Author Interviews, Cost of Health Care, JAMA, Kidney Disease, Medicare / 11.01.2024
Dialysis Facilities Serving Disadvantaged Populations More Frequently Penalized Under Pay-For-Performance Model
MedicalResearch.com Interview with:
Kalli Koukounas, MPH
Ph.D. Student, Health Services Research
Brown University School of Public Health
Providence, RI
MedicalResearch.com: What is the background for this study?
Response: On Jan. 1st, 2021, the Centers for Medicare and Medicaid Services (CMS) implemented the End-Stage Renal Disease Treatment Choices (ETC) Model, one of the largest randomized tests of pay-for-performance incentives ever conducted in the US.
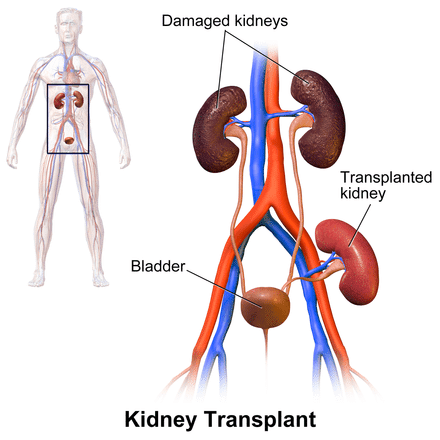
The goal of the model was to enhance the use of home dialysis and kidney transplant or waitlisting among kidney failure patients in traditional Medicare. The model randomly assigned approximately 30% of US dialysis facilities and nephrologists to receive financial incentives, ranging from bonuses of 4% to penalties of 5%, based on their patients’ use of home dialysis and kidney transplant/waitlisiting. The payment adjustments apply to all Medicare-based reimbursement for dialysis services. Prior research has demonstrated that dialysis facilities that disproportionately serve populations with high social risk have lower use of home dialysis and kidney transplant, raising concerns that these sites may fare poorly in the payment model. Using data released by CMS, we examined the first year of ETC model performance and financial penalties across dialysis facilities, stratified by the measured social risk of the facilities’ incident patients.
(more…)















 Lisa-Marie Smale, PharmD
Lisa-Marie Smale, PharmD
 If you've been in a scrape and your noggin took a knock, playing it tough and shaking it off isn't the way to go.
If you've been in a scrape and your noggin took a knock, playing it tough and shaking it off isn't the way to go.