Author Interviews, Breast Cancer, Journal Clinical Oncology, MRI, Yale / 02.12.2015
MRI May Detect More Early Contralateral Breast Cancer But Not Prevent Advanced Disease
[caption id="attachment_19717" align="alignleft" width="125"] Dr. Wang[/caption]
MedicalResearch.com Interview with:
Shiyi Wang, MD, PhD
Assistant Professor of Epidemiology (Chronic Diseases)
Yale School of Public Health
Medical Research: What is the background for this study?
Dr. Wang: As magnetic resonance imaging (MRI) of the breast has become part of medical care, there is increasing concern that this highly sensitive test might identify health problems that otherwise would not have had an impact on the patient – so called “overdiagnosis”. However, even if MRI use leads to overdiagnosis, the main “theoretical” benefit of early detection by MRI is to prevent future advanced diseases, the prognosis of which is deleterious. A systematic literature review found that, compared to mammography and/or ultrasound, MRI had a 4.1% incremental contralateral breast cancer (breast cancer in the opposite breast) detection rate. At this point, the impact of MRI on long-term contralateral breast cancer outcomes remains unclear.
Medical Research: What are the main findings?
Dr. Wang: Analyzing the Surveillance, Epidemiology, and End Results-Medicare dataset, we compared two groups of women who had breast cancer (one group receiving an MRI, and the other not) in terms of stage-specific contralateral breast cancer occurrences. We found that after five years, the MRI group had a higher detection rate of cancer in the opposite breast than the non-MRI group (7.2 % vs. 4.0%). Specifically, MRI use approximately doubles the detection rate of early stage contralateral breast cancer, but does not decrease the incidence of advanced stage contralateral breast cancer occurrences after a 5-year follow-up. Our results indicate that nearly half of additional breast cancers detected by the preoperative MRI were overdiagnosed, which means that many of these occult cancers not detected by MRI would not have become clinically evident over the subsequent 5 years. There was no evidence that MRI use was benefiting women because the rate of advanced cancer was similar in the MRI and the non-MRI groups.
Dr. Wang[/caption]
MedicalResearch.com Interview with:
Shiyi Wang, MD, PhD
Assistant Professor of Epidemiology (Chronic Diseases)
Yale School of Public Health
Medical Research: What is the background for this study?
Dr. Wang: As magnetic resonance imaging (MRI) of the breast has become part of medical care, there is increasing concern that this highly sensitive test might identify health problems that otherwise would not have had an impact on the patient – so called “overdiagnosis”. However, even if MRI use leads to overdiagnosis, the main “theoretical” benefit of early detection by MRI is to prevent future advanced diseases, the prognosis of which is deleterious. A systematic literature review found that, compared to mammography and/or ultrasound, MRI had a 4.1% incremental contralateral breast cancer (breast cancer in the opposite breast) detection rate. At this point, the impact of MRI on long-term contralateral breast cancer outcomes remains unclear.
Medical Research: What are the main findings?
Dr. Wang: Analyzing the Surveillance, Epidemiology, and End Results-Medicare dataset, we compared two groups of women who had breast cancer (one group receiving an MRI, and the other not) in terms of stage-specific contralateral breast cancer occurrences. We found that after five years, the MRI group had a higher detection rate of cancer in the opposite breast than the non-MRI group (7.2 % vs. 4.0%). Specifically, MRI use approximately doubles the detection rate of early stage contralateral breast cancer, but does not decrease the incidence of advanced stage contralateral breast cancer occurrences after a 5-year follow-up. Our results indicate that nearly half of additional breast cancers detected by the preoperative MRI were overdiagnosed, which means that many of these occult cancers not detected by MRI would not have become clinically evident over the subsequent 5 years. There was no evidence that MRI use was benefiting women because the rate of advanced cancer was similar in the MRI and the non-MRI groups.
 Dr. Wang[/caption]
MedicalResearch.com Interview with:
Shiyi Wang, MD, PhD
Assistant Professor of Epidemiology (Chronic Diseases)
Yale School of Public Health
Medical Research: What is the background for this study?
Dr. Wang: As magnetic resonance imaging (MRI) of the breast has become part of medical care, there is increasing concern that this highly sensitive test might identify health problems that otherwise would not have had an impact on the patient – so called “overdiagnosis”. However, even if MRI use leads to overdiagnosis, the main “theoretical” benefit of early detection by MRI is to prevent future advanced diseases, the prognosis of which is deleterious. A systematic literature review found that, compared to mammography and/or ultrasound, MRI had a 4.1% incremental contralateral breast cancer (breast cancer in the opposite breast) detection rate. At this point, the impact of MRI on long-term contralateral breast cancer outcomes remains unclear.
Medical Research: What are the main findings?
Dr. Wang: Analyzing the Surveillance, Epidemiology, and End Results-Medicare dataset, we compared two groups of women who had breast cancer (one group receiving an MRI, and the other not) in terms of stage-specific contralateral breast cancer occurrences. We found that after five years, the MRI group had a higher detection rate of cancer in the opposite breast than the non-MRI group (7.2 % vs. 4.0%). Specifically, MRI use approximately doubles the detection rate of early stage contralateral breast cancer, but does not decrease the incidence of advanced stage contralateral breast cancer occurrences after a 5-year follow-up. Our results indicate that nearly half of additional breast cancers detected by the preoperative MRI were overdiagnosed, which means that many of these occult cancers not detected by MRI would not have become clinically evident over the subsequent 5 years. There was no evidence that MRI use was benefiting women because the rate of advanced cancer was similar in the MRI and the non-MRI groups.
Dr. Wang[/caption]
MedicalResearch.com Interview with:
Shiyi Wang, MD, PhD
Assistant Professor of Epidemiology (Chronic Diseases)
Yale School of Public Health
Medical Research: What is the background for this study?
Dr. Wang: As magnetic resonance imaging (MRI) of the breast has become part of medical care, there is increasing concern that this highly sensitive test might identify health problems that otherwise would not have had an impact on the patient – so called “overdiagnosis”. However, even if MRI use leads to overdiagnosis, the main “theoretical” benefit of early detection by MRI is to prevent future advanced diseases, the prognosis of which is deleterious. A systematic literature review found that, compared to mammography and/or ultrasound, MRI had a 4.1% incremental contralateral breast cancer (breast cancer in the opposite breast) detection rate. At this point, the impact of MRI on long-term contralateral breast cancer outcomes remains unclear.
Medical Research: What are the main findings?
Dr. Wang: Analyzing the Surveillance, Epidemiology, and End Results-Medicare dataset, we compared two groups of women who had breast cancer (one group receiving an MRI, and the other not) in terms of stage-specific contralateral breast cancer occurrences. We found that after five years, the MRI group had a higher detection rate of cancer in the opposite breast than the non-MRI group (7.2 % vs. 4.0%). Specifically, MRI use approximately doubles the detection rate of early stage contralateral breast cancer, but does not decrease the incidence of advanced stage contralateral breast cancer occurrences after a 5-year follow-up. Our results indicate that nearly half of additional breast cancers detected by the preoperative MRI were overdiagnosed, which means that many of these occult cancers not detected by MRI would not have become clinically evident over the subsequent 5 years. There was no evidence that MRI use was benefiting women because the rate of advanced cancer was similar in the MRI and the non-MRI groups.

 Kevin Bieniek[/caption]
MedicalResearch.com Interview with:
Kevin Bieniek B.Sc.
Biology and Psychology
Neuroscience researcher
Mayo Clinic’s campus in Florida.
