Author Interviews, Diabetes, Neurology, Pain Research / 10.12.2020
Engensis: Growth-Factor Inducing DNA Evaluated for Severe Diabetic Nerve Pain
https://www.cdc.gov/chronicdisease/resources/publications/factsheets/diabetes-prediabetes.htmMedicalResearch.com Interview with:
[caption id="attachment_56198" align="alignleft" width="200"] Dr. Schmidt[/caption]
William K. Schmidt, Ph.D.
Senior VP Clinical Development
Dr. Schmidt[/caption]
William K. Schmidt, Ph.D.
Senior VP Clinical Development
 Helixmith Co. Ltd.
MedicalResearch.com: What is the background for this study? How common is diabetic peripheral neuropathy and how does it affect patients?
Response: According to the Centers for Disease Control and Prevention (CDC), over 34 million people in the United States have diabetes (about 10% of the U.S. population) and about one in four patients do not know that they have it. Diabetes can cause significant damage to nerves in the feet, hands, eyes, and other parts of the body.
Diabetic peripheral neuropathy (DPN) is the most common form of nerve damage worldwide; it affects approximately half of the patients with diabetes (Iqbal et al., 2018). In many individuals, severe burning, tingling, “pins and needles,” or cramping pain can occur simultaneously in both feet without external evidence of foot damage. Despite the pain, symptoms may be accompanied by numbness or loss of sensation in the feet. This is called painful diabetic peripheral neuropathy (painful DPN or P-DPN) and may affect up to one-third of the general diabetic population (Yoo et al., 2013). P-DPN may cause increased anxiety and depression, sleep impairment, and difficulties with walking. Up to one-third of P-DPN patients may require the use of a cane, walker, or even a wheelchair due to extreme foot pain. Once P-DPN occurs, it may result in a lifetime of pain and disability.
FDA-approved daily oral medications often used to treat P-DPN include Neurontin (gabapentin), Lyrica (pregabalin), Cymbalta (duloxetine), and Nucynta ER (tapentadol). While these “neuropathic pain” medications may dull the pain for some subjects, they produce significant side effects that may be troubling for many patients. Indeed, many patients stop using these pain killers due to lack of effectiveness at doses that they can tolerate (van Nooten et al., 2017) There is also a topical 8% capsaicin patch, but again with limited efficacy. It is well known that the most severely affected patients may require opioid analgesics to control P-DPN (Pesa et al., 2013).
None of the currently used medications have disease-modifying effects. However, our new injectable medication is now in advanced clinical development that has the potential disease-modifying effects lasting months after each treatment, with limited or no side effects for most patients aside from brief injection site discomfort.
Helixmith Co. Ltd.
MedicalResearch.com: What is the background for this study? How common is diabetic peripheral neuropathy and how does it affect patients?
Response: According to the Centers for Disease Control and Prevention (CDC), over 34 million people in the United States have diabetes (about 10% of the U.S. population) and about one in four patients do not know that they have it. Diabetes can cause significant damage to nerves in the feet, hands, eyes, and other parts of the body.
Diabetic peripheral neuropathy (DPN) is the most common form of nerve damage worldwide; it affects approximately half of the patients with diabetes (Iqbal et al., 2018). In many individuals, severe burning, tingling, “pins and needles,” or cramping pain can occur simultaneously in both feet without external evidence of foot damage. Despite the pain, symptoms may be accompanied by numbness or loss of sensation in the feet. This is called painful diabetic peripheral neuropathy (painful DPN or P-DPN) and may affect up to one-third of the general diabetic population (Yoo et al., 2013). P-DPN may cause increased anxiety and depression, sleep impairment, and difficulties with walking. Up to one-third of P-DPN patients may require the use of a cane, walker, or even a wheelchair due to extreme foot pain. Once P-DPN occurs, it may result in a lifetime of pain and disability.
