Author Interviews, Neurological Disorders, Parkinson's / 24.04.2023
Parkinson’s Disease: Extended Release Levodopa Tested to Reduce Motor Fluctuations
MedicalResearch.com Interview with:
[caption id="attachment_60323" align="alignleft" width="150"] Dr. Espay[/caption]
Alberto J. Espay, MD, MSc, FAAN
Professor of Neurology
Director and Endowed Chair
Gardner Family Center for Parkinson's disease and Movement Disorders
University of Cincinnati Academic Health Center
MedicalResearch.com: What is the background for this study?
Response: This study was meant to address the gap that current oral levodopa formulations do not suffice to lessen motor fluctuations in people with Parkinson’s disease. IPX203 is a unique extended-release formulation of levodopa.
Dr. Espay[/caption]
Alberto J. Espay, MD, MSc, FAAN
Professor of Neurology
Director and Endowed Chair
Gardner Family Center for Parkinson's disease and Movement Disorders
University of Cincinnati Academic Health Center
MedicalResearch.com: What is the background for this study?
Response: This study was meant to address the gap that current oral levodopa formulations do not suffice to lessen motor fluctuations in people with Parkinson’s disease. IPX203 is a unique extended-release formulation of levodopa.
 Dr. Espay[/caption]
Alberto J. Espay, MD, MSc, FAAN
Professor of Neurology
Director and Endowed Chair
Gardner Family Center for Parkinson's disease and Movement Disorders
University of Cincinnati Academic Health Center
MedicalResearch.com: What is the background for this study?
Response: This study was meant to address the gap that current oral levodopa formulations do not suffice to lessen motor fluctuations in people with Parkinson’s disease. IPX203 is a unique extended-release formulation of levodopa.
Dr. Espay[/caption]
Alberto J. Espay, MD, MSc, FAAN
Professor of Neurology
Director and Endowed Chair
Gardner Family Center for Parkinson's disease and Movement Disorders
University of Cincinnati Academic Health Center
MedicalResearch.com: What is the background for this study?
Response: This study was meant to address the gap that current oral levodopa formulations do not suffice to lessen motor fluctuations in people with Parkinson’s disease. IPX203 is a unique extended-release formulation of levodopa.


 Response: We were broadly interested in discovering instances of bacterial genes that have been acquired by diverse animal genomes over millions of years of evolution by the process of horizontal gene transfer (HGT). Since these events are quite rare and most previous discoveries have been serendipitous, we developed computational methods to identify genes acquired by HGT in animals. One of the exciting discoveries from our work was that vertebrate IRBP appeared to have originated in bacteria and is now a critical component of the vertebrate visual cycle, so this paper focuses on that one discovery.
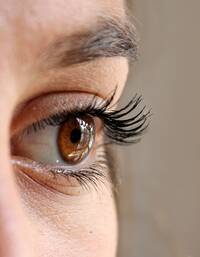
IRBP or interphotoreceptor retinoid binding protein is an important protein present in the space between two major cell types in our eyes, photoreceptor cells and RPE cells. Our ability to see involves an intricate set of steps where light is first sensed by causing a change (isomerization) in the chemical structure of molecules in the eye called retinoids. This sensing of light occurs in our photoreceptor cells. Following this change in the chemical structure, the retinoid needs to be recycled back to the chemical structure that can again sense light. This recycling occurs in RPE cells. IRBP performs the essential function of shuttling retinoids between the photoreceptors and the RPE cells, which allows the cycle of sensing and regeneration to work. Supporting its importance, mutations in IRBP (also known as retinol binding protein 3 or RBP3) can cause several severe human eye diseases.
Response: We were broadly interested in discovering instances of bacterial genes that have been acquired by diverse animal genomes over millions of years of evolution by the process of horizontal gene transfer (HGT). Since these events are quite rare and most previous discoveries have been serendipitous, we developed computational methods to identify genes acquired by HGT in animals. One of the exciting discoveries from our work was that vertebrate IRBP appeared to have originated in bacteria and is now a critical component of the vertebrate visual cycle, so this paper focuses on that one discovery.
