Facial Fillers Carry Rare But Significant Side Effects and Risks
 Dr. Paskhover[/caption]
Boris Paskhover, MD
Associate Professor,Department of Otolaryngology-Head and Neck Surgery
Rutgers New Jersey Medical School
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Facial fillers include a wide range of cosmetic products used by physicians for augmenting the face. Some fillers are permanent, while others are temporary. Lip filler material is included in this category. Any physician is allowed to perform these procedures but patient’s need to be aware that these are not benign procedures and have some serious complications. It’s important to always go to an experienced facial plastic surgeon, general plastic surgeon or possibly dermatologist for your aesthetic fillers. Our study detailed a decade-long review of FDA reported complications with aesthetic fillers.
Dr. Paskhover[/caption]
Boris Paskhover, MD
Associate Professor,Department of Otolaryngology-Head and Neck Surgery
Rutgers New Jersey Medical School
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Facial fillers include a wide range of cosmetic products used by physicians for augmenting the face. Some fillers are permanent, while others are temporary. Lip filler material is included in this category. Any physician is allowed to perform these procedures but patient’s need to be aware that these are not benign procedures and have some serious complications. It’s important to always go to an experienced facial plastic surgeon, general plastic surgeon or possibly dermatologist for your aesthetic fillers. Our study detailed a decade-long review of FDA reported complications with aesthetic fillers. Dr. Brestoff-Parker[/caption]
Jonathan R. Brestoff-Parker, MD, PhD
PSTP Resident, Clinical Pathology
Department of Pathology & Immunology
Washington University School of Medicine
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Red meat allergy is a recently recognized food allergy in which people experience a delayed allergic response about 3-6 hours after eating red meats that contain the allergen alpha-gal.
Red meat allergy is thought to be caused by tick bites which expose humans to alpha-gal, however other factors that contribute to disease risk are not well described. Alpha-gal looks a lot like the B antigen, which is one of the factors that determines blood type. So we wondered whether people with blood types B or AB are protected from getting red meat allergy. We were amazed when we found that patients who make the B antigen (blood types B or AB) are 5 times less likely to have red meat allergy than patients who do not make the B antigen (blood types O or A).
Dr. Brestoff-Parker[/caption]
Jonathan R. Brestoff-Parker, MD, PhD
PSTP Resident, Clinical Pathology
Department of Pathology & Immunology
Washington University School of Medicine
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Red meat allergy is a recently recognized food allergy in which people experience a delayed allergic response about 3-6 hours after eating red meats that contain the allergen alpha-gal.
Red meat allergy is thought to be caused by tick bites which expose humans to alpha-gal, however other factors that contribute to disease risk are not well described. Alpha-gal looks a lot like the B antigen, which is one of the factors that determines blood type. So we wondered whether people with blood types B or AB are protected from getting red meat allergy. We were amazed when we found that patients who make the B antigen (blood types B or AB) are 5 times less likely to have red meat allergy than patients who do not make the B antigen (blood types O or A). AI Trained Computer Program Can Monitor Health Forums To Detect Adverse Drug Reactions
 Dr. Sarin[/caption]
Kavita Sarin, M.D., Ph.D.
Assistant Professor of Dermatology
Stanford University Medical Center
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Drug reactions occur in the majority of patients undergoing cancer therapies. Half of serious drug reactions are detected after market approval which can result in painful complications and interruption in therapy. Post-market drug surveillance platforms such as FDA monitoring rely on medical publications and physician reporting and take time to identify trends. We sought to determine if we could identify trends in patient discussions in internet health forums to more rapidly identify chemotherapeutic drug reactions. We chose skin reactions as a proof-of-principle because patients can more easily describe what they see on their skin.
Julia Ransohoff, a medical student, and Azadeh Nikfarham, an informatics postdoctoral fellow trained a computer to recognize when a patient undergoing anti-cancer treatment with PD-1 antagonists or EGFR-inhibitors described a drug reaction in their internet forum posts.
Dr. Sarin[/caption]
Kavita Sarin, M.D., Ph.D.
Assistant Professor of Dermatology
Stanford University Medical Center
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Drug reactions occur in the majority of patients undergoing cancer therapies. Half of serious drug reactions are detected after market approval which can result in painful complications and interruption in therapy. Post-market drug surveillance platforms such as FDA monitoring rely on medical publications and physician reporting and take time to identify trends. We sought to determine if we could identify trends in patient discussions in internet health forums to more rapidly identify chemotherapeutic drug reactions. We chose skin reactions as a proof-of-principle because patients can more easily describe what they see on their skin.
Julia Ransohoff, a medical student, and Azadeh Nikfarham, an informatics postdoctoral fellow trained a computer to recognize when a patient undergoing anti-cancer treatment with PD-1 antagonists or EGFR-inhibitors described a drug reaction in their internet forum posts.
Can Probiotics and Fish Oil Supplements During Pregnancy Reduce Childhood Allergies?
Social Media Does Not Displace Face-to-Face Communication With Family and Friends
 Dr. Hall[/caption]
Jeffrey A. Hall, Ph.D.
Associate Professor
The University of Kansas
Relationships and Technology Lab
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The idea that new forms of media displace our face-to-face relationships with close friends and family is an old idea. Two decades ago, when the internet experienced a period of rapid growth, the most recent form of the social displacement hypothesis emerged. Studies from that time ended up finding little to no evidence of displacement by the internet.
The main findings of this study focus on displacement by social media. The first study was conducted with a longitudinal, nationally representative sample of Americans from 2009-2011. This study found that during a period of rapid social media adoption, there was little to no association between adopting and using social media and direct social contact over the three years of the study. Furthermore, using more social media did not result in lowered well-being.
The second study in this paper looked at data from 2015, and found that using social media in a day had little bearing on who people communicated with and how they communicated. That is, passive social media use did not seem to displaced face-to-face communication with close friends and family.
Dr. Hall[/caption]
Jeffrey A. Hall, Ph.D.
Associate Professor
The University of Kansas
Relationships and Technology Lab
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The idea that new forms of media displace our face-to-face relationships with close friends and family is an old idea. Two decades ago, when the internet experienced a period of rapid growth, the most recent form of the social displacement hypothesis emerged. Studies from that time ended up finding little to no evidence of displacement by the internet.
