MedicalResearch.com Interview with:
[caption id="attachment_56565" align="alignleft" width="200"]

Dr. Devine[/caption]
Gregor J. Devine, Ph.D
Mosquito Control LaboratoryQIMR Berghofer Medical Research Institute
Brisbane, Queensland, Australia
MedicalResearch.com: What is the background for this study?
Scale of the problem: Dengue, Zika and chikungunya are all transmitted by the same mosquito species. That mosquito,
Aedes aegypti, is superbly adapted to the human, urban environment – it lays its eggs and develops in the standing water that collects in the myriad containers associated with modern living (plastic bottles, food packaging, buckets, planters, crumpled tarpaulins etc.). Unusually they rely almost entirely on human blood for their nutritional requirements and they subsequently bite multiple times during each egg laying cycle. That reliance on human blood means that they are usually found resting indoors, a behaviour that also offers them some protection from weather extremes and predators. Once infected, and having incubated the virus until it is transmissible, a mosquito that survives for just a couple of weeks can infect many humans within the same and neighbouring households.
In poorer tropical urban environments with dense human populations, unscreened houses, no air-conditioning, and innumerable rain-filled containers to develop in, Aedes aegypti proliferates and so do those diseases, causing ca 400M annual infections of dengue alone by some estimates. The economic impact of the dengue, which normally causes a high fever, muscle and joint pains and nausea, is pronounced; especially in poor households with few savings and no welfare system. Every year, about 500,000 of those dengue cases develop into severe dengue, or dengue haemorrhagic fever (typified by plasma leakage, severe bleeding and organ impairment). There are about 25,000 deaths annually.

The Zika pandemic of 2015-2016 resulted in 1000s of babies born with microcephaly and damage to their brains and eyes. For 1000s of other children, the impacts of Zika on their cognitive development did not manifest in their first, formative years. Chikungunya is endemic in Asia and Africa but between 2010 and 2014, outbreaks and epidemics spread across the Indian Ocean, the Caribbean, the Americas and the Pacific Islands. It causes severe, often debilitating joint pain in infected patients. Those affected also suffer from headaches, fever, severe muscle pain and conjunctivitis. Joint pain can persist in subacute or chronic form for several months or even years, particularly in older patients. The ubiquity of the mosquito Aedes aegypti across the tropics and sub tropics ensures that further epidemics of Zika and chikungunya will occur, outside their usual ranges. It’s simply impossible to predict when that will occur.



 Dr. Traverso[/caption]
Carlo Giovanni Traverso, MB, BChir, PhD
Associate Physician, Brigham and Women's Hospital
Assistant Professor,
[caption id="attachment_56823" align="alignleft" width="150"]
Dr. Traverso[/caption]
Carlo Giovanni Traverso, MB, BChir, PhD
Associate Physician, Brigham and Women's Hospital
Assistant Professor,
[caption id="attachment_56823" align="alignleft" width="150"] Dr. Chai[/caption]
Peter R. Chai, MD, MMS
Emergency Medicine Physician and Medical Toxicologist
Harvard Medical School
Brigham and Women's Hospital
Department of Medicine
Dr. Chai[/caption]
Peter R. Chai, MD, MMS
Emergency Medicine Physician and Medical Toxicologist
Harvard Medical School
Brigham and Women's Hospital
Department of Medicine
 MedicalResearch.com: What is the background for this study? What are some of the functions that Dr. Spot can facilitate?
Response: During the COVID-19 pandemic, we wanted to consider innovative methods to provide additional social distance for physicians evaluating low acuity individuals who may have COVID-19 disease in the emergency department. While other health systems had instituted processes like evaluating patients from outside of emergency department rooms or calling patients to obtain a history, we considered the use of a mobile robotic system in collaboration with Boston Dynamics to provide telemedicine triage on an agile platform that could be navigated around a busy emergency department. Dr. Spot was built with a camera system to help an operator navigate it through an emergency department into a patient room where an on-board tablet would permit face-to-face triage and assessment of individuals.
MedicalResearch.com: What is the background for this study? What are some of the functions that Dr. Spot can facilitate?
Response: During the COVID-19 pandemic, we wanted to consider innovative methods to provide additional social distance for physicians evaluating low acuity individuals who may have COVID-19 disease in the emergency department. While other health systems had instituted processes like evaluating patients from outside of emergency department rooms or calling patients to obtain a history, we considered the use of a mobile robotic system in collaboration with Boston Dynamics to provide telemedicine triage on an agile platform that could be navigated around a busy emergency department. Dr. Spot was built with a camera system to help an operator navigate it through an emergency department into a patient room where an on-board tablet would permit face-to-face triage and assessment of individuals.