Medical Research: What is the background for this study? What are the main findings?
Response: Chronic traumatic encephalopathy (CTE) is a progressive neurodegenerative disorder linked to repetitive traumatic brain injury often sustained through contact sports and military blast exposure. While CTE was first described in boxers in the 1920s, to date many descriptions of CTE have been made in high-profile professional athletes, but the frequency of Chronic traumatic encephalopathy pathology in athletes with more modest contact sports participation is unknown. For this study, researchers at the Mayo Clinic in Jacksonville, FL examined the Mayo Clinic Brain Bank, one of the largest brain banks of neurodegenerative diseases. In searching through medical records of over 1,700 patients, 66 individuals with clinically-documented contact sports participation were identified. Of these 66 former athletes, 21 or 32% had pathologic changes in their brains consistent with CTE. By comparison, none of 198 control individuals that did not have contact sports documentation in their medical records (including 66 women) had CTE pathology. These results have been recently published in the December issue of the journal Acta Neuropathologica <<hyperlink:
Kevin Bieniek[/caption]
MedicalResearch.com Interview with:
Kevin Bieniek B.Sc.
Biology and Psychology
Neuroscience researcher
Mayo Clinic’s campus in Florida.
Medical Research: What is the background for this study? What are the main findings?
Response: Chronic traumatic encephalopathy (CTE) is a progressive neurodegenerative disorder linked to repetitive traumatic brain injury often sustained through contact sports and military blast exposure. While CTE was first described in boxers in the 1920s, to date many descriptions of CTE have been made in high-profile professional athletes, but the frequency of Chronic traumatic encephalopathy pathology in athletes with more modest contact sports participation is unknown. For this study, researchers at the Mayo Clinic in Jacksonville, FL examined the Mayo Clinic Brain Bank, one of the largest brain banks of neurodegenerative diseases. In searching through medical records of over 1,700 patients, 66 individuals with clinically-documented contact sports participation were identified. Of these 66 former athletes, 21 or 32% had pathologic changes in their brains consistent with CTE. By comparison, none of 198 control individuals that did not have contact sports documentation in their medical records (including 66 women) had CTE pathology. These results have been recently published in the December issue of the journal Acta Neuropathologica <<hyperlink:  Dr. Peterson[/caption]
MedicalResearch.com Interview with:
Mark D. Peterson, Ph.D., M.S.
University of Michigan, Medicine
Department of Physical Medicine and Rehabilitation
Ann Arbor, MI
Medical Research: What is the background for this study? What are the main findings?
Dr. Peterson: Cerebral palsy (CP) is a neurodevelopmental condition caused by a disturbance to the developing fetal or infant brain. While the incidence of CP has remained stable in recent years, the mortality rate of children with Cerebral palsy has declined, suggesting that adults with Cerebral palsy represent a growing population whose healthcare needs are poorly understood. More than half of children with Cerebral palsy are independently mobile at 8 years of age; however, a large proportion lose mobility in adulthood. These declines are attributed to pain, fatigue, and muscle weakness, and result in chronic inactivity and accelerated aging. Despite this, there have been virtually no specific surveillance efforts or even epidemiologic studies to examine the prevalence of lifestyle-related chronic diseases in adults with Cerebral palsy. Therefore, the purpose of this study was to examine estimates of chronic conditions in a large, U.S. population-representative sample of adults with CP (n=1,015 fromthe Medical Expenditure Panel Survey (MEPS) (2002-2010). We demonstrated that adults with cerebral palsy had significantly greater estimates of chronic diseases, including diabetes, asthma, hypertension and other heart conditions, stroke, emphysema, joint pain, and arthritis as compared with adults without Cerebral palsy.
Dr. Peterson[/caption]
MedicalResearch.com Interview with:
Mark D. Peterson, Ph.D., M.S.
University of Michigan, Medicine
Department of Physical Medicine and Rehabilitation
Ann Arbor, MI
Medical Research: What is the background for this study? What are the main findings?
Dr. Peterson: Cerebral palsy (CP) is a neurodevelopmental condition caused by a disturbance to the developing fetal or infant brain. While the incidence of CP has remained stable in recent years, the mortality rate of children with Cerebral palsy has declined, suggesting that adults with Cerebral palsy represent a growing population whose healthcare needs are poorly understood. More than half of children with Cerebral palsy are independently mobile at 8 years of age; however, a large proportion lose mobility in adulthood. These declines are attributed to pain, fatigue, and muscle weakness, and result in chronic inactivity and accelerated aging. Despite this, there have been virtually no specific surveillance efforts or even epidemiologic studies to examine the prevalence of lifestyle-related chronic diseases in adults with Cerebral palsy. Therefore, the purpose of this study was to examine estimates of chronic conditions in a large, U.S. population-representative sample of adults with CP (n=1,015 fromthe Medical Expenditure Panel Survey (MEPS) (2002-2010). We demonstrated that adults with cerebral palsy had significantly greater estimates of chronic diseases, including diabetes, asthma, hypertension and other heart conditions, stroke, emphysema, joint pain, and arthritis as compared with adults without Cerebral palsy.
 Dr. Ratanawongsa[/caption]
MedicalResearch.com Interview with:
Neda Ratanawongsa, MD, MPH
CMIO for CareLinkSF
Associate Professor, Division of General Internal Medicine
UCSF Center for Vulnerable Populations
Physician, Richard H. Fine People's Clinic (RHPC)
San Francisco, CA 94110
Medical Research: What is the background for this study?
Dr. Ratanawongsa: Many people are concerned about the growing intrusion of computers into the patient-provider relationship. Touted as systems that will make care safer and more cost-effective, electronic health records (EHRs) have proliferated rapidly across the country, fueled by HITECH funding. However, some health care professionals feel like computers keep them from connecting with their patients. Also prior research has shown that computer use can change communication in the exam room and shift agenda from patients' concerns toward medical talk.
Safety net patients already face communication barriers in routine care, particularly language and literacy barriers. Although EHRs could help improve care and communication with these vulnerable patients by helping clinicians fill in the gaps (e.g., what happened in the ED, what medication were you given by that specialist), EHRs could also worsen communication by drawing clinicians' focus away from patients during visits.
Dr. Ratanawongsa[/caption]
MedicalResearch.com Interview with:
Neda Ratanawongsa, MD, MPH
CMIO for CareLinkSF
Associate Professor, Division of General Internal Medicine
UCSF Center for Vulnerable Populations
Physician, Richard H. Fine People's Clinic (RHPC)
San Francisco, CA 94110
Medical Research: What is the background for this study?
Dr. Ratanawongsa: Many people are concerned about the growing intrusion of computers into the patient-provider relationship. Touted as systems that will make care safer and more cost-effective, electronic health records (EHRs) have proliferated rapidly across the country, fueled by HITECH funding. However, some health care professionals feel like computers keep them from connecting with their patients. Also prior research has shown that computer use can change communication in the exam room and shift agenda from patients' concerns toward medical talk.
Safety net patients already face communication barriers in routine care, particularly language and literacy barriers. Although EHRs could help improve care and communication with these vulnerable patients by helping clinicians fill in the gaps (e.g., what happened in the ED, what medication were you given by that specialist), EHRs could also worsen communication by drawing clinicians' focus away from patients during visits.
 Dr. Soroush Zaghi[/caption]
MedicalResearch.com Interview with:
Soroush Zaghi, MD
Department of Head and Neck Surgery
David Geffen School of Medicine at UCLA
University of California, Los Angeles
MedicalResearch: What is the central message for clinicians and surgeons from your results?
