Author Interviews, COVID -19 Coronavirus, Occupational Health, Weight Research / 01.08.2021
Newtopia: Successful Weight Loss During Covid-19 with a Virtual Habit Change Provider
MedicalResearch.com Interview with:
 Jeff Ruby, JD, MBA, Founder and Chief Executive Officer
Leonard Fensterheim, MPH
Vice President of Analytics
MedicalResearch.com: What is the background for this study? What are common weight-change findings during the pandemic?
Obesity has been linked to increased risk of serious complications and the need for costly medical utilization – all of which has been exacerbated by the COVID-19 pandemic. There has been an increase of imposed restrictions that impact healthy lifestyles – the closing of gyms as an example – leading to additional stress and the complete disruption of daily lives. It’s no surprise that many people have gained weight since the beginning of the pandemic.
According to the Centers for Disease Control and Prevention (CDC), before the pandemic about 40% of Americans had obesity in the United States. This was already an alarming figure, but given that the American Psychological Association found that 42% of U.S. adults report undesired weight gain, with an average gain of 29 lbs. since the start of the pandemic, we expect that percentage has continued to grow.
Against this backdrop, Newtopia sought to evaluate the impact of a guided habit change program on weight loss for 12 months during the COVID-19 pandemic.
Method:
Jeff Ruby, JD, MBA, Founder and Chief Executive Officer
Leonard Fensterheim, MPH
Vice President of Analytics
MedicalResearch.com: What is the background for this study? What are common weight-change findings during the pandemic?
Obesity has been linked to increased risk of serious complications and the need for costly medical utilization – all of which has been exacerbated by the COVID-19 pandemic. There has been an increase of imposed restrictions that impact healthy lifestyles – the closing of gyms as an example – leading to additional stress and the complete disruption of daily lives. It’s no surprise that many people have gained weight since the beginning of the pandemic.
According to the Centers for Disease Control and Prevention (CDC), before the pandemic about 40% of Americans had obesity in the United States. This was already an alarming figure, but given that the American Psychological Association found that 42% of U.S. adults report undesired weight gain, with an average gain of 29 lbs. since the start of the pandemic, we expect that percentage has continued to grow.
Against this backdrop, Newtopia sought to evaluate the impact of a guided habit change program on weight loss for 12 months during the COVID-19 pandemic.
Method:
 Jeff Ruby, JD, MBA, Founder and Chief Executive Officer
Leonard Fensterheim, MPH
Vice President of Analytics
MedicalResearch.com: What is the background for this study? What are common weight-change findings during the pandemic?
Obesity has been linked to increased risk of serious complications and the need for costly medical utilization – all of which has been exacerbated by the COVID-19 pandemic. There has been an increase of imposed restrictions that impact healthy lifestyles – the closing of gyms as an example – leading to additional stress and the complete disruption of daily lives. It’s no surprise that many people have gained weight since the beginning of the pandemic.
According to the Centers for Disease Control and Prevention (CDC), before the pandemic about 40% of Americans had obesity in the United States. This was already an alarming figure, but given that the American Psychological Association found that 42% of U.S. adults report undesired weight gain, with an average gain of 29 lbs. since the start of the pandemic, we expect that percentage has continued to grow.
Against this backdrop, Newtopia sought to evaluate the impact of a guided habit change program on weight loss for 12 months during the COVID-19 pandemic.
Method:
Jeff Ruby, JD, MBA, Founder and Chief Executive Officer
Leonard Fensterheim, MPH
Vice President of Analytics
MedicalResearch.com: What is the background for this study? What are common weight-change findings during the pandemic?
Obesity has been linked to increased risk of serious complications and the need for costly medical utilization – all of which has been exacerbated by the COVID-19 pandemic. There has been an increase of imposed restrictions that impact healthy lifestyles – the closing of gyms as an example – leading to additional stress and the complete disruption of daily lives. It’s no surprise that many people have gained weight since the beginning of the pandemic.
According to the Centers for Disease Control and Prevention (CDC), before the pandemic about 40% of Americans had obesity in the United States. This was already an alarming figure, but given that the American Psychological Association found that 42% of U.S. adults report undesired weight gain, with an average gain of 29 lbs. since the start of the pandemic, we expect that percentage has continued to grow.