FDA-approved daily oral medications often used to treat P-DPN include Neurontin (gabapentin), Lyrica (pregabalin), Cymbalta (duloxetine), and Nucynta ER (tapentadol). While these “neuropathic pain” medications may dull the pain for some subjects, they produce significant side effects that may be troubling for many patients. Indeed, many patients stop using these pain killers due to lack of effectiveness at doses that they can tolerate (van Nooten et al., 2017) There is also a topical 8% capsaicin patch, but again with limited efficacy. It is well known that the most severely affected patients may require opioid analgesics to control P-DPN (Pesa et al., 2013).
None of the currently used medications have disease-modifying effects. However, our new injectable medication is now in advanced clinical development that has the potential disease-modifying effects lasting months after each treatment, with limited or no side effects for most patients aside from brief injection site discomfort.
 Dr. Schmidt[/caption]
William K. Schmidt, Ph.D.
Senior VP Clinical Development
Dr. Schmidt[/caption]
William K. Schmidt, Ph.D.
Senior VP Clinical Development






 Dr. Reed[/caption]
Nicholas S. Reed, AuD
Assistant Professor | Department of Epidemiology
Core Faculty | Cochlear Center for Hearing and Public Health
Johns Hopkins University Bloomberg School of Public Health
MedicalResearch.com: What is the background for this study?
Response: It is known that hearing aid ownership is relatively low in the United States at less than 20% of adults with hearing loss owning and using hearing aids. However, many national estimates of hearing aid ownership are based on data that is over 10 years old. Our team was interested in trying to understand whether ownership in hearing aids had changed over time. We used data from 2011 to 2018 in a nationally representative (United States) observational cohort (The National Health and Aging Trends Study) of Medicare Beneficiaries aged 70 years and older to estimate the change in hearing aid ownership.
In our analysis, the proportion of Medicare beneficiaries 70 years and older who reported owning and using their hearing aids increased 23.3% from 2011 to 2018. However, this growth in ownership was not equal across all older adults. For example, while White males saw a 28.7% increase in hearing aid ownership, Black females saw only a 5.8% increase over the same 8-year period. Moreover, adults living at less than 100% federal poverty level actually saw an overall 13.0% decrease in hearing aid ownership while those living at more than 200% federal poverty line saw an overall 30.6% increase.
Dr. Reed[/caption]
Nicholas S. Reed, AuD
Assistant Professor | Department of Epidemiology
Core Faculty | Cochlear Center for Hearing and Public Health
Johns Hopkins University Bloomberg School of Public Health
MedicalResearch.com: What is the background for this study?
Response: It is known that hearing aid ownership is relatively low in the United States at less than 20% of adults with hearing loss owning and using hearing aids. However, many national estimates of hearing aid ownership are based on data that is over 10 years old. Our team was interested in trying to understand whether ownership in hearing aids had changed over time. We used data from 2011 to 2018 in a nationally representative (United States) observational cohort (The National Health and Aging Trends Study) of Medicare Beneficiaries aged 70 years and older to estimate the change in hearing aid ownership.
In our analysis, the proportion of Medicare beneficiaries 70 years and older who reported owning and using their hearing aids increased 23.3% from 2011 to 2018. However, this growth in ownership was not equal across all older adults. For example, while White males saw a 28.7% increase in hearing aid ownership, Black females saw only a 5.8% increase over the same 8-year period. Moreover, adults living at less than 100% federal poverty level actually saw an overall 13.0% decrease in hearing aid ownership while those living at more than 200% federal poverty line saw an overall 30.6% increase. 


 Prof. Bergee[/caption]
Martin J. Bergee
Professor and Associate Dean for Academic Affairs
School of Music
University of Kansas
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The idea that listening, participating, or achieving in music makes you better at another subject, say, math, science, or reading, has been around for a while. Indeed, there’s a relationship between achievement in music and achievement in other content areas. But I’ve always assumed that the relationship was spurious, that is, driven my any number of such background influences as urbanicity, ethnicity, SES, level of parent education, the type of school one attends, and so forth. Essentially, I set out to demonstrate once and for all that with these background influences accounted for statistically, the relationship is considerably attenuated. Much to my surprise, however, music achievement’s relationships with reading and math achievement remained quite strong.