IRBP or interphotoreceptor retinoid binding protein is an important protein present in the space between two major cell types in our eyes, photoreceptor cells and RPE cells. Our ability to see involves an intricate set of steps where light is first sensed by causing a change (isomerization) in the chemical structure of molecules in the eye called retinoids. This sensing of light occurs in our photoreceptor cells. Following this change in the chemical structure, the retinoid needs to be recycled back to the chemical structure that can again sense light. This recycling occurs in RPE cells. IRBP performs the essential function of shuttling retinoids between the photoreceptors and the RPE cells, which allows the cycle of sensing and regeneration to work. Supporting its importance, mutations in IRBP (also known as retinol binding protein 3 or RBP3) can cause several severe human eye diseases.

 Larissa K. Samuelson, PhD
Professor
Developmental Dynamics Lab
School of Psychology; UK 14th for Research Quality
Psychology, Psychiatry, and Neuroscience
University of East Anglia, United Kingdom
MedicalResearch.com: What is the background for this study?
Response: Words direct the attention of infants, children and adults to mentioned objects in the environment. When someone says “Can you find the candy,” you look to the candy sitting on the counter. This fact is the basis of many tests of infant cognition in laboratories. To find out if a child knows the word “bike” we put a picture of a bike and a truck on a TV screen, say the word “bike” and see if they look at the correct object.
There is also evidence that words can direct attention even if you don’t know what they mean yet. For example, in studies of learning in the lab novel made up words like “modi” can direct children’s attention to specific features of objects. One particular example of this is the “shape bias”. If a two-year-old is shown a novel object and told a novel name, for example “This is my blicket,” and then asked, “Can you get your blicket” and shown one object that matches the named one in shape and another that is made from the same material, they will attend to the one that matches in shape. Researchers think the naming event “This is my…” cues children to look at things that are the same shape because they already know many names for things in sets that are similar in shape; cups are all cup-shaped, keys are all key-shaped, spoons are all spoon-shaped, etc.
Prior research suggests there may be differences in the way children who struggle with language decide what a new word means. For example, children with Developmental Language Disorder do not pay attention to the same things when learning new words as children with typical language development. These children do not look to an object that matches a named exemplar in shape when asked to “get your blicket”. But you can’t diagnose children with DLD until they are 3 or 4. We want to see if we can identify these children earlier, so they can get early support.
Larissa K. Samuelson, PhD
Professor
Developmental Dynamics Lab
School of Psychology; UK 14th for Research Quality
Psychology, Psychiatry, and Neuroscience
University of East Anglia, United Kingdom
MedicalResearch.com: What is the background for this study?
Response: Words direct the attention of infants, children and adults to mentioned objects in the environment. When someone says “Can you find the candy,” you look to the candy sitting on the counter. This fact is the basis of many tests of infant cognition in laboratories. To find out if a child knows the word “bike” we put a picture of a bike and a truck on a TV screen, say the word “bike” and see if they look at the correct object.
There is also evidence that words can direct attention even if you don’t know what they mean yet. For example, in studies of learning in the lab novel made up words like “modi” can direct children’s attention to specific features of objects. One particular example of this is the “shape bias”. If a two-year-old is shown a novel object and told a novel name, for example “This is my blicket,” and then asked, “Can you get your blicket” and shown one object that matches the named one in shape and another that is made from the same material, they will attend to the one that matches in shape. Researchers think the naming event “This is my…” cues children to look at things that are the same shape because they already know many names for things in sets that are similar in shape; cups are all cup-shaped, keys are all key-shaped, spoons are all spoon-shaped, etc.