Against this backdrop, Newtopia sought to evaluate the impact of a guided habit change program on weight loss for 12 months during the COVID-19 pandemic.
Method:
- This was a retrospective study that looked at 1436 participants who began participating in the Newtopia experience in early 2020.
- This analysis focused on weight change and was restricted to those participants with a body mass index >
- 52% of participants were female, and the average age of the total study population was 46.5 years old (±10.6).
- The percentage of participants with a 4.3% weight reduction after 12 months was assessed. This has been shown to be associated with meaningful reduction in healthcare costs.
- The average weight loss and the percentage BMI decrease was also assessed.
- 77% of participants lost weight.
- 44% of participants had a weight loss of >3%.
- Average weight loss was 4.2% (p<.0001).
- 22% of obese participants dropped a BMI category.




 Dr. Blumenthal[/caption]
Kimberly G. Blumenthal, MD, MSc
Massachusetts General Hospital
The Mongan Institute
Boston, MA 02114
[caption id="attachment_57828" align="alignleft" width="100"]
Dr. Blumenthal[/caption]
Kimberly G. Blumenthal, MD, MSc
Massachusetts General Hospital
The Mongan Institute
Boston, MA 02114
[caption id="attachment_57828" align="alignleft" width="100"] Dr. Krantz[/caption]
Matthew S. Krantz, MD
Division of Allergy, Pulmonary and Critical Care Medicine
Department of Medicine,
Vanderbilt University Medical Center,
Nashville, Tennessee
MedicalResearch.com: What is the background for this study?
Response: During the initial COVID-19 vaccine campaign with healthcare workers in December 2020, there was an unexpected higher than anticipated rate of immediate allergic reactions after Pfizer and Moderna mRNA vaccines. This prompted both patient and provider concerns, particularly in those with underlying allergic histories, on the associated risks for immediate allergic reactions with the mRNA vaccines.
Because of the significantly improved effectiveness of two doses of an mRNA vaccine compared to one dose, it was important to determine if those who experienced immediate allergic reaction symptoms after their first dose could go on to tolerate a second dose safely.
Dr. Krantz[/caption]
Matthew S. Krantz, MD
Division of Allergy, Pulmonary and Critical Care Medicine
Department of Medicine,
Vanderbilt University Medical Center,
Nashville, Tennessee
MedicalResearch.com: What is the background for this study?
Response: During the initial COVID-19 vaccine campaign with healthcare workers in December 2020, there was an unexpected higher than anticipated rate of immediate allergic reactions after Pfizer and Moderna mRNA vaccines. This prompted both patient and provider concerns, particularly in those with underlying allergic histories, on the associated risks for immediate allergic reactions with the mRNA vaccines.
Because of the significantly improved effectiveness of two doses of an mRNA vaccine compared to one dose, it was important to determine if those who experienced immediate allergic reaction symptoms after their first dose could go on to tolerate a second dose safely. 


 Dr. Correa[/caption]
Andres F. Correa, MD
Assistant Professor
Department of Surgical Oncology, and
[caption id="attachment_57815" align="alignleft" width="150"]
Dr. Correa[/caption]
Andres F. Correa, MD
Assistant Professor
Department of Surgical Oncology, and
[caption id="attachment_57815" align="alignleft" width="150"] Dr. Bernstein[/caption]
Adrien Bernstein, MD
Second Year Urologic Oncology Fellow
Fox Chase Cancer Center
MedicalResearch.com: What is the background for this study?
Response: Unfortunately, it has been well-established that historically Black Americans experience increased cancer specific mortality compared to white patients. In prostate cancer specifically studies have shown that when access to care is equitable this gap resolves. This suggests that biological factors are not driving these differences but rather the result of the complex interplay of social determinants and systemic inequities in our healthcare system.
Early in the pandemic, multiple studies demonstrated that minority communities disproportionately shouldered poor COVID-19 outcomes. On March 13th 2020, the American College of Surgeons recommended against elective procedures; however, the definition of an elective oncologic case was left to the discretion of the provider. As prostate cancer treatment can be safely deferred up to a year follow diagnosis, management of prostate cancer during the initial lockdown period of the COVID-19 Pandemic provided a useful analysis of the differential restrictions placed on non-emergent health care during the Pandemic.
Dr. Bernstein[/caption]
Adrien Bernstein, MD
Second Year Urologic Oncology Fellow
Fox Chase Cancer Center
MedicalResearch.com: What is the background for this study?
