Anxiety, poor quality of sleep, and sleep apnea are all interrelated in many cases....
Addiction / 27.12.2022
A Guide to Drug Rehabilitation
Addiction is a serious problem that affects millions of people across the world. If you or someone you love is struggling with addiction, it’s important to know that there is hope. Drug rehabilitation centers provide individuals with the resources they need to break free from addiction and start living a healthier, more productive life.
What Is Drug Rehab?
Drug rehab centers are treatment facilities that specialize in helping individuals overcome their addictions. These centers offer individualized treatments plans and support services designed to help individuals learn how to manage their cravings for drugs or alcohol and develop healthy coping skills that will allow them to resist temptation in the future. Additionally, drug rehab centers also provide educational programs and therapy sessions to help patients gain a better understanding of their addiction and how it has impacted their lives.
You might have heard good things about CBD oil. You heard that it can assist with numerous conditions and symptoms. However, what you heard might have been simply hearsay and not necessarily proven fact. What you want to know is the science-backed health benefits about CBD oil from actual studies and research, which we provide below.
- Alleviate Stress & Anxiety
Author Interviews, Biomarkers, Heart Disease, JACC, University of Michigan / 21.12.2022
U Michigan Study Finds Biomarkers Can Predict Myocarditis from Immune Checkpoint Inhibitors
MedicalResearch.com Interview with:
[caption id="attachment_59873" align="alignleft" width="130"] Dr. Hayek[/caption]
Salim S. Hayek MD
Assistant Professor
Medical Director of the Frankel Cardiovascular Center Clinics
University of Michigan
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Essentially, immune checkpoint myocarditis is a rare but deadly complication of immune checkpoint inhibitors – amazing drugs that are increasingly used for the treatment of various cancers. Most patients present late, and when they do, they’re very ill and have a 50% chance of death.
Diagnosing ICI myocarditis is challenging, given there is no one test that can differentiate it from other causes of cardiac injury. It is important to diagnose it fast, early and accurately in order to start immunosuppressive therapy as soon as possible.
What we did in this study was look at commonly measured biomarkers in all patients receiving ICI at the University of Michigan.
What we found was that patients who developed ICI myocarditis had early signs of muscle destruction (rise in CPK) levels and hepatitis (rise in AST, ALT), and that all patients who had myocarditis with bad outcomes had rises in all of the aforementioned biomarkers. Creatinine phosphokinase was the most sensitive.
Dr. Hayek[/caption]
Salim S. Hayek MD
Assistant Professor
Medical Director of the Frankel Cardiovascular Center Clinics
University of Michigan
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Essentially, immune checkpoint myocarditis is a rare but deadly complication of immune checkpoint inhibitors – amazing drugs that are increasingly used for the treatment of various cancers. Most patients present late, and when they do, they’re very ill and have a 50% chance of death.
Diagnosing ICI myocarditis is challenging, given there is no one test that can differentiate it from other causes of cardiac injury. It is important to diagnose it fast, early and accurately in order to start immunosuppressive therapy as soon as possible.
What we did in this study was look at commonly measured biomarkers in all patients receiving ICI at the University of Michigan.
What we found was that patients who developed ICI myocarditis had early signs of muscle destruction (rise in CPK) levels and hepatitis (rise in AST, ALT), and that all patients who had myocarditis with bad outcomes had rises in all of the aforementioned biomarkers. Creatinine phosphokinase was the most sensitive.
 Dr. Hayek[/caption]
Salim S. Hayek MD
Assistant Professor
Medical Director of the Frankel Cardiovascular Center Clinics
University of Michigan
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Essentially, immune checkpoint myocarditis is a rare but deadly complication of immune checkpoint inhibitors – amazing drugs that are increasingly used for the treatment of various cancers. Most patients present late, and when they do, they’re very ill and have a 50% chance of death.
Diagnosing ICI myocarditis is challenging, given there is no one test that can differentiate it from other causes of cardiac injury. It is important to diagnose it fast, early and accurately in order to start immunosuppressive therapy as soon as possible.
What we did in this study was look at commonly measured biomarkers in all patients receiving ICI at the University of Michigan.
What we found was that patients who developed ICI myocarditis had early signs of muscle destruction (rise in CPK) levels and hepatitis (rise in AST, ALT), and that all patients who had myocarditis with bad outcomes had rises in all of the aforementioned biomarkers. Creatinine phosphokinase was the most sensitive.
Dr. Hayek[/caption]
Salim S. Hayek MD
Assistant Professor
Medical Director of the Frankel Cardiovascular Center Clinics
University of Michigan
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Essentially, immune checkpoint myocarditis is a rare but deadly complication of immune checkpoint inhibitors – amazing drugs that are increasingly used for the treatment of various cancers. Most patients present late, and when they do, they’re very ill and have a 50% chance of death.
Diagnosing ICI myocarditis is challenging, given there is no one test that can differentiate it from other causes of cardiac injury. It is important to diagnose it fast, early and accurately in order to start immunosuppressive therapy as soon as possible.
What we did in this study was look at commonly measured biomarkers in all patients receiving ICI at the University of Michigan.
What we found was that patients who developed ICI myocarditis had early signs of muscle destruction (rise in CPK) levels and hepatitis (rise in AST, ALT), and that all patients who had myocarditis with bad outcomes had rises in all of the aforementioned biomarkers. Creatinine phosphokinase was the most sensitive.
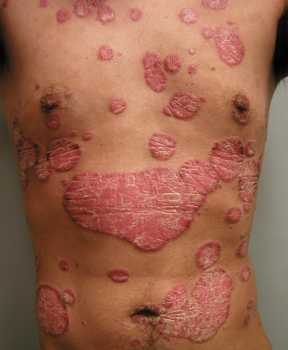
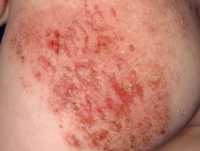
Autoimmune skin conditions like Psoriasis can lead to a lifetime of problems. Treatments are one of the many steps professionals...
Accidents & Violence, Author Interviews, JAMA, Pediatrics / 20.12.2022
Child Homicides, Rising for Years, Rise Sharply in 2020
MedicalResearch.com Interview with:
Rebecca F. Wilson, PhD
Division of Violence Prevention
National Center for Injury Prevention and Control
US Centers for Disease Control and Prevention, Atlanta, Georgia
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Our report shows the homicide rate among children aged 0 to 17 years has been increasing annually on average 4.3% since 2013, and rose sharply from 2019 to 2020. The largest 2019 to 2020 rate increases were among children 11-17 years old, boys, and Black children. Overall increases varied by geography and demographics, with some racial and ethnic disparities persisting for more than 20 years. Firearms were the most common weapon used in child homicides. Homicides of younger children (infants to 10 years) were mostly perpetrated by parents and caregivers and precipitated by abuse and/or neglect.
Homicides of older children (11-17 years) were mostly perpetrated by someone known to them, like a friend or acquaintance, and precipitated by crime, arguments, and community violence.
Author Interviews, Neurology / 19.12.2022
Reeve Foundation: Results of “Living with Paralysis & Caregiver National Survey”
MedicalResearch.com Interview with:
[caption id="attachment_59862" align="alignleft" width="200"] Regina Blye[/caption]
Regina Blye, Chief Program and Policy Officer
Discusses the Living with Paralysis & Caregiver National Survey
Conducted by the Christopher and Dana Reeve Foundation
MedicalResearch.com: How large is the population of Americans living with paralysis?
Response: There is a significant population of Americans living with paralysis. To note, a 2013 study by the Christopher & Dana Reeve Foundation found that 1 in 50 people in the US are living with paralysis. This is approximately 5.4 million people. I, myself, have lived with a spinal cord injury (SCI) for over 35 years. While some progress has been made over the past few decades, there is still work to be done.
In a new survey conducted by the Christopher & Dana Reeve Foundation called “Living with Paralysis & Caregiver National Survey,” we learned that a majority of Americans (69%) underestimate the prevalence of those living with paralysis in the U.S. - about two out of every 100 individuals.
Given the notable size of the population, we must work together to educate and inform families, business leaders, advocates, policymakers and the general public to help improve the quality of life for those living with, or impacted by paralysis.
The Christopher & Dana Reeve Foundation is dedicated to curing spinal cord injury by advancing innovative research and improving the quality of life for individuals and families impacted by paralysis. While we’ve been fortunate to make advancements with significant support from the community, we must all unite to accelerate comprehensive information, resources, referral services, and innovative research together.
Regina Blye[/caption]
Regina Blye, Chief Program and Policy Officer
Discusses the Living with Paralysis & Caregiver National Survey
Conducted by the Christopher and Dana Reeve Foundation
MedicalResearch.com: How large is the population of Americans living with paralysis?
Response: There is a significant population of Americans living with paralysis. To note, a 2013 study by the Christopher & Dana Reeve Foundation found that 1 in 50 people in the US are living with paralysis. This is approximately 5.4 million people. I, myself, have lived with a spinal cord injury (SCI) for over 35 years. While some progress has been made over the past few decades, there is still work to be done.
