AHA Journals, Author Interviews, Obstructive Sleep Apnea, UCSF / 21.06.2021
AHA Scientific Statement Highlights Link Between Obstructive Sleep Apnea and Heart Disease
MedicalResearch.com Interview with:
[caption id="attachment_57673" align="alignleft" width="200"] Dr. Yeghiazarians[/caption]
Yerem Yeghiazarians, MD
Professor of Medicine
Leone-Perkins Family Endowed Chair in Cardiology
San Francisco Board Past-President, American Heart Association
Co-Director, Adult Cardiac Catheterization Laboratory
Director, Peripheral Interventional Cardiology Program
Director, Translational Cardiac Stem Cell Program
Cardiovascular Research Institute
Eli and Edythe Broad Center of Regeneration Medicine and Stem Cell Research
Associate Member in Experimental Therapeutics, UCSF Helen Diller Cancer Center
University of California, San Francisco
MedicalResearch.com: What is the background for this study?
Response: Obstructive sleep apnea is very common, undiagnosed and undertreated. The AHA Scientific Statement was prepared to increase awareness amongst physicians and patients about this condition and to encourage more screening and therapy as appropriate.
Obesity is certainly one of the significant risk factors for sleep apnea and we highlight this in the Scientific Statement:
“The risk of OSA correlates with body mass index, and obesity remains the one major modifiable
risk factor for OSA. In a population-based cohort study of 690 subjects, a 10% weight gain was associated with nearly 32% increase in the apnea-hypopnea index (AHI), and even modest weight control was effective in reducing the new occurrence of sleep-disordered breathing. An even stronger correlation exists between OSA and increased waist circumference and neck size.
Neck sizes predisposing to OSA are usually >17 and 16 in for men and women, respectively.”
Dr. Yeghiazarians[/caption]
Yerem Yeghiazarians, MD
Professor of Medicine
Leone-Perkins Family Endowed Chair in Cardiology
San Francisco Board Past-President, American Heart Association
Co-Director, Adult Cardiac Catheterization Laboratory
Director, Peripheral Interventional Cardiology Program
Director, Translational Cardiac Stem Cell Program
Cardiovascular Research Institute
Eli and Edythe Broad Center of Regeneration Medicine and Stem Cell Research
Associate Member in Experimental Therapeutics, UCSF Helen Diller Cancer Center
University of California, San Francisco
MedicalResearch.com: What is the background for this study?
Response: Obstructive sleep apnea is very common, undiagnosed and undertreated. The AHA Scientific Statement was prepared to increase awareness amongst physicians and patients about this condition and to encourage more screening and therapy as appropriate.
Obesity is certainly one of the significant risk factors for sleep apnea and we highlight this in the Scientific Statement:
“The risk of OSA correlates with body mass index, and obesity remains the one major modifiable
risk factor for OSA. In a population-based cohort study of 690 subjects, a 10% weight gain was associated with nearly 32% increase in the apnea-hypopnea index (AHI), and even modest weight control was effective in reducing the new occurrence of sleep-disordered breathing. An even stronger correlation exists between OSA and increased waist circumference and neck size.
Neck sizes predisposing to OSA are usually >17 and 16 in for men and women, respectively.”
 Dr. Yeghiazarians[/caption]
Yerem Yeghiazarians, MD
Professor of Medicine
Leone-Perkins Family Endowed Chair in Cardiology
San Francisco Board Past-President, American Heart Association
Co-Director, Adult Cardiac Catheterization Laboratory
Director, Peripheral Interventional Cardiology Program
Director, Translational Cardiac Stem Cell Program
Cardiovascular Research Institute
Eli and Edythe Broad Center of Regeneration Medicine and Stem Cell Research
Associate Member in Experimental Therapeutics, UCSF Helen Diller Cancer Center
University of California, San Francisco
MedicalResearch.com: What is the background for this study?
Response: Obstructive sleep apnea is very common, undiagnosed and undertreated. The AHA Scientific Statement was prepared to increase awareness amongst physicians and patients about this condition and to encourage more screening and therapy as appropriate.