The main findings of this study focus on displacement by social media. The first study was conducted with a longitudinal, nationally representative sample of Americans from 2009-2011. This study found that during a period of rapid social media adoption, there was little to no association between adopting and using social media and direct social contact over the three years of the study. Furthermore, using more social media did not result in lowered well-being.
The second study in this paper looked at data from 2015, and found that using social media in a day had little bearing on who people communicated with and how they communicated. That is, passive social media use did not seem to displaced face-to-face communication with close friends and family. Short-Range Human Travel Helps Trigger and Spread Flu Infections Each Year
 Dr. Chattopadhyay[/caption]
Ishanu Chattopadhyay, PhD
Assistant Professor, Department of Medicine
Section of Hospital Medicine
Institute for Genomics and Systems Biology
University of Chicago
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: It is estimated that flu kills thousands every year in US, some estimates put the yearly death toll to around 30,000 -- that is just in US, and that is irrespective of whether a new virus emerges. But why do waves of the disease sweep the globe every year, as if on a schedule? It had been suggested before that the trigger is a specific change in weather conditions, specifically, when normally humid air turns dry.
In this new study, we explore this question in much greater detail than was possible before, bringing to bear massive amounts data, such as 150 million individual medical histories recorded over the last decade, along with massive climate datasets. What we found was both fascinating, and consequential -- no single factor is responsible wholly, and it requires a complex, yet precise, mix of weather conditions, demographic makeup, socio-economic variables, vaccination coverage, antigenic drift states of the virus, and human traveling habits, among others, to trigger the seasonal epidemic waves.
Quite surprisingly, long range air-travel is far less important compared to short range ground travel. This work attempts to finally settle the lack of consensus in the scientific community on which factors are responsible, as well as each factor’s relative importance.
Dr. Chattopadhyay[/caption]
Ishanu Chattopadhyay, PhD
Assistant Professor, Department of Medicine
Section of Hospital Medicine
Institute for Genomics and Systems Biology
University of Chicago
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: It is estimated that flu kills thousands every year in US, some estimates put the yearly death toll to around 30,000 -- that is just in US, and that is irrespective of whether a new virus emerges. But why do waves of the disease sweep the globe every year, as if on a schedule? It had been suggested before that the trigger is a specific change in weather conditions, specifically, when normally humid air turns dry.
In this new study, we explore this question in much greater detail than was possible before, bringing to bear massive amounts data, such as 150 million individual medical histories recorded over the last decade, along with massive climate datasets. What we found was both fascinating, and consequential -- no single factor is responsible wholly, and it requires a complex, yet precise, mix of weather conditions, demographic makeup, socio-economic variables, vaccination coverage, antigenic drift states of the virus, and human traveling habits, among others, to trigger the seasonal epidemic waves.
Quite surprisingly, long range air-travel is far less important compared to short range ground travel. This work attempts to finally settle the lack of consensus in the scientific community on which factors are responsible, as well as each factor’s relative importance.Focusing On Employment Early Improves Success In Veterans with PTSD
 Dr. Davis[/caption]
Dr. Lori Davis, MD
Research and Development Service, Tuscaloosa Veterans Affairs (VA) Medical Center,
Department of Psychiatry, School of Medicine, University of Alabama, Tuscaloosa
Tuscaloosa, Alabama
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Symptoms of posttraumatic stress disorder (PTSD) interfere with a person’s ability to function at work, making it harder to stay employed and establish oneself in a career. Veterans with PTSD are uniquely challenged given their motivation to serve others, be leaders and not be generally receptive to reaching out for help.
Conventional wisdom about PTSD and employment has traditionally been to first commit to treatment, learn coping skills, manage one’s symptoms and then reintegrate into mainstream employment. However, this view is being transformed by our research that suggests a more assertive recovery-oriented approach to the treatment of PTSD that involves returning to meaningful competitive employment as soon as possible.
This study compared Evidence-based Supported Employment (also known as Individual Placement and Support or IPS) integrated within PTSD treatment teams to the treatment as usual Transitional Work model offered within the VA. This multisite trial demonstrated significantly greater effectiveness of the IPS-supported employment over stepwise, transitional work vocational rehabilitation for Veterans living with chronic PTSD.
Dr. Davis[/caption]
Dr. Lori Davis, MD
Research and Development Service, Tuscaloosa Veterans Affairs (VA) Medical Center,
Department of Psychiatry, School of Medicine, University of Alabama, Tuscaloosa
Tuscaloosa, Alabama
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Symptoms of posttraumatic stress disorder (PTSD) interfere with a person’s ability to function at work, making it harder to stay employed and establish oneself in a career. Veterans with PTSD are uniquely challenged given their motivation to serve others, be leaders and not be generally receptive to reaching out for help.
Conventional wisdom about PTSD and employment has traditionally been to first commit to treatment, learn coping skills, manage one’s symptoms and then reintegrate into mainstream employment. However, this view is being transformed by our research that suggests a more assertive recovery-oriented approach to the treatment of PTSD that involves returning to meaningful competitive employment as soon as possible.
This study compared Evidence-based Supported Employment (also known as Individual Placement and Support or IPS) integrated within PTSD treatment teams to the treatment as usual Transitional Work model offered within the VA. This multisite trial demonstrated significantly greater effectiveness of the IPS-supported employment over stepwise, transitional work vocational rehabilitation for Veterans living with chronic PTSD.
Selfies Distort Your Face and Make Your Nose Look Bigger
 Dr. Paskhover[/caption]
Boris Paskhover, MD
Rutgers New Jersey Medical School
Adjunct Instructor,Department of Otolaryngology-Head and Neck Surgery
NYU Langone Medical Center
MedicalResearch.com: What is the background for this study?
Response: Patient's and the general public routinely mention that their nose appears large, especially when they look at photos taken with their phone. I realized that patients in general are taking selfies more often nowadays. In my training, we routinely would tell patient’s not to use selfies as a marker of how they look, and we instead would take a 5ft distance photograph since we knew that is more realistic. I looked through the medical literature, and it appeared to me that no one had thoroughly discussed why selfies are a bad when evaluating the nose. I contacted a colleague at Stanford who has a PhD with interest in computer graphics and we developed a model for the face/nose.