Dr. Zaghi: Multiple studies from different practitioners and institutions agree that Maxillomandibular Advancement (MMA) is a highly effective surgical option for patients with obstructive sleep apnea who cannot tolerate positive pressure therapy and have not found success with other surgical procedures.
Dr. Soroush Zaghi[/caption]
MedicalResearch.com Interview with:
Soroush Zaghi, MD
Department of Head and Neck Surgery
David Geffen School of Medicine at UCLA
University of California, Los Angeles
MedicalResearch: What is the central message for clinicians and surgeons from your results?
Dr. Zaghi: Multiple studies from different practitioners and institutions agree that Maxillomandibular Advancement (MMA) is a highly effective surgical option for patients with obstructive sleep apnea who cannot tolerate positive pressure therapy and have not found success with other surgical procedures.
 Dr. Ambarish Pandey[/caption]
Ambarish
MedicalResearch.com Interview with:
Ambarish Pandey M.D.
Division of Cardiology
University of Texas Southwestern Medical Center
Dallas, TX
Medical Research: What is the background for this study? What are the main findings?
Dr. Pandey: Pulmonary artery (PA) catheters have been used for invasive bedside hemodynamic monitoring for past four decades. The ESCAPE trial, published in October 2005, demonstrated that use of Pulmonary Artery catheter was not associated with a significant improvement in clinical outcomes of patients with heart failure. Accordingly, the current ACC/AHA guidelines discourage the routine use of PA catheter for routine management of acute heart failure in absence of cardiogenic shock or respiratory failure (Class III). Despite the significant evolution of available evidence base and guideline recommendations regarding use of Pulmonary Artery catheters, national patterns of PA catheter utilization in hospitalized heart failure patients remain unknown.
In this study, we observed that use of PA catheter among patients with heart failure decline significantly in the Pre-ESCAPE era (2001 – 2006) followed by a consistent increase in its use in the Post-ESCAPE era (2007-2012). We also observed that the increase in use of Pulmonary Artery catheters is most significant among heart failure patients without underlying cardiogenic shock or respiratory failure.
Dr. Ambarish Pandey[/caption]
Ambarish
MedicalResearch.com Interview with:
Ambarish Pandey M.D.
Division of Cardiology
University of Texas Southwestern Medical Center
Dallas, TX
Medical Research: What is the background for this study? What are the main findings?
Dr. Pandey: Pulmonary artery (PA) catheters have been used for invasive bedside hemodynamic monitoring for past four decades. The ESCAPE trial, published in October 2005, demonstrated that use of Pulmonary Artery catheter was not associated with a significant improvement in clinical outcomes of patients with heart failure. Accordingly, the current ACC/AHA guidelines discourage the routine use of PA catheter for routine management of acute heart failure in absence of cardiogenic shock or respiratory failure (Class III). Despite the significant evolution of available evidence base and guideline recommendations regarding use of Pulmonary Artery catheters, national patterns of PA catheter utilization in hospitalized heart failure patients remain unknown.
In this study, we observed that use of PA catheter among patients with heart failure decline significantly in the Pre-ESCAPE era (2001 – 2006) followed by a consistent increase in its use in the Post-ESCAPE era (2007-2012). We also observed that the increase in use of Pulmonary Artery catheters is most significant among heart failure patients without underlying cardiogenic shock or respiratory failure.
 Dr. David Katz[/caption]
MedicalResearch.com Interview with:
David L. Katz, MD, MPH, FACPM, FACP, FACLM
Director, Yale University Prevention Research Center
Griffin Hospital
President, American College of Lifestyle Medicine
Founder, True Health Initiative
Medical Research: What is the background for this study? What are the main findings?
Dr. Katz: the evidence that nuts in general, and walnuts in particular, have health promoting properties is vast and conclusive. In our own prior research, we have shown that daily ingestion of walnuts ameliorates overall cardiac risk in type 2 diabetics (
Dr. David Katz[/caption]
MedicalResearch.com Interview with:
David L. Katz, MD, MPH, FACPM, FACP, FACLM
Director, Yale University Prevention Research Center
Griffin Hospital
President, American College of Lifestyle Medicine
Founder, True Health Initiative
Medical Research: What is the background for this study? What are the main findings?
Dr. Katz: the evidence that nuts in general, and walnuts in particular, have health promoting properties is vast and conclusive. In our own prior research, we have shown that daily ingestion of walnuts ameliorates overall cardiac risk in type 2 diabetics ( Dr. McNaughton[/caption]
MedicalResearch.com Interview with:
Candace D. McNaughton, MD MPH FACEP
Assistant Professor
Emergency Medicine Research
Department of Emergency Medicine, Research Division
Vanderbilt University Medical Center
Medical Research: What is the background for this study? What are the main findings?
Dr. McNaughton: Hypertension, or high blood pressure, affects 1/3rd of adults in the United States and more than 1 billion people worldwide. It is also the #1 risk factor for cardiovascular disease such as heart attack and stroke, so it is very important to treat.
The burden of hypertension in the emergency department is not well understood. The ER is not usually thought of as a place where perhaps we could or should be addressing hypertension; that has traditionally be left up to primary care providers. Through this study, our goals were to gain a better understanding of how many ER visits were either related to hypertension or were solely because of hypertension, and to determine whether this changed from 2006 to 2012.
We found that
Dr. McNaughton[/caption]
MedicalResearch.com Interview with:
Candace D. McNaughton, MD MPH FACEP
Assistant Professor
Emergency Medicine Research
Department of Emergency Medicine, Research Division
Vanderbilt University Medical Center
Medical Research: What is the background for this study? What are the main findings?
Dr. McNaughton: Hypertension, or high blood pressure, affects 1/3rd of adults in the United States and more than 1 billion people worldwide. It is also the #1 risk factor for cardiovascular disease such as heart attack and stroke, so it is very important to treat.
The burden of hypertension in the emergency department is not well understood. The ER is not usually thought of as a place where perhaps we could or should be addressing hypertension; that has traditionally be left up to primary care providers. Through this study, our goals were to gain a better understanding of how many ER visits were either related to hypertension or were solely because of hypertension, and to determine whether this changed from 2006 to 2012.
We found that  Dr. Gunderson[/caption]
MedicalResearch.com Interview with:
Erica P. Gunderson, PhD, MPH, MS, RD
Senior Research Scientist, Division of Research, Cardiovascular and Metabolic Conditions Section
Kaiser Permanente Northern California
Oakland, CA 94612
Medical Research: What is the background for this study?
Dr. Gunderson: Gestational diabetes mellitus (GDM) is a disorder of glucose tolerance affecting 5-9 percent of all U.S. pregnancies (approximately 250,000 annually), with a 7-fold higher risk of progression to type 2 diabetes. Strategies during the postpartum period for prevention of diabetes focus on modification of lifestyle behaviors, including dietary intake and physical activity to promote weight loss.
Lactation is a modifiable postpartum behavior that improves glucose and lipid metabolism, and increases insulin sensitivity, with favorable metabolic effects that persist post-weaning. Despite these metabolic benefits, evidence that lactation prevents type 2 diabetes remains inconclusive, particularly among women with
Dr. Gunderson[/caption]
MedicalResearch.com Interview with:
Erica P. Gunderson, PhD, MPH, MS, RD
Senior Research Scientist, Division of Research, Cardiovascular and Metabolic Conditions Section
Kaiser Permanente Northern California
Oakland, CA 94612
Medical Research: What is the background for this study?
