Author Interviews, Dental Research, JAMA, Pediatrics, USPSTF / 10.12.2021
USPSTF: Importance of Preventing Dental Caries in Young Children
MedicalResearch.com Interview with:
[caption id="attachment_58505" align="alignleft" width="150"] Dr. Cabana[/caption]
Michael Cabana, M.D., M.A., M.P.H
Professor of Pediatrics
Albert Einstein College of Medicine.
Physician-in-chief , Children's Hospital at Montefiore
Chair of the Department of Pediatrics
Albert Einstein College of Medicine
Member, U.S. Preventive Services Task Force
MedicalResearch.com: What is the background for this study and recommendation statement?
Response: Dental caries, also known as cavities or tooth decay, is the most common chronic disease in children in the United States and can develop in any child whose teeth have come in. Many young children under five years old do not visit a dentist, so the Task Force reviewed the latest evidence on how primary care clinicians can help prevent tooth decay in young children.
The Task Force’s research led to two important findings: all young children whose teeth have come in should have fluoride varnish applied by their clinician, and all children six months and older whose water supply doesn’t contain enough fluoride should receive fluoride supplements. Both approaches can help prevent cavities in kids.
The Task Force also determined that there is not enough evidence to recommend for or against screening for tooth decay in the primary care setting for children under five. This is consistent with the Task Force’s 2014 recommendation on dental caries.
Dr. Cabana[/caption]
Michael Cabana, M.D., M.A., M.P.H
Professor of Pediatrics
Albert Einstein College of Medicine.
Physician-in-chief , Children's Hospital at Montefiore
Chair of the Department of Pediatrics
Albert Einstein College of Medicine
Member, U.S. Preventive Services Task Force
MedicalResearch.com: What is the background for this study and recommendation statement?
Response: Dental caries, also known as cavities or tooth decay, is the most common chronic disease in children in the United States and can develop in any child whose teeth have come in. Many young children under five years old do not visit a dentist, so the Task Force reviewed the latest evidence on how primary care clinicians can help prevent tooth decay in young children.
The Task Force’s research led to two important findings: all young children whose teeth have come in should have fluoride varnish applied by their clinician, and all children six months and older whose water supply doesn’t contain enough fluoride should receive fluoride supplements. Both approaches can help prevent cavities in kids.
The Task Force also determined that there is not enough evidence to recommend for or against screening for tooth decay in the primary care setting for children under five. This is consistent with the Task Force’s 2014 recommendation on dental caries.
 Dr. Cabana[/caption]
Michael Cabana, M.D., M.A., M.P.H
Professor of Pediatrics
Albert Einstein College of Medicine.
Physician-in-chief , Children's Hospital at Montefiore
Chair of the Department of Pediatrics
Albert Einstein College of Medicine
Member, U.S. Preventive Services Task Force
MedicalResearch.com: What is the background for this study and recommendation statement?
Response: Dental caries, also known as cavities or tooth decay, is the most common chronic disease in children in the United States and can develop in any child whose teeth have come in. Many young children under five years old do not visit a dentist, so the Task Force reviewed the latest evidence on how primary care clinicians can help prevent tooth decay in young children.
The Task Force’s research led to two important findings: all young children whose teeth have come in should have fluoride varnish applied by their clinician, and all children six months and older whose water supply doesn’t contain enough fluoride should receive fluoride supplements. Both approaches can help prevent cavities in kids.
The Task Force also determined that there is not enough evidence to recommend for or against screening for tooth decay in the primary care setting for children under five. This is consistent with the Task Force’s 2014 recommendation on dental caries.
Dr. Cabana[/caption]
Michael Cabana, M.D., M.A., M.P.H
Professor of Pediatrics
Albert Einstein College of Medicine.
Physician-in-chief , Children's Hospital at Montefiore
Chair of the Department of Pediatrics
Albert Einstein College of Medicine
Member, U.S. Preventive Services Task Force
MedicalResearch.com: What is the background for this study and recommendation statement?
Response: Dental caries, also known as cavities or tooth decay, is the most common chronic disease in children in the United States and can develop in any child whose teeth have come in. Many young children under five years old do not visit a dentist, so the Task Force reviewed the latest evidence on how primary care clinicians can help prevent tooth decay in young children.
