Author Interviews, Dermatology, Yale / 08.04.2022
JAK Inhibitors Show Promise For Treatment of Severe Alopecia Areata
MedicalResearch.com Interview with:
 Brett King, MD, PhD, FAAD
Associate Professor of Dermatology
Yale School of Medicine
MedicalResearch.com: What is the background for this study?
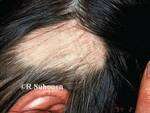
Response: Alopecia areata is an autoimmune disorder marked by disfiguring, non-scarring hair loss, and there are no therapies approved by the U.S. Food and Drug Administration for treatment of the disease. JAK inhibitors are showing promise for treatment of severe alopecia areata. In this work, the pooled results of two phase 3 clinical trials of the JAK inhibitor baricitinib were reported out to 52 weeks.
Brett King, MD, PhD, FAAD
Associate Professor of Dermatology
Yale School of Medicine
MedicalResearch.com: What is the background for this study?
Response: Alopecia areata is an autoimmune disorder marked by disfiguring, non-scarring hair loss, and there are no therapies approved by the U.S. Food and Drug Administration for treatment of the disease. JAK inhibitors are showing promise for treatment of severe alopecia areata. In this work, the pooled results of two phase 3 clinical trials of the JAK inhibitor baricitinib were reported out to 52 weeks.
 Brett King, MD, PhD, FAAD
Associate Professor of Dermatology
Yale School of Medicine
MedicalResearch.com: What is the background for this study?
Response: Alopecia areata is an autoimmune disorder marked by disfiguring, non-scarring hair loss, and there are no therapies approved by the U.S. Food and Drug Administration for treatment of the disease. JAK inhibitors are showing promise for treatment of severe alopecia areata. In this work, the pooled results of two phase 3 clinical trials of the JAK inhibitor baricitinib were reported out to 52 weeks.
Brett King, MD, PhD, FAAD
Associate Professor of Dermatology
Yale School of Medicine
MedicalResearch.com: What is the background for this study?
Response: Alopecia areata is an autoimmune disorder marked by disfiguring, non-scarring hair loss, and there are no therapies approved by the U.S. Food and Drug Administration for treatment of the disease. JAK inhibitors are showing promise for treatment of severe alopecia areata. In this work, the pooled results of two phase 3 clinical trials of the JAK inhibitor baricitinib were reported out to 52 weeks.



 Dr. Ying-Hui Fu[/caption]
Ying-Hui Fu, PhD
Professor, Neurology
Weill Institute for Neurosciences
UCSF
MedicalResearch.com: What is the background for this study?
Response: Most people are aware that a lack of sleep is associated with all sorts of health issues. However, familial natural short sleeper (FNSS) individuals sleep 4-6.5 hours a night most of their live and stay healthy. We set out to determine whether natural short sleep mutations can offer protection from various diseases. We chose Alzheimer as an example to start.
Dr. Ying-Hui Fu[/caption]
Ying-Hui Fu, PhD
Professor, Neurology
Weill Institute for Neurosciences
UCSF
MedicalResearch.com: What is the background for this study?
Response: Most people are aware that a lack of sleep is associated with all sorts of health issues. However, familial natural short sleeper (FNSS) individuals sleep 4-6.5 hours a night most of their live and stay healthy. We set out to determine whether natural short sleep mutations can offer protection from various diseases. We chose Alzheimer as an example to start.


