Author Interviews, Cancer Research, Immunotherapy, Melanoma, Science, UT Southwestern / 22.03.2023
UT Southwestern Lab Studies Interaction of Gut Microbiota and Cancer Immunotherapy
MedicalResearch.com Interview with:
[caption id="attachment_60218" align="alignleft" width="150"] Dr. Koh[/caption]
Andrew Y. Koh, M.D.
Associate Professor, Pediatrics and Microbiology
University of Texas Southwestern Medical Center
Director of Pediatric Cellular and ImmunoTherapeutics Program
University of Texas Southwestern Medical Center and Children's Health
MedicalResearch.com: What is the background for this study?
Response: We asked the basic question how does a bacteria in your gut help your immune system fight a cancer outside the gut (extraintestinal tumor). Based on work that our group and others have published in the infectious diseases, microbiology, and inflammation fields, we knew that certain conditions (e.g. inflammation, infection) promote gut microbiota to move from the gut to the mesenteric lymph nodes. So we hypothesized that immune checkpoint therapy (which essentially induces inflammation to promote tumor killing) might induce gut microbiota translocation to the mesenteric lymph nodes and that this might be the first step by which gut bacteria can engage with host immune cells.
Dr. Koh[/caption]
Andrew Y. Koh, M.D.
Associate Professor, Pediatrics and Microbiology
University of Texas Southwestern Medical Center
Director of Pediatric Cellular and ImmunoTherapeutics Program
University of Texas Southwestern Medical Center and Children's Health
MedicalResearch.com: What is the background for this study?
Response: We asked the basic question how does a bacteria in your gut help your immune system fight a cancer outside the gut (extraintestinal tumor). Based on work that our group and others have published in the infectious diseases, microbiology, and inflammation fields, we knew that certain conditions (e.g. inflammation, infection) promote gut microbiota to move from the gut to the mesenteric lymph nodes. So we hypothesized that immune checkpoint therapy (which essentially induces inflammation to promote tumor killing) might induce gut microbiota translocation to the mesenteric lymph nodes and that this might be the first step by which gut bacteria can engage with host immune cells.
 Dr. Koh[/caption]
Andrew Y. Koh, M.D.
Associate Professor, Pediatrics and Microbiology
University of Texas Southwestern Medical Center
Director of Pediatric Cellular and ImmunoTherapeutics Program
University of Texas Southwestern Medical Center and Children's Health
MedicalResearch.com: What is the background for this study?
Response: We asked the basic question how does a bacteria in your gut help your immune system fight a cancer outside the gut (extraintestinal tumor). Based on work that our group and others have published in the infectious diseases, microbiology, and inflammation fields, we knew that certain conditions (e.g. inflammation, infection) promote gut microbiota to move from the gut to the mesenteric lymph nodes. So we hypothesized that immune checkpoint therapy (which essentially induces inflammation to promote tumor killing) might induce gut microbiota translocation to the mesenteric lymph nodes and that this might be the first step by which gut bacteria can engage with host immune cells.
Dr. Koh[/caption]
Andrew Y. Koh, M.D.
Associate Professor, Pediatrics and Microbiology
University of Texas Southwestern Medical Center
Director of Pediatric Cellular and ImmunoTherapeutics Program
University of Texas Southwestern Medical Center and Children's Health
MedicalResearch.com: What is the background for this study?
Response: We asked the basic question how does a bacteria in your gut help your immune system fight a cancer outside the gut (extraintestinal tumor). Based on work that our group and others have published in the infectious diseases, microbiology, and inflammation fields, we knew that certain conditions (e.g. inflammation, infection) promote gut microbiota to move from the gut to the mesenteric lymph nodes. So we hypothesized that immune checkpoint therapy (which essentially induces inflammation to promote tumor killing) might induce gut microbiota translocation to the mesenteric lymph nodes and that this might be the first step by which gut bacteria can engage with host immune cells.