The Task Force’s research led to two important findings: all young children whose teeth have come in should have fluoride varnish applied by their clinician, and all children six months and older whose water supply doesn’t contain enough fluoride should receive fluoride supplements. Both approaches can help prevent cavities in kids.
The Task Force also determined that there is not enough evidence to recommend for or against screening for tooth decay in the primary care setting for children under five. This is consistent with the Task Force’s 2014 recommendation on dental caries.







 Dr. Lee[/caption]
Cecilia S. Lee, MD, MS
Associate Professor,Director, Clinical Research
Department of Ophthalmology
Harborview Medical Center
University of Washington Seattle, WA
MedicalResearch.com: What is the background for this study?
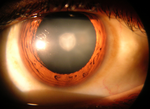
Response: Cataract is a natural aging process of the eye and affects the majority of older adults who are at risk for dementia. Sensory loss, including vision and hearing, is of interest to the research community as a possible risk factor for dementia, and also as a potential point of intervention. Because cataract surgery improves visual function, we hypothesized that older people who undergo cataract surgery may have a decreased risk of developing Alzheimer disease and dementia.
We used the longitudinal data from an ongoing, prospective, community based cohort, Adult Changes in Thought (ACT) study. The ACT study includes over 5000 participants to date who are dementia free at recruitment and followed until they develop Alzheimer disease or dementia. We had access to their extensive medical history including comprehensive ophthalmology visit data. We investigated whether cataract surgery was associated with a decreased risk of developing Alzheimer disease and dementia.
Dr. Lee[/caption]
Cecilia S. Lee, MD, MS
Associate Professor,Director, Clinical Research
Department of Ophthalmology
Harborview Medical Center
University of Washington Seattle, WA
MedicalResearch.com: What is the background for this study?
Response: Cataract is a natural aging process of the eye and affects the majority of older adults who are at risk for dementia. Sensory loss, including vision and hearing, is of interest to the research community as a possible risk factor for dementia, and also as a potential point of intervention. Because cataract surgery improves visual function, we hypothesized that older people who undergo cataract surgery may have a decreased risk of developing Alzheimer disease and dementia.
We used the longitudinal data from an ongoing, prospective, community based cohort, Adult Changes in Thought (ACT) study. The ACT study includes over 5000 participants to date who are dementia free at recruitment and followed until they develop Alzheimer disease or dementia. We had access to their extensive medical history including comprehensive ophthalmology visit data. We investigated whether cataract surgery was associated with a decreased risk of developing Alzheimer disease and dementia. 
 Dr. Smyth[/caption]
Professor Andrew Smyth MB, BCh, BAO, MMedSc, MRCPI, PhD
Professor of Clinical Epidemiology
NUI Galway
Director of the HRB-Clinical Research Facility Galway
Consultant Nephrologist at Galway University Hospitals
MedicalResearch.com: What is the background for this study?
Response: We know that there are multiple medium to long-term risk factors for stroke, as people with conditions such as hypertension (high blood pressure) or diabetes mellitus (high blood glucose levels) and those with risk factors (such as smoking, obesity, poor diet quality and others) are at increased risk of stroke. However, we still find it difficult to predict who will have a stroke.
We were interested in exploring if short-term exposures to anger or emotional upset or a period of heavy physical exertion might lead to, or ‘trigger’ a stroke. We looked at this previously for myocardial infarction (heart attack) in a study called INTERHEART. Some smaller studies have looked at this before, with less people experiencing a stroke and often confined to one country or geographical region. Here, in INTERSTROKE, we included over 13,000 people who had a stroke and asked about the one hour period before the onset of the stroke and also about the same period on the day before.
Dr. Smyth[/caption]
Professor Andrew Smyth MB, BCh, BAO, MMedSc, MRCPI, PhD
Professor of Clinical Epidemiology
NUI Galway
Director of the HRB-Clinical Research Facility Galway
Consultant Nephrologist at Galway University Hospitals
MedicalResearch.com: What is the background for this study?