Obesity is certainly one of the significant risk factors for sleep apnea and we highlight this in the Scientific Statement:
“The risk of OSA correlates with body mass index, and obesity remains the one major modifiable
risk factor for OSA. In a population-based cohort study of 690 subjects, a 10% weight gain was associated with nearly 32% increase in the apnea-hypopnea index (AHI), and even modest weight control was effective in reducing the new occurrence of sleep-disordered breathing. An even stronger correlation exists between OSA and increased waist circumference and neck size.
Neck sizes predisposing to OSA are usually >17 and 16 in for men and women, respectively.”
Dr. Yeghiazarians[/caption]
Yerem Yeghiazarians, MD
Professor of Medicine
Leone-Perkins Family Endowed Chair in Cardiology
San Francisco Board Past-President, American Heart Association
Co-Director, Adult Cardiac Catheterization Laboratory
Director, Peripheral Interventional Cardiology Program
Director, Translational Cardiac Stem Cell Program
Cardiovascular Research Institute
Eli and Edythe Broad Center of Regeneration Medicine and Stem Cell Research
Associate Member in Experimental Therapeutics, UCSF Helen Diller Cancer Center
University of California, San Francisco
MedicalResearch.com: What is the background for this study?
Response: Obstructive sleep apnea is very common, undiagnosed and undertreated. The AHA Scientific Statement was prepared to increase awareness amongst physicians and patients about this condition and to encourage more screening and therapy as appropriate.
Obesity is certainly one of the significant risk factors for sleep apnea and we highlight this in the Scientific Statement:
“The risk of OSA correlates with body mass index, and obesity remains the one major modifiable
risk factor for OSA. In a population-based cohort study of 690 subjects, a 10% weight gain was associated with nearly 32% increase in the apnea-hypopnea index (AHI), and even modest weight control was effective in reducing the new occurrence of sleep-disordered breathing. An even stronger correlation exists between OSA and increased waist circumference and neck size.
Neck sizes predisposing to OSA are usually >17 and 16 in for men and women, respectively.”






 Dr. Hwang[/caption]
Geelsu Hwang, Ph.D.
Assistant Professor
Department of Preventive and Restorative Sciences
Center for Innovation and Precision Dentistry (CiPD)
School of Dental Medicine
University of Pennsylvania
MedicalResearch.com: What is the background for this study? What is the significance of this oral biofilm?
Response: Dental caries is one of the most common and costly biofilm-dependent diseases that afflict children and adults worldwide. Particularly, Early Childhood Caries (ECC) is a hyper-virulent type of chronic tooth decay that most frequently afflicts underprivileged preschool children. The onset and progression of carious lesions in ECC are rapid and aggressive, causing rampant destruction of the smooth surfaces of teeth.
ECC is painful and often requires surgical procedure under general anesthesia, while current treatment modalities are inefficient and recurrence of ECC is common. Notably, interactions between a fungus, Candida albicans, and a bacterium, Streptococcus mutans, have been known to play important roles in the pathogenesis of dental caries.
Thus, we attempted to strategically develop a targeted measure to effectively prevent cross-kingdom interactions and subsequent biofilm development.
Dr. Hwang[/caption]
Geelsu Hwang, Ph.D.
Assistant Professor
Department of Preventive and Restorative Sciences
Center for Innovation and Precision Dentistry (CiPD)
School of Dental Medicine
University of Pennsylvania
MedicalResearch.com: What is the background for this study? What is the significance of this oral biofilm?
Response: Dental caries is one of the most common and costly biofilm-dependent diseases that afflict children and adults worldwide. Particularly, Early Childhood Caries (ECC) is a hyper-virulent type of chronic tooth decay that most frequently afflicts underprivileged preschool children. The onset and progression of carious lesions in ECC are rapid and aggressive, causing rampant destruction of the smooth surfaces of teeth.
ECC is painful and often requires surgical procedure under general anesthesia, while current treatment modalities are inefficient and recurrence of ECC is common. Notably, interactions between a fungus, Candida albicans, and a bacterium, Streptococcus mutans, have been known to play important roles in the pathogenesis of dental caries.
