Author Interviews, Health Care Systems, JAMA / 13.02.2023
Georgetown Study Finds Medical Malpractice Is Not Random
MedicalResearch.com Interview with:
[caption id="attachment_60011" align="alignleft" width="150"] David A. Hyman, JD, MD[/caption]
David A. Hyman, JD, MD
The Scott K. Ginsburg Professor of Health Law & Policy
Georgetown University Law Center
Washington, DC
MedicalResearch.com: What is the background for this study?
Response: Many doctors believe medical malpractice claiming is effectively random — meaning good doctors are equally likely as bad doctors to end up being the target of a malpractice claim. Past research has studied whether physicians with 2 paid claims are likely to have another claim than doctors with 1 paid claim.
We study whether physicians with 1 paid claim are more likely to have another paid claim, compared to physicians with zero paid claims. We also compare the pattern of observed claims with what we would expect to find if claiming were truly random (by running a simulation).
David A. Hyman, JD, MD[/caption]
David A. Hyman, JD, MD
The Scott K. Ginsburg Professor of Health Law & Policy
Georgetown University Law Center
Washington, DC
MedicalResearch.com: What is the background for this study?
Response: Many doctors believe medical malpractice claiming is effectively random — meaning good doctors are equally likely as bad doctors to end up being the target of a malpractice claim. Past research has studied whether physicians with 2 paid claims are likely to have another claim than doctors with 1 paid claim.
We study whether physicians with 1 paid claim are more likely to have another paid claim, compared to physicians with zero paid claims. We also compare the pattern of observed claims with what we would expect to find if claiming were truly random (by running a simulation).
 David A. Hyman, JD, MD[/caption]
David A. Hyman, JD, MD
The Scott K. Ginsburg Professor of Health Law & Policy
Georgetown University Law Center
Washington, DC
MedicalResearch.com: What is the background for this study?
Response: Many doctors believe medical malpractice claiming is effectively random — meaning good doctors are equally likely as bad doctors to end up being the target of a malpractice claim. Past research has studied whether physicians with 2 paid claims are likely to have another claim than doctors with 1 paid claim.
We study whether physicians with 1 paid claim are more likely to have another paid claim, compared to physicians with zero paid claims. We also compare the pattern of observed claims with what we would expect to find if claiming were truly random (by running a simulation).
David A. Hyman, JD, MD[/caption]
David A. Hyman, JD, MD
The Scott K. Ginsburg Professor of Health Law & Policy
Georgetown University Law Center
Washington, DC
MedicalResearch.com: What is the background for this study?
Response: Many doctors believe medical malpractice claiming is effectively random — meaning good doctors are equally likely as bad doctors to end up being the target of a malpractice claim. Past research has studied whether physicians with 2 paid claims are likely to have another claim than doctors with 1 paid claim.
We study whether physicians with 1 paid claim are more likely to have another paid claim, compared to physicians with zero paid claims. We also compare the pattern of observed claims with what we would expect to find if claiming were truly random (by running a simulation).

 Dr. Kim[/caption]
Brian S Kim, MD, MTR
Sol and Clara Kest Professor
Vice Chair of Research | Site Chair, Mount Sinai West and Morningside
Director, Mark Lebwohl Center for Neuroinflammation and Sensation
The Kimberly and Eric J. Waldman Department of Dermatology
Precision Immunology Institute | Friedman Brain Institute
Icahn School of Medicine at Mount Sinai
MedicalResearch.com: What is the background for this study?
Response: We generated preliminary data in mice that difelikefalin suppresses itch robustly with very little to no effect on inflammation in a model of atopic dermatitis. This led us to hypothesize that the primary mode of action of difelikefalin must be by direct modulation of sensory neurons to suppress itch and thus would be best suited for a neuropathic itch condition. These are conditions in which itch occurs relatively independently of skin inflammation as in atopic dermatitis due to hyperactive nerves.
Dr. Kim[/caption]
Brian S Kim, MD, MTR
Sol and Clara Kest Professor
Vice Chair of Research | Site Chair, Mount Sinai West and Morningside
Director, Mark Lebwohl Center for Neuroinflammation and Sensation
The Kimberly and Eric J. Waldman Department of Dermatology
Precision Immunology Institute | Friedman Brain Institute
Icahn School of Medicine at Mount Sinai
MedicalResearch.com: What is the background for this study?
Response: We generated preliminary data in mice that difelikefalin suppresses itch robustly with very little to no effect on inflammation in a model of atopic dermatitis. This led us to hypothesize that the primary mode of action of difelikefalin must be by direct modulation of sensory neurons to suppress itch and thus would be best suited for a neuropathic itch condition. These are conditions in which itch occurs relatively independently of skin inflammation as in atopic dermatitis due to hyperactive nerves.