Dr. Paskhover[/caption]
Boris Paskhover, MD
Rutgers New Jersey Medical School
Adjunct Instructor,Department of Otolaryngology-Head and Neck Surgery
NYU Langone Medical Center
MedicalResearch.com: What is the background for this study?
Response: Patient's and the general public routinely mention that their nose appears large, especially when they look at photos taken with their phone. I realized that patients in general are taking selfies more often nowadays. In my training, we routinely would tell patient’s not to use selfies as a marker of how they look, and we instead would take a 5ft distance photograph since we knew that is more realistic. I looked through the medical literature, and it appeared to me that no one had thoroughly discussed why selfies are a bad when evaluating the nose. I contacted a colleague at Stanford who has a PhD with interest in computer graphics and we developed a model for the face/nose.
 Julia F. van den Berg, PhD
Leiden University, Department of Clinical Psychology
Leiden, The Netherlands
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Caffeine is the most used psychoactive substance worldwide, mostly consumed via coffee, energy drinks, tea and chocolate. Experimental studies have shown that caffeine can negatively affect sleep quality. The timing of caffeine consumption may play a role; the closer to bedtime, the more caffeine consumption is likely to have a negative effect on sleep. We also wondered if chronotype, being a morning or evening person, would make a difference in the effect of caffeine on sleep.
We sent out questionnaires on sleep quality, chronotype, and a detailed questionnaire on type and timing of caffeine use to 880 secondary education students (mean age 21.3 years). We found that for the entire group, the amount of caffeine per week was not associated with sleep quality, regardless of chronotype. However, when we divided the group into subgroups of students who did, and students who did not usually consume caffeine in the evening (after 6PM), we found something interesting. Only for students who did not consume caffeine in the evening (20% of the total sample), a higher total caffeine consumption per week was associated with poorer sleep, in spite of the fact that these students consumed a lot less caffeine per week than the group who did consume caffeine in the evening.
This suggests a self-regulatory mechanism: students who know they are sensitive to caffeine do not drink it in the evening, nevertheless, the caffeinated beverages they drink during the day do affect their sleep.
Julia F. van den Berg, PhD
Leiden University, Department of Clinical Psychology
Leiden, The Netherlands
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Caffeine is the most used psychoactive substance worldwide, mostly consumed via coffee, energy drinks, tea and chocolate. Experimental studies have shown that caffeine can negatively affect sleep quality. The timing of caffeine consumption may play a role; the closer to bedtime, the more caffeine consumption is likely to have a negative effect on sleep. We also wondered if chronotype, being a morning or evening person, would make a difference in the effect of caffeine on sleep.
We sent out questionnaires on sleep quality, chronotype, and a detailed questionnaire on type and timing of caffeine use to 880 secondary education students (mean age 21.3 years). We found that for the entire group, the amount of caffeine per week was not associated with sleep quality, regardless of chronotype. However, when we divided the group into subgroups of students who did, and students who did not usually consume caffeine in the evening (after 6PM), we found something interesting. Only for students who did not consume caffeine in the evening (20% of the total sample), a higher total caffeine consumption per week was associated with poorer sleep, in spite of the fact that these students consumed a lot less caffeine per week than the group who did consume caffeine in the evening.
This suggests a self-regulatory mechanism: students who know they are sensitive to caffeine do not drink it in the evening, nevertheless, the caffeinated beverages they drink during the day do affect their sleep.
Balanced IV Fluids Can Reduce Kidney Damage and Death in Critically Ill Patients
 Dr. Rice[/caption]
Todd W. Rice, MD, MSc
Associate Professor of Medicine
Director, Vanderbilt University Hospital Medical Intensive Care Unit
Division of Allergy, Pulmonary, and Critical Care Medicine
Nashville, TN
MedicalResearch.com: What is the background for this study?
Response: Our study (called the SMART study) evaluates the effects of different types of intravenous fluids used in practice in critically ill patients. It is very similar to the companion study (called the SALT-ED study and published in the same issue) which compares the effects of different types of intravenous fluids on non-critically ill patients admitted to the hospital. Saline is the most commonly used intravenous fluid in critically ill patients. It contains higher levels of sodium and chloride than are present in the human blood. Balanced fluids contain levels of sodium and chloride closer to those seen in human blood.
Large observational studies and studies in animals have suggested that the higher sodium and chloride content in saline may cause or worsen damage to the kidney or cause death. Only a few large studies have been done in humans and the results are a bit inconclusive.
Dr. Rice[/caption]
Todd W. Rice, MD, MSc
Associate Professor of Medicine
Director, Vanderbilt University Hospital Medical Intensive Care Unit
Division of Allergy, Pulmonary, and Critical Care Medicine
Nashville, TN
MedicalResearch.com: What is the background for this study?
Response: Our study (called the SMART study) evaluates the effects of different types of intravenous fluids used in practice in critically ill patients. It is very similar to the companion study (called the SALT-ED study and published in the same issue) which compares the effects of different types of intravenous fluids on non-critically ill patients admitted to the hospital. Saline is the most commonly used intravenous fluid in critically ill patients. It contains higher levels of sodium and chloride than are present in the human blood. Balanced fluids contain levels of sodium and chloride closer to those seen in human blood.
Large observational studies and studies in animals have suggested that the higher sodium and chloride content in saline may cause or worsen damage to the kidney or cause death. Only a few large studies have been done in humans and the results are a bit inconclusive.
For Most Patients Balanced IV Fluids Better Than Saline
 Dr. Self[/caption]
Wesley H. Self, MD, MPH
Associate Professor
Department of Emergency Medicine
Vanderbilt University Medical Center
Nashville, TN
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Doctors have been giving IV fluids to patients for more than 100 years. The most common IV fluid during this time has been saline; it has high levels of sodium and chloride in it (similar to table salt). Balanced fluids are an alternative type of IV fluid that has lower levels of sodium and chloride that are more similar to human blood.
Our studies were designed to see if treating patients with these balanced fluids resulted in better outcomes than saline. We found that patients treated with balanced fluids had lower rates of death and kidney damage than patients treated with saline.