Thus, we attempted to strategically develop a targeted measure to effectively prevent cross-kingdom interactions and subsequent biofilm development.


 Dr. Clarke[/caption]
Katherine Clark, MD MBA
Division of Cardiovascular Medicine
Department of Internal Medicine
Yale School of Medicine
MedicalResearch.com: What is the background for this study?
Response: Racial and ethnic disparities affect cardiac transplantation outcomes. In cohort analyses of racial and ethnic groups from the previous three decades, Black patients were constantly at a higher risk of mortality after cardiac transplantation. In 2018, the United Network for Organ Sharing (UNOS) revised the allocation system to expand access to organs for the most medically urgent patients and reduce disparities and regional differences. We sought to evaluate contemporary trends and impact of the new 2018 allocation system.
Dr. Clarke[/caption]
Katherine Clark, MD MBA
Division of Cardiovascular Medicine
Department of Internal Medicine
Yale School of Medicine
MedicalResearch.com: What is the background for this study?
Response: Racial and ethnic disparities affect cardiac transplantation outcomes. In cohort analyses of racial and ethnic groups from the previous three decades, Black patients were constantly at a higher risk of mortality after cardiac transplantation. In 2018, the United Network for Organ Sharing (UNOS) revised the allocation system to expand access to organs for the most medically urgent patients and reduce disparities and regional differences. We sought to evaluate contemporary trends and impact of the new 2018 allocation system.

 Dr. Hoberman[/caption]
Alejandro Hoberman, M.D.
Vice Chair of Clinical Research, Division Director, General Academic Pediatrics, and Professor of Pediatrics and Clinical and Translational Science
Jack L. Paradise, MD Endowed Professor of Pediatric Research, UPMC Children's Hospital of PittsburghPresident, UPMC Children's Community Pediatrics
MedicalResearch.com: What is the background for this study?
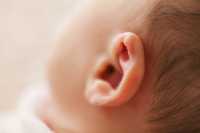
Response: Acute otitis media (AOM) is the most frequently diagnosed illness in children in the United States for which antibiotics are prescribed. Recurrent AOM is the principal indication for tympanostomy-tube placement, the most frequently performed operation in children after the newborn period. Supporting the performance of tympanostomy-tube placement for recurrent acute otitis media has been the commonplace observation, after surgery, of acute otitis media–free periods of varying duration. Counterbalancing this view have been the cost of tympanostomy-tube placement; risks and possible late sequelae of anesthesia in young children; the possible occurrence of refractory tube otorrhea, tube blockage, premature extrusion, or dislocation of the tube into the middle-ear cavity; various structural tympanic membrane sequelae; and the possible development of mild conductive hearing loss. Tempering support for surgery is the progressive reduction in the incidence of acute otitis media that usually accompanies a child’s increasing age.
Previous trials of tympanostomy-tube placement for recurrent acute otitis media, all conducted before the introduction of pneumococcal conjugate vaccine, have given mixed results and were limited, variously, by small sample size, uncertain validity of diagnoses of acute otitis media determining trial eligibility, short periods of follow-up, and substantial attrition of participants. Official recommendations regarding tympanostomy-tube placement for children with recurrent acute otitis media differ — an otolaryngologic guideline recommends the procedure for children with recurrent acute otitis media, provided that middle-ear effusion is present in at least one ear; a contemporaneous pediatric guideline discusses tympanostomy-tube placement as an “option [that] clinicians may offer.”
Given these uncertainties, we undertook the present trial involving children 6 to 35 months of age who had a history of recurrent acute otitis media to determine whether tympanostomy-tube placement, as compared with medical management (comprising episodic antimicrobial treatment, with the option of tympanostomy-tube placement in the event of treatment failure), would result in a greater reduction in the children’s rate of recurrence of acute otitis media during the ensuing 2-year period.
Dr. Hoberman[/caption]
Alejandro Hoberman, M.D.