Response: Unfortunately, it has been well-established that historically Black Americans experience increased cancer specific mortality compared to white patients. In prostate cancer specifically studies have shown that when access to care is equitable this gap resolves. This suggests that biological factors are not driving these differences but rather the result of the complex interplay of social determinants and systemic inequities in our healthcare system.
Early in the pandemic, multiple studies demonstrated that minority communities disproportionately shouldered poor COVID-19 outcomes. On March 13th 2020, the American College of Surgeons recommended against elective procedures; however, the definition of an elective oncologic case was left to the discretion of the provider. As prostate cancer treatment can be safely deferred up to a year follow diagnosis, management of prostate cancer during the initial lockdown period of the COVID-19 Pandemic provided a useful analysis of the differential restrictions placed on non-emergent health care during the Pandemic.
 MedicalResearch.com Interview with:
Eleonora Leucci, Ph.D Assistant Professor
Laboratory for RNA Cancer Biology
Department of Oncology
KU Leuven
MedicalResearch.com: What is the background for this study?
Response: Back in 2016, while I was characterising the RNA SAMMSON as essential for mitochondrial translation in melanoma, I noticed that its inhibition was causing cell death across a large spectrum of melanoma cell lines and models, irrespectively of their genetic background and cell state. At that time I still did not know why the effect was so pronounced on melanoma cells, but I knew that antibiotics of the tetracycline family could also block mitochondrial translation and I thought about repurposing them to treat melanoma.
MedicalResearch.com Interview with:
Eleonora Leucci, Ph.D Assistant Professor
Laboratory for RNA Cancer Biology
Department of Oncology
KU Leuven
MedicalResearch.com: What is the background for this study?
Response: Back in 2016, while I was characterising the RNA SAMMSON as essential for mitochondrial translation in melanoma, I noticed that its inhibition was causing cell death across a large spectrum of melanoma cell lines and models, irrespectively of their genetic background and cell state. At that time I still did not know why the effect was so pronounced on melanoma cells, but I knew that antibiotics of the tetracycline family could also block mitochondrial translation and I thought about repurposing them to treat melanoma.

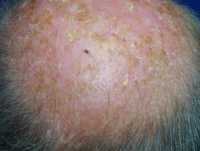






 Dr. Strauss[/caption]
David Strauss, MD, PhD
Director, Division of Applied Regulatory Science
[caption id="attachment_57763" align="alignleft" width="150"]
Dr. Strauss[/caption]
David Strauss, MD, PhD
Director, Division of Applied Regulatory Science
[caption id="attachment_57763" align="alignleft" width="150"] Dr. Keire[/caption]
David Keire, PhD
Director, Office of Testing and Research
U.S. Food and Drug Administration
Center for Drug Evaluation and Research
MedicalResearch.com: What is the background for this study?
Response: In 2019, the US Food and Drug Administration (FDA) received a citizen petition indicating that ranitidine, a widely used prescription and over-the-counter drug, contained the probable human carcinogen N-nitrosodimethylamine (NDMA). In addition, the petitioner proposed that ranitidine could convert to NDMA in humans; however, this was based on a small clinical study with limitations and an in vitro study that included high level of supplemental nitrite. In response, the FDA immediately alerted the public and began an investigation.
The FDA’s initial research found that the procedures previously used to quantify NDMA were not appropriate for assessing its presence in ranitidine, owing to the use of high temperatures that could convert ranitidine to NDMA during that analysis. New lower-temperature analytical methods found that the amounts of NDMA contained in ranitidine products were 3,000-fold lower than those reported in the citizen petition; however, these lower amounts of NDMA were still above the FDA-acceptable level and could increase over time, prompting the FDA to request the market withdrawal of ranitidine products.
The FDA noted, however, that if ranitidine products could be manufactured to control NDMA amounts, they could be allowed back on the market—but additional information would first be needed to understand whether NDMA could form in vivo from ranitidine in humans.
Dr. Keire[/caption]
David Keire, PhD
Director, Office of Testing and Research
U.S. Food and Drug Administration
Center for Drug Evaluation and Research
MedicalResearch.com: What is the background for this study?
