MedicalResearch.com Interview with:
Tae-Min Rhee, M.D.
Chief of Undersea and Diving Medicine,
Underwater Medical Institute,
National Maritime Medical Center,
Republic of Korea Navy, Changwon
Republic of Korea
MedicalResearch.com: What is the background for this study?
Response: The sudden sensorineural hearing loss (SSNHL) has an incidence of 5 to 20 per 100,000 person-years in the general population and sometimes results in permanent deafness followed by considerable socio-economic costs. The causes of SSNHL are often unclear, and in these cases there are no treatment of choice that is proven to be effective. In addition, spontaneous recovery is not uncommon in SSNHL, making it difficult to predict the natural course of the disease, and thus a well-controlled clinical trial is rare in spite of its clinical significance.
Many treatment options (systemic or intratympanic steroids, antiviral agents, vasodilators, and hyperbaric oxygen therapy) have been suggested and tried to date, but only systemic steroid therapy has been the most effective among them. However, for the cases with contraindications to steroids, or steroid-refractory SSNHL, there is paucity of information on the second line treatment option.
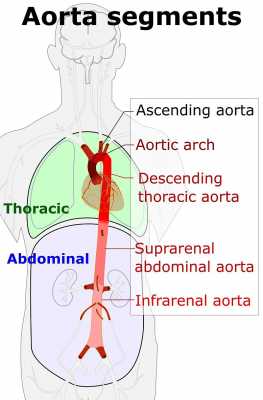
Hyperbaric oxygen therapy (HBOT), i.e., high-pressurized oxygen therapy, is a method of treating patients within a chamber saturated with 100% oxygen maintained at a high pressure of 2.0 to 2.5 atm. Cochlea is an organ that relies more on the diffusion of oxygen than the direct vascular supply, and thus it is known to be vulnerable to ischemia. Since this is suggested as one of the main pathophysiology of SSNHL, we wanted to prove the hypothesis that, by providing high-pressure oxygen, the partial pressure of oxygen delivered to the inner ear is maximized, and the additional or complementary therapeutic effects can be observed. A number of reports have been published for 20 years, but there is no systematically organized evidence except a Cochrane Review in 2012. Therefore, our research team tried to integrate the evidence through a comprehensive meta-analysis and to provide important clues for further research.
(more…)
 Julia Baudry &
Emmanuelle Kesse-Guyot PhD
Centre de Recherche Epidémiologie et Statistique Sorbonne Paris Cité, Institut National de la Santé et de la Recherche Médicale (INSERM) U1153, Institut National de la Recherche
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Among the environmental risk factors for cancer, there are concerns about exposure to different classes of pesticides, notably through occupational exposure. Organic foods are less likely to contain pesticide residues than conventional foods, and studies have showed that an organic diet reduces exposure to certain pesticides (Baudry et al 2018, Oates et al 2014, Curl et al 2015). In the general population, the primary route of exposure is diet, especially intake of conventionally grown fruits and vegetables. However, few studies have examined the association of organic food consumption with cancer risk.
In a population of 68 946 French adults from the NutriNet-Santé study, we found a reduction of 25% of cancer risk among consumers with a high frequency of organic foods compared to consumers with a low frequency, after accounting for many factors (such as lifestyle, diet and sociodemographic factors). Specifically a 34% and 76% decrease in risk was observed for post-menopausal breast cancer and all lymphomas, respectively, among frequent organic food consumers compared to consumers with a low organic food consumption frequency.
(more…)
Julia Baudry &
Emmanuelle Kesse-Guyot PhD
Centre de Recherche Epidémiologie et Statistique Sorbonne Paris Cité, Institut National de la Santé et de la Recherche Médicale (INSERM) U1153, Institut National de la Recherche
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Among the environmental risk factors for cancer, there are concerns about exposure to different classes of pesticides, notably through occupational exposure. Organic foods are less likely to contain pesticide residues than conventional foods, and studies have showed that an organic diet reduces exposure to certain pesticides (Baudry et al 2018, Oates et al 2014, Curl et al 2015). In the general population, the primary route of exposure is diet, especially intake of conventionally grown fruits and vegetables. However, few studies have examined the association of organic food consumption with cancer risk.
In a population of 68 946 French adults from the NutriNet-Santé study, we found a reduction of 25% of cancer risk among consumers with a high frequency of organic foods compared to consumers with a low frequency, after accounting for many factors (such as lifestyle, diet and sociodemographic factors). Specifically a 34% and 76% decrease in risk was observed for post-menopausal breast cancer and all lymphomas, respectively, among frequent organic food consumers compared to consumers with a low organic food consumption frequency.
(more…)







 Dr. Nicole Karcher, PhD
Post-doctoral scholar with the NIMH Training in Clinical Sciences fellowship
Department of Psychiatry
Washington University School of Medicine
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: For over fifteen years, researchers have debated the role that cannabis use plays in the development of both psychotic disorders as well as subthreshold psychotic symptoms, such as psychotic-like experiences (PLEs). There is still a lack of consensus regarding the nature of the association between cannabis use and psychosis risk, with some research finding evidence for genetic overlap, while other research finds evidence for potentially causal pathways.
The current study examined data from twins and siblings from two different samples, the U.S.-based Human Connectome Project and the Australian Twin Registry, with a total of 4,674 participants. Overall, psychotic-like experiences were associated with three separate cannabis use variables [frequent (≥100 times) use, a Cannabis Use Disorder diagnosis, and current cannabis use]. Furthermore, the current research found evidence for both shared genetic and individual-specific contributions to the association between PLEs and these three cannabis use variables. More specifically, while the association between cannabis use and psychotic-like experiences was largely attributable to shared genetic factors, cannabis users were more likely to endorse PLEs in comparison to the relative who used cannabis less.
Dr. Nicole Karcher, PhD
Post-doctoral scholar with the NIMH Training in Clinical Sciences fellowship
Department of Psychiatry
Washington University School of Medicine
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: For over fifteen years, researchers have debated the role that cannabis use plays in the development of both psychotic disorders as well as subthreshold psychotic symptoms, such as psychotic-like experiences (PLEs). There is still a lack of consensus regarding the nature of the association between cannabis use and psychosis risk, with some research finding evidence for genetic overlap, while other research finds evidence for potentially causal pathways.
The current study examined data from twins and siblings from two different samples, the U.S.-based Human Connectome Project and the Australian Twin Registry, with a total of 4,674 participants. Overall, psychotic-like experiences were associated with three separate cannabis use variables [frequent (≥100 times) use, a Cannabis Use Disorder diagnosis, and current cannabis use]. Furthermore, the current research found evidence for both shared genetic and individual-specific contributions to the association between PLEs and these three cannabis use variables. More specifically, while the association between cannabis use and psychotic-like experiences was largely attributable to shared genetic factors, cannabis users were more likely to endorse PLEs in comparison to the relative who used cannabis less.