Dr. Gunderson: Gestational diabetes mellitus (GDM) is a disorder of glucose tolerance affecting 5-9 percent of all U.S. pregnancies (approximately 250,000 annually), with a 7-fold higher risk of progression to type 2 diabetes. Strategies during the postpartum period for prevention of diabetes focus on modification of lifestyle behaviors, including dietary intake and physical activity to promote weight loss.
Lactation is a modifiable postpartum behavior that improves glucose and lipid metabolism, and increases insulin sensitivity, with favorable metabolic effects that persist post-weaning. Despite these metabolic benefits, evidence that lactation prevents type 2 diabetes remains inconclusive, particularly among women with  Dr. Aaron White[/caption]
MedicalResearch.com Interview with:
Aaron White, PhD
Senior Scientific Advisor to the Director
Office of the Director
National Institute on Alcohol Abuse and Alcoholism
National Institutes of Health
Bethesda, MD
Medical Research: What is the background for this study? What are the main findings?
Dr. White: Recent studies and anecdotal evidence suggest that alcohol use by women in the United States might be on the rise and that long-standing gender gaps in drinking and related consequences might be narrowing. Using data from the National Survey on Drug Use and Health, we found that differences in the drinking patterns of females and males ages 12+ narrowed between 2002 and 2012 for current drinking (drinking at least once in the last 30 days), number of drinking days per month, past year DSM-IV alcohol abuse, and past-year driving under the influence of alcohol. For instance, the percentage of women who drank in the previous 30 days rose from 44% to 48%, while for men the percentage decreased from 57% to 56%. Average
Dr. Aaron White[/caption]
MedicalResearch.com Interview with:
Aaron White, PhD
Senior Scientific Advisor to the Director
Office of the Director
National Institute on Alcohol Abuse and Alcoholism
National Institutes of Health
Bethesda, MD
Medical Research: What is the background for this study? What are the main findings?
Dr. White: Recent studies and anecdotal evidence suggest that alcohol use by women in the United States might be on the rise and that long-standing gender gaps in drinking and related consequences might be narrowing. Using data from the National Survey on Drug Use and Health, we found that differences in the drinking patterns of females and males ages 12+ narrowed between 2002 and 2012 for current drinking (drinking at least once in the last 30 days), number of drinking days per month, past year DSM-IV alcohol abuse, and past-year driving under the influence of alcohol. For instance, the percentage of women who drank in the previous 30 days rose from 44% to 48%, while for men the percentage decreased from 57% to 56%. Average  Dr. Nesper[/caption]
MedicalResearch.com Interview with:
Arica Nesper, MD, MAS
Resident Physician
Stanford/Kaiser Emergency Medicine Residency
Stanford University Medical Center
Department of Emergency Medicine
Stanford
Medical Research: What is the background for this study? What are the main findings?
Dr. Nesper: Patients with severe mental illness are a distinct demographic in the emergency department. Unfortunately, resources to help these vulnerable patients are frequently the target of funding cuts. We aimed to describe the effect of these cuts on our emergency department and the care provided to our patients. In this study we evaluated data from before our county mental health facility cut its inpatient capacity by half and closed its outpatient unit, and compared this data with data collected after this closure. We found that the mean number of daily psychiatric consultations in our emergency department more than tripled and that the average length of stay for these patients increased by nearly eight hours. These two data combined demonstrate a five-fold increase in daily emergency department bed hours for psychiatric patients, placing a significant strain on the emergency department and demonstrating a delay in definitive care provided to these vulnerable patients.
Dr. Nesper[/caption]
MedicalResearch.com Interview with:
Arica Nesper, MD, MAS
Resident Physician
Stanford/Kaiser Emergency Medicine Residency
Stanford University Medical Center
Department of Emergency Medicine
Stanford
Medical Research: What is the background for this study? What are the main findings?
Dr. Nesper: Patients with severe mental illness are a distinct demographic in the emergency department. Unfortunately, resources to help these vulnerable patients are frequently the target of funding cuts. We aimed to describe the effect of these cuts on our emergency department and the care provided to our patients. In this study we evaluated data from before our county mental health facility cut its inpatient capacity by half and closed its outpatient unit, and compared this data with data collected after this closure. We found that the mean number of daily psychiatric consultations in our emergency department more than tripled and that the average length of stay for these patients increased by nearly eight hours. These two data combined demonstrate a five-fold increase in daily emergency department bed hours for psychiatric patients, placing a significant strain on the emergency department and demonstrating a delay in definitive care provided to these vulnerable patients.
 Dr. Jason Gold[/caption]
MedicalResearch.com Interview with:
Jason S. Gold MD FACS
Chief of Surgical Oncology, VA Boston Healthcare System
Assistant Professor of Surgery, Harvard Medical School
Brigham and Women’s Hospital
Medical Research: What is the background for this study?
Dr. Gold: Pancreas cancer is a lethal disease. While advances in the best available care for pancreas cancer are desperately needed, improvements can be made in addressing disparities in care. This study aimed to evaluate associations of social and demographic variables with the utilization of surgical resection as well as with survival after surgical resection for early-stage pancreas cancer.
Medical Research: What are the main findings?
Dr. Gold: The main findings are the following:
1: We found that less than half of patients with early-stage pancreas cancer undergo resection in the United States. Interestingly, the rate of resection has not changed with time during the eight-year study period.
2. We also found significant disparities associated with the utilization of surgical resection for early-stage pancreas cancer in the United States. African American patients, Hispanic patients, single patients, and uninsured patients were significantly less likely to have their tumors removed. There were regional variations in the utilization of surgical resection as well. Patients in the Southeast were significantly less likely to have a pancreas resection for cancer compared to patients in the Northeast.
3. Among the patients who underwent surgical resection for early-stage pancreas cancer, we did not see significant independent associations with survival for most of the social and demographic variables analyzed. Surprisingly, however, patients from the Southeast had worse long-term survival after pancreas cancer resection compared to those in other regions of the United States even after adjusting for other variables.
Dr. Jason Gold[/caption]
MedicalResearch.com Interview with:
Jason S. Gold MD FACS
Chief of Surgical Oncology, VA Boston Healthcare System
Assistant Professor of Surgery, Harvard Medical School
Brigham and Women’s Hospital
Medical Research: What is the background for this study?
Dr. Gold: Pancreas cancer is a lethal disease. While advances in the best available care for pancreas cancer are desperately needed, improvements can be made in addressing disparities in care. This study aimed to evaluate associations of social and demographic variables with the utilization of surgical resection as well as with survival after surgical resection for early-stage pancreas cancer.
Medical Research: What are the main findings?
Dr. Gold: The main findings are the following:
1: We found that less than half of patients with early-stage pancreas cancer undergo resection in the United States. Interestingly, the rate of resection has not changed with time during the eight-year study period.
2. We also found significant disparities associated with the utilization of surgical resection for early-stage pancreas cancer in the United States. African American patients, Hispanic patients, single patients, and uninsured patients were significantly less likely to have their tumors removed. There were regional variations in the utilization of surgical resection as well. Patients in the Southeast were significantly less likely to have a pancreas resection for cancer compared to patients in the Northeast.
3. Among the patients who underwent surgical resection for early-stage pancreas cancer, we did not see significant independent associations with survival for most of the social and demographic variables analyzed. Surprisingly, however, patients from the Southeast had worse long-term survival after pancreas cancer resection compared to those in other regions of the United States even after adjusting for other variables.