In a new survey conducted by the Christopher & Dana Reeve Foundation called “Living with Paralysis & Caregiver National Survey,” we learned that a majority of Americans (69%) underestimate the prevalence of those living with paralysis in the U.S. - about two out of every 100 individuals.
Given the notable size of the population, we must work together to educate and inform families, business leaders, advocates, policymakers and the general public to help improve the quality of life for those living with, or impacted by paralysis.
The Christopher & Dana Reeve Foundation is dedicated to curing spinal cord injury by advancing innovative research and improving the quality of life for individuals and families impacted by paralysis. While we’ve been fortunate to make advancements with significant support from the community, we must all unite to accelerate comprehensive information, resources, referral services, and innovative research together.
 Regina Blye[/caption]
Regina Blye, Chief Program and Policy Officer
Discusses the Living with Paralysis & Caregiver National Survey
Conducted by the Christopher and Dana Reeve Foundation
MedicalResearch.com: How large is the population of Americans living with paralysis?
Response: There is a significant population of Americans living with paralysis. To note, a 2013 study by the Christopher & Dana Reeve Foundation found that 1 in 50 people in the US are living with paralysis. This is approximately 5.4 million people. I, myself, have lived with a spinal cord injury (SCI) for over 35 years. While some progress has been made over the past few decades, there is still work to be done.
In a new survey conducted by the Christopher & Dana Reeve Foundation called “Living with Paralysis & Caregiver National Survey,” we learned that a majority of Americans (69%) underestimate the prevalence of those living with paralysis in the U.S. - about two out of every 100 individuals.
Given the notable size of the population, we must work together to educate and inform families, business leaders, advocates, policymakers and the general public to help improve the quality of life for those living with, or impacted by paralysis.
The Christopher & Dana Reeve Foundation is dedicated to curing spinal cord injury by advancing innovative research and improving the quality of life for individuals and families impacted by paralysis. While we’ve been fortunate to make advancements with significant support from the community, we must all unite to accelerate comprehensive information, resources, referral services, and innovative research together.
Regina Blye[/caption]
Regina Blye, Chief Program and Policy Officer
Discusses the Living with Paralysis & Caregiver National Survey
Conducted by the Christopher and Dana Reeve Foundation
MedicalResearch.com: How large is the population of Americans living with paralysis?
Response: There is a significant population of Americans living with paralysis. To note, a 2013 study by the Christopher & Dana Reeve Foundation found that 1 in 50 people in the US are living with paralysis. This is approximately 5.4 million people. I, myself, have lived with a spinal cord injury (SCI) for over 35 years. While some progress has been made over the past few decades, there is still work to be done.
In a new survey conducted by the Christopher & Dana Reeve Foundation called “Living with Paralysis & Caregiver National Survey,” we learned that a majority of Americans (69%) underestimate the prevalence of those living with paralysis in the U.S. - about two out of every 100 individuals.
Given the notable size of the population, we must work together to educate and inform families, business leaders, advocates, policymakers and the general public to help improve the quality of life for those living with, or impacted by paralysis.
The Christopher & Dana Reeve Foundation is dedicated to curing spinal cord injury by advancing innovative research and improving the quality of life for individuals and families impacted by paralysis. While we’ve been fortunate to make advancements with significant support from the community, we must all unite to accelerate comprehensive information, resources, referral services, and innovative research together.
Author Interviews, Cost of Health Care, JAMA / 19.12.2022
Physician Weekly Work Hours Fall Especially for Doctor Fathers
MedicalResearch.com Interview with:
[caption id="attachment_59851" align="alignleft" width="125"] Dr. Goldman[/caption]
Anna L. Goldman, M.D., M.P.A., M.P.H
Assistant Professor of Medicine
General Internal Medicine
Boston University Chobanian & Avedisian School of Medicine
MedicalResearch.com: What is the background for this study?
Response: Experts on the healthcare labor market have long debated the existence and magnitude of a physician shortage. Physician work hours are a major contributor to physician supply issues, but little research is available on recent trends in work hours by physicians. In addition, no available studies have rigorously estimated changes in the physician workforce size during the pandemic.
Dr. Goldman[/caption]
Anna L. Goldman, M.D., M.P.A., M.P.H
Assistant Professor of Medicine
General Internal Medicine
Boston University Chobanian & Avedisian School of Medicine
MedicalResearch.com: What is the background for this study?
Response: Experts on the healthcare labor market have long debated the existence and magnitude of a physician shortage. Physician work hours are a major contributor to physician supply issues, but little research is available on recent trends in work hours by physicians. In addition, no available studies have rigorously estimated changes in the physician workforce size during the pandemic.
 Dr. Goldman[/caption]
Anna L. Goldman, M.D., M.P.A., M.P.H
Assistant Professor of Medicine
General Internal Medicine
Boston University Chobanian & Avedisian School of Medicine
MedicalResearch.com: What is the background for this study?
Response: Experts on the healthcare labor market have long debated the existence and magnitude of a physician shortage. Physician work hours are a major contributor to physician supply issues, but little research is available on recent trends in work hours by physicians. In addition, no available studies have rigorously estimated changes in the physician workforce size during the pandemic.
Dr. Goldman[/caption]
Anna L. Goldman, M.D., M.P.A., M.P.H
Assistant Professor of Medicine
General Internal Medicine
Boston University Chobanian & Avedisian School of Medicine
MedicalResearch.com: What is the background for this study?
Response: Experts on the healthcare labor market have long debated the existence and magnitude of a physician shortage. Physician work hours are a major contributor to physician supply issues, but little research is available on recent trends in work hours by physicians. In addition, no available studies have rigorously estimated changes in the physician workforce size during the pandemic.
Addiction, Author Interviews / 19.12.2022
Molecular Containers May Be Able to Bind and Reverse Effects of Dangerous Addictive Drugs
MedicalResearch.com Interview with:
[caption id="attachment_59854" align="alignleft" width="150"] Prof. Isaacs[/caption]
Lyle Isaacs, Professor
University of Maryland
Prof. Isaacs[/caption]
Lyle Isaacs, Professor
University of Maryland
Department of Chemistry and Biochemistry
College Park, MD 20742 MedicalResearch.com: What is the background for this study? Response: The Isaacs laboratory has a long-standing interest in molecular containers compounds and their molecular recognition properties toward chemically and biologically important targets. Molecular containers include well known pharmaceutical excipients that help dissolve and deliver drugs (e.g. sulfobutyl-beta-cyclodextrin (SBE-b-CD)) and even sequester active pharmaceutical ingredients (e.g. Sugammadex reverses the effects of neuromuscular blockers). Our lab has previously studied a class of molecular containers called cucurbiturils and found that they bind tightly (nanomolar Kd) to hydrophobic cations in aqueous solution. Recently, we translated our knowledge of tight binding to design and synthesize a novel tight binding molecular container known as Pillar[6]MaxQ and showed that it has superior binding affinity toward hydrophobic cations.[reference = Angewandte Chemie International Edition 2020, 59, 13313]
 Prof. Isaacs[/caption]
Lyle Isaacs, Professor
University of Maryland
Prof. Isaacs[/caption]
Lyle Isaacs, Professor
University of Maryland Department of Chemistry and Biochemistry
College Park, MD 20742 MedicalResearch.com: What is the background for this study? Response: The Isaacs laboratory has a long-standing interest in molecular containers compounds and their molecular recognition properties toward chemically and biologically important targets. Molecular containers include well known pharmaceutical excipients that help dissolve and deliver drugs (e.g. sulfobutyl-beta-cyclodextrin (SBE-b-CD)) and even sequester active pharmaceutical ingredients (e.g. Sugammadex reverses the effects of neuromuscular blockers). Our lab has previously studied a class of molecular containers called cucurbiturils and found that they bind tightly (nanomolar Kd) to hydrophobic cations in aqueous solution. Recently, we translated our knowledge of tight binding to design and synthesize a novel tight binding molecular container known as Pillar[6]MaxQ and showed that it has superior binding affinity toward hydrophobic cations.[reference = Angewandte Chemie International Edition 2020, 59, 13313]
Addiction / 16.12.2022
The Benefits of an Intensive Outpatient Program
In an intensive outpatient program, patients have the opportunity to meet with their therapist or case manager multiple times per...
Accidents & Violence, Aging, Author Interviews, BMJ, Brain Injury, Brigham & Women's - Harvard, Exercise - Fitness / 15.12.2022
NFL Players Found to Lose About 10 Years of HealthSpan
MedicalResearch.com Interview with:
[caption id="attachment_59841" align="alignleft" width="150"] Dr. Grashow[/caption]
Rachel Grashow PhD
Research Scientist
Department of Environmental Health
Football Players Health Study at Harvard University
Harvard T.H. Chan School of Public Health
MedicalResearch.com: What is the background for this study?
Response: Anecdotally, we heard from former NFL players that they felt older than their chronological age. At the same time, doctors and medical care providers treating former players also observed that players appeared clinically older in some health domains. These observations motivated us to ask: despite superior fitness and success as young men, are football players experiencing early aging and living with illness and disability for more years than their non-football peers?