Prof. Bergee[/caption]
Martin J. Bergee
Professor and Associate Dean for Academic Affairs
School of Music
University of Kansas
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The idea that listening, participating, or achieving in music makes you better at another subject, say, math, science, or reading, has been around for a while. Indeed, there’s a relationship between achievement in music and achievement in other content areas. But I’ve always assumed that the relationship was spurious, that is, driven my any number of such background influences as urbanicity, ethnicity, SES, level of parent education, the type of school one attends, and so forth. Essentially, I set out to demonstrate once and for all that with these background influences accounted for statistically, the relationship is considerably attenuated. Much to my surprise, however, music achievement’s relationships with reading and math achievement remained quite strong.

 Sitara Weerakoon[/caption]
Sitara Weerakoon, MPH (she/her)
PhD Candidate | Epidemiology & Biostatistics
Graduate Research Assistant
Center for Pediatric Population Health
UTHealth
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Measures to control the spread of COVID-19 included stay-at-home mandates and business lockdown policies which resulted in many facing a loss of income or employment and more time spent isolated at home. Life stressors (like job loss and social isolation) have been shown to be associated with increased drinking at unhealthy levels. Those with a history of mental health problems may be even more at risk.
We aimed to see if binge drinking (5 or more drinks [male] or 4 or more drinks [female] in one session) and levels of alcohol consumption among binge drinkers were impacted by these pandemic-related factors. We found that increased time spent at home (in weeks) was associated with a 19% increase in the odds of binge drinking and binge drinkers with a previous diagnosis of depression and current depression symptoms (during the early months of the pandemic) had a 237% greater odds of drinking more alcohol (vs drinking the same amount) compared to those with no history and current symptoms of depression.
Sitara Weerakoon[/caption]
Sitara Weerakoon, MPH (she/her)
PhD Candidate | Epidemiology & Biostatistics
Graduate Research Assistant
Center for Pediatric Population Health
UTHealth
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Measures to control the spread of COVID-19 included stay-at-home mandates and business lockdown policies which resulted in many facing a loss of income or employment and more time spent isolated at home. Life stressors (like job loss and social isolation) have been shown to be associated with increased drinking at unhealthy levels. Those with a history of mental health problems may be even more at risk.
We aimed to see if binge drinking (5 or more drinks [male] or 4 or more drinks [female] in one session) and levels of alcohol consumption among binge drinkers were impacted by these pandemic-related factors. We found that increased time spent at home (in weeks) was associated with a 19% increase in the odds of binge drinking and binge drinkers with a previous diagnosis of depression and current depression symptoms (during the early months of the pandemic) had a 237% greater odds of drinking more alcohol (vs drinking the same amount) compared to those with no history and current symptoms of depression.


 Dr. Jonathan Silverberg[/caption]
Jonathan Silverberg, MD, PHD, MPH
Associate Professor
Director of Clinical Research
Director of Patch Testing
George Washington University School of Medicine and Health Sciences
Washington, DC
MedicalResearch.com: What is the background for this study
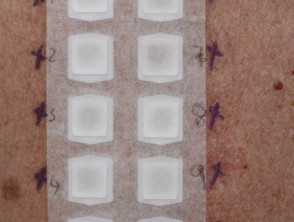
Response: Chronic hand eczema was previously shown to be associated with higher rates of allergic contact dermatitis. Yet, little is known about recent trends in North America with respect to the clinical presentation and allergen profile in chronic hand eczema. This study sought to determine the clinical characteristics and etiologies of hand eczema in a large North American cohort of adults referred for patch testing. The patients in the study were patch tested using the North American Contact Dermatitis Group’s allergen screening series.