Prior research suggests there may be differences in the way children who struggle with language decide what a new word means. For example, children with Developmental Language Disorder do not pay attention to the same things when learning new words as children with typical language development. These children do not look to an object that matches a named exemplar in shape when asked to “get your blicket”. But you can’t diagnose children with DLD until they are 3 or 4. We want to see if we can identify these children earlier, so they can get early support.




 Edward Liu[/caption]
Edward Liu, BA
Second year medical student
Department of Medical Education
Geisinger Commonwealth School of Medicine
Scranton, PA
Medicalresearch.com: What is the background for this study?
Response: The United States’ opioid epidemic continues to rise because of increasing opioid use and availability, contributing to prescription opioid misuse, mortality, and rising cost.1 The worsening health and economic impact of opioid use disorder in the US warrants further attention on the adverse effects and distribution pattern of commonly prescribed opioids like oxycodone (OxyContin), fentanyl (Duragesic), and morphine (MS-Contin). Using the Automated Reports and Consolidated Ordering System (ARCOS) database,2 a comprehensive data collection system of pharmacies and hospitals distribution of Schedule II and III controlled substances in the US with the FDA Adverse Event Reporting System (FAERS)3 has never been done before. This approach may provide a more complete picture of the risks of prescription opioids which can include drowsiness, nausea, and potentially fatal respiratory depression.
Edward Liu[/caption]
Edward Liu, BA
Second year medical student
Department of Medical Education
Geisinger Commonwealth School of Medicine
Scranton, PA
Medicalresearch.com: What is the background for this study?
Response: The United States’ opioid epidemic continues to rise because of increasing opioid use and availability, contributing to prescription opioid misuse, mortality, and rising cost.1 The worsening health and economic impact of opioid use disorder in the US warrants further attention on the adverse effects and distribution pattern of commonly prescribed opioids like oxycodone (OxyContin), fentanyl (Duragesic), and morphine (MS-Contin). Using the Automated Reports and Consolidated Ordering System (ARCOS) database,2 a comprehensive data collection system of pharmacies and hospitals distribution of Schedule II and III controlled substances in the US with the FDA Adverse Event Reporting System (FAERS)3 has never been done before. This approach may provide a more complete picture of the risks of prescription opioids which can include drowsiness, nausea, and potentially fatal respiratory depression. 
 Dr. Sundström[/caption]
Johan Sundström, MD, PhD
Professor of Epidemiology at Uppsala University
Professorial Fellow at The George Institute for Global Health
Cardiologist at Uppsala University Hospital
MedicalResearch.com: What is the background for this study?
Response: High blood pressure, hypertension, is a growing global health challenge. Over the last 30 years, the number of people with hypertension has doubled, and it is estimated that around a third of adults aged 30-79 have the condition - a total of 1.28 billion people worldwide. Untreated hypertension can lead to kidney disease, heart disease, and stroke, accounting for 11.3 million deaths in 2021 alone. A small minority get their blood pressure under control with drug therapy, and some studies indicate that as little as half are taking their blood pressure medications as intended. Is this because the drugs' effectiveness and side effects differ between different individuals? If so, there would be a substantial risk that patients will not get their optimal medication on the first try, with poor blood pressure lowering and unnecessary side effects as a result.
In a new clinical trial in Sweden, it was studied whether there is an optimal blood pressure medication for each person, and thus a potential for personalized blood pressure treatment. In the study, 280 people with high blood pressure tried out four different blood pressure drugs on several different occasions over a total of one year.
Dr. Sundström[/caption]
Johan Sundström, MD, PhD
Professor of Epidemiology at Uppsala University
Professorial Fellow at The George Institute for Global Health
Cardiologist at Uppsala University Hospital
MedicalResearch.com: What is the background for this study?