 Dr. Zimmerman[/caption]
Frederick Zimmerman, PhD
Professor, Department of Health Policy and Management
Fielding School of Public Health
UCLA
MedicalResearch.com: What is the background for this study?
Response: The science on school transmissions of COVID is becoming clearer all the time in its conclusion that there is little to no transmission in school environments as long as reasonable precautions are taken. Yet one recent study got a lot of attention for claiming that states that allowed their schools to remain open in the early days of the pandemic saw more cases. That study did not control for several important factors that might explain this association, so our study aimed to correct that work.
Dr. Zimmerman[/caption]
Frederick Zimmerman, PhD
Professor, Department of Health Policy and Management
Fielding School of Public Health
UCLA
MedicalResearch.com: What is the background for this study?
Response: The science on school transmissions of COVID is becoming clearer all the time in its conclusion that there is little to no transmission in school environments as long as reasonable precautions are taken. Yet one recent study got a lot of attention for claiming that states that allowed their schools to remain open in the early days of the pandemic saw more cases. That study did not control for several important factors that might explain this association, so our study aimed to correct that work.



 Dr. Swerlick[/caption]
Robert A. Swerlick, MD
Professor and Alicia Leizman Stonecipher Chair of Dermatology
Emory University School of Medicine
Atlanta, GA 30322
MedicalResearch.com: What is the background for this study?
Response: Financial incentives have the potential to drive provider behavior, even unintentionally. The aim of this study was to evaluate differences in clinic “productivity” measures that occur in outpatient dermatology encounters. Specifically, we used data from 2016-2020 at one academic dermatology practice to evaluate differences in work relative value units (wRVUs, a measure of clinical productivity) and financial reimbursement by patient race, sex, and age. 66,463 encounters were included in this study, among which 70.1% of encounters were for white patients, 59.6% were for females, and the mean age was 55.9 years old.
Dr. Swerlick[/caption]
Robert A. Swerlick, MD
Professor and Alicia Leizman Stonecipher Chair of Dermatology
Emory University School of Medicine
Atlanta, GA 30322
MedicalResearch.com: What is the background for this study?
Response: Financial incentives have the potential to drive provider behavior, even unintentionally. The aim of this study was to evaluate differences in clinic “productivity” measures that occur in outpatient dermatology encounters. Specifically, we used data from 2016-2020 at one academic dermatology practice to evaluate differences in work relative value units (wRVUs, a measure of clinical productivity) and financial reimbursement by patient race, sex, and age. 66,463 encounters were included in this study, among which 70.1% of encounters were for white patients, 59.6% were for females, and the mean age was 55.9 years old.



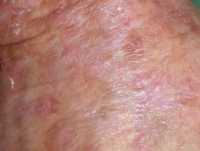
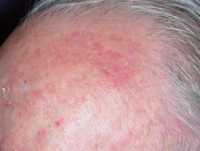 One example of actinic keratoses on scalp
One example of actinic keratoses on scalp



 Elodie Warren[/caption]
Elodie C. Warren, MPH
Columbia University Mailman School of Public Health Graduate
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: We know that the US has been experiencing an opioid crisis for the past two decades. And we know that among communities of color, rates of overdose deaths are continuing to increase, even though overall national rates decreased between 2017 and 2018.
To better understand how the opioid crisis has differently affected racial/ethnic groups, we looked at how heroin treatment admissions changed over time by race/ethnicity, age, and sex. We found that there were stark differences when comparing non-Hispanic Black men and women to non-Hispanic White men and women.
Importantly, our study suggests the existence of an aging cohort of Black men and women (likely including survivors of a heroin epidemic that hit urban areas more than 40 years ago) that continues to struggle with heroin addiction. This points to the need for targeted interventions in chronically underserved communities.
Elodie Warren[/caption]
Elodie C. Warren, MPH
Columbia University Mailman School of Public Health Graduate
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: We know that the US has been experiencing an opioid crisis for the past two decades. And we know that among communities of color, rates of overdose deaths are continuing to increase, even though overall national rates decreased between 2017 and 2018.
To better understand how the opioid crisis has differently affected racial/ethnic groups, we looked at how heroin treatment admissions changed over time by race/ethnicity, age, and sex. We found that there were stark differences when comparing non-Hispanic Black men and women to non-Hispanic White men and women.
Importantly, our study suggests the existence of an aging cohort of Black men and women (likely including survivors of a heroin epidemic that hit urban areas more than 40 years ago) that continues to struggle with heroin addiction. This points to the need for targeted interventions in chronically underserved communities. 