 Dr. Mosley[/caption]
Jonathan Mosley, MD, PhD
Associate Professor
Division of Clinical Pharmacology
Departments of Internal Medicine and Biomedical Informatics
Vanderbilt University Medical Center
MedicalResearch.com: What is the background for this study?
Response: Prostate cancer is an important source of morbidity and mortality among men. Earlier detection of disease is essential to reduce these adverse outcomes. Prostate cancer is heritable, and many single nucleotide polymorphisms (SNPs) associated with disease risk have been identified. Thus, there is considerable interest in using tools such as polygenic risk scores, which measure the burden of genetic risk variants an individual carries, to identify men at elevated risk of disease.
Dr. Mosley[/caption]
Jonathan Mosley, MD, PhD
Associate Professor
Division of Clinical Pharmacology
Departments of Internal Medicine and Biomedical Informatics
Vanderbilt University Medical Center
MedicalResearch.com: What is the background for this study?
Response: Prostate cancer is an important source of morbidity and mortality among men. Earlier detection of disease is essential to reduce these adverse outcomes. Prostate cancer is heritable, and many single nucleotide polymorphisms (SNPs) associated with disease risk have been identified. Thus, there is considerable interest in using tools such as polygenic risk scores, which measure the burden of genetic risk variants an individual carries, to identify men at elevated risk of disease.

 Dr. Tsirigos[/caption]
Aristotelis Tsirigos, Ph.D.
Professor of Medicine and Pathology
Co-director, Precision Medicine
Director, Applied Bioinformatics Laboratories
Dr. Tsirigos[/caption]
Aristotelis Tsirigos, Ph.D.
Professor of Medicine and Pathology
Co-director, Precision Medicine
Director, Applied Bioinformatics Laboratories

 Yuxia Wei[/caption]
Yuxia Wei | PhD Student
Unit of Epidemiology
Institute of Environmental Medicine
Karolinska Institutet
Stockholm | Sweden
MedicalResearch.com: What is the background for this study?
Response: Diabetes is traditionally known for having two types (type 1 diabetes and type 2 diabetes). However, it is becoming increasingly clear that diabetes is much more complex than this traditional classification. Several attempts have been made to address this heterogeneity and in 2018, a Swedish ground-breaking study proposed that there are five distinct subtypes of diabetes in adults. They have been replicated in different populations and it has been shown that there are differences between the subtypes in terms of genetics and risks of complications. Another way of elucidating the relevance of these subtypes is to investigate whether the influence of known risk factors for diabetes is different on different subtypes. Our study is one of the first attempts to address this. We used a study design known as Mendelian randomization, to investigate the influence of childhood obesity on these diabetes subtypes that typically occur after age 35. This work was a collaboration between Karolinska institutet in Stockholm, University of Bristol in the UK and Sun Yat-Sen University in China.
Yuxia Wei[/caption]
Yuxia Wei | PhD Student
Unit of Epidemiology
Institute of Environmental Medicine
Karolinska Institutet
Stockholm | Sweden
MedicalResearch.com: What is the background for this study?
Response: Diabetes is traditionally known for having two types (type 1 diabetes and type 2 diabetes). However, it is becoming increasingly clear that diabetes is much more complex than this traditional classification. Several attempts have been made to address this heterogeneity and in 2018, a Swedish ground-breaking study proposed that there are five distinct subtypes of diabetes in adults. They have been replicated in different populations and it has been shown that there are differences between the subtypes in terms of genetics and risks of complications. Another way of elucidating the relevance of these subtypes is to investigate whether the influence of known risk factors for diabetes is different on different subtypes. Our study is one of the first attempts to address this. We used a study design known as Mendelian randomization, to investigate the influence of childhood obesity on these diabetes subtypes that typically occur after age 35. This work was a collaboration between Karolinska institutet in Stockholm, University of Bristol in the UK and Sun Yat-Sen University in China.