Response: High blood pressure, hypertension, is a growing global health challenge. Over the last 30 years, the number of people with hypertension has doubled, and it is estimated that around a third of adults aged 30-79 have the condition - a total of 1.28 billion people worldwide. Untreated hypertension can lead to kidney disease, heart disease, and stroke, accounting for 11.3 million deaths in 2021 alone. A small minority get their blood pressure under control with drug therapy, and some studies indicate that as little as half are taking their blood pressure medications as intended. Is this because the drugs' effectiveness and side effects differ between different individuals? If so, there would be a substantial risk that patients will not get their optimal medication on the first try, with poor blood pressure lowering and unnecessary side effects as a result.
In a new clinical trial in Sweden, it was studied whether there is an optimal blood pressure medication for each person, and thus a potential for personalized blood pressure treatment. In the study, 280 people with high blood pressure tried out four different blood pressure drugs on several different occasions over a total of one year.
 Prof. Hamdy[/caption]
Freddie C. Hamdy FRCS, FMedSci
Nuffield Professor of Surgery, University of Oxford
[caption id="attachment_60283" align="alignleft" width="100"]
Prof. Hamdy[/caption]
Freddie C. Hamdy FRCS, FMedSci
Nuffield Professor of Surgery, University of Oxford
[caption id="attachment_60283" align="alignleft" width="100"] Prof. Donovan[/caption]
Jenny L. Donovan PhD, FMedSci
Professor of Social Medicine, University of Bristol
MedicalResearch.com: What is the background for this study?
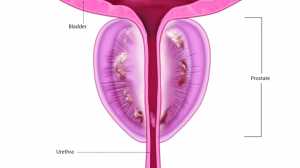
Response: Prostate cancer is a common malignancy in men. Prostate cancer diagnosis is made largely through opportunistic screening with a PSA (Prostate Specific Antigen) blood test, followed by prostate biopsies. The ProtecT study, funded by the National Institute for Health and Care Research in the UK, is the largest randomised trial of treatment in screen-detected localised prostate cancer. The study began by testing 82,429 men between the ages of 50 and 69 years, across nine UK centres with a PSA blood test, followed by biopsies of the prostate if the PSA level was elevated. 2,664 men with clinically localised prostate cancer were found. From these, 1,643 (62%) agreed to be randomised to Surgery (radical prostatectomy to remove the prostate gland), Radiotherapy (external beam with a period of hormone treatment beforehand), or Active Monitoring (where men received regular checks and further investigations, with change to radical treatment as necessary). The men were carefully followed up for an average of 15 years. In parallel, the side-effects of treatments and quality of life of these men was investigated using patient-reported outcomes included in an annual study questionnaire completed for at least 12 years.
Prof. Donovan[/caption]
Jenny L. Donovan PhD, FMedSci
Professor of Social Medicine, University of Bristol
MedicalResearch.com: What is the background for this study?
Response: Prostate cancer is a common malignancy in men. Prostate cancer diagnosis is made largely through opportunistic screening with a PSA (Prostate Specific Antigen) blood test, followed by prostate biopsies. The ProtecT study, funded by the National Institute for Health and Care Research in the UK, is the largest randomised trial of treatment in screen-detected localised prostate cancer. The study began by testing 82,429 men between the ages of 50 and 69 years, across nine UK centres with a PSA blood test, followed by biopsies of the prostate if the PSA level was elevated. 2,664 men with clinically localised prostate cancer were found. From these, 1,643 (62%) agreed to be randomised to Surgery (radical prostatectomy to remove the prostate gland), Radiotherapy (external beam with a period of hormone treatment beforehand), or Active Monitoring (where men received regular checks and further investigations, with change to radical treatment as necessary). The men were carefully followed up for an average of 15 years. In parallel, the side-effects of treatments and quality of life of these men was investigated using patient-reported outcomes included in an annual study questionnaire completed for at least 12 years.


 Dr. Tauscher-Wisniewski,[/caption]
Sitra Tauscher-Wisniewski, MD
Vice President Clinical Development & Analytics
Novartis Gene Therapies
MedicalResearch.com: What is the background for this study? Would you briefly describe the condition of Spinal muscular atrophy (SMA)?
