MedicalResearch.com Interview with:
[caption id="attachment_44899" align="alignleft" width="200"]

Dr. Manon Eckhardt[/caption]
Manon Eckhardt, PhD
Gladstone Institutes
The Quantitative Biosciences Institute
University of California San Francisco
MedicalResearch.com: What is the background for this study? What are the main findings?
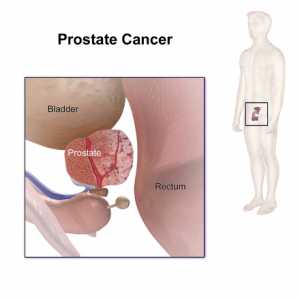
Response: Infection with Human Papillomavirus (HPV) causes 5% of all cancers worldwide, including cervical cancer and an increasing number of head and neck cancers. Most cancers are caused by mutations in genes, leading to the production of malfunctioning proteins that result in unconstrained cell division. However, certain viruses like HPV can cause cancer without introducing mutations.
In this study, we compared cancers of the same type (
i.e. head and neck) that are caused by either mutation or virus infection to identify important processes that are dysregulated in both subsets. We hypothesized that identifying which proteins the virus binds can lead the way to prioritize which of the proteins and cellular processes (pathways) that are affected in cancer cells are most important. To do this, we identified the complete set of human proteins that interact with HPV. We next determined genes that were more frequently mutated in non-viral cancers, and combined both data sets. The proteins we find to be both binding to HPV and mutated in non-viral cancers will be potential targets for new, more specific drug development, and help better understand the development of head and neck cancer.
From the many pathways we identified in this study, we highlighted two pathways with further mechanistic studies: the oxidative stress response, which helps cancer cells survive, as well as a pathway that allows the cancer to spread to other parts of the body.