 Dr. Sesso[/caption]
Howard D. Sesso, ScD, MPH
Associate Professor of Medicine
Division of Preventive Medicine
Brigham and Women's Hospital
MedicalResearch.com: What is the background for this study? How does the amount of flavanols in the study arm compare to what might be obtained in a typical diet?
Response: The COcoa Supplement and Multivitamin Outcomes Study (COSMOS) is a randomized, double-blind, placebo-controlled clinical trial that tested the effects of two promising dietary supplements on cardiovascular disease (CVD) and cancer in 21,442 older adults. Cocoa flavanols have been shown to have favorable vascular effects in small and short-term clinical trials. The 500 mg/day flavanols tested in COSMOS exceeds that readily obtained in the diet typically from cocoa, tea, grapes, and berries. Of note, flavanol content in not typically listed on food labels.
COSMOS also tested a multivitamin, the most common dietary supplement taken by US adults and previously linked with a potential modest reduction in cancer in a previous long-term trial of men conducted by our research group at the Division of Preventive Medicine at Brigham and Women’s Hospital.
Dr. Sesso[/caption]
Howard D. Sesso, ScD, MPH
Associate Professor of Medicine
Division of Preventive Medicine
Brigham and Women's Hospital
MedicalResearch.com: What is the background for this study? How does the amount of flavanols in the study arm compare to what might be obtained in a typical diet?
Response: The COcoa Supplement and Multivitamin Outcomes Study (COSMOS) is a randomized, double-blind, placebo-controlled clinical trial that tested the effects of two promising dietary supplements on cardiovascular disease (CVD) and cancer in 21,442 older adults. Cocoa flavanols have been shown to have favorable vascular effects in small and short-term clinical trials. The 500 mg/day flavanols tested in COSMOS exceeds that readily obtained in the diet typically from cocoa, tea, grapes, and berries. Of note, flavanol content in not typically listed on food labels.
COSMOS also tested a multivitamin, the most common dietary supplement taken by US adults and previously linked with a potential modest reduction in cancer in a previous long-term trial of men conducted by our research group at the Division of Preventive Medicine at Brigham and Women’s Hospital.
 Dr. Launer[/caption]
Lenore J. Launer, Ph.D.
Chief, Laboratory of Epidemiology and Population Sciences
Intramural Research Program, National Institute on Aging.
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Identifying early risk factors and early changes in the brain will have a major impact on future clinical and public health priorities related to the looming epidemic of dementia. Several studies based on older populations suggest mid-life is an important period to start prevention measures. To date control of blood pressure levels has been the most robust and promising candidate to target for prevention of future cognitive impairment. Although several studies have looked at levels of blood pressure and risk for cognitive impairment, it was not known whether trajectories from young adulthood to middle age studies provided additional information about risk. To investigate possible biomarkers of future risk, we chose to examine the association of the mean arterial blood pressure trajectories to indicators of pathology seen on MRI and that are associated with cognition.
We highlight the results of the mean arterial blood pressure (MAP) measure, which is an integrated measure of systolic and diastolic blood pressure.
Dr. Launer[/caption]
Lenore J. Launer, Ph.D.
Chief, Laboratory of Epidemiology and Population Sciences
Intramural Research Program, National Institute on Aging.
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Identifying early risk factors and early changes in the brain will have a major impact on future clinical and public health priorities related to the looming epidemic of dementia. Several studies based on older populations suggest mid-life is an important period to start prevention measures. To date control of blood pressure levels has been the most robust and promising candidate to target for prevention of future cognitive impairment. Although several studies have looked at levels of blood pressure and risk for cognitive impairment, it was not known whether trajectories from young adulthood to middle age studies provided additional information about risk. To investigate possible biomarkers of future risk, we chose to examine the association of the mean arterial blood pressure trajectories to indicators of pathology seen on MRI and that are associated with cognition.
We highlight the results of the mean arterial blood pressure (MAP) measure, which is an integrated measure of systolic and diastolic blood pressure.

 Response: Cigarette smoking is one of the well-established causes of periodontitis, but the effect of using electronic cigarettes (e-cig), especially its long-term impact on periodontal health, is not yet clearly understood. Considering the increased popularity of e-cig use, especially among teenagers and young adults, and the known effect of high nicotine concentration in e-cigarette products, we conducted this clinical research to see if there were differences in periodontal health between e-cig users, traditional smokers, and nonsmokers. The study consisted of two visits, 6 months apart, where measures of oral and periodontal health were obtained.
Our data showed significantly greater clinical attachment loss in the e-cigarette users and cigarette smokers than in the non-smokers at both study visits. In only e-cigarette users, we observed an over 0.2 mm average increase in the clinical attachment loss after 6 months.
Response: Cigarette smoking is one of the well-established causes of periodontitis, but the effect of using electronic cigarettes (e-cig), especially its long-term impact on periodontal health, is not yet clearly understood. Considering the increased popularity of e-cig use, especially among teenagers and young adults, and the known effect of high nicotine concentration in e-cigarette products, we conducted this clinical research to see if there were differences in periodontal health between e-cig users, traditional smokers, and nonsmokers. The study consisted of two visits, 6 months apart, where measures of oral and periodontal health were obtained.
Our data showed significantly greater clinical attachment loss in the e-cigarette users and cigarette smokers than in the non-smokers at both study visits. In only e-cigarette users, we observed an over 0.2 mm average increase in the clinical attachment loss after 6 months. 