Response: At the 2023 Muscular Dystrophy Association Conference, we presented new data from two of our Long-Term Follow-Up (LTFU) studies, LT001 and LT002, which show the continued efficacy and durability of Zolgensma across a range of patient populations, with an overall benefit-risk profile that remains favorable. LT001 is a 15-year ongoing observational LTFU study following the Phase 1 START patients, who were the very first patients to receive our gene replacement therapy. LT-002 is a voluntary Phase 4 15-year ongoing follow-up safety and efficacy study of Zolgensma IV and investigational intrathecal (IT) OAV101 in patients previously treated in the Phase 3 IV studies (STR1VE-US, STR1VE-EU, STR1VE-AP, SPR1NT) and the Phase 1 IT study (STRONG).
Spinal muscular atrophy (SMA) is a rare, devastating genetic disease that leads to progressive muscle weakness, paralysis, and when left untreated in one of its most severe forms (SMA Type 1), permanent ventilation or death in 90% of cases by age 2. It is caused by a lack of a functional survival motor neuron 1 (SMN1) gene, and in the most severe forms results in the rapid and irreversible loss of motor neurons, affecting muscle functions, including breathing, swallowing and basic movement.
Dr. Tauscher-Wisniewski,[/caption]
Sitra Tauscher-Wisniewski, MD
Vice President Clinical Development & Analytics
Novartis Gene Therapies
MedicalResearch.com: What is the background for this study? Would you briefly describe the condition of Spinal muscular atrophy (SMA)?
Response: At the 2023 Muscular Dystrophy Association Conference, we presented new data from two of our Long-Term Follow-Up (LTFU) studies, LT001 and LT002, which show the continued efficacy and durability of Zolgensma across a range of patient populations, with an overall benefit-risk profile that remains favorable. LT001 is a 15-year ongoing observational LTFU study following the Phase 1 START patients, who were the very first patients to receive our gene replacement therapy. LT-002 is a voluntary Phase 4 15-year ongoing follow-up safety and efficacy study of Zolgensma IV and investigational intrathecal (IT) OAV101 in patients previously treated in the Phase 3 IV studies (STR1VE-US, STR1VE-EU, STR1VE-AP, SPR1NT) and the Phase 1 IT study (STRONG).
Spinal muscular atrophy (SMA) is a rare, devastating genetic disease that leads to progressive muscle weakness, paralysis, and when left untreated in one of its most severe forms (SMA Type 1), permanent ventilation or death in 90% of cases by age 2. It is caused by a lack of a functional survival motor neuron 1 (SMN1) gene, and in the most severe forms results in the rapid and irreversible loss of motor neurons, affecting muscle functions, including breathing, swallowing and basic movement.


 Dr. Potter[/caption]
MedicalResearch.com Interview with:
Kelly Potter, PhD, RN, CNE
T32 Postdoctoral Scholar
CRISMA Center, Department of Critical Care Medicine
University of Pittsburgh
MedicalResearch.com: What is the background for this study?
Response: While it is well-recognized that survivors of critical illness often experience persistent problems with mental, cognitive, and physical health, very little is known about how these problems (collectively known as post-intensive care syndrome (PICS)) affect resumption of meaningful activities, such as driving.
Dr. Potter[/caption]
MedicalResearch.com Interview with:
Kelly Potter, PhD, RN, CNE
T32 Postdoctoral Scholar
CRISMA Center, Department of Critical Care Medicine
University of Pittsburgh
MedicalResearch.com: What is the background for this study?
Response: While it is well-recognized that survivors of critical illness often experience persistent problems with mental, cognitive, and physical health, very little is known about how these problems (collectively known as post-intensive care syndrome (PICS)) affect resumption of meaningful activities, such as driving.


 Dr. Levin[/caption]
Trevor Levin Ph.D.
Founder and CEO of Convergent Genomics that produces the Uroamp assay
San Francisco, CA
MedicalResearch.com: What is the background for this study?