 Dr. Curry[/caption]
MedicalResearch.com Interview with:
Dr. Michael P. Curry, MD
Medical Director for Liver Transplantation
Harvard Medical Faculty Physicians
Beth Israel Deaconess Medical Center
Medical Research: What is the background for this study? What are the main findings
Dr. Curry: As the population that is infected with the hepatitis C virus (HCV) ages, the number of patients with decompensated cirrhosis is expected to increase. For many years, the only treatment option for these patients was liver transplantation. Recently, however, clinical trials of newly approved direct-acting antiviral agents (DAAs) have shown that it is possible to treat HCV infection safely and effectively in patients with decompensated cirrhosis. We conducted this Phase 3, open-label trial to assess the efficacy and safety of a fixed dose combination of sofosbuvir/velpatasvir with or without ribavirin for 12 weeks or sofosbuvir/velpatasvir for 24 weeks in patients infected with hepatitis C virus genotypes 1 through 6 and with decompensated cirrhosis. We found that treatment with sofosbuvir/velpatasvir resulted in high rates of sustained virologic response (SVR) and early improvements in hepatic function in this patient population. SVR rates were 83 percent in patients who received sofosbuvir/velpatasvir for 12 weeks, 94 percent among those who received sofosbuvir/velpatasvir plus ribavirin, and 86 percent among those who received sofosbuvir/velpatasvir for 24 weeks.
Dr. Curry[/caption]
MedicalResearch.com Interview with:
Dr. Michael P. Curry, MD
Medical Director for Liver Transplantation
Harvard Medical Faculty Physicians
Beth Israel Deaconess Medical Center
Medical Research: What is the background for this study? What are the main findings
Dr. Curry: As the population that is infected with the hepatitis C virus (HCV) ages, the number of patients with decompensated cirrhosis is expected to increase. For many years, the only treatment option for these patients was liver transplantation. Recently, however, clinical trials of newly approved direct-acting antiviral agents (DAAs) have shown that it is possible to treat HCV infection safely and effectively in patients with decompensated cirrhosis. We conducted this Phase 3, open-label trial to assess the efficacy and safety of a fixed dose combination of sofosbuvir/velpatasvir with or without ribavirin for 12 weeks or sofosbuvir/velpatasvir for 24 weeks in patients infected with hepatitis C virus genotypes 1 through 6 and with decompensated cirrhosis. We found that treatment with sofosbuvir/velpatasvir resulted in high rates of sustained virologic response (SVR) and early improvements in hepatic function in this patient population. SVR rates were 83 percent in patients who received sofosbuvir/velpatasvir for 12 weeks, 94 percent among those who received sofosbuvir/velpatasvir plus ribavirin, and 86 percent among those who received sofosbuvir/velpatasvir for 24 weeks.
 Dr. Cooper[/caption]
MedicalResearch.com Interview with:
Lauren Cooper, MD
Fellow in Cardiovascular Diseases
Duke University Medical Center
Duke Clinical Research Institute
Medical Research: What is the background for this study?
Dr. Cooper: The HF-ACTION study, published in 2009, showed that exercise training is associated with reduced risk of death or hospitalization, and is a safe and effective therapy for patients with heart failure and reduced ejection fraction. Subsequently, Medicare began to cover cardiac rehabilitation for patients with heart failure. However, many patients referred to an exercise training program are not fully adherent to the program. Our study looked at psychosocial reasons that may impact participation in an exercise program.
Medical Research: What are the main findings?
Dr. Cooper: We found that patients with higher levels of social support and fewer barriers to exercise exercised more than patients with lower levels of social support and more barriers to exercise. And patients who exercised less had a higher risk of cardiovascular death or heart failure hospitalization compared to patients who exercised more.
Dr. Cooper[/caption]
MedicalResearch.com Interview with:
Lauren Cooper, MD
Fellow in Cardiovascular Diseases
Duke University Medical Center
Duke Clinical Research Institute
Medical Research: What is the background for this study?
Dr. Cooper: The HF-ACTION study, published in 2009, showed that exercise training is associated with reduced risk of death or hospitalization, and is a safe and effective therapy for patients with heart failure and reduced ejection fraction. Subsequently, Medicare began to cover cardiac rehabilitation for patients with heart failure. However, many patients referred to an exercise training program are not fully adherent to the program. Our study looked at psychosocial reasons that may impact participation in an exercise program.
Medical Research: What are the main findings?
Dr. Cooper: We found that patients with higher levels of social support and fewer barriers to exercise exercised more than patients with lower levels of social support and more barriers to exercise. And patients who exercised less had a higher risk of cardiovascular death or heart failure hospitalization compared to patients who exercised more.
 Dr. Wang[/caption]
MedicalResearch.com Interview with:
Cunlin Wang, MD, PhD
Division of Epidemiology I,
Office of Surveillance and Epidemiology,
Center for Drug Evaluation and Research
US Food and Drug Administration
MedicalResearch: What is the background for this study? What are the main findings?
Dr. Wang: IV Iron has been known for its risk of anaphylactic reaction, but there has been little research on the comparative safety of individual IV Iron products from a large population-based study. This study included 688,183 new users of IV iron not on dialysis from the U.S. Medicare program over a ten-year span (January 2003 to December 2013). The main findings of the study are: the risk for anaphylaxis at first exposure was higher for iron dextran than non-dextran IV iron products combined (iron sucrose, gluconate and ferumoxytol). When individual IV Iron products were compared, the data suggested that iron dextran has the highest risk of anaphylaxis and Iron sucrose has the lowest risk, estimated both at the first time exposure and after cumulative exposures. The low and high molecular weight dextran products could not be individually identified during most of study period. However, from January 2006 through March 2008, during which the use of two dextran products could be distinguished, there was very low use of high molecular weight dextran (Dexferrum@). This suggested that the study results likely represent the risk of the low molecular weight dextran (Infed@).
Dr. Wang[/caption]
MedicalResearch.com Interview with:
Cunlin Wang, MD, PhD
Division of Epidemiology I,
Office of Surveillance and Epidemiology,
Center for Drug Evaluation and Research
US Food and Drug Administration
MedicalResearch: What is the background for this study? What are the main findings?
Dr. Wang: IV Iron has been known for its risk of anaphylactic reaction, but there has been little research on the comparative safety of individual IV Iron products from a large population-based study. This study included 688,183 new users of IV iron not on dialysis from the U.S. Medicare program over a ten-year span (January 2003 to December 2013). The main findings of the study are: the risk for anaphylaxis at first exposure was higher for iron dextran than non-dextran IV iron products combined (iron sucrose, gluconate and ferumoxytol). When individual IV Iron products were compared, the data suggested that iron dextran has the highest risk of anaphylaxis and Iron sucrose has the lowest risk, estimated both at the first time exposure and after cumulative exposures. The low and high molecular weight dextran products could not be individually identified during most of study period. However, from January 2006 through March 2008, during which the use of two dextran products could be distinguished, there was very low use of high molecular weight dextran (Dexferrum@). This suggested that the study results likely represent the risk of the low molecular weight dextran (Infed@).
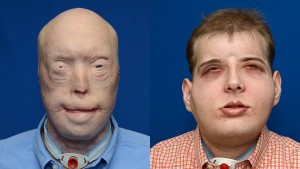 Patrick Hardison before surgery (left) and in November 2015, nearly three months after the surgery.[/caption]
Mr. Hardison was referred to
Patrick Hardison before surgery (left) and in November 2015, nearly three months after the surgery.[/caption]
Mr. Hardison was referred to  Dr. Givens
Dr. Givens
 Dr. Qin[/caption]
MedicalResearch.com Interview with:
Bo (Bonnie) Qin, PhD
Postdoctoral associate at Rutgers Cancer Institute of New Jersey
Medical Research: What is the background for this study? What are the main findings?