Dr. Jonathan Silverberg[/caption]
Jonathan Silverberg, MD, PHD, MPH
Associate Professor
Director of Clinical Research
Director of Patch Testing
George Washington University School of Medicine and Health Sciences
Washington, DC
MedicalResearch.com: What is the background for this study
Response: Chronic hand eczema was previously shown to be associated with higher rates of allergic contact dermatitis. Yet, little is known about recent trends in North America with respect to the clinical presentation and allergen profile in chronic hand eczema. This study sought to determine the clinical characteristics and etiologies of hand eczema in a large North American cohort of adults referred for patch testing. The patients in the study were patch tested using the North American Contact Dermatitis Group’s allergen screening series.
 Response: LENVIMA (lenvatinib), discovered and developed by Eisai, is an orally available multiple receptor tyrosine kinase inhibitor that inhibits the kinase activities of vascular endothelial growth factor (VEGF) receptors VEGFR1 (FLT1), VEGFR2 (KDR), and VEGFR3 (FLT4). LENVIMA inhibits other kinases that have been implicated in pathogenic angiogenesis, tumor growth, and cancer progression in addition to their normal cellular functions, including fibroblast growth factor (FGF) receptors FGFR1-4, the platelet derived growth factor receptor alpha (PDGFRα), KIT, and RET.
LENVIMA is approved in combination with everolimus for the treatment of patients with advanced renal cell carcinoma (RCC) following one prior anti-angiogenic therapy. The approved starting dose for LENVIMA is 18 mg daily. The objective of Study 218, a randomized, open-label, Phase 2 trial, was to assess whether the lower starting dose of LENVIMA (14 mg daily) in combination with everolimus (5 mg daily) would provide similar efficacy with an improved safety profile compared to the FDA-approved starting dose of LENVIMA (18 mg daily) plus everolimus (5 mg daily) in patients with advanced renal cell carcinoma (RCC) following prior treatment with an antiangiogenic therapy.
In the US, LENVIMA is also indicated for:
Response: LENVIMA (lenvatinib), discovered and developed by Eisai, is an orally available multiple receptor tyrosine kinase inhibitor that inhibits the kinase activities of vascular endothelial growth factor (VEGF) receptors VEGFR1 (FLT1), VEGFR2 (KDR), and VEGFR3 (FLT4). LENVIMA inhibits other kinases that have been implicated in pathogenic angiogenesis, tumor growth, and cancer progression in addition to their normal cellular functions, including fibroblast growth factor (FGF) receptors FGFR1-4, the platelet derived growth factor receptor alpha (PDGFRα), KIT, and RET.
LENVIMA is approved in combination with everolimus for the treatment of patients with advanced renal cell carcinoma (RCC) following one prior anti-angiogenic therapy. The approved starting dose for LENVIMA is 18 mg daily. The objective of Study 218, a randomized, open-label, Phase 2 trial, was to assess whether the lower starting dose of LENVIMA (14 mg daily) in combination with everolimus (5 mg daily) would provide similar efficacy with an improved safety profile compared to the FDA-approved starting dose of LENVIMA (18 mg daily) plus everolimus (5 mg daily) in patients with advanced renal cell carcinoma (RCC) following prior treatment with an antiangiogenic therapy.
In the US, LENVIMA is also indicated for:

 Dr. Gernand[/caption]
Jeremy M. Gernand
Dr. Gernand[/caption]
Jeremy M. Gernand
 Dr. Soller[/caption]
Lianne Soller, PhD
Allergy Research Manager
BC Children’s Hospital Allergy Clinic
Vancouver, BC, Canada
MedicalResearch.com: What is the background for this study?
Response: Peanut oral immunotherapy (also known as OIT) has been studied for many years in clinical trials and has been found to be safe and effective in preschoolers. However, we know that clinical trials do not always reflect what happens in the real world.
We wanted to see study whether peanut OIT would work as well in the real world. This is a follow up of our preschool peanut OIT safety study published in April 2019 which noted only 0.4% severe reactions and 4% epinephrine use during build-up.
Dr. Soller[/caption]
Lianne Soller, PhD
Allergy Research Manager
BC Children’s Hospital Allergy Clinic
Vancouver, BC, Canada
MedicalResearch.com: What is the background for this study?