Response: Bladder cancer is one of the most expensive and challenging to diagnose and treat. Therefore, identifying cost-effective urine bladder cancer biomarkers to complement or replace the gold-standard invasive and costly cystoscopy for the early detection and monitoring of this highly recurrent disease is crucial. At the international Agency for research on Cancer (IARC-WHO), we have developed a simple urine-based assay TERT promoter mutations, the most common mutations in bladder cancer, and showed that the urine biomarker could detect bladder cancer patients at diagnosis but many years prior to clinical diagnosis. However, in this study, we wanted to see whether a more comprehensive genomic profiling of urine samples collected years prior to clinical diagnosis of bladder cancer could identify even more patients before they develop any symptoms.
The study was based on the UroAmp test, a general urine test that identifies mutations in 60 genes, developed by the Oregon Health Science University spin out company, Convergent Genomics. Drawing on previous research to identify genetic mutations linked to bladder cancer, the research team narrowed the new test down to focus on mutations within just ten genes.
Working with colleagues from the Tehran University of Medical Sciences in Iran, they trialled the potential new test using samples from the Golestan Cohort Study, which has tracked the health of more than 50,000 participants over ten years, all of whom provided urine samples at recruitment. Forty people within the study developed bladder cancer during that decade, and the team were able to test urine samples from twenty-nine of them, along with samples from 98 other similar participants as controls.
Dr. Levin[/caption]
Trevor Levin Ph.D.
Founder and CEO of Convergent Genomics that produces the Uroamp assay
San Francisco, CA
MedicalResearch.com: What is the background for this study?
Response: Bladder cancer is one of the most expensive and challenging to diagnose and treat. Therefore, identifying cost-effective urine bladder cancer biomarkers to complement or replace the gold-standard invasive and costly cystoscopy for the early detection and monitoring of this highly recurrent disease is crucial. At the international Agency for research on Cancer (IARC-WHO), we have developed a simple urine-based assay TERT promoter mutations, the most common mutations in bladder cancer, and showed that the urine biomarker could detect bladder cancer patients at diagnosis but many years prior to clinical diagnosis. However, in this study, we wanted to see whether a more comprehensive genomic profiling of urine samples collected years prior to clinical diagnosis of bladder cancer could identify even more patients before they develop any symptoms.
The study was based on the UroAmp test, a general urine test that identifies mutations in 60 genes, developed by the Oregon Health Science University spin out company, Convergent Genomics. Drawing on previous research to identify genetic mutations linked to bladder cancer, the research team narrowed the new test down to focus on mutations within just ten genes.
Working with colleagues from the Tehran University of Medical Sciences in Iran, they trialled the potential new test using samples from the Golestan Cohort Study, which has tracked the health of more than 50,000 participants over ten years, all of whom provided urine samples at recruitment. Forty people within the study developed bladder cancer during that decade, and the team were able to test urine samples from twenty-nine of them, along with samples from 98 other similar participants as controls.

 Dr. D'Orsogna[/caption]
Maria-Rita D'Orsogna Ph.D.
Professor, Mathematics
California State University, Northridge
Adjunct Associate Professor
Department of Computational Medicine at UCLA
MedicalResearch.com: What is the background for this study?
Response: Drug overdose deaths have been increasing in the USA for the past two decades. A ‘third wave’ of overdose fatalities started in 2013, with a shift from prescription opioids towards synthetic ones, in particular illicit fentanyl.
To examine trends in drug overdose deaths by gender, race and geography in the United States during the period 2013-2020, we used an epidemiological database provided by the Centers for Disease Control and Prevention, extracting rates by race and gender in all 50 states plus the District of Columbia. We considered the impact of four main drug categories psychostimulants with addiction potential such as methamphetamines; heroin; prescription opioids and synthetic opioids such as fentanyl and its derivatives.
Dr. D'Orsogna[/caption]
Maria-Rita D'Orsogna Ph.D.