Vice Chair of Clinical Research, Division Director, General Academic Pediatrics, and Professor of Pediatrics and Clinical and Translational Science
Jack L. Paradise, MD Endowed Professor of Pediatric Research, UPMC Children's Hospital of PittsburghPresident, UPMC Children's Community Pediatrics
MedicalResearch.com: What is the background for this study?
Response: Acute otitis media (AOM) is the most frequently diagnosed illness in children in the United States for which antibiotics are prescribed. Recurrent AOM is the principal indication for tympanostomy-tube placement, the most frequently performed operation in children after the newborn period. Supporting the performance of tympanostomy-tube placement for recurrent acute otitis media has been the commonplace observation, after surgery, of acute otitis media–free periods of varying duration. Counterbalancing this view have been the cost of tympanostomy-tube placement; risks and possible late sequelae of anesthesia in young children; the possible occurrence of refractory tube otorrhea, tube blockage, premature extrusion, or dislocation of the tube into the middle-ear cavity; various structural tympanic membrane sequelae; and the possible development of mild conductive hearing loss. Tempering support for surgery is the progressive reduction in the incidence of acute otitis media that usually accompanies a child’s increasing age.
Previous trials of tympanostomy-tube placement for recurrent acute otitis media, all conducted before the introduction of pneumococcal conjugate vaccine, have given mixed results and were limited, variously, by small sample size, uncertain validity of diagnoses of acute otitis media determining trial eligibility, short periods of follow-up, and substantial attrition of participants. Official recommendations regarding tympanostomy-tube placement for children with recurrent acute otitis media differ — an otolaryngologic guideline recommends the procedure for children with recurrent acute otitis media, provided that middle-ear effusion is present in at least one ear; a contemporaneous pediatric guideline discusses tympanostomy-tube placement as an “option [that] clinicians may offer.”
Given these uncertainties, we undertook the present trial involving children 6 to 35 months of age who had a history of recurrent acute otitis media to determine whether tympanostomy-tube placement, as compared with medical management (comprising episodic antimicrobial treatment, with the option of tympanostomy-tube placement in the event of treatment failure), would result in a greater reduction in the children’s rate of recurrence of acute otitis media during the ensuing 2-year period.


 Dr. Salciccioli[/caption]
Justin Salciccioli, MBBS, MA
Research Fellow in Medicine
[caption id="attachment_57392" align="alignleft" width="150"]
Dr. Salciccioli[/caption]
Justin Salciccioli, MBBS, MA
Research Fellow in Medicine
[caption id="attachment_57392" align="alignleft" width="150"] Dr. Israel[/caption]
Elliot Israel, MD
Professor of Medicine, Harvard Medical School
Pulmonary and Critical Care, Rheumatology, Medicine
Brigham and Women's Hospital
MedicalResearch.com: What is the background for this study?
Response: Asthma attacks account for almost 50% of the cost of asthma care, which costs $80 billion each year in the United States. Asthma is more severe in African-American/Black and Hispanic/Latinx patients, with these groups having double the rates of attacks and hospitalizations as the general population. The PREPARE study is an ongoing national clinical trial for African American/Black and Hispanic/Latinx adults with moderate-to-severe asthma from different U.S. cities in which reporting of asthma control and asthma exacerbations was monitored entirely remotely.
With the arrival of the Covid19 pandemic, several studies suggested that asthma exacerbations may have decreased during the pandemic. However, multiple reports have suggested people were avoiding health services because of the pandemic, making it difficult to tell whether exacerbations truly decreased or whether people were simply avoiding their doctors. This is the first study done to assess asthma exacerbations before and during the pandemic that is unlikely to be impacted by patient healthcare avoidance.
Dr. Israel[/caption]
Elliot Israel, MD
Professor of Medicine, Harvard Medical School
Pulmonary and Critical Care, Rheumatology, Medicine
Brigham and Women's Hospital
MedicalResearch.com: What is the background for this study?
Response: Asthma attacks account for almost 50% of the cost of asthma care, which costs $80 billion each year in the United States. Asthma is more severe in African-American/Black and Hispanic/Latinx patients, with these groups having double the rates of attacks and hospitalizations as the general population. The PREPARE study is an ongoing national clinical trial for African American/Black and Hispanic/Latinx adults with moderate-to-severe asthma from different U.S. cities in which reporting of asthma control and asthma exacerbations was monitored entirely remotely.