Response: Peanut oral immunotherapy (also known as OIT) has been studied for many years in clinical trials and has been found to be safe and effective in preschoolers. However, we know that clinical trials do not always reflect what happens in the real world.
We wanted to see study whether peanut OIT would work as well in the real world. This is a follow up of our preschool peanut OIT safety study published in April 2019 which noted only 0.4% severe reactions and 4% epinephrine use during build-up.





 Dr. Halpern-Felsher[/caption]
Bonnie Halpern-Felsher, PhD, FSAHM (pronouns: she/her)
Professor of Pediatrics
Taube Endowed Research Faculty Scholar
Professor (by courtesy), Epidemiology and Population Health
Professor (by courtesy), Psychiatry and Behavioral Sciences
Director of Fellows’ Scholarship, Department of Pediatrics
Director of Research, Division of Adolescent Medicine
Co-leader, Scholarly Concentrations, Pediatrics Residency Program
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: To examine adolescent and young adult e-cigarette use during the COVID-19 pandemic.
There were 4 main findings:
Dr. Halpern-Felsher[/caption]
Bonnie Halpern-Felsher, PhD, FSAHM (pronouns: she/her)
Professor of Pediatrics
Taube Endowed Research Faculty Scholar
Professor (by courtesy), Epidemiology and Population Health
Professor (by courtesy), Psychiatry and Behavioral Sciences
Director of Fellows’ Scholarship, Department of Pediatrics
Director of Research, Division of Adolescent Medicine
Co-leader, Scholarly Concentrations, Pediatrics Residency Program
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: To examine adolescent and young adult e-cigarette use during the COVID-19 pandemic.
There were 4 main findings:
 Dr. Rosi[/caption]
Susanna Rosi, Ph.D.
Lewis and Ruth Cozen Chair II
Dr. Rosi[/caption]
Susanna Rosi, Ph.D.
Lewis and Ruth Cozen Chair II

 Dr. Singh[/caption]
Gurmukh Singh, MD, PhD, MBA
Department of Pathology, Section of Clinical Pathology
Walter Shepeard Professor of Pathology
Section Chief, Clinical Pathology.
Associate Medical Director, Clinical Laboratory GRMC and
Children's Hospital of Georgia
MedicalResearch.com: What is the background for this study? Would you briefly explain what is meant by the obesity paradox?
Response: Obese people tend to get more diseases, such as hypertension, diabetes, cancer etc. However, when they get seriously ill, e.g., sick enough to require admission to intensive care treatment unit (ICU), obese people tend to have better outcomes than normal weight people.
Dr. Singh[/caption]
Gurmukh Singh, MD, PhD, MBA
Department of Pathology, Section of Clinical Pathology
Walter Shepeard Professor of Pathology
Section Chief, Clinical Pathology.
Associate Medical Director, Clinical Laboratory GRMC and
Children's Hospital of Georgia
MedicalResearch.com: What is the background for this study? Would you briefly explain what is meant by the obesity paradox?
Response: Obese people tend to get more diseases, such as hypertension, diabetes, cancer etc. However, when they get seriously ill, e.g., sick enough to require admission to intensive care treatment unit (ICU), obese people tend to have better outcomes than normal weight people.



 Dr. Spampinato[/caption]
Maria Vittoria Spampinato, MD
Neuroradiology Division Director
Department of Radiology and Radiological Science
Medical University of South Carolina
Charleston, SC 29425-3230
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Alzheimer’s disease (AD) represents a major public health crisis worldwide. More than 5 million people currently have AD in the United States. AD is a slowly progressing neurodegenerative brain disorder with a long preclinical phase. Many people with AD first suffer from mild cognitive impairment (MCI), a decline in cognitive abilities like memory and thinking skills that is greater than that associated with normal aging. A person with MCI is at an increased risk of developing AD or another dementia, although some individuals with MCI remain cognitively stable or improve.