 Dr. Pierce[/caption]
Karen Pierce, Ph.D.
Professor, Department of Neurosciences, UCSD
Co-Director, Autism Center of Excellence, UCSD
MedicalResearch.com: What is the background for this study?
Response: The mean age of ASD diagnosis and eventual treatment remains at ~52 months in the United States1 - years beyond the disorder’s prenatal origins2, and beyond the age when it can be reliably diagnosed in many cases3.
Currently the only way to determine if a child has autism spectrum disorder (ASD) is to receive a developmental evaluation from an experienced clinician (usually a licensed clinical psychologist). There are often long waiting lists, and only a small number of clinicians have the experience required to make early-age (i.e., between 12-36 months) diagnoses of ASD. Thus, there are many places in the country as well as world wide wherein children wait months or years to receive a formal diagnosis due to a lack of available expertise. Moreover, diagnostic evaluations are expensive and usually cost the parent and/or insurance approximately ~$2,000 or more per evaluation. Finally, clinical evaluations usually take between 2-3 hours to complete and result in fatigue for both the parent and toddler.
Eye-tracking, which generates biologically-relevant, objective, and quantifiable metrics of both visual and auditory preference profiles in babies and toddlers in just minutes, is a technology that can dramatically change how ASD is diagnosed.
Dr. Pierce[/caption]
Karen Pierce, Ph.D.
Professor, Department of Neurosciences, UCSD
Co-Director, Autism Center of Excellence, UCSD
MedicalResearch.com: What is the background for this study?
Response: The mean age of ASD diagnosis and eventual treatment remains at ~52 months in the United States1 - years beyond the disorder’s prenatal origins2, and beyond the age when it can be reliably diagnosed in many cases3.
Currently the only way to determine if a child has autism spectrum disorder (ASD) is to receive a developmental evaluation from an experienced clinician (usually a licensed clinical psychologist). There are often long waiting lists, and only a small number of clinicians have the experience required to make early-age (i.e., between 12-36 months) diagnoses of ASD. Thus, there are many places in the country as well as world wide wherein children wait months or years to receive a formal diagnosis due to a lack of available expertise. Moreover, diagnostic evaluations are expensive and usually cost the parent and/or insurance approximately ~$2,000 or more per evaluation. Finally, clinical evaluations usually take between 2-3 hours to complete and result in fatigue for both the parent and toddler.
Eye-tracking, which generates biologically-relevant, objective, and quantifiable metrics of both visual and auditory preference profiles in babies and toddlers in just minutes, is a technology that can dramatically change how ASD is diagnosed.

 Dr. García Cenoz[/caption]
Manuel García Cenoz MD, PhD
Dr. García Cenoz[/caption]
Manuel García Cenoz MD, PhD



 Dr. Caraballo-Cordovez[/caption]
César Caraballo-Cordovez, MD
Dr. Caraballo-Cordovez[/caption]
César Caraballo-Cordovez, MD