 Dr. Pierce[/caption]
Karen Pierce, Ph.D.
Professor, Department of Neurosciences, UCSD
Co-Director, Autism Center of Excellence, UCSD
MedicalResearch.com: What is the background for this study?
Response: The mean age of ASD diagnosis and eventual treatment remains at ~52 months in the United States1 - years beyond the disorder’s prenatal origins2, and beyond the age when it can be reliably diagnosed in many cases3.
Currently the only way to determine if a child has autism spectrum disorder (ASD) is to receive a developmental evaluation from an experienced clinician (usually a licensed clinical psychologist). There are often long waiting lists, and only a small number of clinicians have the experience required to make early-age (i.e., between 12-36 months) diagnoses of ASD. Thus, there are many places in the country as well as world wide wherein children wait months or years to receive a formal diagnosis due to a lack of available expertise. Moreover, diagnostic evaluations are expensive and usually cost the parent and/or insurance approximately ~$2,000 or more per evaluation. Finally, clinical evaluations usually take between 2-3 hours to complete and result in fatigue for both the parent and toddler.
Eye-tracking, which generates biologically-relevant, objective, and quantifiable metrics of both visual and auditory preference profiles in babies and toddlers in just minutes, is a technology that can dramatically change how ASD is diagnosed.
Dr. Pierce[/caption]
Karen Pierce, Ph.D.
Professor, Department of Neurosciences, UCSD
Co-Director, Autism Center of Excellence, UCSD
MedicalResearch.com: What is the background for this study?
Response: The mean age of ASD diagnosis and eventual treatment remains at ~52 months in the United States1 - years beyond the disorder’s prenatal origins2, and beyond the age when it can be reliably diagnosed in many cases3.
Currently the only way to determine if a child has autism spectrum disorder (ASD) is to receive a developmental evaluation from an experienced clinician (usually a licensed clinical psychologist). There are often long waiting lists, and only a small number of clinicians have the experience required to make early-age (i.e., between 12-36 months) diagnoses of ASD. Thus, there are many places in the country as well as world wide wherein children wait months or years to receive a formal diagnosis due to a lack of available expertise. Moreover, diagnostic evaluations are expensive and usually cost the parent and/or insurance approximately ~$2,000 or more per evaluation. Finally, clinical evaluations usually take between 2-3 hours to complete and result in fatigue for both the parent and toddler.
Eye-tracking, which generates biologically-relevant, objective, and quantifiable metrics of both visual and auditory preference profiles in babies and toddlers in just minutes, is a technology that can dramatically change how ASD is diagnosed.


 Dr. Caraballo-Cordovez[/caption]
César Caraballo-Cordovez, MD
Dr. Caraballo-Cordovez[/caption]
César Caraballo-Cordovez, MD




 Dr. Harris[/caption]
MedicalResearch.com Interview with:
Rebecca Arden Harris, MD, MSc
Assistant Professor of Family Medicine and Community Health at the Hospital of the University of Pennsylvania
Senior Fellow, Leonard Davis Institute of Health Economics
Perelman School of Medicine, University of Pennsylvania
MedicalResearch.com: What is the background for this study?
Response: The impact of the nationwide overdose epidemic on Black women has received little attention from policy-makers, researchers, or the press.
MedicalResearch.com: What are the main findings?
Response: Over the 7-year study period, preventable overdose deaths among Black women resulted in nearly 0.75 million years of life lost (YLL). Women aged 25-34 have suffered a rising proportion of this burden.
Dr. Harris[/caption]
MedicalResearch.com Interview with:
Rebecca Arden Harris, MD, MSc
Assistant Professor of Family Medicine and Community Health at the Hospital of the University of Pennsylvania
Senior Fellow, Leonard Davis Institute of Health Economics
Perelman School of Medicine, University of Pennsylvania
MedicalResearch.com: What is the background for this study?
Response: The impact of the nationwide overdose epidemic on Black women has received little attention from policy-makers, researchers, or the press.
MedicalResearch.com: What are the main findings?
Response: Over the 7-year study period, preventable overdose deaths among Black women resulted in nearly 0.75 million years of life lost (YLL). Women aged 25-34 have suffered a rising proportion of this burden.