Dr. Grashow[/caption]
Rachel Grashow PhD
Research Scientist
Department of Environmental Health
Football Players Health Study at Harvard University
Harvard T.H. Chan School of Public Health
MedicalResearch.com: What is the background for this study?
Response: Anecdotally, we heard from former NFL players that they felt older than their chronological age. At the same time, doctors and medical care providers treating former players also observed that players appeared clinically older in some health domains. These observations motivated us to ask: despite superior fitness and success as young men, are football players experiencing early aging and living with illness and disability for more years than their non-football peers?
 Dr. Grashow[/caption]
Rachel Grashow PhD
Research Scientist
Department of Environmental Health
Football Players Health Study at Harvard University
Harvard T.H. Chan School of Public Health
MedicalResearch.com: What is the background for this study?
Response: Anecdotally, we heard from former NFL players that they felt older than their chronological age. At the same time, doctors and medical care providers treating former players also observed that players appeared clinically older in some health domains. These observations motivated us to ask: despite superior fitness and success as young men, are football players experiencing early aging and living with illness and disability for more years than their non-football peers?
Dr. Grashow[/caption]
Rachel Grashow PhD
Research Scientist
Department of Environmental Health
Football Players Health Study at Harvard University
Harvard T.H. Chan School of Public Health
MedicalResearch.com: What is the background for this study?
Response: Anecdotally, we heard from former NFL players that they felt older than their chronological age. At the same time, doctors and medical care providers treating former players also observed that players appeared clinically older in some health domains. These observations motivated us to ask: despite superior fitness and success as young men, are football players experiencing early aging and living with illness and disability for more years than their non-football peers?
Addiction, Author Interviews, JAMA, Mental Health Research, Race/Ethnic Diversity, University of Pennsylvania / 15.12.2022
Overdose Deaths Among Black Women: High and Rising
[caption id="attachment_59828" align="alignleft" width="150"] Dr. Harris[/caption]
MedicalResearch.com Interview with:
Rebecca Arden Harris, MD, MSc
Assistant Professor of Family Medicine and Community Health at the Hospital of the University of Pennsylvania
Senior Fellow, Leonard Davis Institute of Health Economics
Perelman School of Medicine, University of Pennsylvania
MedicalResearch.com: What is the background for this study?
Response: The impact of the nationwide overdose epidemic on Black women has received little attention from policy-makers, researchers, or the press.
MedicalResearch.com: What are the main findings?
Response: Over the 7-year study period, preventable overdose deaths among Black women resulted in nearly 0.75 million years of life lost (YLL). Women aged 25-34 have suffered a rising proportion of this burden.
Dr. Harris[/caption]
MedicalResearch.com Interview with:
Rebecca Arden Harris, MD, MSc
Assistant Professor of Family Medicine and Community Health at the Hospital of the University of Pennsylvania
Senior Fellow, Leonard Davis Institute of Health Economics
Perelman School of Medicine, University of Pennsylvania
MedicalResearch.com: What is the background for this study?
Response: The impact of the nationwide overdose epidemic on Black women has received little attention from policy-makers, researchers, or the press.
MedicalResearch.com: What are the main findings?
Response: Over the 7-year study period, preventable overdose deaths among Black women resulted in nearly 0.75 million years of life lost (YLL). Women aged 25-34 have suffered a rising proportion of this burden.
 Dr. Harris[/caption]
MedicalResearch.com Interview with:
Rebecca Arden Harris, MD, MSc
Assistant Professor of Family Medicine and Community Health at the Hospital of the University of Pennsylvania
Senior Fellow, Leonard Davis Institute of Health Economics
Perelman School of Medicine, University of Pennsylvania
MedicalResearch.com: What is the background for this study?
Response: The impact of the nationwide overdose epidemic on Black women has received little attention from policy-makers, researchers, or the press.
MedicalResearch.com: What are the main findings?
Response: Over the 7-year study period, preventable overdose deaths among Black women resulted in nearly 0.75 million years of life lost (YLL). Women aged 25-34 have suffered a rising proportion of this burden.
Dr. Harris[/caption]
MedicalResearch.com Interview with:
Rebecca Arden Harris, MD, MSc
Assistant Professor of Family Medicine and Community Health at the Hospital of the University of Pennsylvania
Senior Fellow, Leonard Davis Institute of Health Economics
Perelman School of Medicine, University of Pennsylvania
MedicalResearch.com: What is the background for this study?
Response: The impact of the nationwide overdose epidemic on Black women has received little attention from policy-makers, researchers, or the press.
MedicalResearch.com: What are the main findings?
Response: Over the 7-year study period, preventable overdose deaths among Black women resulted in nearly 0.75 million years of life lost (YLL). Women aged 25-34 have suffered a rising proportion of this burden.
Author Interviews, Genetic Research, Infections, Neurological Disorders / 14.12.2022
Genetic Test Can Predict Predisposition to Drug-Induced Brain Infection PML
MedicalResearch.com Interview with:
[caption id="attachment_59834" align="alignleft" width="150"] Dr. Hatchwell[/caption]
Dr. Eli Hatchwell, MA MB BChir (Cantab) DPhil (Oxon) BA (OU)
Chief Scientific Officer
Population Bio UK, Inc.
Begbroke Science Park Begbroke Hill
Begbroke, Oxfordshire
United Kingdom
MedicalResearch.com: What is the background for this study?
Response: Progressive Multifocal Leukoencephalopathy (PML) is a devastating condition that is associated with a number of clinical situations, including treatment with a variety of drugs. Of these, the best known is natalizumab (Tysabri), which is a very successful drug in the treatment of MS (multiple sclerosis). Only a small proportion of patients treated with natalizumab develop PML and this has always been a mystery. The study was based on a hypothesis that some individuals have an underlying susceptibility to developing PML, based on the presence of variants in genes that are important in the immune system. The study identified several of these variants.
Dr. Hatchwell[/caption]
Dr. Eli Hatchwell, MA MB BChir (Cantab) DPhil (Oxon) BA (OU)
Chief Scientific Officer
Population Bio UK, Inc.
Begbroke Science Park Begbroke Hill
Begbroke, Oxfordshire
United Kingdom
MedicalResearch.com: What is the background for this study?
Response: Progressive Multifocal Leukoencephalopathy (PML) is a devastating condition that is associated with a number of clinical situations, including treatment with a variety of drugs. Of these, the best known is natalizumab (Tysabri), which is a very successful drug in the treatment of MS (multiple sclerosis). Only a small proportion of patients treated with natalizumab develop PML and this has always been a mystery. The study was based on a hypothesis that some individuals have an underlying susceptibility to developing PML, based on the presence of variants in genes that are important in the immune system. The study identified several of these variants.
 Dr. Hatchwell[/caption]
Dr. Eli Hatchwell, MA MB BChir (Cantab) DPhil (Oxon) BA (OU)
Chief Scientific Officer
Population Bio UK, Inc.
Begbroke Science Park Begbroke Hill
Begbroke, Oxfordshire
United Kingdom
MedicalResearch.com: What is the background for this study?
Response: Progressive Multifocal Leukoencephalopathy (PML) is a devastating condition that is associated with a number of clinical situations, including treatment with a variety of drugs. Of these, the best known is natalizumab (Tysabri), which is a very successful drug in the treatment of MS (multiple sclerosis). Only a small proportion of patients treated with natalizumab develop PML and this has always been a mystery. The study was based on a hypothesis that some individuals have an underlying susceptibility to developing PML, based on the presence of variants in genes that are important in the immune system. The study identified several of these variants.
Dr. Hatchwell[/caption]
Dr. Eli Hatchwell, MA MB BChir (Cantab) DPhil (Oxon) BA (OU)
Chief Scientific Officer
Population Bio UK, Inc.
Begbroke Science Park Begbroke Hill
Begbroke, Oxfordshire
United Kingdom
MedicalResearch.com: What is the background for this study?
Response: Progressive Multifocal Leukoencephalopathy (PML) is a devastating condition that is associated with a number of clinical situations, including treatment with a variety of drugs. Of these, the best known is natalizumab (Tysabri), which is a very successful drug in the treatment of MS (multiple sclerosis). Only a small proportion of patients treated with natalizumab develop PML and this has always been a mystery. The study was based on a hypothesis that some individuals have an underlying susceptibility to developing PML, based on the presence of variants in genes that are important in the immune system. The study identified several of these variants.
Author Interviews, Dermatology, Lancet / 13.12.2022
Atopic Dermatitis- Eczema: New Antibody Therapy Has Potential to Modify Disease Course
MedicalResearch.com Interview with:
[caption id="attachment_59823" align="alignleft" width="130"] Dr. Guttman-Yassky[/caption]
Dr. Emma Guttman-Yassky, MD, PhD
Waldman Professor and System Chair
The Kimberly and Eric J. Waldman Department of Dermatology
Director, Center of Excellence in Eczema
Director, Laboratory of Inflammatory Skin Diseases
Icahn School of Medicine at Mount Sinai
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The background for this study are studies that show that OX40 is a pathway that is upregulated in patients with atopic dermatitis (or eczema). OX40 is involved in activation of immune molecules associated with allergy and atopy, and also with formation of memory immune cells that are required for disease recurrence. The hypothesis to the study was that giving an OX40 antagonist will not only ameliorate the disease but perhaps have a remittive effect in that the disease will not come back.