Response: Ovarian cancer is among the top five causes of cancer death among women in the US. Compared to white women, African-American women tend to have a worse 5-year survival rate of ovarian cancer. It highlights a critical need for identifying preventive factors in African Americans, particularly through dietary modification, which is relatively low cost and low risk compared to medical treatments.
We found that adherence to an overall healthy dietary pattern i.e. Alternate Healthy Eating Index (AHEI)-2010 may reduce ovarian cancer risk in African-American women, and particularly among postmenopausal women. Adherence to the current Dietary Guidelines for Americans i.e. Healthy Eating Index-2010, were also strongly associated with reduced risk of ovarian cancer among postmenopausal African-American women.
Dr. Qin[/caption]
MedicalResearch.com Interview with:
Bo (Bonnie) Qin, PhD
Postdoctoral associate at Rutgers Cancer Institute of New Jersey
Medical Research: What is the background for this study? What are the main findings?
Response: Ovarian cancer is among the top five causes of cancer death among women in the US. Compared to white women, African-American women tend to have a worse 5-year survival rate of ovarian cancer. It highlights a critical need for identifying preventive factors in African Americans, particularly through dietary modification, which is relatively low cost and low risk compared to medical treatments.
We found that adherence to an overall healthy dietary pattern i.e. Alternate Healthy Eating Index (AHEI)-2010 may reduce ovarian cancer risk in African-American women, and particularly among postmenopausal women. Adherence to the current Dietary Guidelines for Americans i.e. Healthy Eating Index-2010, were also strongly associated with reduced risk of ovarian cancer among postmenopausal African-American women.
 Dr. Del Gobbo[/caption]
MedicalResearch.com Interview with:
Liana Del Gobbo PhD
Friedman School of Nutrition Science and Policy, Tufts University, Boston, MA; and
Life Sciences Research Organization, Bethesda, MD
Medical Research: What is the background for this study? What are the main findings?
Dr. Del Gobbo: Accumulating evidence suggests that nut intake lowers risk of cardiovascular disease. But the specific mechanisms by which nuts may exert beneficial effects (eg. through lowering blood cholesterol, blood pressure, inflammation, etc.) were not clear. Two prior reviews on this topic only evaluated one type of nuts, and only a few cardiovascular risk factors.
To address these knowledge gaps, we performed a systematic review and meta-analysis of controlled trials to examine the effects of eating tree nuts (walnuts, pistachios, macadamia nuts, pecans, cashews, almonds, hazelnuts, Brazil nuts) on major cardiovascular risk factors including blood lipids (total cholesterol, LDL, HDL, triglycerides [TG]), lipoproteins (ApoA1, ApoB, ApoB100), blood pressure (systolic, SBP; diastolic, DBP), and inflammation (C-reactive protein, CRP) in adults 18 years or older without cardiovascular disease.
A daily serving of nuts (1oz serving, or 28g per day) significantly lowered total cholesterol, LDL, ApoB, and triglycerides, with no significant effects on other risk factors, such as HDL cholesterol, blood pressure or inflammation. To give you an idea of a 1oz serving size of nuts, it is about 23 almonds, 18 cashews, 21 hazelnuts, 6 Brazil nuts, 12 macadamia nuts, 14 walnut halves, 20 pecan halves, 49 pistachios.
We did not see any differences in cholesterol-lowering effects by nut type.
Dr. Del Gobbo[/caption]
MedicalResearch.com Interview with:
Liana Del Gobbo PhD
Friedman School of Nutrition Science and Policy, Tufts University, Boston, MA; and
Life Sciences Research Organization, Bethesda, MD
Medical Research: What is the background for this study? What are the main findings?
Dr. Del Gobbo: Accumulating evidence suggests that nut intake lowers risk of cardiovascular disease. But the specific mechanisms by which nuts may exert beneficial effects (eg. through lowering blood cholesterol, blood pressure, inflammation, etc.) were not clear. Two prior reviews on this topic only evaluated one type of nuts, and only a few cardiovascular risk factors.
To address these knowledge gaps, we performed a systematic review and meta-analysis of controlled trials to examine the effects of eating tree nuts (walnuts, pistachios, macadamia nuts, pecans, cashews, almonds, hazelnuts, Brazil nuts) on major cardiovascular risk factors including blood lipids (total cholesterol, LDL, HDL, triglycerides [TG]), lipoproteins (ApoA1, ApoB, ApoB100), blood pressure (systolic, SBP; diastolic, DBP), and inflammation (C-reactive protein, CRP) in adults 18 years or older without cardiovascular disease.
A daily serving of nuts (1oz serving, or 28g per day) significantly lowered total cholesterol, LDL, ApoB, and triglycerides, with no significant effects on other risk factors, such as HDL cholesterol, blood pressure or inflammation. To give you an idea of a 1oz serving size of nuts, it is about 23 almonds, 18 cashews, 21 hazelnuts, 6 Brazil nuts, 12 macadamia nuts, 14 walnut halves, 20 pecan halves, 49 pistachios.
We did not see any differences in cholesterol-lowering effects by nut type.
 Dr. Bastian[/caption]
MedicalResearch.com Interview with:
Boris C. Bastian, MD, PhD
Professor of Dermatology and Pathology
Gerson and Barbara Bass Bakar Distinguished Professor in Cancer Research
University of California, San Francisco
Medical Research: What is the background for this study? What are the main findings?
Dr. Bastian: The cost of DNA sequencing has dropped substantially since the initial sequencing of the human genome in 2001. As a result, the most common cancer subtypes have now been sequenced, revealing the pathogenic mutations that drive them. A typical cancer is driven by 5-10 mutations, but we still do not understand the order in which these mutations occur for most cancers.
Determining the order in which mutations occur is challenging for cancers that are detected at a late stage. Melanomas, however, lend themselves to this type of analysis because they are pigmented and found on the surface of the skin, allowing them to be identified early. Sometimes, melanomas are even found adjacent to their remnant precursor neoplasms, such as benign nevi (also known as common moles). We performed detailed genetic analyses of 37 cases of melanomas that were adjacent to their intact precursor neoplasms. We microdissected and sequenced the surrounding uninvolved normal tissue, the precursor neoplasm, and the descendent neoplasm. By comparing the genetic abnormalities in each of the microdissected areas, we were able to decipher the order of genetic alterations for each case.
Our work reveals the stereotypic pattern of mutations as they occur in melanoma. Mutations in the MAPK pathway, usually affecting BRAF or NRAS, occur earliest, followed by TERT promoter mutations, then CDKN2Aalterations, and finally TP53 and PTEN alterations. Benign nevi typically harbor a single pathogenic alteration, whereas fully evolved melanomas harbor three or more pathogenic alterations. We also identified an intermediate stage of neoplasia with some but not all of the pathogenic mutations required for fully evolved melanoma. There has been a longstanding debate whether morphologically intermediate lesions, such as dysplastic nevi, truly constitute biological intermediates or whether they simply represent a gray zone of histopathological assessment. Our data indicates that these neoplasms are genuine biological entities. Finally, we observe evidence of UV-radiation-induced DNA damage at all stages of pathogenesis, implicating UV radiation in both the initiation and progression of melanoma.
Dr. Bastian[/caption]
MedicalResearch.com Interview with:
Boris C. Bastian, MD, PhD
Professor of Dermatology and Pathology
Gerson and Barbara Bass Bakar Distinguished Professor in Cancer Research
University of California, San Francisco
Medical Research: What is the background for this study? What are the main findings?