Response: In 2019, the US Food and Drug Administration (FDA) received a citizen petition indicating that ranitidine, a widely used prescription and over-the-counter drug, contained the probable human carcinogen N-nitrosodimethylamine (NDMA). In addition, the petitioner proposed that ranitidine could convert to NDMA in humans; however, this was based on a small clinical study with limitations and an in vitro study that included high level of supplemental nitrite. In response, the FDA immediately alerted the public and began an investigation.
The FDA’s initial research found that the procedures previously used to quantify NDMA were not appropriate for assessing its presence in ranitidine, owing to the use of high temperatures that could convert ranitidine to NDMA during that analysis. New lower-temperature analytical methods found that the amounts of NDMA contained in ranitidine products were 3,000-fold lower than those reported in the citizen petition; however, these lower amounts of NDMA were still above the FDA-acceptable level and could increase over time, prompting the FDA to request the market withdrawal of ranitidine products.
The FDA noted, however, that if ranitidine products could be manufactured to control NDMA amounts, they could be allowed back on the market—but additional information would first be needed to understand whether NDMA could form in vivo from ranitidine in humans.



 Dr, Ferguson[/caption]
Michael Ferguson, PhD
Instructor in Neurology | Harvard Medical School
Lecturer on Neurospirituality | Harvard Divinity School
Center for Brain Circuit Therapeutics
Brigham and Women’s Hospital
MedicalResearch.com: What is the background for this study?
Response: Over 80% of the global population consider themselves religious with even more identifying as spiritual, but the neural substrates of spirituality and religiosity remain unresolved.
MedicalResearch.com: What are the main findings? Where is this circuit located in the brain? What other effects does this circuit control or influence?
Response: We found that brain lesions associated with self-reported spirituality map to a human brain circuit centered on the periaqueductal grey.
Dr, Ferguson[/caption]
Michael Ferguson, PhD
Instructor in Neurology | Harvard Medical School
Lecturer on Neurospirituality | Harvard Divinity School
Center for Brain Circuit Therapeutics
Brigham and Women’s Hospital
MedicalResearch.com: What is the background for this study?
Response: Over 80% of the global population consider themselves religious with even more identifying as spiritual, but the neural substrates of spirituality and religiosity remain unresolved.
MedicalResearch.com: What are the main findings? Where is this circuit located in the brain? What other effects does this circuit control or influence?
Response: We found that brain lesions associated with self-reported spirituality map to a human brain circuit centered on the periaqueductal grey.
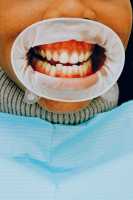
 Dane Kim[/caption]
Dane Kim, Dental Student
University of Pennsylvania School of Dental Medicine
MedicalResearch.com: What is the background for this study?
Response: This large study was inspired, in part, by a previous publication, Gustatory Function After Third Molar Extraction (Shafer et al. 1999), which examined the effect of third molar extractions on human taste function. Their work was based upon more severe extractions and followed patients only up to six months after their surgery. Studies examining taste function over a longer period, i.e., beyond six months from the surgery, were non-existent.
The Smell and Taste Center of Penn Medicine, which is the only center of its type in the United States, has a large unique database of patients who have been thoroughly tested for both smell and taste function. This provided us with the opportunity to compare data from hundreds of persons who had previously received third-molar extractions to those who had not received such extractions. Importantly, the extracts had occurred years before thee taste testing.
Dane Kim[/caption]
Dane Kim, Dental Student
University of Pennsylvania School of Dental Medicine
MedicalResearch.com: What is the background for this study?
Response: This large study was inspired, in part, by a previous publication, Gustatory Function After Third Molar Extraction (Shafer et al. 1999), which examined the effect of third molar extractions on human taste function. Their work was based upon more severe extractions and followed patients only up to six months after their surgery. Studies examining taste function over a longer period, i.e., beyond six months from the surgery, were non-existent.
The Smell and Taste Center of Penn Medicine, which is the only center of its type in the United States, has a large unique database of patients who have been thoroughly tested for both smell and taste function. This provided us with the opportunity to compare data from hundreds of persons who had previously received third-molar extractions to those who had not received such extractions. Importantly, the extracts had occurred years before thee taste testing. 
 Dr. Kelley[/caption]
Mireille E. Kelley Ph.D.
Staff Consultant for Engineering Systems Inc.
MedicalResearch.com: What is the background for this study?