With the arrival of the Covid19 pandemic, several studies suggested that asthma exacerbations may have decreased during the pandemic. However, multiple reports have suggested people were avoiding health services because of the pandemic, making it difficult to tell whether exacerbations truly decreased or whether people were simply avoiding their doctors. This is the first study done to assess asthma exacerbations before and during the pandemic that is unlikely to be impacted by patient healthcare avoidance.


 Dr. Jinhee Hur[/caption]
Jinhee Hur, PhD
Research Fellow
Department of Nutrition
Harvard T.H. Chan School of Public Health
Boston, MA 02115
MedicalResearch.com: What is the background for this study?
Response: Early-onset colorectal cancer (EO-CRC, age <50 years at diagnosis) is rapidly rising in the US since the mid-1980s, with an unclear understanding of its etiology and contributors to the rise. Sugar-sweetened beverages (SSBs) exert adverse metabolic repercussions throughout the life course, including insulin resistance and inflammation. Higher SSB intake can induce obesity, which has been linked to risk of EO-CRC. A recent experimental study also suggests that high fructose corn syrup, a primary sweetener in SSBs, may promote colon tumor growth, independent of metabolic dysregulation. In the US, SSB consumption has dramatically increased during the 2nd half of the 20th century, and adolescents and young adults have been the heaviest SSB drinkers across all age groups. Thus, we expect SSBs may be an emerging risk factor for EO-CRC and likely contribute to the rising incidence of EO-CRC.
Dr. Jinhee Hur[/caption]
Jinhee Hur, PhD
Research Fellow
Department of Nutrition
Harvard T.H. Chan School of Public Health
Boston, MA 02115
MedicalResearch.com: What is the background for this study?
Response: Early-onset colorectal cancer (EO-CRC, age <50 years at diagnosis) is rapidly rising in the US since the mid-1980s, with an unclear understanding of its etiology and contributors to the rise. Sugar-sweetened beverages (SSBs) exert adverse metabolic repercussions throughout the life course, including insulin resistance and inflammation. Higher SSB intake can induce obesity, which has been linked to risk of EO-CRC. A recent experimental study also suggests that high fructose corn syrup, a primary sweetener in SSBs, may promote colon tumor growth, independent of metabolic dysregulation. In the US, SSB consumption has dramatically increased during the 2nd half of the 20th century, and adolescents and young adults have been the heaviest SSB drinkers across all age groups. Thus, we expect SSBs may be an emerging risk factor for EO-CRC and likely contribute to the rising incidence of EO-CRC.



 Dr. Ulhas Nair[/caption]
Nishanth Ulhas Nair, Ph.D.
Affiliation: Staff Scientist at Cancer Data Science Laboratory, Center for Cancer Research
National Cancer Institute (NCI), National Institutes of Health (NIH)
Bethesda, Maryland, USA. Date: April 22, 2021
Dr. Raffit Hassan and Dr. Eytan Ruppin at the National Cancer Institute (NCI) are the senior authors of this study.
MedicalResearch.com: What is the background for this study?
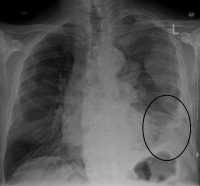
Response: Malignant mesothelioma is an aggressive cancer with limited treatment options and poor prognosis. An in-depth knowledge of genetic, transcriptomic and immunogenic events involved in mesothelioma is critical for successful development of prognostics and therapeutic modalities. In this study we aim to address this by exploring a new large scale patient tumor dataset of 122 mesothelioma patients, called NCI mesothelioma patient data, along with their genomic, transcriptomic, and phenotypic information. Unlike previous large-scale studies which have been focused on malignant pleural mesothelioma patients, our dataset contains an approximately equal representation of malignant pleural and peritoneal mesothelioma patients which allows to identify any differences between them.
Dr. Ulhas Nair[/caption]
Nishanth Ulhas Nair, Ph.D.