Dr. Self[/caption]
Wesley H. Self, MD, MPH
Associate Professor
Department of Emergency Medicine
Vanderbilt University Medical Center
Nashville, TN
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Doctors have been giving IV fluids to patients for more than 100 years. The most common IV fluid during this time has been saline; it has high levels of sodium and chloride in it (similar to table salt). Balanced fluids are an alternative type of IV fluid that has lower levels of sodium and chloride that are more similar to human blood.
Our studies were designed to see if treating patients with these balanced fluids resulted in better outcomes than saline. We found that patients treated with balanced fluids had lower rates of death and kidney damage than patients treated with saline.
How Does Hip-Hop/Rap Music Influence Molly/Ecstasy Use in African Americans?
 Dr. Rigg[/caption]
Khary Rigg, Ph.D.
Assistant Professor
Department of Mental Health Law & Policy
University of South Florida
MedicalResearch.com: What is the background for this study?
Response: Over the past two decades, the demographic profile of MDMA (ecstasy/molly) users has changed. In particular, African American MDMA use has risen in some cities. One possible explanation of this new trend is the drug’s recent popularity (as molly) in hip-hop/rap (HHR) music. Several top rappers endorse the drug as a way to have fun or get women “loose.” There are currently no studies, however, that investigate the extent to which African American MDMA users listen to. hip-hop/rap music or the influence that these pro-MDMA messages have on their use of the drug.
This study used survey and interview data to identify the extent to which hip-hop/rap music is listened to by African American MDMA users and assess the perceived influence of HHR music on their decision to begin using.
Dr. Rigg[/caption]
Khary Rigg, Ph.D.
Assistant Professor
Department of Mental Health Law & Policy
University of South Florida
MedicalResearch.com: What is the background for this study?
Response: Over the past two decades, the demographic profile of MDMA (ecstasy/molly) users has changed. In particular, African American MDMA use has risen in some cities. One possible explanation of this new trend is the drug’s recent popularity (as molly) in hip-hop/rap (HHR) music. Several top rappers endorse the drug as a way to have fun or get women “loose.” There are currently no studies, however, that investigate the extent to which African American MDMA users listen to. hip-hop/rap music or the influence that these pro-MDMA messages have on their use of the drug.
This study used survey and interview data to identify the extent to which hip-hop/rap music is listened to by African American MDMA users and assess the perceived influence of HHR music on their decision to begin using.
Labor Costs Account For Largest Percentage of Operating Room Expenses
 Dr. Childers[/caption]
Dr. Chris Childers, M.D.
Division of General Surgery
David Geffen School of Medicine at UCLA
Los Angeles, CA 90095
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Over 20 million Americans undergo a surgical procedure each year with a price tag over $1 trillion. The operating room (OR) is a particularly resource dense environment, yet little is known about the actual costs of running an OR. Most previous efforts focusing on OR costs have come from single-site studies with little detail about the drivers of OR costs.
Using financial statements from all California hospitals we estimated that the average cost to the hospital for one minute of OR time was between $36 and $37. Perhaps more notable was the composition of these costs. Almost two-thirds ($20-21) was attributable to “direct costs” - those generated by the OR itself - including $14 for the wages and benefits of staff, $2.50-3.50 for surgical supplies, and $3 for “other” costs such as equipment repair and depreciation. Interestingly, the remainder ($14-16) was dedicated to “indirect costs” such as the costs associated with hospital security and parking. While these indirect costs are necessary for a hospital to run, they are not under the purview of the operating room.
Finally, we also learned that OR costs have increased quickly over the past 10 years – faster than other sectors of healthcare as well as the rest of the economy.
Dr. Childers[/caption]
Dr. Chris Childers, M.D.
Division of General Surgery
David Geffen School of Medicine at UCLA
Los Angeles, CA 90095
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Over 20 million Americans undergo a surgical procedure each year with a price tag over $1 trillion. The operating room (OR) is a particularly resource dense environment, yet little is known about the actual costs of running an OR. Most previous efforts focusing on OR costs have come from single-site studies with little detail about the drivers of OR costs.
Using financial statements from all California hospitals we estimated that the average cost to the hospital for one minute of OR time was between $36 and $37. Perhaps more notable was the composition of these costs. Almost two-thirds ($20-21) was attributable to “direct costs” - those generated by the OR itself - including $14 for the wages and benefits of staff, $2.50-3.50 for surgical supplies, and $3 for “other” costs such as equipment repair and depreciation. Interestingly, the remainder ($14-16) was dedicated to “indirect costs” such as the costs associated with hospital security and parking. While these indirect costs are necessary for a hospital to run, they are not under the purview of the operating room.
Finally, we also learned that OR costs have increased quickly over the past 10 years – faster than other sectors of healthcare as well as the rest of the economy.Collaborative Heart Failure Care Did Not Reduce Hospitalizations or Mortality, But Reduced Depression and Fatigue
 Dr. Bekelman[/caption]
David Bekelman, MD, MPH
Associate Professor of Medicine and Nursing
Eastern Colorado Health Care System, Department of Veterans Affairs, Denver, CO
University of Colorado School of Medicine at the Anschutz Medical Campus, Aurora, CO
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Many of the 5.8 million Americans with heart failure live with bothersome symptoms, reduced function and poor quality of life. Improving their care is important because many people with heart failure live with these challenges for years.
Dr. Bekelman[/caption]
David Bekelman, MD, MPH
Associate Professor of Medicine and Nursing
Eastern Colorado Health Care System, Department of Veterans Affairs, Denver, CO
University of Colorado School of Medicine at the Anschutz Medical Campus, Aurora, CO
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Many of the 5.8 million Americans with heart failure live with bothersome symptoms, reduced function and poor quality of life. Improving their care is important because many people with heart failure live with these challenges for years.
This study evaluated the effect of a team intervention, Collaborative Care to Alleviate Symptoms and Adjust to Illness, also called CASA, on several aspects of quality of life in 314 patients with heart failure. The patients, who received care at diverse health systems in Colorado, were randomized to receive usual care or usual care supplemented with the CASA intervention, which included a nurse and a social worker who collaborated with a primary care provider, cardiologist, and palliative care physician to address the patients’ needs.
The study found that the CASA intervention did not influence the primary outcome of heart failure health status, yet did improve patients’ depression and fatigue. CASA did not influence number of patient hospitalizations or mortality.