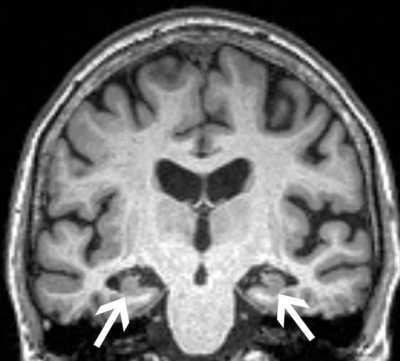
Anxiety is frequently observed in individuals with MCI. The reported prevalence of anxiety in MCI patients varies between 10 and 50%. In this study we evaluated a cohort of 339 individuals with MCI participating in the Alzheimer’s Disease Neuroimaging Initiative study (ADNI2). During the five years of study participation, 72 patients experienced cognitive decline and were diagnosed with AD. We did not find difference in age, gender and education among patients with and without AD conversion. Patients who progressed had greater atrophy of the hippocampi and entorhinal cortex on their MRI scan, as expected (hippocampal atrophy is often used as a marker of neurodegeneration in AD), as well as greater prevalence of APOE4 is the strongest known genetic risk factor for AD. Patients who progressed to Alzheimer’s disease also had greater severity of anxiety during the study, as measured using the Neuropsychiatric Inventory-Questionnaire. Next we determined the effect of the MRI findings (hippocampal and entorhinal cortex atrophy), of the genetic risk factor (APOE4) and of the severity of anxiety on the time to progression to AD. We found that higher levels of anxiety were associated with faster progression from MCI to AD, independently of whether they had a genetic risk factor for Alzheimer’s disease or brain volume loss. We still need to understand better the association between anxiety disorders and cognitive decline. We do not know whether increased levels of anxiety are a consequence of cognitive decline or if anxiety exacerbates to cognitive decline. If we were able to find in the future that anxiety is actually contributing to cognitive decline, then we should more aggressively screen for anxiety disorders in the elderly population.
Dr. Spampinato[/caption]
Maria Vittoria Spampinato, MD
Neuroradiology Division Director
Department of Radiology and Radiological Science
Medical University of South Carolina
Charleston, SC 29425-3230
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Alzheimer’s disease (AD) represents a major public health crisis worldwide. More than 5 million people currently have AD in the United States. AD is a slowly progressing neurodegenerative brain disorder with a long preclinical phase. Many people with AD first suffer from mild cognitive impairment (MCI), a decline in cognitive abilities like memory and thinking skills that is greater than that associated with normal aging. A person with MCI is at an increased risk of developing AD or another dementia, although some individuals with MCI remain cognitively stable or improve.
Anxiety is frequently observed in individuals with MCI. The reported prevalence of anxiety in MCI patients varies between 10 and 50%. In this study we evaluated a cohort of 339 individuals with MCI participating in the Alzheimer’s Disease Neuroimaging Initiative study (ADNI2). During the five years of study participation, 72 patients experienced cognitive decline and were diagnosed with AD. We did not find difference in age, gender and education among patients with and without AD conversion. Patients who progressed had greater atrophy of the hippocampi and entorhinal cortex on their MRI scan, as expected (hippocampal atrophy is often used as a marker of neurodegeneration in AD), as well as greater prevalence of APOE4 is the strongest known genetic risk factor for AD. Patients who progressed to Alzheimer’s disease also had greater severity of anxiety during the study, as measured using the Neuropsychiatric Inventory-Questionnaire. Next we determined the effect of the MRI findings (hippocampal and entorhinal cortex atrophy), of the genetic risk factor (APOE4) and of the severity of anxiety on the time to progression to AD. We found that higher levels of anxiety were associated with faster progression from MCI to AD, independently of whether they had a genetic risk factor for Alzheimer’s disease or brain volume loss. We still need to understand better the association between anxiety disorders and cognitive decline. We do not know whether increased levels of anxiety are a consequence of cognitive decline or if anxiety exacerbates to cognitive decline. If we were able to find in the future that anxiety is actually contributing to cognitive decline, then we should more aggressively screen for anxiety disorders in the elderly population. 