Indeed all drug doses were significantly effective at week 16, the primary endpoint compared to placebo and continued to improve towards week 36, the secondary endpoint. In addition, the responders to treatment maintained their responses for an additional 20 weeks, which is unusual, suggesting a potential for disease modification.
Dr. Guttman-Yassky[/caption]
Dr. Emma Guttman-Yassky, MD, PhD
Waldman Professor and System Chair
The Kimberly and Eric J. Waldman Department of Dermatology
Director, Center of Excellence in Eczema
Director, Laboratory of Inflammatory Skin Diseases
Icahn School of Medicine at Mount Sinai
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The background for this study are studies that show that OX40 is a pathway that is upregulated in patients with atopic dermatitis (or eczema). OX40 is involved in activation of immune molecules associated with allergy and atopy, and also with formation of memory immune cells that are required for disease recurrence. The hypothesis to the study was that giving an OX40 antagonist will not only ameliorate the disease but perhaps have a remittive effect in that the disease will not come back.
Indeed all drug doses were significantly effective at week 16, the primary endpoint compared to placebo and continued to improve towards week 36, the secondary endpoint. In addition, the responders to treatment maintained their responses for an additional 20 weeks, which is unusual, suggesting a potential for disease modification.
 Dr. Guttman-Yassky[/caption]
Dr. Emma Guttman-Yassky, MD, PhD
Waldman Professor and System Chair
The Kimberly and Eric J. Waldman Department of Dermatology
Director, Center of Excellence in Eczema
Director, Laboratory of Inflammatory Skin Diseases
Icahn School of Medicine at Mount Sinai
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The background for this study are studies that show that OX40 is a pathway that is upregulated in patients with atopic dermatitis (or eczema). OX40 is involved in activation of immune molecules associated with allergy and atopy, and also with formation of memory immune cells that are required for disease recurrence. The hypothesis to the study was that giving an OX40 antagonist will not only ameliorate the disease but perhaps have a remittive effect in that the disease will not come back.
Indeed all drug doses were significantly effective at week 16, the primary endpoint compared to placebo and continued to improve towards week 36, the secondary endpoint. In addition, the responders to treatment maintained their responses for an additional 20 weeks, which is unusual, suggesting a potential for disease modification.
Dr. Guttman-Yassky[/caption]
Dr. Emma Guttman-Yassky, MD, PhD
Waldman Professor and System Chair
The Kimberly and Eric J. Waldman Department of Dermatology
Director, Center of Excellence in Eczema
Director, Laboratory of Inflammatory Skin Diseases
Icahn School of Medicine at Mount Sinai
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The background for this study are studies that show that OX40 is a pathway that is upregulated in patients with atopic dermatitis (or eczema). OX40 is involved in activation of immune molecules associated with allergy and atopy, and also with formation of memory immune cells that are required for disease recurrence. The hypothesis to the study was that giving an OX40 antagonist will not only ameliorate the disease but perhaps have a remittive effect in that the disease will not come back.
Indeed all drug doses were significantly effective at week 16, the primary endpoint compared to placebo and continued to improve towards week 36, the secondary endpoint. In addition, the responders to treatment maintained their responses for an additional 20 weeks, which is unusual, suggesting a potential for disease modification.
Author Interviews, CHEST, Pulmonary Disease, Sleep Disorders / 12.12.2022
Severe Obstructive Sleep Apnea Associated with Increased Risk of Hospitalization with Pneumonia
MedicalResearch.com Interview with:
[caption id="attachment_59819" align="alignleft" width="150"] Dr. Lutsey[/caption]
Pamela L. Lutsey, PhD, MPH
Minneapolis, Minnesota
Professor, Division of Epidemiology and Community Health
School of Public Health
University of Minnesota
MedicalResearch.com: What is the background for this study?
Response: Emerging evidence suggests that patients with OSA may be more susceptible to developing pneumonia. Mechanistically, OSA causes upper airway sensory dysfunction and excessive microaspirations, which can result in significant increases in bacterial organisms in the airway leading to upper airway and laryngeal inflammation. Systemically, healthy sleep is believed to play an important role in the body’s inflammation control and immune system regulation. Despite this evidence, few studies have prospectively evaluated whether individuals with OSA are at elevated risk of being hospitalized with pneumonia, respiratory infection, or any infection
Dr. Lutsey[/caption]
Pamela L. Lutsey, PhD, MPH
Minneapolis, Minnesota
Professor, Division of Epidemiology and Community Health
School of Public Health
University of Minnesota
MedicalResearch.com: What is the background for this study?
Response: Emerging evidence suggests that patients with OSA may be more susceptible to developing pneumonia. Mechanistically, OSA causes upper airway sensory dysfunction and excessive microaspirations, which can result in significant increases in bacterial organisms in the airway leading to upper airway and laryngeal inflammation. Systemically, healthy sleep is believed to play an important role in the body’s inflammation control and immune system regulation. Despite this evidence, few studies have prospectively evaluated whether individuals with OSA are at elevated risk of being hospitalized with pneumonia, respiratory infection, or any infection
 Dr. Lutsey[/caption]
Pamela L. Lutsey, PhD, MPH
Minneapolis, Minnesota
Professor, Division of Epidemiology and Community Health
School of Public Health
University of Minnesota
MedicalResearch.com: What is the background for this study?
Response: Emerging evidence suggests that patients with OSA may be more susceptible to developing pneumonia. Mechanistically, OSA causes upper airway sensory dysfunction and excessive microaspirations, which can result in significant increases in bacterial organisms in the airway leading to upper airway and laryngeal inflammation. Systemically, healthy sleep is believed to play an important role in the body’s inflammation control and immune system regulation. Despite this evidence, few studies have prospectively evaluated whether individuals with OSA are at elevated risk of being hospitalized with pneumonia, respiratory infection, or any infection
Dr. Lutsey[/caption]
Pamela L. Lutsey, PhD, MPH
Minneapolis, Minnesota
Professor, Division of Epidemiology and Community Health
School of Public Health
University of Minnesota
MedicalResearch.com: What is the background for this study?
Response: Emerging evidence suggests that patients with OSA may be more susceptible to developing pneumonia. Mechanistically, OSA causes upper airway sensory dysfunction and excessive microaspirations, which can result in significant increases in bacterial organisms in the airway leading to upper airway and laryngeal inflammation. Systemically, healthy sleep is believed to play an important role in the body’s inflammation control and immune system regulation. Despite this evidence, few studies have prospectively evaluated whether individuals with OSA are at elevated risk of being hospitalized with pneumonia, respiratory infection, or any infection
Author Interviews / 12.12.2022
5 Ways to Get the Most out of ELISAs
Are you just starting with ELISAs and want to know what to buy? ELISA is a well-known scientific test method used in the lab to detect protein-antibody interactions. It is not only helpful in conducting medical research applications, but it also has excellent industrial uses like tracking down pathogens in food, environmental diagnostics, etc. Use this quick guide to learn exactly how to get the most from your coating buffer.
Know Your Antigen
ELISA (Enzyme-Linked Immunosorbent Assay) is the gold standard in testing for allergic reactions. They don't just get the job done; they get it right every time! In ELISAs and many other infectious diseases, a single cell or virus may be able to infect another in the same manner and replicate. This is called the passive spread. There are a lot of inactive contacts between people in this community, so your immune system can easily recognize your specific antigen. Since everyone is exposed to this disease at some point in their lives, you should know your particular antigen well enough so that you'll be able to fight it more effectively if it ever re-appears again.
Author Interviews, Breast Cancer, Mammograms / 07.12.2022
Contrast-enhanced mammography significantly improved detection of early breast cancer in women with Personal History of Breast Cancer
MedicalResearch.com Interview with:
[caption id="attachment_59804" align="alignleft" width="150"] Dr. Berg[/caption]
Wendie Berg, MD, PhD, FACR
Professor of Radiology
University of Pittsburgh
MedicalResearch.com: What is the background for this study?
Response: Mammography misses many cancers in women with a personal history of breast cancer (PHBC). MRI improves early detection of cancer in women with PHBC and the American College of Radiology recommends adding MRI every year for women with PHBC and dense breasts or diagnosis by age 50 but not every woman can tolerate MRI.
Contrast-enhanced mammography (CEM) appears to be a good alternative to MRI. Our study examined performance of CEM after tomosynthesis in women with PHBC. We first trained our radiologists in CEM (Berg WA et al JBI 2021) and two radiologists interpreted both tomosynthesis and CEM on every participant.
Dr. Berg[/caption]
Wendie Berg, MD, PhD, FACR
Professor of Radiology
University of Pittsburgh
MedicalResearch.com: What is the background for this study?
Response: Mammography misses many cancers in women with a personal history of breast cancer (PHBC). MRI improves early detection of cancer in women with PHBC and the American College of Radiology recommends adding MRI every year for women with PHBC and dense breasts or diagnosis by age 50 but not every woman can tolerate MRI.
