MedicalResearch.com Interview with:
[caption id="attachment_39686" align="alignleft" width="247"]
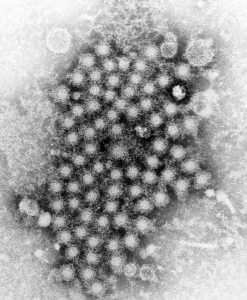
In the United States, hepatitis A, hepatitis B and hepatitis C are the most common types, but also included are hepatitis D and E.
CDC/ E.H. Cook, Jr.[/caption]
Stefan Zeuzem, M.D.
Professor of Medicine
Chief Internal Medicine
Goethe University Hospital
Frankfurt, Germany
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Chronic hepatitis C virus (HCV) infection is a major global public health problem with more than 71 million people infected worldwide, and can result in significant morbidity and mortality, including liver cirrhosis, hepatocellular carcinoma, and death.
1
This publication describes the efficacy and safety results from two Phase 3 clinical trials, ENDURANCE-1 and ENDURANCE-3, in patients with chronic HCV genotypes (GT) 1 or 3 infection who were treated with an all-oral, once-daily combination regimen of direct-acting antiviral agents (DAA) glecaprevir (GLE) at 300 mg and pibrentasvir (PIB) at 120 mg.
The findings from ENDURANCE-1 trial show that the GLE/PIB combination regimen (G/P) given for 8 weeks to HCV GT1 chronically infected non-cirrhotic treatment-naïve or treatment-experienced (with sofosbuvir and/or interferon with ribavirin) patients was safe and well-tolerated, achieved high efficacy with a sustained virologic response at post-treatment week 12 (SVR12) rate >99% and was non-inferior to 12-week treatment with G/P.
The trial also included subjects who were co-infected with human immunodeficiency virus (HIV), and all of these subjects achieved SVR12 while maintaining HIV suppression throughout the study. ENDURANCE-3 trial results show that the G/P regimen given for 8 weeks to HCV GT3 chronically infected non-cirrhotic treatment-naïve patients was safe and well-tolerated, achieved high efficacy in this historically difficult to cure GT with an SVR12 rate >94%, and was non-inferior to 12-week treatment with G/P, which in turn was non-inferior to the treatment with 12-week DAA regimen of sofosbivir and daclatasvir.
 Dr. Saxe[/caption]
Glenn N. Saxe, MD
Professor of Child & Adolescent Psychiatry
Hassenfeld Children’s Hospital at NYU Langone
Department of Child and Adolescent Psychiatry
Child Study Center, One Park Avenue
New York, NY 10016
MedicalResearch.com: What is the background for this study? Would you briefly explain what is meant by brain entropy and how it relates to intelligence?
Response: Think of human intelligence as the capacity for a human being to understand their complex and ever-changing world. The world of a person is really complex and constantly in flux so the human brain must be ready to understand whatever may come – when there is no way beforehand to predict what might come. How does the brain understand its world? It creates specific models of the information it receives through specific patterns of neuronal connection. These are called brain states. The way the brain understands its world is largely through using such models, or brain states, to accurately predict what comes next. So you can see that for an intelligent brain to properly understand and predict events in the world, it will need to have access to a very, very large number of brain states. And this is how entropy is defined.
Entropy is a very old and very powerful concept in the history of science. Not only is it fundamental for thermodynamics – what we learned in high school physics – but it is also fundamental for the nature of information and it’s processing. Entropy is defined as the number of states – or distinct configurations – any system has access to at any point in time. High entropy means access to a very large number of states. Low entropy means access to a very small number of states. A solid is a phenomenon with very low entropy. A gas is a phenomenon with very high entropy. Life, and the brain, are somewhere in between.
Although it is impossible to precisely measure the number of states a brain has access to at any one moment, there is a highly related concept that can be measured. A system with access to a very high number of possible states (like a gas) has components with behavior that is highly unpredictable. A system with access to very few possible states (like a solid) has components whose behavior is highly predictable. We measured brain entropy through the predictability of the brains components at the smallest scale we had access to: what are called voxels in an fMRI scan. These are 3mm cubes of neurons in a functional MRI scan, and there are many thousands of these voxels in our measurement and each of these voxels contains information on the activity of hundreds of thousands of neurons. We measured the predictability of each of these voxels and then found clusters of voxels where their predictability - or entropy - was related to intelligence.
Dr. Saxe[/caption]
Glenn N. Saxe, MD
Professor of Child & Adolescent Psychiatry
Hassenfeld Children’s Hospital at NYU Langone
Department of Child and Adolescent Psychiatry
Child Study Center, One Park Avenue
New York, NY 10016
MedicalResearch.com: What is the background for this study? Would you briefly explain what is meant by brain entropy and how it relates to intelligence?
Response: Think of human intelligence as the capacity for a human being to understand their complex and ever-changing world. The world of a person is really complex and constantly in flux so the human brain must be ready to understand whatever may come – when there is no way beforehand to predict what might come. How does the brain understand its world? It creates specific models of the information it receives through specific patterns of neuronal connection. These are called brain states. The way the brain understands its world is largely through using such models, or brain states, to accurately predict what comes next. So you can see that for an intelligent brain to properly understand and predict events in the world, it will need to have access to a very, very large number of brain states. And this is how entropy is defined.
Entropy is a very old and very powerful concept in the history of science. Not only is it fundamental for thermodynamics – what we learned in high school physics – but it is also fundamental for the nature of information and it’s processing. Entropy is defined as the number of states – or distinct configurations – any system has access to at any point in time. High entropy means access to a very large number of states. Low entropy means access to a very small number of states. A solid is a phenomenon with very low entropy. A gas is a phenomenon with very high entropy. Life, and the brain, are somewhere in between.
Although it is impossible to precisely measure the number of states a brain has access to at any one moment, there is a highly related concept that can be measured. A system with access to a very high number of possible states (like a gas) has components with behavior that is highly unpredictable. A system with access to very few possible states (like a solid) has components whose behavior is highly predictable. We measured brain entropy through the predictability of the brains components at the smallest scale we had access to: what are called voxels in an fMRI scan. These are 3mm cubes of neurons in a functional MRI scan, and there are many thousands of these voxels in our measurement and each of these voxels contains information on the activity of hundreds of thousands of neurons. We measured the predictability of each of these voxels and then found clusters of voxels where their predictability - or entropy - was related to intelligence.