 Casey Hribar[/caption]
Casey Hribar
Fourth-year medical student
University of North Carolina
MedicalResearch.com: What is the background for this study?
Response: Several great pieces of literature already exist about patient perception of doctors wearing white coats, formal attire, business attire, and the like. But recently, scrubs are garnering favor, especially as a result of the COVID-19 pandemic.
While there has been some interest in what is worn over scrubs (jackets, vests, name tags, etc.), to our knowledge, there has not been any investigation into scrub color. Scrubs are a highly variable article of clothing, from fit, to pockets, pattern, and color, and it makes sense that these variations could have their own associated perceptions. Our study served as a way to open up the conversation around scrubs and the potential impact of their color on patients.
Casey Hribar[/caption]
Casey Hribar
Fourth-year medical student
University of North Carolina
MedicalResearch.com: What is the background for this study?
Response: Several great pieces of literature already exist about patient perception of doctors wearing white coats, formal attire, business attire, and the like. But recently, scrubs are garnering favor, especially as a result of the COVID-19 pandemic.
While there has been some interest in what is worn over scrubs (jackets, vests, name tags, etc.), to our knowledge, there has not been any investigation into scrub color. Scrubs are a highly variable article of clothing, from fit, to pockets, pattern, and color, and it makes sense that these variations could have their own associated perceptions. Our study served as a way to open up the conversation around scrubs and the potential impact of their color on patients.





 Dr. Goldman[/caption]
Anna L. Goldman, M.D., M.P.A., M.P.H
Assistant Professor of Medicine
General Internal Medicine
Dr. Goldman[/caption]
Anna L. Goldman, M.D., M.P.A., M.P.H
Assistant Professor of Medicine
General Internal Medicine


 Dr. Harris[/caption]
MedicalResearch.com Interview with:
Rebecca Arden Harris, MD, MSc
Assistant Professor of Family Medicine and Community Health at the Hospital of the University of Pennsylvania
Senior Fellow, Leonard Davis Institute of Health Economics
Perelman School of Medicine, University of Pennsylvania
MedicalResearch.com: What is the background for this study?
Response: The impact of the nationwide overdose epidemic on Black women has received little attention from policy-makers, researchers, or the press.
MedicalResearch.com: What are the main findings?
Response: Over the 7-year study period, preventable overdose deaths among Black women resulted in nearly 0.75 million years of life lost (YLL). Women aged 25-34 have suffered a rising proportion of this burden.
Dr. Harris[/caption]
MedicalResearch.com Interview with:
Rebecca Arden Harris, MD, MSc
Assistant Professor of Family Medicine and Community Health at the Hospital of the University of Pennsylvania
Senior Fellow, Leonard Davis Institute of Health Economics
Perelman School of Medicine, University of Pennsylvania
MedicalResearch.com: What is the background for this study?
Response: The impact of the nationwide overdose epidemic on Black women has received little attention from policy-makers, researchers, or the press.
MedicalResearch.com: What are the main findings?
Response: Over the 7-year study period, preventable overdose deaths among Black women resulted in nearly 0.75 million years of life lost (YLL). Women aged 25-34 have suffered a rising proportion of this burden.
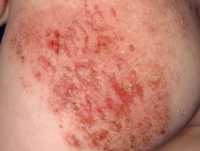
 Dr. Guttman-Yassky[/caption]
Dr. Emma Guttman-Yassky, MD, PhD
Waldman Professor and System Chair
The Kimberly and Eric J. Waldman Department of Dermatology
Director, Center of Excellence in Eczema
Director, Laboratory of Inflammatory Skin Diseases
Icahn School of Medicine at Mount Sinai
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The background for this study are studies that show that OX40 is a pathway that is upregulated in patients with atopic dermatitis (or eczema). OX40 is involved in activation of immune molecules associated with allergy and atopy, and also with formation of memory immune cells that are required for disease recurrence. The hypothesis to the study was that giving an OX40 antagonist will not only ameliorate the disease but perhaps have a remittive effect in that the disease will not come back.
Indeed all drug doses were significantly effective at week 16, the primary endpoint compared to placebo and continued to improve towards week 36, the secondary endpoint. In addition, the responders to treatment maintained their responses for an additional 20 weeks, which is unusual, suggesting a potential for disease modification.
Dr. Guttman-Yassky[/caption]
Dr. Emma Guttman-Yassky, MD, PhD
Waldman Professor and System Chair
The Kimberly and Eric J. Waldman Department of Dermatology
Director, Center of Excellence in Eczema
Director, Laboratory of Inflammatory Skin Diseases
Icahn School of Medicine at Mount Sinai
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The background for this study are studies that show that OX40 is a pathway that is upregulated in patients with atopic dermatitis (or eczema). OX40 is involved in activation of immune molecules associated with allergy and atopy, and also with formation of memory immune cells that are required for disease recurrence. The hypothesis to the study was that giving an OX40 antagonist will not only ameliorate the disease but perhaps have a remittive effect in that the disease will not come back.
Indeed all drug doses were significantly effective at week 16, the primary endpoint compared to placebo and continued to improve towards week 36, the secondary endpoint. In addition, the responders to treatment maintained their responses for an additional 20 weeks, which is unusual, suggesting a potential for disease modification.