Contrast-enhanced mammography (CEM) appears to be a good alternative to MRI. Our study examined performance of CEM after tomosynthesis in women with PHBC. We first trained our radiologists in CEM (Berg WA et al JBI 2021) and two radiologists interpreted both tomosynthesis and CEM on every participant.
 Dr. Berg[/caption]
Wendie Berg, MD, PhD, FACR
Professor of Radiology
University of Pittsburgh
MedicalResearch.com: What is the background for this study?
Response: Mammography misses many cancers in women with a personal history of breast cancer (PHBC). MRI improves early detection of cancer in women with PHBC and the American College of Radiology recommends adding MRI every year for women with PHBC and dense breasts or diagnosis by age 50 but not every woman can tolerate MRI.
Contrast-enhanced mammography (CEM) appears to be a good alternative to MRI. Our study examined performance of CEM after tomosynthesis in women with PHBC. We first trained our radiologists in CEM (Berg WA et al JBI 2021) and two radiologists interpreted both tomosynthesis and CEM on every participant.
Dr. Berg[/caption]
Wendie Berg, MD, PhD, FACR
Professor of Radiology
University of Pittsburgh
MedicalResearch.com: What is the background for this study?
Response: Mammography misses many cancers in women with a personal history of breast cancer (PHBC). MRI improves early detection of cancer in women with PHBC and the American College of Radiology recommends adding MRI every year for women with PHBC and dense breasts or diagnosis by age 50 but not every woman can tolerate MRI.
Contrast-enhanced mammography (CEM) appears to be a good alternative to MRI. Our study examined performance of CEM after tomosynthesis in women with PHBC. We first trained our radiologists in CEM (Berg WA et al JBI 2021) and two radiologists interpreted both tomosynthesis and CEM on every participant.
Author Interviews, Cancer Research, Duke, Heart Disease, Pediatrics / 06.12.2022
Multiple Demographic Disparities in Cardiovascular Risk After Pediatric and Youth Cancer
MedicalResearch.com Interview with:
[caption id="attachment_59798" align="alignleft" width="150"] Dr. Berkman[/caption]
Amy Berkman, MD
Department of Pediatrics
Duke University School of Medicine
MedicalResearch.com: What is the background for this study?
Response: Cancer incidence in adolescents and young adults (AYAs, aged 15-39 years at diagnosis) is increasing, with approximately 90,000 new diagnoses annually in the US. Improvements in 5-year survival have led to a growing population of survivors of AYA cancer, currently estimated at >600,000 survivors. Survivors are at increased risk of treatment related chronic conditions including cardiovascular disease (CVD).
We wanted to determine whether certain sociodemographic and medical history factors further increase the risk of CVD in AYA cancer survivors and also compare risk of CVD between AYA cancer survivors and the general population.
Dr. Berkman[/caption]
Amy Berkman, MD
Department of Pediatrics
Duke University School of Medicine
MedicalResearch.com: What is the background for this study?
Response: Cancer incidence in adolescents and young adults (AYAs, aged 15-39 years at diagnosis) is increasing, with approximately 90,000 new diagnoses annually in the US. Improvements in 5-year survival have led to a growing population of survivors of AYA cancer, currently estimated at >600,000 survivors. Survivors are at increased risk of treatment related chronic conditions including cardiovascular disease (CVD).
We wanted to determine whether certain sociodemographic and medical history factors further increase the risk of CVD in AYA cancer survivors and also compare risk of CVD between AYA cancer survivors and the general population.
 Dr. Berkman[/caption]
Amy Berkman, MD
Department of Pediatrics
Duke University School of Medicine
MedicalResearch.com: What is the background for this study?
Response: Cancer incidence in adolescents and young adults (AYAs, aged 15-39 years at diagnosis) is increasing, with approximately 90,000 new diagnoses annually in the US. Improvements in 5-year survival have led to a growing population of survivors of AYA cancer, currently estimated at >600,000 survivors. Survivors are at increased risk of treatment related chronic conditions including cardiovascular disease (CVD).
We wanted to determine whether certain sociodemographic and medical history factors further increase the risk of CVD in AYA cancer survivors and also compare risk of CVD between AYA cancer survivors and the general population.
Dr. Berkman[/caption]
Amy Berkman, MD
Department of Pediatrics
Duke University School of Medicine
MedicalResearch.com: What is the background for this study?
Response: Cancer incidence in adolescents and young adults (AYAs, aged 15-39 years at diagnosis) is increasing, with approximately 90,000 new diagnoses annually in the US. Improvements in 5-year survival have led to a growing population of survivors of AYA cancer, currently estimated at >600,000 survivors. Survivors are at increased risk of treatment related chronic conditions including cardiovascular disease (CVD).
We wanted to determine whether certain sociodemographic and medical history factors further increase the risk of CVD in AYA cancer survivors and also compare risk of CVD between AYA cancer survivors and the general population.
Author Interviews, Heart Disease, JACC, Supplements / 06.12.2022
Personalized Micronutrients May Benefit Cardiovascular Health
MedicalResearch.com Interview with:
[caption id="attachment_59776" align="alignleft" width="200"] Dr. Simin Liu[/caption]
Simin Liu MD MPH ScD
Professor of Epidemiology at the School of Public Health,
Professor of Medicine (Endocrinology) and
Professor of Surgery at the Alpert School of Medicine
Brown University
MedicalResearch.com: What is the background for this study?
Response: Our research team has been researching the roles of environmental and genetic determinants of chronic diseases for nearly three decades, with special emphasis on evaluating micronutrients, minerals, and trace elements in relation to cardiometabolic outcomes, and findings of which have contributed to the design of several large, randomized trials of dietary supplements in the US (Liu JAMA 1999; 2011; Diabetes Care 2005a,b; Diabetes 2006). Several large intervention trials have consistently shown beneficial effects on clinical cardiometabolic outcomes of a diet pattern rich in micronutrients, although research on micronutrient supplementation has mainly focused on the health effects of a single or a few vitamins and minerals.
We decided to take a comprehensive and systematic approach to evaluate all the publicly available/accessible studies reporting all micronutrients including phytochemicals and antioxidant supplements and their effects on cardiovascular risk factors as well as multiple CVDs.
Dr. Simin Liu[/caption]
Simin Liu MD MPH ScD
Professor of Epidemiology at the School of Public Health,
Professor of Medicine (Endocrinology) and
Professor of Surgery at the Alpert School of Medicine
Brown University
MedicalResearch.com: What is the background for this study?
Response: Our research team has been researching the roles of environmental and genetic determinants of chronic diseases for nearly three decades, with special emphasis on evaluating micronutrients, minerals, and trace elements in relation to cardiometabolic outcomes, and findings of which have contributed to the design of several large, randomized trials of dietary supplements in the US (Liu JAMA 1999; 2011; Diabetes Care 2005a,b; Diabetes 2006). Several large intervention trials have consistently shown beneficial effects on clinical cardiometabolic outcomes of a diet pattern rich in micronutrients, although research on micronutrient supplementation has mainly focused on the health effects of a single or a few vitamins and minerals.
We decided to take a comprehensive and systematic approach to evaluate all the publicly available/accessible studies reporting all micronutrients including phytochemicals and antioxidant supplements and their effects on cardiovascular risk factors as well as multiple CVDs.
 Dr. Simin Liu[/caption]
Simin Liu MD MPH ScD
Professor of Epidemiology at the School of Public Health,
Professor of Medicine (Endocrinology) and
Professor of Surgery at the Alpert School of Medicine
Brown University
MedicalResearch.com: What is the background for this study?
Response: Our research team has been researching the roles of environmental and genetic determinants of chronic diseases for nearly three decades, with special emphasis on evaluating micronutrients, minerals, and trace elements in relation to cardiometabolic outcomes, and findings of which have contributed to the design of several large, randomized trials of dietary supplements in the US (Liu JAMA 1999; 2011; Diabetes Care 2005a,b; Diabetes 2006). Several large intervention trials have consistently shown beneficial effects on clinical cardiometabolic outcomes of a diet pattern rich in micronutrients, although research on micronutrient supplementation has mainly focused on the health effects of a single or a few vitamins and minerals.
We decided to take a comprehensive and systematic approach to evaluate all the publicly available/accessible studies reporting all micronutrients including phytochemicals and antioxidant supplements and their effects on cardiovascular risk factors as well as multiple CVDs.
Dr. Simin Liu[/caption]
Simin Liu MD MPH ScD
Professor of Epidemiology at the School of Public Health,
Professor of Medicine (Endocrinology) and
Professor of Surgery at the Alpert School of Medicine
Brown University
MedicalResearch.com: What is the background for this study?
Response: Our research team has been researching the roles of environmental and genetic determinants of chronic diseases for nearly three decades, with special emphasis on evaluating micronutrients, minerals, and trace elements in relation to cardiometabolic outcomes, and findings of which have contributed to the design of several large, randomized trials of dietary supplements in the US (Liu JAMA 1999; 2011; Diabetes Care 2005a,b; Diabetes 2006). Several large intervention trials have consistently shown beneficial effects on clinical cardiometabolic outcomes of a diet pattern rich in micronutrients, although research on micronutrient supplementation has mainly focused on the health effects of a single or a few vitamins and minerals.