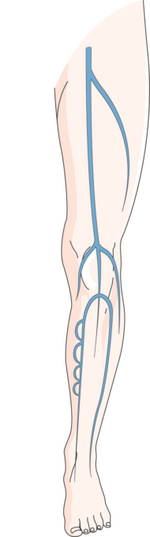
Varicose Veins Associated With Increased Risk of Deep Vein Blood Clots
 Shyueluen Chang[/caption]
Shyueluen Chang MD
Phlebologist with Dermatologist background
Vein Clinic, Department of Dermatology,
Chang Gung Memorial Hospital
Taoyuan, Taiwan
MedicalResearch.com: What is the background for this study?
Response: Varicose veins are common, with about 23 percent of U.S. adults having the condition, but they are rarely thought to be associated with serious health risks.
In contrast, venous thrombosis (DVT), pulmonary embolism (PE), and peripheral artery disease (PAD) are also vascular diseases that are associated with serious systemic effects. Not much is known about varicose veins and the risk of other vascular diseases. Elucidating potential associations between varicose veins and health-threatening diseases is important.
Partner's note: Understanding the broader impact of vascular diseases can provide valuable insights into the risks associated with varicose veins.
Shyueluen Chang[/caption]
Shyueluen Chang MD
Phlebologist with Dermatologist background
Vein Clinic, Department of Dermatology,
Chang Gung Memorial Hospital
Taoyuan, Taiwan
MedicalResearch.com: What is the background for this study?
Response: Varicose veins are common, with about 23 percent of U.S. adults having the condition, but they are rarely thought to be associated with serious health risks.
In contrast, venous thrombosis (DVT), pulmonary embolism (PE), and peripheral artery disease (PAD) are also vascular diseases that are associated with serious systemic effects. Not much is known about varicose veins and the risk of other vascular diseases. Elucidating potential associations between varicose veins and health-threatening diseases is important.
Partner's note: Understanding the broader impact of vascular diseases can provide valuable insights into the risks associated with varicose veins.
How Old is Old?
 William Chopik PhD
Department of Psychology
Michigan State University
East Lansing, MI
MedicalResearch.com: What is the background for this study?
Response: The motivation for the study was that we saw a lot of differences in the way people defined "old age". We also noticed that there is a stigma that goes along with being old. So we had a natural curiosity to see how these perceptions my change as people age.
As people aged, the tended to report feeling younger and consider an older adult as "always in the future"--never quite where they are now.
We found that our results confirmed a lot of existing theories about how our attitudes toward aging change as we age ourselves.
William Chopik PhD
Department of Psychology
Michigan State University
East Lansing, MI
MedicalResearch.com: What is the background for this study?
Response: The motivation for the study was that we saw a lot of differences in the way people defined "old age". We also noticed that there is a stigma that goes along with being old. So we had a natural curiosity to see how these perceptions my change as people age.
As people aged, the tended to report feeling younger and consider an older adult as "always in the future"--never quite where they are now.
We found that our results confirmed a lot of existing theories about how our attitudes toward aging change as we age ourselves.
Decision Aids Can Help Heart Failure Patients Determine If They Want an LVAD
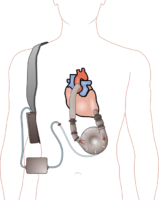 A left ventricular assist device (LVAD) pumping blood from the left ventricle to the aorta, connected to an externally worn control unit and battery pack.
A left ventricular assist device (LVAD) pumping blood from the left ventricle to the aorta, connected to an externally worn control unit and battery pack.Wikipedia image[/caption] Larry A. Allen, MD, MHS Associate Professor, Medicine Associate Head for Clinical Affairs, Cardiology Medical Director, Advanced Heart Failure Aurora, CO 80045 MedicalResearch.com: What is the background for this study? What are the main findings? Response: Deciding whether or not to get a left ventricular assist device (LVAD) is one of the most challenging medical decisions created by modern medicine. LVADs improve overall survival but also come with serious risks and lifestyle changes. Particularly for older patients with multiple medical problems, this is a complex choice. Our research group at the University of Colorado spent years systematically developing unbiased pamphlet and video decision aids for patients and caregivers. We also developed a clinician-directed decision support training for LVAD program staff. The DECIDE-LVAD trial studied the implementation and effectiveness of this decision support intervention with patients and their caregivers in 6 hospitals in the U.S. When compared to previously used education materials, the decision aids appeared to improve patients’ decision quality and lowered the total number of patients getting LVADs.
Genetic Variant of p53 Associated With Poor Breast Cancer Survival
Standardization and Collaboration Reduced Use of Costly CRRT Treatment for Critically Ill Patients
 Dr. Alban[/caption]
Rodrigo F. Alban, MD FACS
Associate Director Performance Improvement
Associate Residency Program Director
NSQIP Surgeon Champion
Department of Surgery
Cedars-Sinai Medical Center
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Continuous Renal Replacement Therapy (CRRT) is a modality of hemodialysis commonly used to manage renal failure in critically ill patients who have significant hemodynamic compromise. However, it is also resource-intensive and costly and its usage is highly variable and lacks standardization.
Our institution organized a multidisciplinary task force to target high value care in critically ill patients requiring CRRT by standardizing its process flow, promoting cross-disciplinary discussions with patients and family members, and increasing visibility/awareness of CRRT use. After our interventions, the mean duration of CRRT decreased by 11.3% from 7.43 to 6.59 days per patient. We also saw a 9.8% decrease in the mean direct cost of CRRT from $11642 to $10506 per patient. Finally, we also saw a decrease in the proportion of patients expiring on CRRT, and an increase in the proportion of patients transitioning to comfort care.
Dr. Alban[/caption]
Rodrigo F. Alban, MD FACS
Associate Director Performance Improvement
Associate Residency Program Director
NSQIP Surgeon Champion
Department of Surgery
Cedars-Sinai Medical Center
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Continuous Renal Replacement Therapy (CRRT) is a modality of hemodialysis commonly used to manage renal failure in critically ill patients who have significant hemodynamic compromise. However, it is also resource-intensive and costly and its usage is highly variable and lacks standardization.