Response: We know that there are multiple medium to long-term risk factors for stroke, as people with conditions such as hypertension (high blood pressure) or diabetes mellitus (high blood glucose levels) and those with risk factors (such as smoking, obesity, poor diet quality and others) are at increased risk of stroke. However, we still find it difficult to predict who will have a stroke.
We were interested in exploring if short-term exposures to anger or emotional upset or a period of heavy physical exertion might lead to, or ‘trigger’ a stroke. We looked at this previously for myocardial infarction (heart attack) in a study called INTERHEART. Some smaller studies have looked at this before, with less people experiencing a stroke and often confined to one country or geographical region. Here, in INTERSTROKE, we included over 13,000 people who had a stroke and asked about the one hour period before the onset of the stroke and also about the same period on the day before.

 Dr. Dalton[/caption]
Kristine Dalton PhD FAAO, FBCLA
School of Optometry & Vision Science
University of Waterloo
Waterloo, Canada
MedicalResearch.com: What is the background for this study?
Response: Dynamic visual acuity refers to the ability to detect and perceive small details in objects that are moving relative to an observer. Dynamic visual acuity is a complex visual function, that involves a number of different aspects of vision, including detecting the target, moving the eyes appropriately to observe the target, and processing the visual information from the target in the brain to interpret what we are seeing. What makes dynamic visual acuity so interesting to study, is that as a visual function, it appears to play an important role in a number of real-world situations, including playing sports, driving, and piloting, and it may provide us more information about how the visual system is functioning compared to the more traditional, static vision tests alone.
Previous research has demonstrated that consumption of caffeine has been shown to benefit physiological, psychomotor, and cognitive performance. More recently there has been an increased interest in studying the impacts of caffeine on the vision system, however the impact of caffeine on dynamic visual acuity has not been studied. This study was designed to address this limitation in the literature, particularly because dynamic visual acuity appears to be such an important visual function for real-world activities.
Dr. Dalton[/caption]
Kristine Dalton PhD FAAO, FBCLA
School of Optometry & Vision Science
University of Waterloo
Waterloo, Canada
MedicalResearch.com: What is the background for this study?
Response: Dynamic visual acuity refers to the ability to detect and perceive small details in objects that are moving relative to an observer. Dynamic visual acuity is a complex visual function, that involves a number of different aspects of vision, including detecting the target, moving the eyes appropriately to observe the target, and processing the visual information from the target in the brain to interpret what we are seeing. What makes dynamic visual acuity so interesting to study, is that as a visual function, it appears to play an important role in a number of real-world situations, including playing sports, driving, and piloting, and it may provide us more information about how the visual system is functioning compared to the more traditional, static vision tests alone.
Previous research has demonstrated that consumption of caffeine has been shown to benefit physiological, psychomotor, and cognitive performance. More recently there has been an increased interest in studying the impacts of caffeine on the vision system, however the impact of caffeine on dynamic visual acuity has not been studied. This study was designed to address this limitation in the literature, particularly because dynamic visual acuity appears to be such an important visual function for real-world activities. 
 Dr. Dickerman[/caption]
Dr. Barbra Dickerman, PhD
CAUSALab investigator and instructor
Department of Epidemiology
Harvard T.H. Chan School of Public Health
MedicalResearch.com: What is the background for this study?
Response: Early randomized trials showed that the BNT162b2 (Pfizer-BioNTech) and mRNA-1273 (Moderna) vaccines were both remarkably effective at preventing symptomatic disease, when comparing each vaccine with no vaccine. However, head-to-head comparisons of these vaccines have been lacking, leaving open the question of which vaccine is more effective.
In this study, we analyzed the VA’s high-quality databases in a way that emulated the design of the hypothetical trial that would have answered this question. Specifically, we used the findings from the original trials to benchmark our methods and then extended them to provide novel evidence for the comparative effectiveness of these two vaccines in a real-world setting and across diverse subgroups and different time periods.
Dr. Dickerman[/caption]
Dr. Barbra Dickerman, PhD
CAUSALab investigator and instructor
Department of Epidemiology
Harvard T.H. Chan School of Public Health
MedicalResearch.com: What is the background for this study?