 Dr. Simin Liu[/caption]
Simin Liu MD MPH ScD
Professor of Epidemiology at the School of Public Health,
Professor of Medicine (Endocrinology) and
Professor of Surgery at the Alpert School of Medicine
Brown University
MedicalResearch.com: What is the background for this study?
Response: Our research team has been researching the roles of environmental and genetic determinants of chronic diseases for nearly three decades, with special emphasis on evaluating micronutrients, minerals, and trace elements in relation to cardiometabolic outcomes, and findings of which have contributed to the design of several large, randomized trials of dietary supplements in the US (Liu JAMA 1999; 2011; Diabetes Care 2005a,b; Diabetes 2006). Several large intervention trials have consistently shown beneficial effects on clinical cardiometabolic outcomes of a diet pattern rich in micronutrients, although research on micronutrient supplementation has mainly focused on the health effects of a single or a few vitamins and minerals.
We decided to take a comprehensive and systematic approach to evaluate all the publicly available/accessible studies reporting all micronutrients including phytochemicals and antioxidant supplements and their effects on cardiovascular risk factors as well as multiple CVDs.
Dr. Simin Liu[/caption]
Simin Liu MD MPH ScD
Professor of Epidemiology at the School of Public Health,
Professor of Medicine (Endocrinology) and
Professor of Surgery at the Alpert School of Medicine
Brown University
MedicalResearch.com: What is the background for this study?
Response: Our research team has been researching the roles of environmental and genetic determinants of chronic diseases for nearly three decades, with special emphasis on evaluating micronutrients, minerals, and trace elements in relation to cardiometabolic outcomes, and findings of which have contributed to the design of several large, randomized trials of dietary supplements in the US (Liu JAMA 1999; 2011; Diabetes Care 2005a,b; Diabetes 2006). Several large intervention trials have consistently shown beneficial effects on clinical cardiometabolic outcomes of a diet pattern rich in micronutrients, although research on micronutrient supplementation has mainly focused on the health effects of a single or a few vitamins and minerals.
We decided to take a comprehensive and systematic approach to evaluate all the publicly available/accessible studies reporting all micronutrients including phytochemicals and antioxidant supplements and their effects on cardiovascular risk factors as well as multiple CVDs.


 Dr. Kubik[/caption]
Martha Kubik, Ph.D., R.N.
Professor, School of Nursing
College of Health and Human Services
George Mason University
Member, U.S. Preventive Services Task Force
MedicalResearch.com: What is the background for this study?
Response: Obstructive sleep apnea is a health condition in which part or all of a person’s airway gets blocked during sleep, causing their breathing to stop and restart many times. Untreated sleep apnea is associated with heart disease, stroke, and diabetes. However, there is currently very limited evidence on screening people who don’t have signs or symptoms like snoring and excessive daytime sleepiness.
Dr. Kubik[/caption]
Martha Kubik, Ph.D., R.N.
Professor, School of Nursing
College of Health and Human Services
George Mason University
Member, U.S. Preventive Services Task Force
MedicalResearch.com: What is the background for this study?
Response: Obstructive sleep apnea is a health condition in which part or all of a person’s airway gets blocked during sleep, causing their breathing to stop and restart many times. Untreated sleep apnea is associated with heart disease, stroke, and diabetes. However, there is currently very limited evidence on screening people who don’t have signs or symptoms like snoring and excessive daytime sleepiness.