Our institution organized a multidisciplinary task force to target high value care in critically ill patients requiring CRRT by standardizing its process flow, promoting cross-disciplinary discussions with patients and family members, and increasing visibility/awareness of CRRT use. After our interventions, the mean duration of CRRT decreased by 11.3% from 7.43 to 6.59 days per patient. We also saw a 9.8% decrease in the mean direct cost of CRRT from $11642 to $10506 per patient. Finally, we also saw a decrease in the proportion of patients expiring on CRRT, and an increase in the proportion of patients transitioning to comfort care.
Both Vegetarian and Mediterranean Diets Beneficial for Weight Loss and Heart Health
 Francesco Sofi, MD PhD
Department of Experimental and Clinical Medicine
University of Florence, Florence, Italy; Clinical Nutrition Unit, Careggi University Hospital
Don Carlo Gnocchi Foundation Italy, Onlus IRCCS
Florence, Italy
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Mediterranean and Vegetarian diets are two of the most beneficial dietary patterns for prevention of chronic degenerative diseases.
No studies have been conducted in the same group of subjects, by comparing these two dietary profiles.
Main results are that both diets have been found to be beneficial for cardiovascular prevention, in the same group of subjects at low risk of cardiovascular disease.
In particular, vegetarian diet determined a reduction of total and LDL-cholesterol, whereas Mediterranean diet resulted in lower levels of triglycerides and some inflammatory parameters
Francesco Sofi, MD PhD
Department of Experimental and Clinical Medicine
University of Florence, Florence, Italy; Clinical Nutrition Unit, Careggi University Hospital
Don Carlo Gnocchi Foundation Italy, Onlus IRCCS
Florence, Italy
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Mediterranean and Vegetarian diets are two of the most beneficial dietary patterns for prevention of chronic degenerative diseases.
No studies have been conducted in the same group of subjects, by comparing these two dietary profiles.
Main results are that both diets have been found to be beneficial for cardiovascular prevention, in the same group of subjects at low risk of cardiovascular disease.
In particular, vegetarian diet determined a reduction of total and LDL-cholesterol, whereas Mediterranean diet resulted in lower levels of triglycerides and some inflammatory parameters
Heart Attacks Rarely Misdiagnosed in Emergency Rooms
 Daniel A. Waxman, MD, PhD
Department of Emergency Medicine
David Geffen School of Medicine
University of California, Los Angeles
RAND Corporation Santa Monica, California
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: When people talk about medical error, they are usually referring to treatment error—giving the wrong medication, operating on the wrong side of the body, etc. But many believe that diagnostic error—the failure to diagnose a condition when a patient seeks care—is at least as widespread and consequential a problem. However, diagnostic errors are intrinsically difficult to measure, since one can rarely prove that a condition was present at the time it was not diagnosed.
In this study, we introduce a novel method for measuring how often patients who come to the emergency room with symptoms of an imminent cardiovascular emergency such as acute myocardial infarction (heart attack) are discharged home without a diagnosis.
We find that among Medicare patients whose ER visits were attributable to symptoms of an imminent infarction, only about 2.3% were discharged home, and that the figure was under 5% for each of the other four conditions we studied. However, we also found that these relatively low rates did not improve between 2007 and 2014.
Daniel A. Waxman, MD, PhD
Department of Emergency Medicine
David Geffen School of Medicine
University of California, Los Angeles
RAND Corporation Santa Monica, California
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: When people talk about medical error, they are usually referring to treatment error—giving the wrong medication, operating on the wrong side of the body, etc. But many believe that diagnostic error—the failure to diagnose a condition when a patient seeks care—is at least as widespread and consequential a problem. However, diagnostic errors are intrinsically difficult to measure, since one can rarely prove that a condition was present at the time it was not diagnosed.
In this study, we introduce a novel method for measuring how often patients who come to the emergency room with symptoms of an imminent cardiovascular emergency such as acute myocardial infarction (heart attack) are discharged home without a diagnosis.
We find that among Medicare patients whose ER visits were attributable to symptoms of an imminent infarction, only about 2.3% were discharged home, and that the figure was under 5% for each of the other four conditions we studied. However, we also found that these relatively low rates did not improve between 2007 and 2014.
Despite Advancing Neonatal Health, Preterm Babies Still Risk Cognitive Impairment
 Sabrina Twilhaar[/caption]
Sabrina Twilhaar, MS, PhD candidate
Child Study Group, sectie Klinische Neuropsychologie
Vrije Universiteit Amsterdam
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: It is well-known that preterm birth has negative consequences for cognitive development.
During the early 1990s important progress in neonatal health care resulted in a considerable increase in the survival of preterm infants. Earlier meta-analyses showed large differences in intelligence between very preterm and full-term born children. However, these meta-analyses included mostly studies on children born before 1990. Because of the advances in neonatal health care since that time, it was important to update our knowledge on the outcomes of more recently born preterm infants. We combined the results of 71 studies, together including 7752 very preterm and 5155 full-term born children, and found a difference in intelligence between very preterm and full-term children that was still large.
Interestingly, despite advancing neonatal health care, we also found no indication of improvement in the cognitive outcomes of very preterm born children during the period from 1990 to 2008. In addition, we searched for factors that increase the risk for poor cognitive outcomes in these children and we found that children with a chronic lung disease that is amongst others caused by mechanical ventilation of the immature lungs are even more at risk for poor cognitive outcomes.
Sabrina Twilhaar[/caption]
Sabrina Twilhaar, MS, PhD candidate
Child Study Group, sectie Klinische Neuropsychologie
Vrije Universiteit Amsterdam
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: It is well-known that preterm birth has negative consequences for cognitive development.
During the early 1990s important progress in neonatal health care resulted in a considerable increase in the survival of preterm infants. Earlier meta-analyses showed large differences in intelligence between very preterm and full-term born children. However, these meta-analyses included mostly studies on children born before 1990. Because of the advances in neonatal health care since that time, it was important to update our knowledge on the outcomes of more recently born preterm infants. We combined the results of 71 studies, together including 7752 very preterm and 5155 full-term born children, and found a difference in intelligence between very preterm and full-term children that was still large.
Interestingly, despite advancing neonatal health care, we also found no indication of improvement in the cognitive outcomes of very preterm born children during the period from 1990 to 2008. In addition, we searched for factors that increase the risk for poor cognitive outcomes in these children and we found that children with a chronic lung disease that is amongst others caused by mechanical ventilation of the immature lungs are even more at risk for poor cognitive outcomes.