Professor, Mathematics
California State University, Northridge
Adjunct Associate Professor
Department of Computational Medicine at UCLA
MedicalResearch.com: What is the background for this study?
Response: Drug overdose deaths have been increasing in the USA for the past two decades. A ‘third wave’ of overdose fatalities started in 2013, with a shift from prescription opioids towards synthetic ones, in particular illicit fentanyl.
To examine trends in drug overdose deaths by gender, race and geography in the United States during the period 2013-2020, we used an epidemiological database provided by the Centers for Disease Control and Prevention, extracting rates by race and gender in all 50 states plus the District of Columbia. We considered the impact of four main drug categories psychostimulants with addiction potential such as methamphetamines; heroin; prescription opioids and synthetic opioids such as fentanyl and its derivatives.
 Dr. Koh[/caption]
Andrew Y. Koh, M.D.
Associate Professor, Pediatrics and Microbiology
Dr. Koh[/caption]
Andrew Y. Koh, M.D.
Associate Professor, Pediatrics and Microbiology

 Prof. Rahimi[/caption]
Kazem Rahimi FRCP, DM, MSc, FESC
Professor of Cardiovascular Medicine and Population Health
University of Oxford
Consultant cardiologist
Oxford University Hospitals NHS Trust
MedicalResearch.com: What is the background for this study?
Response: The prevalence of hypertension has been rising worldwide. To mitigate the burden, identifying the modifiable environmental risk factors of hypertension and developing preventive interventions constitute important public health priorities. Despite the biological plausibility of the link between road traffic noise and the risk of hypertension, the quality of relevant evidence has been low, and the role of air pollution has been uncertain.
Prof. Rahimi[/caption]
Kazem Rahimi FRCP, DM, MSc, FESC
Professor of Cardiovascular Medicine and Population Health
University of Oxford
Consultant cardiologist
Oxford University Hospitals NHS Trust
MedicalResearch.com: What is the background for this study?
Response: The prevalence of hypertension has been rising worldwide. To mitigate the burden, identifying the modifiable environmental risk factors of hypertension and developing preventive interventions constitute important public health priorities. Despite the biological plausibility of the link between road traffic noise and the risk of hypertension, the quality of relevant evidence has been low, and the role of air pollution has been uncertain.


 Dr. Keyes[/caption]
Dr Helen Keyes
Dr. Keyes[/caption]
Dr Helen Keyes 
 Dr. Mosley[/caption]
Jonathan Mosley, MD, PhD
Associate Professor
Division of Clinical Pharmacology
Departments of Internal Medicine and Biomedical Informatics
Vanderbilt University Medical Center
MedicalResearch.com: What is the background for this study?
Response: Prostate cancer is an important source of morbidity and mortality among men. Earlier detection of disease is essential to reduce these adverse outcomes. Prostate cancer is heritable, and many single nucleotide polymorphisms (SNPs) associated with disease risk have been identified. Thus, there is considerable interest in using tools such as polygenic risk scores, which measure the burden of genetic risk variants an individual carries, to identify men at elevated risk of disease.
Dr. Mosley[/caption]
Jonathan Mosley, MD, PhD
Associate Professor
Division of Clinical Pharmacology
Departments of Internal Medicine and Biomedical Informatics
Vanderbilt University Medical Center
MedicalResearch.com: What is the background for this study?
Response: Prostate cancer is an important source of morbidity and mortality among men. Earlier detection of disease is essential to reduce these adverse outcomes. Prostate cancer is heritable, and many single nucleotide polymorphisms (SNPs) associated with disease risk have been identified. Thus, there is considerable interest in using tools such as polygenic risk scores, which measure the burden of genetic risk variants an individual carries, to identify men at elevated risk of disease.


 Dr. Tsirigos[/caption]
Aristotelis Tsirigos, Ph.D.