Dr. Bastian: The cost of DNA sequencing has dropped substantially since the initial sequencing of the human genome in 2001. As a result, the most common cancer subtypes have now been sequenced, revealing the pathogenic mutations that drive them. A typical cancer is driven by 5-10 mutations, but we still do not understand the order in which these mutations occur for most cancers.
Determining the order in which mutations occur is challenging for cancers that are detected at a late stage. Melanomas, however, lend themselves to this type of analysis because they are pigmented and found on the surface of the skin, allowing them to be identified early. Sometimes, melanomas are even found adjacent to their remnant precursor neoplasms, such as benign nevi (also known as common moles). We performed detailed genetic analyses of 37 cases of melanomas that were adjacent to their intact precursor neoplasms. We microdissected and sequenced the surrounding uninvolved normal tissue, the precursor neoplasm, and the descendent neoplasm. By comparing the genetic abnormalities in each of the microdissected areas, we were able to decipher the order of genetic alterations for each case.
Our work reveals the stereotypic pattern of mutations as they occur in melanoma. Mutations in the MAPK pathway, usually affecting BRAF or NRAS, occur earliest, followed by TERT promoter mutations, then CDKN2Aalterations, and finally TP53 and PTEN alterations. Benign nevi typically harbor a single pathogenic alteration, whereas fully evolved melanomas harbor three or more pathogenic alterations. We also identified an intermediate stage of neoplasia with some but not all of the pathogenic mutations required for fully evolved melanoma. There has been a longstanding debate whether morphologically intermediate lesions, such as dysplastic nevi, truly constitute biological intermediates or whether they simply represent a gray zone of histopathological assessment. Our data indicates that these neoplasms are genuine biological entities. Finally, we observe evidence of UV-radiation-induced DNA damage at all stages of pathogenesis, implicating UV radiation in both the initiation and progression of melanoma.
 Dr. Lubitz[/caption]
MedicalResearch.com Interview with:
Carrie C. Lubitz, MD, MPH
Assistant Professor of Surgery, Harvard Medical School
Senior Scientist, Institute for Technology Assessment
Attending Surgeon, Mass General/North Shore Center for Outpatient Care
Danvers, Massachusetts
Medical Research: What is the background for this study? What are the main findings?
Dr. Lubitz: Given reported estimates of resistant hypertension and the proportion of resistant hypertensive patients with primary hyperaldosteronism (PA) - the most common form of secondary hypertension caused by a nodule or hyperplasia of the adrenal glands – we estimate over a million Americans have undiagnosed PA. Furthermore, it has been shown that patients with PA with the same blood pressure as comparable patients with primary hypertension have worse outcomes.
In our study, we found that identifying and appropriately treating patients with PA can improve long-term outcomes in patients in a large number of patients who have resistant hypertension.
Dr. Lubitz[/caption]
MedicalResearch.com Interview with:
Carrie C. Lubitz, MD, MPH
Assistant Professor of Surgery, Harvard Medical School
Senior Scientist, Institute for Technology Assessment
Attending Surgeon, Mass General/North Shore Center for Outpatient Care
Danvers, Massachusetts
Medical Research: What is the background for this study? What are the main findings?
Dr. Lubitz: Given reported estimates of resistant hypertension and the proportion of resistant hypertensive patients with primary hyperaldosteronism (PA) - the most common form of secondary hypertension caused by a nodule or hyperplasia of the adrenal glands – we estimate over a million Americans have undiagnosed PA. Furthermore, it has been shown that patients with PA with the same blood pressure as comparable patients with primary hypertension have worse outcomes.
In our study, we found that identifying and appropriately treating patients with PA can improve long-term outcomes in patients in a large number of patients who have resistant hypertension.
 Dr. Shah[/caption]
MedicalResearch.com Interview with:
Dr. Jatin J. Shah, MD
Associate Professor, Department of Lymphoma/Myeloma
Assistant Professor, Lymphoma/Myeloma
Division of Cancer Medicine
The University of Texas, MD Anderson Cancer Center
Houston, TX
Medical Research: What is the background for this study? What are the main findings?
Dr. Shah: The ubiquitin-proteasome system (UPS) is one of the key regulatory systems in our body’s cells. It controls the destruction of the majority of cellular proteins, which can be involved in making cells grow, expand, or die, among other functions. Defects in the UPS can result in a number of diseases, including cancer, for example by destroying too quickly the proteins that cause cells to die. The UPS has already been shown to be a rational target for cancer therapy: the approved drugs bortezomib and carfilzomib inhibit the proteasome itself, thus causing cancer cells to die. However, by completely blocking the proteasome, which is at the ‘end’ of the UPS, these drugs block the destruction of 100% of proteins, and can cause side effects. By contrast, blocking the NEDD8-activating enzyme (NAE) stops the cellular processes that are responsible for only approximately 20% of proteins being degraded by the UPS – including proteins of relevance to cancer development. Previous studies of pevonedistat in animals have shown that inhibiting NAE alters the ability of a cancer cell to repair its DNA after it is damaged; this leads to the death of cancer cells.
The man finding is this was the first reported study of pevonedistat in patients with multiple myeloma or lymphoma. It demonstrated that pevonedistat hits its target in cancer cells, exerted anticipated pharmacodynamic effects, and has modest activity as a single-agent in heavily pretreated patients with relapsed/refractory lymphoma.
Dr. Shah[/caption]
MedicalResearch.com Interview with:
Dr. Jatin J. Shah, MD
Associate Professor, Department of Lymphoma/Myeloma
Assistant Professor, Lymphoma/Myeloma
Division of Cancer Medicine
The University of Texas, MD Anderson Cancer Center
Houston, TX
Medical Research: What is the background for this study? What are the main findings?
Dr. Shah: The ubiquitin-proteasome system (UPS) is one of the key regulatory systems in our body’s cells. It controls the destruction of the majority of cellular proteins, which can be involved in making cells grow, expand, or die, among other functions. Defects in the UPS can result in a number of diseases, including cancer, for example by destroying too quickly the proteins that cause cells to die. The UPS has already been shown to be a rational target for cancer therapy: the approved drugs bortezomib and carfilzomib inhibit the proteasome itself, thus causing cancer cells to die. However, by completely blocking the proteasome, which is at the ‘end’ of the UPS, these drugs block the destruction of 100% of proteins, and can cause side effects. By contrast, blocking the NEDD8-activating enzyme (NAE) stops the cellular processes that are responsible for only approximately 20% of proteins being degraded by the UPS – including proteins of relevance to cancer development. Previous studies of pevonedistat in animals have shown that inhibiting NAE alters the ability of a cancer cell to repair its DNA after it is damaged; this leads to the death of cancer cells.
The man finding is this was the first reported study of pevonedistat in patients with multiple myeloma or lymphoma. It demonstrated that pevonedistat hits its target in cancer cells, exerted anticipated pharmacodynamic effects, and has modest activity as a single-agent in heavily pretreated patients with relapsed/refractory lymphoma.
 Dr. Vonberg[/caption]
MedicalResearch.com Interview with:
Frederick W. Vonberg, MA, MBBS
Research Fellow in Neurocritical Care
Boston Children's Hospital and Harvard Medical School
Medical Research: What is the background for this study? What are the main findings?
Response: An association between schizophrenia and epilepsy has long been suspected, ever since people noticed similarities in some aspects of the presentation of the two conditions, and in their epidemiology. For example, people with epilepsy are thought to be more at risk of developing schizophrenia. Furthermore, a psychosis resembling schizophrenia can characterize some forms of
Dr. Vonberg[/caption]
MedicalResearch.com Interview with:
Frederick W. Vonberg, MA, MBBS
Research Fellow in Neurocritical Care
Boston Children's Hospital and Harvard Medical School
Medical Research: What is the background for this study? What are the main findings?