Mammograms Reduce Mortality From Higher Grade Breast Cancers
 Prof. Duffy[/caption]
Prof. Duffy[/caption]
Stephen W. Duffy Professor of Cancer Screening Wolfson Institute of Preventive Medicine, Barts and The London School of Medicine and Dentistry Queen Mary University of London
MedicalResearch.com: What is the background for this study? What are the main findings? Response: The phenomenon of length bias, whereby screening has more chance of detecting slow growing tumours, has been known about for some years. This has led some colleagues to speculate that breast cancer screening only benefits those with slow-growing, less aggressive cancers, and does not reduce deaths from more aggressive, rapidly progressing cancers. In this study, we addressed this question directly using data from a randomised trial of mammographic screening. We calculated the reduction in mortality from grade 1 (less aggressive), grade 2 (intermediate) and grade 3 (most aggressive) cancers, as a result of screening. We found that the greatest reduction in breast cancer mortality was from the aggressive, fast-growing grade 3 cancers, contrary to what had been suspected.Kids with Kidney Disease Likely To Experience Lower IQ and Educational Outcomes Into Adulthood
 L-R: Kerry Chen, Anita van Zwieten, Madeleine Didsbury, Germaine Wong[/caption]
Dr. Kerry Chen
Centre for Kidney Research, The Kids Research Institute
The Children’s Hospital at Westmead, Sydney School of Public Health,
The University of Sydney
Sydney, New South Wales, Australia
MedicalResearch.com: What is the background for this study?
Response: Chronic kidney disease is a major public health issue, with end-stage disease often requiring a combination of complex medication regimens, dialysis and/or transplant surgery. In children, the major causes of CKD are genetic and congenital. The consequences of CKD in children can be long-term and debilitating especially as they transition into adulthood, affecting their physical, intellectual and emotional well-being.
To better understand these changes, the Kids Health and Wealth Study (KCAD) is the largest longitudinal cohort study of children and adolescents with CKD in Australia and New Zealand. Spread across 5 paediatric nephrology centres so far, the KCAD Study takes a life-course approach to collecting and analysing data pertaining to the interactions between reduced renal function and associated clinical, socio-economic, quality of life, psychological, cognitive and educational outcomes in children, especially as they progress in CKD stage and also as they transition into adulthood.
L-R: Kerry Chen, Anita van Zwieten, Madeleine Didsbury, Germaine Wong[/caption]
Dr. Kerry Chen
Centre for Kidney Research, The Kids Research Institute
The Children’s Hospital at Westmead, Sydney School of Public Health,
The University of Sydney
Sydney, New South Wales, Australia
MedicalResearch.com: What is the background for this study?
Response: Chronic kidney disease is a major public health issue, with end-stage disease often requiring a combination of complex medication regimens, dialysis and/or transplant surgery. In children, the major causes of CKD are genetic and congenital. The consequences of CKD in children can be long-term and debilitating especially as they transition into adulthood, affecting their physical, intellectual and emotional well-being.
To better understand these changes, the Kids Health and Wealth Study (KCAD) is the largest longitudinal cohort study of children and adolescents with CKD in Australia and New Zealand. Spread across 5 paediatric nephrology centres so far, the KCAD Study takes a life-course approach to collecting and analysing data pertaining to the interactions between reduced renal function and associated clinical, socio-economic, quality of life, psychological, cognitive and educational outcomes in children, especially as they progress in CKD stage and also as they transition into adulthood.
Salivary Assay Developed for HIV Can Be Used To Detect Zika
 Researchers at NYU College of Dentistry are developing a test for Zika virus that uses saliva to identify diagnostic markers of the virus in a fraction of the time of current tests.
Researchers at NYU College of Dentistry are developing a test for Zika virus that uses saliva to identify diagnostic markers of the virus in a fraction of the time of current tests.NYU/Sapna Parikh[/caption] Maite Sabalza Ph.D Post Doctoral Associate Department of Basic Science and Craniofacial Biology College of Dentistry, New York University New York, NY 10010 MedicalResearch.com: What is the background for this study? What are the main findings? Response: With previous NIH funding we were able to develop an automated “dual assay” (able to detect both host antibodies and viral RNA) for HIV. In relatively short time, we were able to migrate those findings into the new assay for ZIKA Virus.
Repeated Less Serious Infections Do Not Affect Children’s School Performance
 Ole Köhler-Forsberg[/caption]
Ole Köhler-Forsberg, PhD Student
Department of Clinical Medicine - Psychosis Research Unit
Aarhus University
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Prior studies have demonstrated that serious illnesses, for example severe infections such as measles, rubella or meningitis, which we vaccinate against, affect the brain and thereby the child's ability to learn. From this we know that illnesses and in particular infections to some degree have an influence on our brains.
In this study, we decided to look at how children perform following the less severe infections that many of them frequently experience during their childhood. After all, this is the largest group of children, but this has not been studied previously in such a large population.
Basically, we found that among 598,553 Danes born 1987-1997, the less severe infections treated with anti-infective agents during childhood did not affect the child´s ability to perform well in school, nonetheless whether 5, 10 or 15 prescriptions had been prescribed.
On the other hand, we found that children who had been admitted to hospital as a result of severe infections had a lower chance of completing 9th grade. The decisive factor is therefore the severity of the disease, but not necessarily the number of sick days.
Ole Köhler-Forsberg[/caption]
Ole Köhler-Forsberg, PhD Student
Department of Clinical Medicine - Psychosis Research Unit
Aarhus University
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Prior studies have demonstrated that serious illnesses, for example severe infections such as measles, rubella or meningitis, which we vaccinate against, affect the brain and thereby the child's ability to learn. From this we know that illnesses and in particular infections to some degree have an influence on our brains.
In this study, we decided to look at how children perform following the less severe infections that many of them frequently experience during their childhood. After all, this is the largest group of children, but this has not been studied previously in such a large population.
Basically, we found that among 598,553 Danes born 1987-1997, the less severe infections treated with anti-infective agents during childhood did not affect the child´s ability to perform well in school, nonetheless whether 5, 10 or 15 prescriptions had been prescribed.
On the other hand, we found that children who had been admitted to hospital as a result of severe infections had a lower chance of completing 9th grade. The decisive factor is therefore the severity of the disease, but not necessarily the number of sick days.