 Dr. Curhan[/caption]
Sharon G. Curhan, MD, ScM|
Director, CHEARS: The Conservation of Hearing Study
Channing Division of Network Medicine
Department of Medicine
Brigham and Women’s Hospital
Harvard Medical School
Boston, MA 02114
MedicalResearch.com: What is the background for this study?
Response: Herpes zoster, commonly known as “shingles,” is a viral infection that often causes a painful rash. Shingles can occur anywhere on the head or body. Shingles is caused by the varicella zoster virus (VZV), the same virus that causes chickenpox. After a person has chickenpox, the virus stays in their body for the rest of their life. Years and even decades later, the virus may reactivate as shingles. Almost all individuals age 50 years and older in the US have been infected with the varicella zoster virus and therefore they are at risk for shingles.
About 1 in 3 people will develop shingles during their lifetime, and since age is a risk factor for shingles, this number may increase as the population ages. The risk is also higher among individuals of any age who are immunocompromised due to disease or treatment. A number of serious complications can occur when a person develops shingles, such as post-herpetic neuralgia (long-lasting pain), but there was limited information on whether there are other adverse long-term health implications of developing shingles.
There is a growing body of evidence that links VZV, the virus that causes shingles, to vascular disease. VZV vasculopathy may cause damage to blood vessels and increase the risk of stroke or coronary heart disease. Although some previous studies showed a higher risk of stroke or heart attack around the time of the shingles infection, it was not known whether this higher risk persisted in the long term. Therefore, the question we aimed to address in this study was to investigate whether shingles is associated with higher long-term risk of stroke or coronary heart disease.
To address this question, we conducted a prospective longitudinal study in 3 large US cohorts of >200,000 women and men, the Nurses’ Health Study (>79,000 women), the Nurses’ Health Study II (almost 94,000 women) and the Health Professionals Follow-Up Study (>31,000 men), without a prior history of stroke or coronary heart disease. We collected information on shingles, stroke and coronary heart disease on biennial questionnaires and confirmed the diagnoses with medical record review. We followed the participants for up to 16 years and evaluated whether those who had developed shingles were at higher risk for stroke or coronary heart disease years after the shingles episode. The outcomes we measured were incident stroke, incident coronary heart disease [defined as having a non-fatal or fatal myocardial infarction (heart attack) or a coronary revascularization procedure (CABG, coronary artery bypass graft or percutaneous transluminal coronary angioplasty)]. We also evaluated a combined outcome of cardiovascular disease, which included either stroke or coronary heart disease, whichever came first.
Dr. Curhan[/caption]
Sharon G. Curhan, MD, ScM|
Director, CHEARS: The Conservation of Hearing Study
Channing Division of Network Medicine
Department of Medicine
Brigham and Women’s Hospital
Harvard Medical School
Boston, MA 02114
MedicalResearch.com: What is the background for this study?
Response: Herpes zoster, commonly known as “shingles,” is a viral infection that often causes a painful rash. Shingles can occur anywhere on the head or body. Shingles is caused by the varicella zoster virus (VZV), the same virus that causes chickenpox. After a person has chickenpox, the virus stays in their body for the rest of their life. Years and even decades later, the virus may reactivate as shingles. Almost all individuals age 50 years and older in the US have been infected with the varicella zoster virus and therefore they are at risk for shingles.
About 1 in 3 people will develop shingles during their lifetime, and since age is a risk factor for shingles, this number may increase as the population ages. The risk is also higher among individuals of any age who are immunocompromised due to disease or treatment. A number of serious complications can occur when a person develops shingles, such as post-herpetic neuralgia (long-lasting pain), but there was limited information on whether there are other adverse long-term health implications of developing shingles.
There is a growing body of evidence that links VZV, the virus that causes shingles, to vascular disease. VZV vasculopathy may cause damage to blood vessels and increase the risk of stroke or coronary heart disease. Although some previous studies showed a higher risk of stroke or heart attack around the time of the shingles infection, it was not known whether this higher risk persisted in the long term. Therefore, the question we aimed to address in this study was to investigate whether shingles is associated with higher long-term risk of stroke or coronary heart disease.
To address this question, we conducted a prospective longitudinal study in 3 large US cohorts of >200,000 women and men, the Nurses’ Health Study (>79,000 women), the Nurses’ Health Study II (almost 94,000 women) and the Health Professionals Follow-Up Study (>31,000 men), without a prior history of stroke or coronary heart disease. We collected information on shingles, stroke and coronary heart disease on biennial questionnaires and confirmed the diagnoses with medical record review. We followed the participants for up to 16 years and evaluated whether those who had developed shingles were at higher risk for stroke or coronary heart disease years after the shingles episode. The outcomes we measured were incident stroke, incident coronary heart disease [defined as having a non-fatal or fatal myocardial infarction (heart attack) or a coronary revascularization procedure (CABG, coronary artery bypass graft or percutaneous transluminal coronary angioplasty)]. We also evaluated a combined outcome of cardiovascular disease, which included either stroke or coronary heart disease, whichever came first.
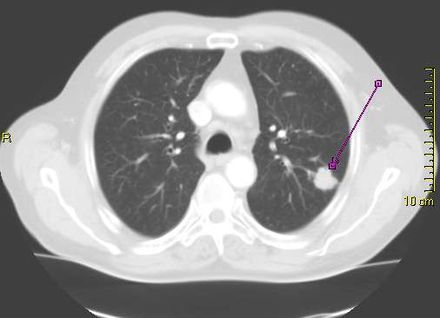
 Dr. Sally Lau[/caption]
Dr. Sally Lau MD
Medical oncologist, NYU Langone’s Perlmutter Cancer Center
Assistant professor of medicine
NYU Grossman School of Medicine
MedicalResearch.com: How big is the problem of
Dr. Sally Lau[/caption]
Dr. Sally Lau MD
Medical oncologist, NYU Langone’s Perlmutter Cancer Center
Assistant professor of medicine
NYU Grossman School of Medicine
MedicalResearch.com: How big is the problem of 