We decided to take a comprehensive and systematic approach to evaluate all the publicly available/accessible studies reporting all micronutrients including phytochemicals and antioxidant supplements and their effects on cardiovascular risk factors as well as multiple CVDs.
Addiction / 02.12.2022
What is Medication Assisted Treatment?
Medication Assisted Treatment can be used to treat a variety of substance use disorders including alcohol use disorder, heroin use...
Addiction, Author Interviews, Pain Research / 01.12.2022
From most prescribed opioid in the US to (almost) discontinued: The demise of Demerol
MedicalResearch.com Interview with:
[caption id="attachment_59795" align="alignleft" width="172"] Lavinia Harrison[/caption]
Lavinia Harrison
Geisinger Commonwealth School of Medicine
Scranton, PA 18509
MedicalResearch.com: What is the background for this study?
Response: The opioid meperidine (Demerol) was widely prescribed in the United States (US) as an analgesic to treat moderate to severe pain. Meperidine was the most used opioid in the US in 1987 and was considered safer than other opioids during acute pancreatitis. Over the past two decades, meperidine has shifted from being frequently prescribed to being used only when patients are experiencing atypical reactions to opioids (e.g., morphine and hydromorphone); to removal from the World Health Organization's essential medication list and receiving strong warnings against its use from many professional organizations including the American Geriatrics Society. The unfortunate Libby Zion (1965-1984) case increased concerns about serotonin syndrome with meperidine.
According to a prior pharmacoepidemiology report, the distribution of meperidine in the United States decreased by 95% between 2001 and 2019 [1]. The aim of the study was to include updated information (2020 and 2021) as well as examine the changes among Medicaid patients [2].
Lavinia Harrison[/caption]
Lavinia Harrison
Geisinger Commonwealth School of Medicine
Scranton, PA 18509
MedicalResearch.com: What is the background for this study?
Response: The opioid meperidine (Demerol) was widely prescribed in the United States (US) as an analgesic to treat moderate to severe pain. Meperidine was the most used opioid in the US in 1987 and was considered safer than other opioids during acute pancreatitis. Over the past two decades, meperidine has shifted from being frequently prescribed to being used only when patients are experiencing atypical reactions to opioids (e.g., morphine and hydromorphone); to removal from the World Health Organization's essential medication list and receiving strong warnings against its use from many professional organizations including the American Geriatrics Society. The unfortunate Libby Zion (1965-1984) case increased concerns about serotonin syndrome with meperidine.
According to a prior pharmacoepidemiology report, the distribution of meperidine in the United States decreased by 95% between 2001 and 2019 [1]. The aim of the study was to include updated information (2020 and 2021) as well as examine the changes among Medicaid patients [2].
 Lavinia Harrison[/caption]
Lavinia Harrison
Geisinger Commonwealth School of Medicine
Scranton, PA 18509
MedicalResearch.com: What is the background for this study?
Response: The opioid meperidine (Demerol) was widely prescribed in the United States (US) as an analgesic to treat moderate to severe pain. Meperidine was the most used opioid in the US in 1987 and was considered safer than other opioids during acute pancreatitis. Over the past two decades, meperidine has shifted from being frequently prescribed to being used only when patients are experiencing atypical reactions to opioids (e.g., morphine and hydromorphone); to removal from the World Health Organization's essential medication list and receiving strong warnings against its use from many professional organizations including the American Geriatrics Society. The unfortunate Libby Zion (1965-1984) case increased concerns about serotonin syndrome with meperidine.
According to a prior pharmacoepidemiology report, the distribution of meperidine in the United States decreased by 95% between 2001 and 2019 [1]. The aim of the study was to include updated information (2020 and 2021) as well as examine the changes among Medicaid patients [2].
Lavinia Harrison[/caption]
Lavinia Harrison
Geisinger Commonwealth School of Medicine
Scranton, PA 18509
MedicalResearch.com: What is the background for this study?
Response: The opioid meperidine (Demerol) was widely prescribed in the United States (US) as an analgesic to treat moderate to severe pain. Meperidine was the most used opioid in the US in 1987 and was considered safer than other opioids during acute pancreatitis. Over the past two decades, meperidine has shifted from being frequently prescribed to being used only when patients are experiencing atypical reactions to opioids (e.g., morphine and hydromorphone); to removal from the World Health Organization's essential medication list and receiving strong warnings against its use from many professional organizations including the American Geriatrics Society. The unfortunate Libby Zion (1965-1984) case increased concerns about serotonin syndrome with meperidine.
According to a prior pharmacoepidemiology report, the distribution of meperidine in the United States decreased by 95% between 2001 and 2019 [1]. The aim of the study was to include updated information (2020 and 2021) as well as examine the changes among Medicaid patients [2].
Author Interviews, Cost of Health Care, Rheumatology, University of Pittsburgh / 01.12.2022
SLE – Lupus: Size of Copay Influences Medication Adherence
MedicalResearch.com Interview with:
Raisa Silva, M.D.
Resident physician in Internal medicine
University of Pittsburgh Medical Center
MedicalResearch.com: What is the background for this study?
Response: Systemic lupus erythematosus (lupus for short) is a complex disease that significantly affects patients’ lives. Adherence to medications for lupus is known to be suboptimal (it can be as low as 15% in some studies). Multiple social factors may affect treatment adherence. For example, costs of medications (including copayments, deductibles, co-sharing), polypharmacy (patients with lupus often have comorbid diseases that also need medications), and potential side effects are some of the reasons why patients may have difficulty in taking medications for lupus every day. The costs of insurance copayment may represent a major obstacle to adherence. The lack of adherence to lupus medications is associated with poor control of disease, more symptoms, and worse disease outcomes, such as more hospitalizations and more severe disease.
In our study, we examined the association between lupus medications copayment and adherence to these medications (some of the most commonly used medications for lupus).
If you have a loved one who needs medical care for a health condition, you might struggle to find the time to provide this care yourself or find adequate carers to visit your loved one at home. Therefore, thinking about care homes can be a useful step. If you or your loved one is unsure about the idea, here are some of the medical benefits that living in a care home can offer.
Professional Carers
You may have been providing at-home care for your loved one for a while now, but in a care home, there are professionally trained carers who have all the necessary skills and techniques to assist every resident. This gives both the resident and the resident's family peace of mind that they are receiving high-quality care.
Nursing Staff
Having nursing staff always available makes a care home a far safer environment for someone with a medical condition that needs regular monitoring and assistance. Many care homes employ skilled nurses to give treatments and medications according to residents' needs. The level of planning and consideration that goes into this is usually far superior to any other setting.
If you find yourself in an emergency situation, then it is important that you have a fully functioning first aid kit to hand. This should be a small kit filled with different supplies that will be helpful for various injuries and ailments.
The Importance of Contents
It is incredibly important that the contents of your first aid kit are of high quality and include everything you need – because without them, you will not be able to use the equipment to its fullest extent in an emergency, and you may lack crucial pieces.
You can buy complete first aid kits online that are already full of everything you need; however, you will have to keep a list of these supplies so that you can replenish your gear as and when you need to. As such, below, this article will discuss the most crucial components that should make up your first aid kit in more detail.
Accidents & Violence, Author Interviews, Brigham & Women's - Harvard, Emory, JAMA, Race/Ethnic Diversity / 29.11.2022
Spike in Firearm Fatalities Differ Among Ethnic and Age Groups
MedicalResearch.com Interview with:
Chris A. Rees, MD, MPH
Assistant Professor of Pediatrics and Emergency Medicine
Research Director, Pediatric Emergency Medicine Fellowship
Emory University School of Medicine
Attending Physician, Children's Healthcare of Atlanta
Pediatric Research Scientist, CHAMPS, U.S. Program Office and
Eric W. Fleegler, MD, MPH, FAAP
Associate in Pediatrics, Division of Emergency Medicine
Director Sedation Service
Boston Children’s Hospital
Assistant Professor of Pediatrics and Emergency Medicine
Harvard Medical School
MedicalResearch.com: What is the background for this study?
Response: Rates of firearm fatalities in the United States have reached a 28-year high. Yet, an understanding of the specific demographic groups who have been most affected, and where in the United States these fatalities have occurred, has not been clearly described in the past.
Sound healing is an alternative therapy that uses sound waves to heal the mind and body. This therapy is based on the belief that all matter is vibrating at a certain frequency and that disease or ill health occurs when the body’s natural frequency is out of alignment. Sound healing practitioners use a variety of tools, including singing bowls, gongs, and tuning forks, to restore the body’s natural frequency.
There are many benefits of sound healing, including reducing stress, promoting relaxation, improving sleep, and reducing pain. Sound healing can also be used to treat a wide range of conditions, such as anxiety, depression, PTSD, and addiction. If you are looking for a non-invasive way to improve your health and well-being, sound healing may be right for you.