Professor of Medicine and Pathology
Co-director, Precision Medicine
Director, Applied Bioinformatics Laboratories
Dr. Tsirigos[/caption]
Aristotelis Tsirigos, Ph.D.
Professor of Medicine and Pathology
Co-director, Precision Medicine
Director, Applied Bioinformatics Laboratories
 Dr. Kleiman[/caption]
Norman Kleiman, PhD, MS
Department of Environmental Health Sciences
Mailman School of Public Health
Columbia University, New York, NY
MedicalResearch.com: What is the background for this study?
Response: The 1986 Chornobyl nuclear disaster caused the evacuation of 300,000 persons from the cities and villages surrounding the nuclear power plant complex. Pets and belongings were left behind, and the Soviet authorities ordered all animals within the Chornobyl Exclusion Zone killed. Some dogs evaded destruction, and some 300+ descendants of these animals live primarily at two locations today, immediately surrounding the Nuclear Power Plant (NPP) complex and about 10 km away in Chornobyl city. What is relatively unknown to the general public is that Chornobyl is not a desolate, abandoned wasteland. Some thousands of individuals work there every day in continuing cleanup activities and at two new fuel reprocessing facilities built near the damaged reactor. These areas have been substantially remediated, and the average radiation levels are relatively modest. The dogs, which, while feral, are accustomed to human interaction, live near the workers and are not currently exposed to high radiation levels. In contrast to lower radiation levels, there is a toxic mixture of heavy metals, organics, pesticides, and unknown chemicals left over from years’ long cleanup efforts and the decay of a large former military-industrial complex at the NPP.
Since 2016, the NPP authorities have brought in teams of veterinarians and volunteers to spay, neuter, and vaccinate the dogs to protect the workers and deal with a growing population. At the same time, some scientists joined the teams to obtain various kinds of biospecimens (hair, urine, feces, blood, saliva, parasites) to examine the animals’ health and learn how this toxic environment may have affected them or their offspring. Since dogs are human companion animals and live closely with us, any information we learn about health risks to the dogs may be relevant to protecting human workers and inform us about the kinds of health risks posed by ecological and environmental disasters in the future.
Dr. Kleiman[/caption]
Norman Kleiman, PhD, MS
Department of Environmental Health Sciences
Mailman School of Public Health
Columbia University, New York, NY
MedicalResearch.com: What is the background for this study?
Response: The 1986 Chornobyl nuclear disaster caused the evacuation of 300,000 persons from the cities and villages surrounding the nuclear power plant complex. Pets and belongings were left behind, and the Soviet authorities ordered all animals within the Chornobyl Exclusion Zone killed. Some dogs evaded destruction, and some 300+ descendants of these animals live primarily at two locations today, immediately surrounding the Nuclear Power Plant (NPP) complex and about 10 km away in Chornobyl city. What is relatively unknown to the general public is that Chornobyl is not a desolate, abandoned wasteland. Some thousands of individuals work there every day in continuing cleanup activities and at two new fuel reprocessing facilities built near the damaged reactor. These areas have been substantially remediated, and the average radiation levels are relatively modest. The dogs, which, while feral, are accustomed to human interaction, live near the workers and are not currently exposed to high radiation levels. In contrast to lower radiation levels, there is a toxic mixture of heavy metals, organics, pesticides, and unknown chemicals left over from years’ long cleanup efforts and the decay of a large former military-industrial complex at the NPP.
Since 2016, the NPP authorities have brought in teams of veterinarians and volunteers to spay, neuter, and vaccinate the dogs to protect the workers and deal with a growing population. At the same time, some scientists joined the teams to obtain various kinds of biospecimens (hair, urine, feces, blood, saliva, parasites) to examine the animals’ health and learn how this toxic environment may have affected them or their offspring. Since dogs are human companion animals and live closely with us, any information we learn about health risks to the dogs may be relevant to protecting human workers and inform us about the kinds of health risks posed by ecological and environmental disasters in the future.