 Dr. Eberly[/caption]
Lauren A. Eberly, MD, MPH
Clinical Fellow, Cardiovascular Medicine
Perelman School of Medicine
Cardiovascular Division, Perelman School of Medicine
Center for Cardiovascular Outcomes, Quality, and Evaluative Research,
Cardiovascular Center for Health Equity and Social Justice,
Leonard Davis Institute of Health Economics
University of Pennsylvania, Philadelphia
MedicalResearch.com: What is the background for this study?
Response: Racial inequities are pervasive in our country, and cardiovascular therapeutics with proven benefit have been shown to be underutilized among Black and Latinx patients.
Glucagon-like peptide-1 receptor agonists (GLP-1 RAs), a recommended treatment option for glycemic control in patients with diabetes, have recently emerged as a cardioprotective therapy as multiple large randomized clinical trials have shown they prevent cardiovascular events among patients with Type 2 Diabetes (T2D), particularly patients with established atherosclerotic cardiovascular disease (ASCVD). Given this, they are now recommended therapy for patients with diabetes and established or high risk of ASCVD.
Given the known inequitable utilization of other therapies, along with the known higher burden of diabetes and cardiovascular disease among Black patients, the aim of this study was to evaluate the uptake of GLP-1 RA as well as for inequities in utilization.
Dr. Eberly[/caption]
Lauren A. Eberly, MD, MPH
Clinical Fellow, Cardiovascular Medicine
Perelman School of Medicine
Cardiovascular Division, Perelman School of Medicine
Center for Cardiovascular Outcomes, Quality, and Evaluative Research,
Cardiovascular Center for Health Equity and Social Justice,
Leonard Davis Institute of Health Economics
University of Pennsylvania, Philadelphia
MedicalResearch.com: What is the background for this study?
Response: Racial inequities are pervasive in our country, and cardiovascular therapeutics with proven benefit have been shown to be underutilized among Black and Latinx patients.
Glucagon-like peptide-1 receptor agonists (GLP-1 RAs), a recommended treatment option for glycemic control in patients with diabetes, have recently emerged as a cardioprotective therapy as multiple large randomized clinical trials have shown they prevent cardiovascular events among patients with Type 2 Diabetes (T2D), particularly patients with established atherosclerotic cardiovascular disease (ASCVD). Given this, they are now recommended therapy for patients with diabetes and established or high risk of ASCVD.
Given the known inequitable utilization of other therapies, along with the known higher burden of diabetes and cardiovascular disease among Black patients, the aim of this study was to evaluate the uptake of GLP-1 RA as well as for inequities in utilization.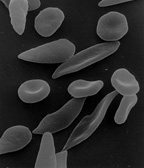
 Dr. Mapara[/caption]
Markus Y Mapara, MD
Professor of Medicine
Director of the Blood and Marrow Transplantation
Columbia University Medical Center
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Sickle cell disease is caused by a point mutation in the beta-globin gene of hemoglobin resulting in the production of abnormal hemoglobin which leads to formation of sickle-shaped RBC under conditions of low oxygen. Sickle cell disease affects about 100,000 patients in the US which are predominantly African American. The only curative approach is to perform an allogeneic bone marrow transplant which is however fraught with significant treatment-related risks if a matched sibling donor is not available.
The current study describes the successful application of a novel gene therapy to treat patients with sickle cell disease. The strategy is based on a gene-addition approach to introduce the genetic information for a Hemoglobin F-like molecule termed HgAT87Q into hematopoietic stem cells. The expression of this novel hemoglobin prevents polymerization of HgbS and has now been demonstrated to prevent the occurrence of vaso-occlusive pain crises in sickle cell disease patients.
Dr. Mapara[/caption]
Markus Y Mapara, MD
Professor of Medicine
Director of the Blood and Marrow Transplantation
Columbia University Medical Center
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Sickle cell disease is caused by a point mutation in the beta-globin gene of hemoglobin resulting in the production of abnormal hemoglobin which leads to formation of sickle-shaped RBC under conditions of low oxygen. Sickle cell disease affects about 100,000 patients in the US which are predominantly African American. The only curative approach is to perform an allogeneic bone marrow transplant which is however fraught with significant treatment-related risks if a matched sibling donor is not available.
The current study describes the successful application of a novel gene therapy to treat patients with sickle cell disease. The strategy is based on a gene-addition approach to introduce the genetic information for a Hemoglobin F-like molecule termed HgAT87Q into hematopoietic stem cells. The expression of this novel hemoglobin prevents polymerization of HgbS and has now been demonstrated to prevent the occurrence of vaso-occlusive pain crises in sickle cell disease patients.

 Dr. Thakrar[/caption]
Ashish Thakrar, MD
Internal Medicine & Addiction Medicine
National Clinician Scholars Program
University of Pennsylvania
MedicalResearch.com: What is the background for this study?
Response: About 1.8 million Americans are currently incarcerated, more than any other country in the world per capita. Of those 1.8 million, about 1 in 7 suffers from opioid addiction, putting them at high risk of overdose and death, particularly in the weeks following release.
Opioid use disorder is a treatable condition, particularly with the medications buprenorphine or methadone, but historically, prisons and jails have not offered treatment. Over the past five years, a few states and municipalities have enacted policies to provide access for OUD treatment. We examined whether these policies were actually improving access to treatment.
Dr. Thakrar[/caption]
Ashish Thakrar, MD
Internal Medicine & Addiction Medicine
National Clinician Scholars Program
University of Pennsylvania
MedicalResearch.com: What is the background for this study?
Response: About 1.8 million Americans are currently incarcerated, more than any other country in the world per capita. Of those 1.8 million, about 1 in 7 suffers from opioid addiction, putting them at high risk of overdose and death, particularly in the weeks following release.
Opioid use disorder is a treatable condition, particularly with the medications buprenorphine or methadone, but historically, prisons and jails have not offered treatment. Over the past five years, a few states and municipalities have enacted policies to provide access for OUD treatment. We examined whether these policies were actually improving access to treatment. 