New Vaccine Administered To Newborns Protects Against Rotavirus Gastroenteritis
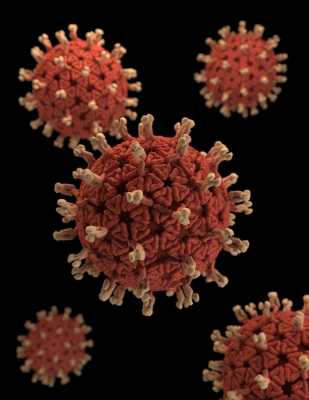 This illustration provides a 3D graphical representation of a number of Rotavirus virions set against a black background. Note the organism’s characteristic wheel-like appearance, which is visible when viewed under the electron microscope. It’s this morphology that gives the Rotavirus its name, which is derived from the Latin rota, meaning "wheel". Rotaviruses are nonenveloped, double-shelled viruses, making them quite stable in the environment.
This illustration provides a 3D graphical representation of a number of Rotavirus virions set against a black background. Note the organism’s characteristic wheel-like appearance, which is visible when viewed under the electron microscope. It’s this morphology that gives the Rotavirus its name, which is derived from the Latin rota, meaning "wheel". Rotaviruses are nonenveloped, double-shelled viruses, making them quite stable in the environment.CDC- PHIL collection: Illustrator: Alissa Eckert[/caption] Professor Julie Bines Inaugural Victor and Loti Smorgon Professor of Paediatrics and Deputy Head of Department of Paediatrics University of Melbourne. Murdoch Childrens Research Institute MedicalResearch.com: What is the background for this study? Would you briefly explain the significance of Rotavirus infections? Diarrhoea is one of the leading causes of child illness and death, and rotavirus is the most common cause of severe diarrhoea. Globally rotaviruses cause approximately 215,000 deaths in children under five years. This disease doesn’t discriminate – it infects children worldwide under the age of five – irrespective of what environment you live in. The rotavirus vaccines that are currently available work very well in places like Australia, the US and Europe but they don’t seem to work as well in low income settings in Africa and Asia where severe gastroenteritis is common and many children die. In a world-first clinical trial conducted in Indonesia, the oral RV3-BB vaccine was administered to babies within their first five days of life. Current rotavirus vaccines can only be administered to children older than six weeks, which leaves newborn babies particularly vulnerable to rotavirus infection. In lower resource settings, birth is often the best contact between mother, baby and health services. The oral RV3-BB vaccine was developed from the human neonatal rotavirus strain RV3 identified in the stool of healthy newborn babies. It does not naturally cause diarrhoea like other rotaviruses. The RV3-BB vaccine program aims to take advantage of the characteristics of this novel strain to target a birth dose vaccination strategy.
USPSTF: Ovarian Cancer Screening Not Recommended in Low-Risk, Asymptomatic Women
 Dr. Barry[/caption]
Michael J. Barry, M.D., Task Force member
Director of the Informed Medical Decisions Program
Health Decision Sciences Center
Massachusetts General Hospital.
Professor of Medicine
Harvard Medical School and
Physician at Massachusetts General Hospital
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Ovarian cancer is the fifth leading cause of cancer death among women in the United States. It is hard to detect, and many women diagnosed with ovarian cancer do not show signs or symptoms early on. As a result, ovarian cancer is often diagnosed at a late stage, when it is hard to treat successfully.
The U.S. Preventive Services Task Force looked at the latest evidence to see if screening women who do not have signs or symptoms of ovarian cancer can prevent them from dying of the disease. Unfortunately, we found that screening for ovarian cancer does not decrease the number of women who die, but it does lead to some women having unnecessary surgery to remove their ovaries. As a result, we are recommending against ovarian cancer screening in women who are not at high risk.
Dr. Barry[/caption]
Michael J. Barry, M.D., Task Force member
Director of the Informed Medical Decisions Program
Health Decision Sciences Center
Massachusetts General Hospital.
Professor of Medicine
Harvard Medical School and
Physician at Massachusetts General Hospital
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Ovarian cancer is the fifth leading cause of cancer death among women in the United States. It is hard to detect, and many women diagnosed with ovarian cancer do not show signs or symptoms early on. As a result, ovarian cancer is often diagnosed at a late stage, when it is hard to treat successfully.
The U.S. Preventive Services Task Force looked at the latest evidence to see if screening women who do not have signs or symptoms of ovarian cancer can prevent them from dying of the disease. Unfortunately, we found that screening for ovarian cancer does not decrease the number of women who die, but it does lead to some women having unnecessary surgery to remove their ovaries. As a result, we are recommending against ovarian cancer screening in women who are not at high risk.
Teen Marijuana Use Did Not Increase After Passage of Medical Marijuana Laws
 Professor Deborah Hasin PhD
Department of Epidemiology in Psychiatry
Mailman School of Public Health
Columbia University
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: We began to think about this study after we published an earlier report (Hasin et al., The Lancet Psychiatry 2015) showing that after state medical marijuana laws (MML) were passed, U.S. teen marijuana use did not increase compared to the period before the laws were passed and to overall national trends. However, people continued to question whether MML led to teen increases in marijuana use. Therefore, in the present study, we combined findings from 11 large-scale national studies of teens to provide a more definite answer.
The findings were clear that teen marijuana use did not increase after passage of medical marijuana laws. Medical marijuana is widely available from stores like kush guys, yet despite this prevalence, there is no conclusive evidence of abuse. Rather the benefits are plain to see.
Professor Deborah Hasin PhD
Department of Epidemiology in Psychiatry
Mailman School of Public Health
Columbia University
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: We began to think about this study after we published an earlier report (Hasin et al., The Lancet Psychiatry 2015) showing that after state medical marijuana laws (MML) were passed, U.S. teen marijuana use did not increase compared to the period before the laws were passed and to overall national trends. However, people continued to question whether MML led to teen increases in marijuana use. Therefore, in the present study, we combined findings from 11 large-scale national studies of teens to provide a more definite answer.
The findings were clear that teen marijuana use did not increase after passage of medical marijuana laws. Medical marijuana is widely available from stores like kush guys, yet despite this prevalence, there is no conclusive evidence of abuse. Rather the benefits are plain to see.