient supplements, to prevent these conditions.
However, we do know that you should not take vitamin E or beta-carotene for this purpose.
Dr. Barry[/caption]
Michael J. Barry, M.D
Director of the Informed Medical Decisions Program
Health Decision Sciences Center
Massachusetts General Hospital.
Professor of medicine at Harvard Medical School
Dr. Barry was appointed as Vice Chair of USPSTF in March 2021.
He previously served as a member from January 2017 through December 2020.
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The Task Force looked at the use of vitamin and mineral supplementation specifically for the prevention of heart disease, stroke, and cancer. We found that there is not enough evidence to recommend for or against taking multivitamin supplements, nor the use of single or paired nutrient supplements, to prevent these conditions.
However, we do know that you should not take vitamin E or beta-carotene for this purpose.













 Dr. Rowe[/caption]
Susannah G. Rowe, MD, MPH
Office of Equity, Vitality and Inclusion
Boston University Medical Group
Boston Medical Center
Boston University School of Medicine
Boston, Massachusetts
MedicalResearch.com: What is the background for this study?
Response: We wanted to learn how frequently mistreatment occurs for clinicians at work and how it impacts their occupational well-being. We began to see more anecdotal reports of workplace mistreatment of clinicians even before the pandemic. In the extraordinarily stressful environment we are currently experiencing, with people feeling exhausted and emotionally threadbare on some level, the problem appears to be growing.
We also predicted that the burden of mistreatment would not borne be equally. It has often been said that we are all in the same storm but in different boats – some of us are riding out the storm in comfortable ocean liners, while others are paddling in canoes without life jackets. What we are learning, though, is that we are not in fact experiencing the same storm. For example, the increasing intolerance and erosion of public civility we have seen in recent years might show up as minor annoyances for some of us, and actual threats of violence for others depending in large part on our gender and racialized identities. Our relationship to privilege and oppression affects our experiences, creating protections or additional burdens, so when studying clinician occupational well-being, it seemed important to consider how these disparities play out in the workplace.
Dr. Rowe[/caption]
Susannah G. Rowe, MD, MPH
Office of Equity, Vitality and Inclusion
Boston University Medical Group
Boston Medical Center
Boston University School of Medicine
Boston, Massachusetts
MedicalResearch.com: What is the background for this study?
Response: We wanted to learn how frequently mistreatment occurs for clinicians at work and how it impacts their occupational well-being. We began to see more anecdotal reports of workplace mistreatment of clinicians even before the pandemic. In the extraordinarily stressful environment we are currently experiencing, with people feeling exhausted and emotionally threadbare on some level, the problem appears to be growing.
We also predicted that the burden of mistreatment would not borne be equally. It has often been said that we are all in the same storm but in different boats – some of us are riding out the storm in comfortable ocean liners, while others are paddling in canoes without life jackets. What we are learning, though, is that we are not in fact experiencing the same storm. For example, the increasing intolerance and erosion of public civility we have seen in recent years might show up as minor annoyances for some of us, and actual threats of violence for others depending in large part on our gender and racialized identities. Our relationship to privilege and oppression affects our experiences, creating protections or additional burdens, so when studying clinician occupational well-being, it seemed important to consider how these disparities play out in the workplace. 

 Dr. Clarke[/caption]
Megan Clarke, Ph.D., M.H.S.,
Earl Stadtman Investigator
Division of Cancer Epidemiology and Genetics
National Cancer Institute
MedicalResearch.com: What is the background for this study?
Dr. Clarke[/caption]
Megan Clarke, Ph.D., M.H.S.,
Earl Stadtman Investigator
Division of Cancer Epidemiology and Genetics
National Cancer Institute
MedicalResearch.com: What is the background for this study?

 Dr. Piantino[/caption]
Juan Piantino, M.D., MCR
Assistant Professor of Pediatrics
Division of Neurology, School of Medicine
Director, Inpatient Child Neurology
Oregon Health Sciences University
MedicalResearch.com: What is the background for this study?
Response: Astronauts are exposed to several stressors during spaceflight, including radiation, lack of gravity, and sleep deprivation. The effects of those stressors on the brain remain unknown. Is it safe to travel to space? For how long can humans survive in space? What are the effects of spending months under zero gravity? With more extended missions, and an increased number of civilians traveling to space, there is increased interest in understanding what happens to our brains when we leave earth.
Dr. Piantino[/caption]
Juan Piantino, M.D., MCR
Assistant Professor of Pediatrics
Division of Neurology, School of Medicine
Director, Inpatient Child Neurology
Oregon Health Sciences University
MedicalResearch.com: What is the background for this study?
Response: Astronauts are exposed to several stressors during spaceflight, including radiation, lack of gravity, and sleep deprivation. The effects of those stressors on the brain remain unknown. Is it safe to travel to space? For how long can humans survive in space? What are the effects of spending months under zero gravity? With more extended missions, and an increased number of civilians traveling to space, there is increased interest in understanding what happens to our brains when we leave earth.
 Dr. Ogedegbe[/caption]
MedicalResearch.com Interview with:
Gbenga Ogedegbe, MD, MPH
Dr. Adolph & Margaret Berger Professor of Population Health
Director, Division of Health & Behavior
Director Center for Healthful Behavior Change
Department of Population Health
NYU Langone Health
NYU School of Medicine
Member of the U.S. Preventive Services Task Force
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Heart disease and stroke are the leading causes of mortality in the United States, accounting for more than one in four deaths.
Taking a daily aspirin may help prevent a first heart attack or stroke in some people, but it can also cause some harm, like internal bleeding. The decision on whether or not to start taking a daily aspirin should be based primarily on age, but cardiovascular disease risk, a person’s chances of bleeding, and other factors should also be taken into account.
Dr. Ogedegbe[/caption]
MedicalResearch.com Interview with:
Gbenga Ogedegbe, MD, MPH
Dr. Adolph & Margaret Berger Professor of Population Health
Director, Division of Health & Behavior
Director Center for Healthful Behavior Change
Department of Population Health
NYU Langone Health
NYU School of Medicine
Member of the U.S. Preventive Services Task Force
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Heart disease and stroke are the leading causes of mortality in the United States, accounting for more than one in four deaths.
Taking a daily aspirin may help prevent a first heart attack or stroke in some people, but it can also cause some harm, like internal bleeding. The decision on whether or not to start taking a daily aspirin should be based primarily on age, but cardiovascular disease risk, a person’s chances of bleeding, and other factors should also be taken into account.
 Prof. McManus[/caption]
Richard McManus MA PhD MBBS FRCGP FRCP
Professor of Primary Care
Dr. McManus chairs the Blood Pressure Monitoring Working Party
of the British Hypertension Society
Nuffield Department of Primary Care Health Sciences
MedicalResearch.com: What is the background for this study?
Response: About one in ten people who are pregnant develop high blood pressure and almost half of these go onto to have pre-eclampsia. Many pregnant women and individuals are already measuring their own blood pressure – well over half of those with high blood pressure in a recent large survey in the UK but until recently there were no data to support this.
Prof. McManus[/caption]
Richard McManus MA PhD MBBS FRCGP FRCP
Professor of Primary Care
Dr. McManus chairs the Blood Pressure Monitoring Working Party
of the British Hypertension Society
Nuffield Department of Primary Care Health Sciences
MedicalResearch.com: What is the background for this study?
Response: About one in ten people who are pregnant develop high blood pressure and almost half of these go onto to have pre-eclampsia. Many pregnant women and individuals are already measuring their own blood pressure – well over half of those with high blood pressure in a recent large survey in the UK but until recently there were no data to support this.