Response: Early randomized trials showed that the BNT162b2 (Pfizer-BioNTech) and mRNA-1273 (Moderna) vaccines were both remarkably effective at preventing symptomatic disease, when comparing each vaccine with no vaccine. However, head-to-head comparisons of these vaccines have been lacking, leaving open the question of which vaccine is more effective.
In this study, we analyzed the VA’s high-quality databases in a way that emulated the design of the hypothetical trial that would have answered this question. Specifically, we used the findings from the original trials to benchmark our methods and then extended them to provide novel evidence for the comparative effectiveness of these two vaccines in a real-world setting and across diverse subgroups and different time periods.



 Dr. Shiou Liang[/caption]
Wee Shiou Liang, PhD
Associate Professor | Health and Social Sciences, Singapore Institute of Technology
Faculty | Geriatric Education and Research Institute
Singapore
MedicalResearch.com: What is the background for this study?
Response: This study was funded by Singapore’s Ministry of Health Geriatric Education and Research Institute.
We randomly recruited 500+ adults aged 21-90+ from the residential town of Yishun. We performed detailed assessments of physical and cognitive performance, body composition using DEXA, and participants also provided information on their levels and frequencies of physical activities (PA) including recreational PA/exercise, commuting, housework and other occupational related PA. The demographics of the sample of participants is the same as that of Singapore in terms of age and ethnic composition. Comparing the results of those aged 21-<65 and those >=65 years, only around a third (36%; 90) of those in the younger group and only around half (48%;116) of those in the older age group, met guidelines recommended physical activity quota exclusively from recreational PA/exercise. But nearly two thirds (61% younger; 152 and 66% older; 159) met this target exclusively through housework.
Dr. Shiou Liang[/caption]
Wee Shiou Liang, PhD
Associate Professor | Health and Social Sciences, Singapore Institute of Technology
Faculty | Geriatric Education and Research Institute
Singapore
MedicalResearch.com: What is the background for this study?
Response: This study was funded by Singapore’s Ministry of Health Geriatric Education and Research Institute.
We randomly recruited 500+ adults aged 21-90+ from the residential town of Yishun. We performed detailed assessments of physical and cognitive performance, body composition using DEXA, and participants also provided information on their levels and frequencies of physical activities (PA) including recreational PA/exercise, commuting, housework and other occupational related PA. The demographics of the sample of participants is the same as that of Singapore in terms of age and ethnic composition. Comparing the results of those aged 21-<65 and those >=65 years, only around a third (36%; 90) of those in the younger group and only around half (48%;116) of those in the older age group, met guidelines recommended physical activity quota exclusively from recreational PA/exercise. But nearly two thirds (61% younger; 152 and 66% older; 159) met this target exclusively through housework.


 Dr. Woodruff[/caption]
Carina M. Woodruff, MD
Department of Dermatolog
University of California, San Francisco
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Rigorous hand hygiene has been an important component of the CDC's COVID-19 guidelines. With millions of Americans now using hand sanitizers regularly, we are seeing many more cases of hand dermatitis. Our study evaluated the key product features and most common allergens in the top-reviewed, commercial hand sanitizers sold by major US retailers.
We found that the most common potential allergens were tocopherol, fragrance, propylene glycol and phenoxyethanol. Our study also showed that nearly 1 in 5 marketing claims on these products was misleading. For example, 70% of sanitizers with the marketing claim "hypoallergenic" included at least one common allergen in its formulation.
Dr. Woodruff[/caption]
Carina M. Woodruff, MD
Department of Dermatolog
University of California, San Francisco
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Rigorous hand hygiene has been an important component of the CDC's COVID-19 guidelines. With millions of Americans now using hand sanitizers regularly, we are seeing many more cases of hand dermatitis. Our study evaluated the key product features and most common allergens in the top-reviewed, commercial hand sanitizers sold by major US retailers.
We found that the most common potential allergens were tocopherol, fragrance, propylene glycol and phenoxyethanol. Our study also showed that nearly 1 in 5 marketing claims on these products was misleading. For example, 70% of sanitizers with the marketing claim "hypoallergenic" included at least one common allergen in its formulation.


 Dr. Israel[/caption]
Ariel Israel, M.D., Ph.D.