Affiliation: Staff Scientist at Cancer Data Science Laboratory, Center for Cancer Research
National Cancer Institute (NCI), National Institutes of Health (NIH)
Bethesda, Maryland, USA. Date: April 22, 2021
Dr. Raffit Hassan and Dr. Eytan Ruppin at the National Cancer Institute (NCI) are the senior authors of this study.
MedicalResearch.com: What is the background for this study?
Response: Malignant mesothelioma is an aggressive cancer with limited treatment options and poor prognosis. An in-depth knowledge of genetic, transcriptomic and immunogenic events involved in mesothelioma is critical for successful development of prognostics and therapeutic modalities. In this study we aim to address this by exploring a new large scale patient tumor dataset of 122 mesothelioma patients, called NCI mesothelioma patient data, along with their genomic, transcriptomic, and phenotypic information. Unlike previous large-scale studies which have been focused on malignant pleural mesothelioma patients, our dataset contains an approximately equal representation of malignant pleural and peritoneal mesothelioma patients which allows to identify any differences between them.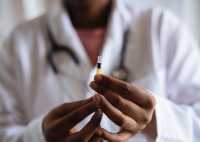
 Dr. Blankson[/caption]
Joel N. Blankson, MD, PhD
Department of Infectious Diseases
Associate Professor
Cellular and Molecular Medicine Program
Johns Hopkins
MedicalResearch.com: What is the background for this study? Which vaccines did you evaluate?
Response: Prior studies from several groups including our own have found T cell cross-recognition of peptides from SARS-CoV-2 and the common cold coronaviruses.
We asked whether as a result of this cross-reactivity, immunization with the SARS-CoV-2 vaccine would also enhance T cell responses to the common cold coronaviruses.
Prior studies also suggested that antibodies elicited from the mRNA vaccines had a reduced ability to neutralize the emerging variants of concern.
Most of the study participants had received the Pfizer vaccine, but a few had received the Moderna vaccine.
Dr. Blankson[/caption]
Joel N. Blankson, MD, PhD
Department of Infectious Diseases
Associate Professor
Cellular and Molecular Medicine Program
Johns Hopkins
MedicalResearch.com: What is the background for this study? Which vaccines did you evaluate?
Response: Prior studies from several groups including our own have found T cell cross-recognition of peptides from SARS-CoV-2 and the common cold coronaviruses.
We asked whether as a result of this cross-reactivity, immunization with the SARS-CoV-2 vaccine would also enhance T cell responses to the common cold coronaviruses.
Prior studies also suggested that antibodies elicited from the mRNA vaccines had a reduced ability to neutralize the emerging variants of concern.
Most of the study participants had received the Pfizer vaccine, but a few had received the Moderna vaccine. 

 Dr. McPeek Hinz[/caption]
Eugenia McPeek Hinz MD MS FAMIA
Associate CMIO - DHTS
Duke University Health System
MedicalResearch.com: What is the background for this study?
Response: Clinician burnout rates have hovered around 50% for much of the past decade. Burnout is a significant concern in healthcare for its effects on care givers and associated downstream adverse implications on patient care for quality and safety. The ubiquitous presence of Electronic Health Records (EHR) along with the increased clerical components and after hours use has been a significant concern for contributing to provider burnout.
Dr. McPeek Hinz[/caption]
Eugenia McPeek Hinz MD MS FAMIA
Associate CMIO - DHTS
Duke University Health System
MedicalResearch.com: What is the background for this study?
Response: Clinician burnout rates have hovered around 50% for much of the past decade. Burnout is a significant concern in healthcare for its effects on care givers and associated downstream adverse implications on patient care for quality and safety. The ubiquitous presence of Electronic Health Records (EHR) along with the increased clerical components and after hours use has been a significant concern for contributing to provider burnout. 
 Dr. Dunietz[/caption]
Galit Levi Dunietz MPH, PhD
Assistant Professor
Dr. Dunietz[/caption]
Galit Levi Dunietz MPH, PhD
Assistant Professor
 Dr. Braley[/caption]
Dr. Braley[/caption]