 Dr. Shan[/caption]
Zhilei Shan, MD, PhD
Postdoctoral fellow on Nutritional Epidemiology
Harvard T.H. Chan School of Public Health
MedicalResearch.com: What is the background for this study?
Response: Unhealthy sleep behaviors and sleep disturbances are associated with higher risk of multiple diseases and mortality. The current profiles of sleep habits and disturbances, particularly the differences between workdays and free days, are unknown in the contemporary US.
MedicalResearch.com: What are the main findings?
Response: In this nationally representative cross-sectional analysis with 9004 adults aged 20 years or older, differences in sleep patterns between workdays and free days were observed. The mean sleep duration was 7.59 hours on workdays and 8.24 hours on free days (difference, 0.65 hour). The mean sleep and wake times were at 11:02 PM and 6:41 AM, respectively, on workdays and 11:25 PM and 7:41 AM, respectively, on free days (differences, 0.23 hour for sleep time and 1.00 hour for wake time). With regard to sleep disturbances, 30.5% of adults experienced 1 hour or more of sleep debt,46.5% experienced 1 hour or more of social jet lag, 29.8% had trouble sleeping, and 27.2% experienced daytime sleepiness.
Dr. Shan[/caption]
Zhilei Shan, MD, PhD
Postdoctoral fellow on Nutritional Epidemiology
Harvard T.H. Chan School of Public Health
MedicalResearch.com: What is the background for this study?
Response: Unhealthy sleep behaviors and sleep disturbances are associated with higher risk of multiple diseases and mortality. The current profiles of sleep habits and disturbances, particularly the differences between workdays and free days, are unknown in the contemporary US.
MedicalResearch.com: What are the main findings?
Response: In this nationally representative cross-sectional analysis with 9004 adults aged 20 years or older, differences in sleep patterns between workdays and free days were observed. The mean sleep duration was 7.59 hours on workdays and 8.24 hours on free days (difference, 0.65 hour). The mean sleep and wake times were at 11:02 PM and 6:41 AM, respectively, on workdays and 11:25 PM and 7:41 AM, respectively, on free days (differences, 0.23 hour for sleep time and 1.00 hour for wake time). With regard to sleep disturbances, 30.5% of adults experienced 1 hour or more of sleep debt,46.5% experienced 1 hour or more of social jet lag, 29.8% had trouble sleeping, and 27.2% experienced daytime sleepiness.