Alzheimer's - Dementia, Author Interviews, Nutrition / 26.11.2022
Study Finds Cognitive Decline Lowest in Those with Lots of Flavenols in Diet
MedicalResearch.com Interview with:
[caption id="attachment_59755" align="alignleft" width="150"] Dr. Holland[/caption]
Thomas M Holland, MD, MS
Assistant Professor
Rush Institute for Health Aging
Rush College of Medicine & Rush College of Health Sciences
https://www.rushu.rush.edu/faculty/thomas-m-holland-md-ms
MedicalResearch.com: What is the background for this study?
Response: My late mentor Martha Clare Morris, ScD had published a manuscript investigating leafy green intake, and the nutrients found therein, and cognition. I wanted to take this thought a step further and investigate the potential association bioactives, found in vegetables, like leafy greens, has to cognition. Further, this is a continuation of the research I published in the green journal in 2020 associating flavonols to incident Alzheimer’s dementia. This study extends the understanding that flavonols are not only beneficial for the most detrimental outcome of Alzheimer’s dementia (in decreasing the risk), but also advantageous in mitigating components of the, clinical syndrome i.e. decreasing the rate of cognitive decline.
Dr. Holland[/caption]
Thomas M Holland, MD, MS
Assistant Professor
Rush Institute for Health Aging
Rush College of Medicine & Rush College of Health Sciences
https://www.rushu.rush.edu/faculty/thomas-m-holland-md-ms
MedicalResearch.com: What is the background for this study?
Response: My late mentor Martha Clare Morris, ScD had published a manuscript investigating leafy green intake, and the nutrients found therein, and cognition. I wanted to take this thought a step further and investigate the potential association bioactives, found in vegetables, like leafy greens, has to cognition. Further, this is a continuation of the research I published in the green journal in 2020 associating flavonols to incident Alzheimer’s dementia. This study extends the understanding that flavonols are not only beneficial for the most detrimental outcome of Alzheimer’s dementia (in decreasing the risk), but also advantageous in mitigating components of the, clinical syndrome i.e. decreasing the rate of cognitive decline.
 Dr. Holland[/caption]
Thomas M Holland, MD, MS
Assistant Professor
Rush Institute for Health Aging
Rush College of Medicine & Rush College of Health Sciences
https://www.rushu.rush.edu/faculty/thomas-m-holland-md-ms
MedicalResearch.com: What is the background for this study?
Response: My late mentor Martha Clare Morris, ScD had published a manuscript investigating leafy green intake, and the nutrients found therein, and cognition. I wanted to take this thought a step further and investigate the potential association bioactives, found in vegetables, like leafy greens, has to cognition. Further, this is a continuation of the research I published in the green journal in 2020 associating flavonols to incident Alzheimer’s dementia. This study extends the understanding that flavonols are not only beneficial for the most detrimental outcome of Alzheimer’s dementia (in decreasing the risk), but also advantageous in mitigating components of the, clinical syndrome i.e. decreasing the rate of cognitive decline.
Dr. Holland[/caption]
Thomas M Holland, MD, MS
Assistant Professor
Rush Institute for Health Aging
Rush College of Medicine & Rush College of Health Sciences
https://www.rushu.rush.edu/faculty/thomas-m-holland-md-ms
MedicalResearch.com: What is the background for this study?
Response: My late mentor Martha Clare Morris, ScD had published a manuscript investigating leafy green intake, and the nutrients found therein, and cognition. I wanted to take this thought a step further and investigate the potential association bioactives, found in vegetables, like leafy greens, has to cognition. Further, this is a continuation of the research I published in the green journal in 2020 associating flavonols to incident Alzheimer’s dementia. This study extends the understanding that flavonols are not only beneficial for the most detrimental outcome of Alzheimer’s dementia (in decreasing the risk), but also advantageous in mitigating components of the, clinical syndrome i.e. decreasing the rate of cognitive decline.
Aging, Author Interviews, Brigham & Women's - Harvard, Dermatology, Heart Disease, Herpes Viruses, Stroke / 23.11.2022
Herpes Zoster: Persistent Increased Risk of Cardiac Event or Stroke After Shingles
MedicalResearch.com Interview with:|
[caption id="attachment_59757" align="alignleft" width="133"] Dr. Curhan[/caption]
Sharon G. Curhan, MD, ScM|
Director, CHEARS: The Conservation of Hearing Study
Channing Division of Network Medicine
Department of Medicine
Brigham and Women’s Hospital
Harvard Medical School
Boston, MA 02114
MedicalResearch.com: What is the background for this study?
Response: Herpes zoster, commonly known as “shingles,” is a viral infection that often causes a painful rash. Shingles can occur anywhere on the head or body. Shingles is caused by the varicella zoster virus (VZV), the same virus that causes chickenpox. After a person has chickenpox, the virus stays in their body for the rest of their life. Years and even decades later, the virus may reactivate as shingles. Almost all individuals age 50 years and older in the US have been infected with the varicella zoster virus and therefore they are at risk for shingles.
About 1 in 3 people will develop shingles during their lifetime, and since age is a risk factor for shingles, this number may increase as the population ages. The risk is also higher among individuals of any age who are immunocompromised due to disease or treatment. A number of serious complications can occur when a person develops shingles, such as post-herpetic neuralgia (long-lasting pain), but there was limited information on whether there are other adverse long-term health implications of developing shingles.
There is a growing body of evidence that links VZV, the virus that causes shingles, to vascular disease. VZV vasculopathy may cause damage to blood vessels and increase the risk of stroke or coronary heart disease. Although some previous studies showed a higher risk of stroke or heart attack around the time of the shingles infection, it was not known whether this higher risk persisted in the long term. Therefore, the question we aimed to address in this study was to investigate whether shingles is associated with higher long-term risk of stroke or coronary heart disease.
To address this question, we conducted a prospective longitudinal study in 3 large US cohorts of >200,000 women and men, the Nurses’ Health Study (>79,000 women), the Nurses’ Health Study II (almost 94,000 women) and the Health Professionals Follow-Up Study (>31,000 men), without a prior history of stroke or coronary heart disease. We collected information on shingles, stroke and coronary heart disease on biennial questionnaires and confirmed the diagnoses with medical record review. We followed the participants for up to 16 years and evaluated whether those who had developed shingles were at higher risk for stroke or coronary heart disease years after the shingles episode. The outcomes we measured were incident stroke, incident coronary heart disease [defined as having a non-fatal or fatal myocardial infarction (heart attack) or a coronary revascularization procedure (CABG, coronary artery bypass graft or percutaneous transluminal coronary angioplasty)]. We also evaluated a combined outcome of cardiovascular disease, which included either stroke or coronary heart disease, whichever came first.
Dr. Curhan[/caption]
Sharon G. Curhan, MD, ScM|
Director, CHEARS: The Conservation of Hearing Study
Channing Division of Network Medicine
Department of Medicine
Brigham and Women’s Hospital
Harvard Medical School
Boston, MA 02114
MedicalResearch.com: What is the background for this study?
Response: Herpes zoster, commonly known as “shingles,” is a viral infection that often causes a painful rash. Shingles can occur anywhere on the head or body. Shingles is caused by the varicella zoster virus (VZV), the same virus that causes chickenpox. After a person has chickenpox, the virus stays in their body for the rest of their life. Years and even decades later, the virus may reactivate as shingles. Almost all individuals age 50 years and older in the US have been infected with the varicella zoster virus and therefore they are at risk for shingles.
About 1 in 3 people will develop shingles during their lifetime, and since age is a risk factor for shingles, this number may increase as the population ages. The risk is also higher among individuals of any age who are immunocompromised due to disease or treatment. A number of serious complications can occur when a person develops shingles, such as post-herpetic neuralgia (long-lasting pain), but there was limited information on whether there are other adverse long-term health implications of developing shingles.
There is a growing body of evidence that links VZV, the virus that causes shingles, to vascular disease. VZV vasculopathy may cause damage to blood vessels and increase the risk of stroke or coronary heart disease. Although some previous studies showed a higher risk of stroke or heart attack around the time of the shingles infection, it was not known whether this higher risk persisted in the long term. Therefore, the question we aimed to address in this study was to investigate whether shingles is associated with higher long-term risk of stroke or coronary heart disease.
To address this question, we conducted a prospective longitudinal study in 3 large US cohorts of >200,000 women and men, the Nurses’ Health Study (>79,000 women), the Nurses’ Health Study II (almost 94,000 women) and the Health Professionals Follow-Up Study (>31,000 men), without a prior history of stroke or coronary heart disease. We collected information on shingles, stroke and coronary heart disease on biennial questionnaires and confirmed the diagnoses with medical record review. We followed the participants for up to 16 years and evaluated whether those who had developed shingles were at higher risk for stroke or coronary heart disease years after the shingles episode. The outcomes we measured were incident stroke, incident coronary heart disease [defined as having a non-fatal or fatal myocardial infarction (heart attack) or a coronary revascularization procedure (CABG, coronary artery bypass graft or percutaneous transluminal coronary angioplasty)]. We also evaluated a combined outcome of cardiovascular disease, which included either stroke or coronary heart disease, whichever came first.