Response: An association between schizophrenia and epilepsy has long been suspected, ever since people noticed similarities in some aspects of the presentation of the two conditions, and in their epidemiology. For example, people with epilepsy are thought to be more at risk of developing schizophrenia. Furthermore, a psychosis resembling schizophrenia can characterize some forms of  Dr. Lei Xu[/caption]
MedicalResearch.com Interview with:
Lei Xu, MD, PhD
Steele Laboratory of Tumor Biology
Radiation Oncology Department
Massachusetts General Hospital
Medical Research: What is the background for this study?
Dr. Lei Xu: Neurofibromatosis 2 is characterized by benign tumors that develop throughout the nervous system. The most common site of these tumors is the eighth cranial nerve, which carries hearing and balance information from the ears to the brain. Although these vestibular schwannomas grow slowly, they usually lead to a significant or total hearing loss by young adulthood or middle age. The tumors can also press on the brain stem, leading to headaches, difficulty swallowing and other serious neurologic symptoms. While the tumors can be surgically removed or destroyed with radiation treatment, both approaches can also damage hearing.
Several previous investigations had suggested that – unlike other benign tumors – vestibular schwannomas induce the formation of new blood vessels, as malignant tumors do. A 2009 New England Journal of Medicine study led by Scott Plotkin, MD, PhD, at Massachusetts General Hospital reported that treatment with the antiangiogenesis drug bevacizumab caused shrinkage of NF2-schwannomas in most of the treated patients and improved hearing in more than half. But the limitations of that approach – the fact that not all patients responded, that the hearing improvement was often transient and that some patients could not tolerate long-term bevacizumab treatment – indicated the need to better understand the mechanisms of anti-angiogenesis on the function of tumor-bearing nerves.
Dr. Lei Xu[/caption]
MedicalResearch.com Interview with:
Lei Xu, MD, PhD
Steele Laboratory of Tumor Biology
Radiation Oncology Department
Massachusetts General Hospital
Medical Research: What is the background for this study?
Dr. Lei Xu: Neurofibromatosis 2 is characterized by benign tumors that develop throughout the nervous system. The most common site of these tumors is the eighth cranial nerve, which carries hearing and balance information from the ears to the brain. Although these vestibular schwannomas grow slowly, they usually lead to a significant or total hearing loss by young adulthood or middle age. The tumors can also press on the brain stem, leading to headaches, difficulty swallowing and other serious neurologic symptoms. While the tumors can be surgically removed or destroyed with radiation treatment, both approaches can also damage hearing.
Several previous investigations had suggested that – unlike other benign tumors – vestibular schwannomas induce the formation of new blood vessels, as malignant tumors do. A 2009 New England Journal of Medicine study led by Scott Plotkin, MD, PhD, at Massachusetts General Hospital reported that treatment with the antiangiogenesis drug bevacizumab caused shrinkage of NF2-schwannomas in most of the treated patients and improved hearing in more than half. But the limitations of that approach – the fact that not all patients responded, that the hearing improvement was often transient and that some patients could not tolerate long-term bevacizumab treatment – indicated the need to better understand the mechanisms of anti-angiogenesis on the function of tumor-bearing nerves.
 MedicalResearch.com Interview with:
Dr. Wanpen Vongpatanasin MD
Program Director, Hypertension Fellowship Program
Professor of Internal Medicine
Director of the University of Texas Southwestern Hypertension Program
Medical Research: What is the background for this study? What are the main findings?
Dr. Vongpatanasin: Home blood pressure measurement may reveal very different number when compared to clinic blood pressure in hypertensive patients. This difference can manifest as white coat hypertension (White Coat Hypertension; elevated office blood pressure with normal ambulatory or home blood pressure), or masked hypertension (MH; elevated ambulatory or home BP with normal office blood pressure). Although numerous epidemiological studies from Europe and Asia have shown increased cardiovascular risks associated with White Coat Hypertension and masked hypertension, previous studies have not addressed cardiovascular outcomes associated with White Coat Hypertension and masked hypertension in the general population in the United States.
We found that participants in the Dallas Heart Study, a multiethnic populational-based study in the Dallas County, both White Coat Hypertension and MH are associated with increased aortic stiffness and markers of kidney damage when compared to the group with normal blood pressure both at home and in the clinic. Furthermore, both white coat hypertension and masked hypertension are associated with increased risk of cardiovascular events, including coronary heart disease, stroke, atrial fibrillation, heart failure, and cardiovascular death over a median follow-up period of 9 years.
MedicalResearch.com Interview with:
Dr. Wanpen Vongpatanasin MD
Program Director, Hypertension Fellowship Program
Professor of Internal Medicine
Director of the University of Texas Southwestern Hypertension Program
Medical Research: What is the background for this study? What are the main findings?
Dr. Vongpatanasin: Home blood pressure measurement may reveal very different number when compared to clinic blood pressure in hypertensive patients. This difference can manifest as white coat hypertension (White Coat Hypertension; elevated office blood pressure with normal ambulatory or home blood pressure), or masked hypertension (MH; elevated ambulatory or home BP with normal office blood pressure). Although numerous epidemiological studies from Europe and Asia have shown increased cardiovascular risks associated with White Coat Hypertension and masked hypertension, previous studies have not addressed cardiovascular outcomes associated with White Coat Hypertension and masked hypertension in the general population in the United States.
We found that participants in the Dallas Heart Study, a multiethnic populational-based study in the Dallas County, both White Coat Hypertension and MH are associated with increased aortic stiffness and markers of kidney damage when compared to the group with normal blood pressure both at home and in the clinic. Furthermore, both white coat hypertension and masked hypertension are associated with increased risk of cardiovascular events, including coronary heart disease, stroke, atrial fibrillation, heart failure, and cardiovascular death over a median follow-up period of 9 years.
 Dr. Nagler[/caption]
MedicalResearch.com Interview with:
Arielle Nagler MD
Instructor, Department of Ronald O. Perelman Department of Dermatology
NYU Langone Medical Center
Medical Research: What are some of the best ways to keep our skin healthy?
Dr. Nagler: Sun protection is the single, most important step you can take to keep your skin healthy. Sun protection can help to prevent many of the signs of aging including wrinkles, changes in skin texture, and uneven pigmentation. Also sun protection has been shown to prevent certain types of skin cancer, which may save you from the distress and scarring of treatment. While we should all be careful in the sun, sun protection doesn’t mean that you have to avoid all outdoor activities and deprive yourself of outdoor fun. If you have any issues with your skin, or want more information, you might want to look into someone like this
Dr. Nagler[/caption]
MedicalResearch.com Interview with:
Arielle Nagler MD
Instructor, Department of Ronald O. Perelman Department of Dermatology
NYU Langone Medical Center
Medical Research: What are some of the best ways to keep our skin healthy?
Dr. Nagler: Sun protection is the single, most important step you can take to keep your skin healthy. Sun protection can help to prevent many of the signs of aging including wrinkles, changes in skin texture, and uneven pigmentation. Also sun protection has been shown to prevent certain types of skin cancer, which may save you from the distress and scarring of treatment. While we should all be careful in the sun, sun protection doesn’t mean that you have to avoid all outdoor activities and deprive yourself of outdoor fun. If you have any issues with your skin, or want more information, you might want to look into someone like this