Response: Youth and high school football players can sustain hundreds of head impacts in a season and while most of these impacts do not result in any signs or symptoms of concussion, there is concern that these repetitive subconcussive impacts may have a negative effect on the brain.
The results of this study are part of an NIH-funded study to understand the effects of subconcussive head impact exposure on imaging data collected at pre- and post-season time points. The present study leveraged the longitudinal data that was collected in the parent study to understand how head impact exposure changes among athletes from season to season and how that relates to changes measured from imaging.
Dr. Kelley[/caption]
Mireille E. Kelley Ph.D.
Staff Consultant for Engineering Systems Inc.
MedicalResearch.com: What is the background for this study?
Response: Youth and high school football players can sustain hundreds of head impacts in a season and while most of these impacts do not result in any signs or symptoms of concussion, there is concern that these repetitive subconcussive impacts may have a negative effect on the brain.
The results of this study are part of an NIH-funded study to understand the effects of subconcussive head impact exposure on imaging data collected at pre- and post-season time points. The present study leveraged the longitudinal data that was collected in the parent study to understand how head impact exposure changes among athletes from season to season and how that relates to changes measured from imaging.



 Dr. Els Broens[/caption]
Els M. Broens DVM, PhD, Dipl. ECVM, EBVS
European Veteirnary Specialist in Veterinary Microbiology
Associate Professor / Director VMDC
Department Biomolecular Health Sciences (Clinical Infectiology)
Faculty of Veterinary Medicine | Utrecht University
MedicalResearch.com: What is the background for this study?
Response: Several events have demonstrated that SARS-CoV-2 can infect animals, felines and mustelids in particular. In companion animals these are currently considered to be incidents with a negligible risk for public health since the main force of the pandemic is transmission between humans. However, it is urgent to understand the potential risk of animal infections for public health in the later stages of the pandemic when SARS-CoV-2 transmission between humans is greatly reduced and a virus reservoir in animals could become more important.
Incidental cases have shown that COVID-19 positive owners can transmit SARS-CoV-2 to their dog or cat. The close contact between owners and their dogs and cats and the interaction between dogs and cats from different households raises questions about the risk for pets to contract the disease and also about role of these animals in the transmission of SARS-CoV-2.
Dr. Els Broens[/caption]
Els M. Broens DVM, PhD, Dipl. ECVM, EBVS
European Veteirnary Specialist in Veterinary Microbiology
Associate Professor / Director VMDC
Department Biomolecular Health Sciences (Clinical Infectiology)
Faculty of Veterinary Medicine | Utrecht University
MedicalResearch.com: What is the background for this study?
Response: Several events have demonstrated that SARS-CoV-2 can infect animals, felines and mustelids in particular. In companion animals these are currently considered to be incidents with a negligible risk for public health since the main force of the pandemic is transmission between humans. However, it is urgent to understand the potential risk of animal infections for public health in the later stages of the pandemic when SARS-CoV-2 transmission between humans is greatly reduced and a virus reservoir in animals could become more important.
Incidental cases have shown that COVID-19 positive owners can transmit SARS-CoV-2 to their dog or cat. The close contact between owners and their dogs and cats and the interaction between dogs and cats from different households raises questions about the risk for pets to contract the disease and also about role of these animals in the transmission of SARS-CoV-2.




 Scott Gray[/caption]
Scott Gray: Founder and CEO of Clincierge, the global leader in patient support services for clinical trials. With a team of patient coordinators around the world, Clincierge helps patients and their caregivers navigate the logistics of clinical trial participation, including prepaid air travel, ground transportation, and lodging as well as rapid reimbursements, translation and interpretation services, and individual solutions for trial participants in remote locations or with complex medical needs. For more information, visit clincierge.com.
MedicalResearch.com: What is the mission of Clincierge?
Scott Gray[/caption]
Scott Gray: Founder and CEO of Clincierge, the global leader in patient support services for clinical trials. With a team of patient coordinators around the world, Clincierge helps patients and their caregivers navigate the logistics of clinical trial participation, including prepaid air travel, ground transportation, and lodging as well as rapid reimbursements, translation and interpretation services, and individual solutions for trial participants in remote locations or with complex medical needs. For more information, visit clincierge.com.
MedicalResearch.com: What is the mission of Clincierge?