 Dr. Wong[/caption]
Mitchell Wong, MD PhD
Professor of Medicine
Executive Vice Chair for Research Training
Department of Medicine
Executive Co-Director, Specialty Training and Advanced Research (STAR) Program
Director, UCLA CTSI KL2 Program
UCLA Division of General Internal Medicine and Health Services Research Los Angeles, CA 90024
MedicalResearch.com: What is the background for this study?
Response: It is estimated that social factors like poverty, education, and housing have a large impact on health. Yet, there are few interventions that exist to directly address those issues. Schools are a promising solution since society already invests heavily in education and schools are an everyday part of most children’s lives.
Dr. Wong[/caption]
Mitchell Wong, MD PhD
Professor of Medicine
Executive Vice Chair for Research Training
Department of Medicine
Executive Co-Director, Specialty Training and Advanced Research (STAR) Program
Director, UCLA CTSI KL2 Program
UCLA Division of General Internal Medicine and Health Services Research Los Angeles, CA 90024
MedicalResearch.com: What is the background for this study?
Response: It is estimated that social factors like poverty, education, and housing have a large impact on health. Yet, there are few interventions that exist to directly address those issues. Schools are a promising solution since society already invests heavily in education and schools are an everyday part of most children’s lives.

 Dr. Ogedegbe[/caption]
Gbenga Ogedegbe, MD, MPH
Dr. Adolph & Margaret Berger Professor of Population Health
Director, Division of Health & Behavior
Director Center for Healthful Behavior Change
Department of Population Health
NYU Langone Health
NYU School of Medicine
Member of the U.S. Preventive Services Task Force
MedicalResearch.com: What is the background for this study?
Response: Syphilis has become more common over the past 20 years, after reaching a record low in 2000. The Task Force found that screening people who are at increased risk for syphilis can identify the infection early so it can be treated before problems develop. For that reason, the Task Force recommends screening people who are at increased risk for syphilis infection.
Dr. Ogedegbe[/caption]
Gbenga Ogedegbe, MD, MPH
Dr. Adolph & Margaret Berger Professor of Population Health
Director, Division of Health & Behavior
Director Center for Healthful Behavior Change
Department of Population Health
NYU Langone Health
NYU School of Medicine
Member of the U.S. Preventive Services Task Force
MedicalResearch.com: What is the background for this study?
Response: Syphilis has become more common over the past 20 years, after reaching a record low in 2000. The Task Force found that screening people who are at increased risk for syphilis can identify the infection early so it can be treated before problems develop. For that reason, the Task Force recommends screening people who are at increased risk for syphilis infection.

 Dr. Robbins[/caption]
Rebecca Robbins, Ph.D.
Instructor in Medicine
Associate Scientist, Division of Sleep and Circadian Disorders
Investigator, Division of Sleep and Circadian Disorders
Departments of Medicine and Neurology
Brigham and Women's Hospital
MedicalResearch.com: What is the background for this study?
Response: Teens face myriad challenges to sleep, ranging from biological factors, including a preference for later bedtimes and increased need for sleep, to social factors, including social pressures and increased academic workloads, all limiting teenagers in their ability to keep a healthy sleep schedule.
In a nationally representative sample, we explored the prevalence of another potential barrier to sleep among teens, which are a set of beliefs that are held in the population, yet are actual counter to scientific principles regarding sleep and circadian rhythms.
Dr. Robbins[/caption]
Rebecca Robbins, Ph.D.
Instructor in Medicine
Associate Scientist, Division of Sleep and Circadian Disorders
Investigator, Division of Sleep and Circadian Disorders
Departments of Medicine and Neurology
Brigham and Women's Hospital
MedicalResearch.com: What is the background for this study?
Response: Teens face myriad challenges to sleep, ranging from biological factors, including a preference for later bedtimes and increased need for sleep, to social factors, including social pressures and increased academic workloads, all limiting teenagers in their ability to keep a healthy sleep schedule.
In a nationally representative sample, we explored the prevalence of another potential barrier to sleep among teens, which are a set of beliefs that are held in the population, yet are actual counter to scientific principles regarding sleep and circadian rhythms.