 Dr. Curhan[/caption]
Sharon G. Curhan, MD, ScM|
Director, CHEARS: The Conservation of Hearing Study
Channing Division of Network Medicine
Department of Medicine
Brigham and Women’s Hospital
Harvard Medical School
Boston, MA 02114
MedicalResearch.com: What is the background for this study?
Response: Herpes zoster, commonly known as “shingles,” is a viral infection that often causes a painful rash. Shingles can occur anywhere on the head or body. Shingles is caused by the varicella zoster virus (VZV), the same virus that causes chickenpox. After a person has chickenpox, the virus stays in their body for the rest of their life. Years and even decades later, the virus may reactivate as shingles. Almost all individuals age 50 years and older in the US have been infected with the varicella zoster virus and therefore they are at risk for shingles.
About 1 in 3 people will develop shingles during their lifetime, and since age is a risk factor for shingles, this number may increase as the population ages. The risk is also higher among individuals of any age who are immunocompromised due to disease or treatment. A number of serious complications can occur when a person develops shingles, such as post-herpetic neuralgia (long-lasting pain), but there was limited information on whether there are other adverse long-term health implications of developing shingles.
There is a growing body of evidence that links VZV, the virus that causes shingles, to vascular disease. VZV vasculopathy may cause damage to blood vessels and increase the risk of stroke or coronary heart disease. Although some previous studies showed a higher risk of stroke or heart attack around the time of the shingles infection, it was not known whether this higher risk persisted in the long term. Therefore, the question we aimed to address in this study was to investigate whether shingles is associated with higher long-term risk of stroke or coronary heart disease.
To address this question, we conducted a prospective longitudinal study in 3 large US cohorts of >200,000 women and men, the Nurses’ Health Study (>79,000 women), the Nurses’ Health Study II (almost 94,000 women) and the Health Professionals Follow-Up Study (>31,000 men), without a prior history of stroke or coronary heart disease. We collected information on shingles, stroke and coronary heart disease on biennial questionnaires and confirmed the diagnoses with medical record review. We followed the participants for up to 16 years and evaluated whether those who had developed shingles were at higher risk for stroke or coronary heart disease years after the shingles episode. The outcomes we measured were incident stroke, incident coronary heart disease [defined as having a non-fatal or fatal myocardial infarction (heart attack) or a coronary revascularization procedure (CABG, coronary artery bypass graft or percutaneous transluminal coronary angioplasty)]. We also evaluated a combined outcome of cardiovascular disease, which included either stroke or coronary heart disease, whichever came first.
Dr. Curhan[/caption]
Sharon G. Curhan, MD, ScM|
Director, CHEARS: The Conservation of Hearing Study
Channing Division of Network Medicine
Department of Medicine
Brigham and Women’s Hospital
Harvard Medical School
Boston, MA 02114
MedicalResearch.com: What is the background for this study?
Response: Herpes zoster, commonly known as “shingles,” is a viral infection that often causes a painful rash. Shingles can occur anywhere on the head or body. Shingles is caused by the varicella zoster virus (VZV), the same virus that causes chickenpox. After a person has chickenpox, the virus stays in their body for the rest of their life. Years and even decades later, the virus may reactivate as shingles. Almost all individuals age 50 years and older in the US have been infected with the varicella zoster virus and therefore they are at risk for shingles.
About 1 in 3 people will develop shingles during their lifetime, and since age is a risk factor for shingles, this number may increase as the population ages. The risk is also higher among individuals of any age who are immunocompromised due to disease or treatment. A number of serious complications can occur when a person develops shingles, such as post-herpetic neuralgia (long-lasting pain), but there was limited information on whether there are other adverse long-term health implications of developing shingles.
There is a growing body of evidence that links VZV, the virus that causes shingles, to vascular disease. VZV vasculopathy may cause damage to blood vessels and increase the risk of stroke or coronary heart disease. Although some previous studies showed a higher risk of stroke or heart attack around the time of the shingles infection, it was not known whether this higher risk persisted in the long term. Therefore, the question we aimed to address in this study was to investigate whether shingles is associated with higher long-term risk of stroke or coronary heart disease.
To address this question, we conducted a prospective longitudinal study in 3 large US cohorts of >200,000 women and men, the Nurses’ Health Study (>79,000 women), the Nurses’ Health Study II (almost 94,000 women) and the Health Professionals Follow-Up Study (>31,000 men), without a prior history of stroke or coronary heart disease. We collected information on shingles, stroke and coronary heart disease on biennial questionnaires and confirmed the diagnoses with medical record review. We followed the participants for up to 16 years and evaluated whether those who had developed shingles were at higher risk for stroke or coronary heart disease years after the shingles episode. The outcomes we measured were incident stroke, incident coronary heart disease [defined as having a non-fatal or fatal myocardial infarction (heart attack) or a coronary revascularization procedure (CABG, coronary artery bypass graft or percutaneous transluminal coronary angioplasty)]. We also evaluated a combined outcome of cardiovascular disease, which included either stroke or coronary heart disease, whichever came first.
Author Interviews, JAMA, Obstructive Sleep Apnea, Sleep Disorders, USPSTF / 23.11.2022
USPSTF: More Evidence Needed Before Routine Screening of Adults Can Be Recommended
MedicalResearch.com Interview with:
[caption id="attachment_58144" align="alignleft" width="150"] Dr. Kubik[/caption]
Martha Kubik, Ph.D., R.N.
Professor, School of Nursing
College of Health and Human Services
George Mason University
Member, U.S. Preventive Services Task Force
MedicalResearch.com: What is the background for this study?
Response: Obstructive sleep apnea is a health condition in which part or all of a person’s airway gets blocked during sleep, causing their breathing to stop and restart many times. Untreated sleep apnea is associated with heart disease, stroke, and diabetes. However, there is currently very limited evidence on screening people who don’t have signs or symptoms like snoring and excessive daytime sleepiness.
Dr. Kubik[/caption]
Martha Kubik, Ph.D., R.N.
Professor, School of Nursing
College of Health and Human Services
George Mason University
Member, U.S. Preventive Services Task Force
MedicalResearch.com: What is the background for this study?
Response: Obstructive sleep apnea is a health condition in which part or all of a person’s airway gets blocked during sleep, causing their breathing to stop and restart many times. Untreated sleep apnea is associated with heart disease, stroke, and diabetes. However, there is currently very limited evidence on screening people who don’t have signs or symptoms like snoring and excessive daytime sleepiness.
 Dr. Kubik[/caption]
Martha Kubik, Ph.D., R.N.
Professor, School of Nursing
College of Health and Human Services
George Mason University
Member, U.S. Preventive Services Task Force
MedicalResearch.com: What is the background for this study?
Response: Obstructive sleep apnea is a health condition in which part or all of a person’s airway gets blocked during sleep, causing their breathing to stop and restart many times. Untreated sleep apnea is associated with heart disease, stroke, and diabetes. However, there is currently very limited evidence on screening people who don’t have signs or symptoms like snoring and excessive daytime sleepiness.
Dr. Kubik[/caption]
Martha Kubik, Ph.D., R.N.
Professor, School of Nursing
College of Health and Human Services
George Mason University
Member, U.S. Preventive Services Task Force
MedicalResearch.com: What is the background for this study?
Response: Obstructive sleep apnea is a health condition in which part or all of a person’s airway gets blocked during sleep, causing their breathing to stop and restart many times. Untreated sleep apnea is associated with heart disease, stroke, and diabetes. However, there is currently very limited evidence on screening people who don’t have signs or symptoms like snoring and excessive daytime sleepiness.
Author Interviews, Dermatology / 22.11.2022
Makeup Applied to Facial Features Improves Perceived Skin Evenness
MedicalResearch.com Interview with:
[caption id="attachment_59707" align="alignleft" width="80"] Dr. Batres[/caption]
Carlota Batres, Ph.D.
Dr. Batres[/caption]
Carlota Batres, Ph.D.
Assistant Professor, Department of Psychology
Director, Preferences Lab PreferencesLab.com
Franklin and Marshall College MedicalResearch.com: What is the background for this study? Response: Previous research has found that complexion-oriented makeup products, such as foundation and concealer, make the skin appear more even. Interestingly, though, the effect size of perceptual judgements has been found to be larger than the effect size of physical measurements, suggesting that there are factors affecting the perception of skin evenness that are not captured by the physical measurements of isolated skin patches.
 Dr. Batres[/caption]
Carlota Batres, Ph.D.
Dr. Batres[/caption]
Carlota Batres, Ph.D.Assistant Professor, Department of Psychology
Director, Preferences Lab PreferencesLab.com
Franklin and Marshall College MedicalResearch.com: What is the background for this study? Response: Previous research has found that complexion-oriented makeup products, such as foundation and concealer, make the skin appear more even. Interestingly, though, the effect size of perceptual judgements has been found to be larger than the effect size of physical measurements, suggesting that there are factors affecting the perception of skin evenness that are not captured by the physical measurements of isolated skin patches.