 Dr. Dai[/caption]
Dr. Hongying Daisy Dai, PhD
Professor and Associate Dean of Research
The College of Public Health
University of Nebraska Medical Center.
MedicalResearch.com: What is the background for this study?
Response: Tobacco use landscape has been changing in the United States with fewer combustible cigarette smokers and more e-cigarette and other emerging tobacco users. Nicotine concentration level is a key product characteristic of modern e-cigarette products and high-nicotine vaping devices have recently become available. This study seeks to examine whether biomarkers of exposure to tobacco-related toxicants have changed since 2013 among adult nicotine e-cigarette users, non-nicotine e-cigarette users, and cigarette smokers.
Dr. Dai[/caption]
Dr. Hongying Daisy Dai, PhD
Professor and Associate Dean of Research
The College of Public Health
University of Nebraska Medical Center.
MedicalResearch.com: What is the background for this study?
Response: Tobacco use landscape has been changing in the United States with fewer combustible cigarette smokers and more e-cigarette and other emerging tobacco users. Nicotine concentration level is a key product characteristic of modern e-cigarette products and high-nicotine vaping devices have recently become available. This study seeks to examine whether biomarkers of exposure to tobacco-related toxicants have changed since 2013 among adult nicotine e-cigarette users, non-nicotine e-cigarette users, and cigarette smokers.

 Dr. Shan[/caption]
Zhilei Shan, MD, PhD
Postdoctoral fellow on Nutritional Epidemiology
Harvard T.H. Chan School of Public Health
MedicalResearch.com: What is the background for this study?
Response: Unhealthy sleep behaviors and sleep disturbances are associated with higher risk of multiple diseases and mortality. The current profiles of sleep habits and disturbances, particularly the differences between workdays and free days, are unknown in the contemporary US.
MedicalResearch.com: What are the main findings?
Response: In this nationally representative cross-sectional analysis with 9004 adults aged 20 years or older, differences in sleep patterns between workdays and free days were observed. The mean sleep duration was 7.59 hours on workdays and 8.24 hours on free days (difference, 0.65 hour). The mean sleep and wake times were at 11:02 PM and 6:41 AM, respectively, on workdays and 11:25 PM and 7:41 AM, respectively, on free days (differences, 0.23 hour for sleep time and 1.00 hour for wake time). With regard to sleep disturbances, 30.5% of adults experienced 1 hour or more of sleep debt,46.5% experienced 1 hour or more of social jet lag, 29.8% had trouble sleeping, and 27.2% experienced daytime sleepiness.
Dr. Shan[/caption]
Zhilei Shan, MD, PhD
Postdoctoral fellow on Nutritional Epidemiology
Harvard T.H. Chan School of Public Health
MedicalResearch.com: What is the background for this study?
Response: Unhealthy sleep behaviors and sleep disturbances are associated with higher risk of multiple diseases and mortality. The current profiles of sleep habits and disturbances, particularly the differences between workdays and free days, are unknown in the contemporary US.
MedicalResearch.com: What are the main findings?
Response: In this nationally representative cross-sectional analysis with 9004 adults aged 20 years or older, differences in sleep patterns between workdays and free days were observed. The mean sleep duration was 7.59 hours on workdays and 8.24 hours on free days (difference, 0.65 hour). The mean sleep and wake times were at 11:02 PM and 6:41 AM, respectively, on workdays and 11:25 PM and 7:41 AM, respectively, on free days (differences, 0.23 hour for sleep time and 1.00 hour for wake time). With regard to sleep disturbances, 30.5% of adults experienced 1 hour or more of sleep debt,46.5% experienced 1 hour or more of social jet lag, 29.8% had trouble sleeping, and 27.2% experienced daytime sleepiness.