Director, Leumit Health Services
Tel Aviv, Israel
MedicalResearch.com: What is the background for this study?
Response: As a research institute of Leumit, one of the four state mandated health funds in Israel, we pursue research projects aimed at improving the health of our members, and reducing the burden of disease. For this purpose, we harness the unique resource of the electronic health records of our members, that is available in a central data warehouse for research purposes.
Israel was one of the first countries to roll-out a large-scale vaccination campaign, and to achieve control of the pandemics through vaccination. Nevertheless, since the middle of June '21, we have observed a gradual increase in the rate of COVID-19 infections among our members, even among the vaccinated. This increase was first believed to be due to the emergence of the delta strain, but when we compared vaccinated individuals who suffered from breakthrough infections to other vaccinated individuals, we found that the time that has elapsed since vaccination was significantly longer for individuals who got infected with COVID-19, in each of the age groups.
This prompted us to investigate the issue of a possible waning effect of the vaccine protection with time, that we present in this report, using the test negative study design.
We examined the electronic health records for 80,057 adults (average age 44 years) who received a PCR test at least three weeks after their second injection, and had no evidence of previous covid-19 infection. Of these 80,057 participants, 7,973 (9.6%) had a positive test result. These individuals were then matched to negative controls of the same age and ethnic group who were tested in the same week.
Dr. Israel[/caption]
Ariel Israel, M.D., Ph.D.
Director, Leumit Health Services
Tel Aviv, Israel
MedicalResearch.com: What is the background for this study?
Response: As a research institute of Leumit, one of the four state mandated health funds in Israel, we pursue research projects aimed at improving the health of our members, and reducing the burden of disease. For this purpose, we harness the unique resource of the electronic health records of our members, that is available in a central data warehouse for research purposes.
Israel was one of the first countries to roll-out a large-scale vaccination campaign, and to achieve control of the pandemics through vaccination. Nevertheless, since the middle of June '21, we have observed a gradual increase in the rate of COVID-19 infections among our members, even among the vaccinated. This increase was first believed to be due to the emergence of the delta strain, but when we compared vaccinated individuals who suffered from breakthrough infections to other vaccinated individuals, we found that the time that has elapsed since vaccination was significantly longer for individuals who got infected with COVID-19, in each of the age groups.
This prompted us to investigate the issue of a possible waning effect of the vaccine protection with time, that we present in this report, using the test negative study design.
We examined the electronic health records for 80,057 adults (average age 44 years) who received a PCR test at least three weeks after their second injection, and had no evidence of previous covid-19 infection. Of these 80,057 participants, 7,973 (9.6%) had a positive test result. These individuals were then matched to negative controls of the same age and ethnic group who were tested in the same week.


 Dr. Ashwin Nathan[/caption]
Ashwin Nathan, MD, MSHP
Assistant Professor, Medicine, Perelman School of Medicine
Interventional Cardiologist
Hospital of the University of Pennsylvania and at the
Corporal Michael C. Crescenz VA Medical Center in Philadelphia
Penn Cardiovascular Outcomes, Quality & Evaluative Research Center
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: We found that the rates of TAVR were lower in areas with higher proportions of Black, Hispanic and socioeconomically disadvantaged patients. Inequities in access in areas with higher proportions of Black and Hispanic patients existed despite adjusting for socioeconomic status.
Dr. Ashwin Nathan[/caption]
Ashwin Nathan, MD, MSHP
Assistant Professor, Medicine, Perelman School of Medicine
Interventional Cardiologist
Hospital of the University of Pennsylvania and at the
Corporal Michael C. Crescenz VA Medical Center in Philadelphia
Penn Cardiovascular Outcomes, Quality & Evaluative Research Center
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: We found that the rates of TAVR were lower in areas with higher proportions of Black, Hispanic and socioeconomically disadvantaged patients. Inequities in access in areas with higher proportions of Black and Hispanic patients existed despite adjusting for socioeconomic status.






 Kelly Gavigan[/caption]
Kelly Gavigan, MPH
Manager, Research and Data Science
Kelly Gavigan[/caption]
Kelly Gavigan, MPH
Manager, Research and Data Science