 Dr. Dickerman[/caption]
Dr. Barbra Dickerman, PhD
CAUSALab investigator and instructor
Department of Epidemiology
Harvard T.H. Chan School of Public Health
MedicalResearch.com: What is the background for this study?
Response: Early randomized trials showed that the BNT162b2 (Pfizer-BioNTech) and mRNA-1273 (Moderna) vaccines were both remarkably effective at preventing symptomatic disease, when comparing each vaccine with no vaccine. However, head-to-head comparisons of these vaccines have been lacking, leaving open the question of which vaccine is more effective.
In this study, we analyzed the VA’s high-quality databases in a way that emulated the design of the hypothetical trial that would have answered this question. Specifically, we used the findings from the original trials to benchmark our methods and then extended them to provide novel evidence for the comparative effectiveness of these two vaccines in a real-world setting and across diverse subgroups and different time periods.
Dr. Dickerman[/caption]
Dr. Barbra Dickerman, PhD
CAUSALab investigator and instructor
Department of Epidemiology
Harvard T.H. Chan School of Public Health
MedicalResearch.com: What is the background for this study?
Response: Early randomized trials showed that the BNT162b2 (Pfizer-BioNTech) and mRNA-1273 (Moderna) vaccines were both remarkably effective at preventing symptomatic disease, when comparing each vaccine with no vaccine. However, head-to-head comparisons of these vaccines have been lacking, leaving open the question of which vaccine is more effective.
In this study, we analyzed the VA’s high-quality databases in a way that emulated the design of the hypothetical trial that would have answered this question. Specifically, we used the findings from the original trials to benchmark our methods and then extended them to provide novel evidence for the comparative effectiveness of these two vaccines in a real-world setting and across diverse subgroups and different time periods.
 Dr. Woodruff[/caption]
Carina M. Woodruff, MD
Department of Dermatolog
University of California, San Francisco
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Rigorous hand hygiene has been an important component of the CDC's COVID-19 guidelines. With millions of Americans now using hand sanitizers regularly, we are seeing many more cases of hand dermatitis. Our study evaluated the key product features and most common allergens in the top-reviewed, commercial hand sanitizers sold by major US retailers.
We found that the most common potential allergens were tocopherol, fragrance, propylene glycol and phenoxyethanol. Our study also showed that nearly 1 in 5 marketing claims on these products was misleading. For example, 70% of sanitizers with the marketing claim "hypoallergenic" included at least one common allergen in its formulation.
Dr. Woodruff[/caption]
Carina M. Woodruff, MD
Department of Dermatolog
University of California, San Francisco
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Rigorous hand hygiene has been an important component of the CDC's COVID-19 guidelines. With millions of Americans now using hand sanitizers regularly, we are seeing many more cases of hand dermatitis. Our study evaluated the key product features and most common allergens in the top-reviewed, commercial hand sanitizers sold by major US retailers.
We found that the most common potential allergens were tocopherol, fragrance, propylene glycol and phenoxyethanol. Our study also showed that nearly 1 in 5 marketing claims on these products was misleading. For example, 70% of sanitizers with the marketing claim "hypoallergenic" included at least one common allergen in its formulation.



 Dr. Ashwin Nathan[/caption]
Ashwin Nathan, MD, MSHP
Assistant Professor, Medicine, Perelman School of Medicine
Interventional Cardiologist
Hospital of the University of Pennsylvania and at the
Corporal Michael C. Crescenz VA Medical Center in Philadelphia
Penn Cardiovascular Outcomes, Quality & Evaluative Research Center
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: We found that the rates of TAVR were lower in areas with higher proportions of Black, Hispanic and socioeconomically disadvantaged patients. Inequities in access in areas with higher proportions of Black and Hispanic patients existed despite adjusting for socioeconomic status.
Dr. Ashwin Nathan[/caption]
Ashwin Nathan, MD, MSHP
Assistant Professor, Medicine, Perelman School of Medicine
Interventional Cardiologist
Hospital of the University of Pennsylvania and at the
Corporal Michael C. Crescenz VA Medical Center in Philadelphia
Penn Cardiovascular Outcomes, Quality & Evaluative Research Center
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: We found that the rates of TAVR were lower in areas with higher proportions of Black, Hispanic and socioeconomically disadvantaged patients. Inequities in access in areas with higher proportions of Black and Hispanic patients existed despite adjusting for socioeconomic status.