 Dr. Devine[/caption]
Gregor J. Devine, Ph.D
Mosquito Control LaboratoryQIMR Berghofer Medical Research Institute
Brisbane, Queensland, Australia
MedicalResearch.com: What is the background for this study?
Scale of the problem: Dengue, Zika and chikungunya are all transmitted by the same mosquito species. That mosquito, Aedes aegypti, is superbly adapted to the human, urban environment – it lays its eggs and develops in the standing water that collects in the myriad containers associated with modern living (plastic bottles, food packaging, buckets, planters, crumpled tarpaulins etc.). Unusually they rely almost entirely on human blood for their nutritional requirements and they subsequently bite multiple times during each egg laying cycle. That reliance on human blood means that they are usually found resting indoors, a behaviour that also offers them some protection from weather extremes and predators. Once infected, and having incubated the virus until it is transmissible, a mosquito that survives for just a couple of weeks can infect many humans within the same and neighbouring households.
In poorer tropical urban environments with dense human populations, unscreened houses, no air-conditioning, and innumerable rain-filled containers to develop in, Aedes aegypti proliferates and so do those diseases, causing ca 400M annual infections of dengue alone by some estimates. The economic impact of the dengue, which normally causes a high fever, muscle and joint pains and nausea, is pronounced; especially in poor households with few savings and no welfare system. Every year, about 500,000 of those dengue cases develop into severe dengue, or dengue haemorrhagic fever (typified by plasma leakage, severe bleeding and organ impairment). There are about 25,000 deaths annually.
Dr. Devine[/caption]
Gregor J. Devine, Ph.D
Mosquito Control LaboratoryQIMR Berghofer Medical Research Institute
Brisbane, Queensland, Australia
MedicalResearch.com: What is the background for this study?
Scale of the problem: Dengue, Zika and chikungunya are all transmitted by the same mosquito species. That mosquito, Aedes aegypti, is superbly adapted to the human, urban environment – it lays its eggs and develops in the standing water that collects in the myriad containers associated with modern living (plastic bottles, food packaging, buckets, planters, crumpled tarpaulins etc.). Unusually they rely almost entirely on human blood for their nutritional requirements and they subsequently bite multiple times during each egg laying cycle. That reliance on human blood means that they are usually found resting indoors, a behaviour that also offers them some protection from weather extremes and predators. Once infected, and having incubated the virus until it is transmissible, a mosquito that survives for just a couple of weeks can infect many humans within the same and neighbouring households.
In poorer tropical urban environments with dense human populations, unscreened houses, no air-conditioning, and innumerable rain-filled containers to develop in, Aedes aegypti proliferates and so do those diseases, causing ca 400M annual infections of dengue alone by some estimates. The economic impact of the dengue, which normally causes a high fever, muscle and joint pains and nausea, is pronounced; especially in poor households with few savings and no welfare system. Every year, about 500,000 of those dengue cases develop into severe dengue, or dengue haemorrhagic fever (typified by plasma leakage, severe bleeding and organ impairment). There are about 25,000 deaths annually.





 Dr. Kovács[/caption]
Balázs Kovács PhD
Associate Professor of Organizational Behavior
Yale School of Management
MedicalResearch.com: What is the background for this study?
Response: Our study looks at the association between the prevalence of legal cannabis stores, called “dispensaries”, and opioid-related mortality rates in the U.S. We find that higher cannabis dispensary counts are associated with reduced opioid-related mortality rates. We find this relationship holds for both medical dispensaries, which only serve patients who have a state-approved medical card or doctor’s recommendation, as well as for recreational dispensaries, which sell to adults 21 years and older. The statistical associations we find appears most pronounced with the class of opioids that includes fentanyl and its analogs.
Dr. Kovács[/caption]
Balázs Kovács PhD
Associate Professor of Organizational Behavior
Yale School of Management
MedicalResearch.com: What is the background for this study?
Response: Our study looks at the association between the prevalence of legal cannabis stores, called “dispensaries”, and opioid-related mortality rates in the U.S. We find that higher cannabis dispensary counts are associated with reduced opioid-related mortality rates. We find this relationship holds for both medical dispensaries, which only serve patients who have a state-approved medical card or doctor’s recommendation, as well as for recreational dispensaries, which sell to adults 21 years and older. The statistical associations we find appears most pronounced with the class of opioids that includes fentanyl and its analogs. 

 Dr. Silverstein[/caption]
Dr. Michael Silverstein M.D., M.P.H
Professor of Pediatrics
Director of the Division of General Academic Pediatrics
Vice Chair of Research, Department of Pediatrics
Boston University School of Medicine
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Tobacco use is the leading preventable cause of disease, disability, and death in the United States and quitting is one of the best things people can do for their health. Additionally, smoking during pregnancy can cause serious harms to both the pregnant person and the baby.
The Task Force continues to recommend that clinicians ask all adults and pregnant people about their tobacco use, advise those who use tobacco to quit, and connect them to proven, safe methods to help them quit.
Dr. Silverstein[/caption]
Dr. Michael Silverstein M.D., M.P.H
Professor of Pediatrics
Director of the Division of General Academic Pediatrics
Vice Chair of Research, Department of Pediatrics
Boston University School of Medicine
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Tobacco use is the leading preventable cause of disease, disability, and death in the United States and quitting is one of the best things people can do for their health. Additionally, smoking during pregnancy can cause serious harms to both the pregnant person and the baby.
The Task Force continues to recommend that clinicians ask all adults and pregnant people about their tobacco use, advise those who use tobacco to quit, and connect them to proven, safe methods to help them quit. 
