Author Interviews, Critical Care - Intensive Care - ICUs, Electronic Records, Infections, Mayo Clinic / 26.10.2015
Electronic Alerts Improved Sepsis Care and Outcomes
[caption id="attachment_18793" align="alignleft" width="125"] Dr. Franco[/caption]
MedicalResearch.com Interview with:
Dr. Pablo Moreno Franco MD
Assistant Professor of Medicine
MAYO Clinic
Medical Research: What is the background for this study? What are the main findings?
Dr. Pablo Franco: Early alerts and prompt management of patient with severe sepsis and septic shock (SS/S) starting in the emergency department (ED) have been shown to improve mortality and other pertinent outcomes. With this in mind, we formed a multidisciplinary sepsis and shock response team (SSRT) in September 2013. Automated electronic sniffer alerted ED providers for possible sepsis and when S/SS was identified, they were encouraged to activate SSRT.
Dr. Franco[/caption]
MedicalResearch.com Interview with:
Dr. Pablo Moreno Franco MD
Assistant Professor of Medicine
MAYO Clinic
Medical Research: What is the background for this study? What are the main findings?
Dr. Pablo Franco: Early alerts and prompt management of patient with severe sepsis and septic shock (SS/S) starting in the emergency department (ED) have been shown to improve mortality and other pertinent outcomes. With this in mind, we formed a multidisciplinary sepsis and shock response team (SSRT) in September 2013. Automated electronic sniffer alerted ED providers for possible sepsis and when S/SS was identified, they were encouraged to activate SSRT.
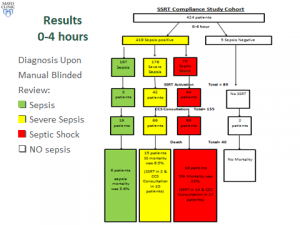 Two blinded reviewers retrospectively abstracted data on clinical trajectory and outcomes of all patients with sepsis and SS/S admitted at a single academic medical center between September 2013 and September 2014. Given importance of timely recognition and interventions in S/SS, we specifically focused on 2 periods: 0-4 hours and 4-12 hours after hospital admission. Additionally, we compared the compliance to “standard of care” between the SSRT pre-implementation period and the study period.
There were 167 patients admitted with sepsis, among which there were 3 SSRT activations and sepsis mortality was 3.6%. There were 176 patients with SS, SSRT was called in 42 (23%) and SS mortality was 8.5%. CCS was involved in 66 patients and mortality was 6.9% if SSRT was activated, versus 21.6% if SSRT was not activated. There were 76 patients with septic shock, SSRT was called in 44 (57%) and septic shock mortality was 25%. Critical Care Service (CCS) was involved in 68 patients and mortality rates with and without SSRT were 30.9% and 15.4%, respectively. The all-or-none compliance with applicable goals of resuscitation improved from the baseline 0% to over 50% at the study period end. Overall observed/expected sepsis mortality index improved from 1.38 pre-SSRT to 0.68 post-SSRT implementation.
Two blinded reviewers retrospectively abstracted data on clinical trajectory and outcomes of all patients with sepsis and SS/S admitted at a single academic medical center between September 2013 and September 2014. Given importance of timely recognition and interventions in S/SS, we specifically focused on 2 periods: 0-4 hours and 4-12 hours after hospital admission. Additionally, we compared the compliance to “standard of care” between the SSRT pre-implementation period and the study period.
There were 167 patients admitted with sepsis, among which there were 3 SSRT activations and sepsis mortality was 3.6%. There were 176 patients with SS, SSRT was called in 42 (23%) and SS mortality was 8.5%. CCS was involved in 66 patients and mortality was 6.9% if SSRT was activated, versus 21.6% if SSRT was not activated. There were 76 patients with septic shock, SSRT was called in 44 (57%) and septic shock mortality was 25%. Critical Care Service (CCS) was involved in 68 patients and mortality rates with and without SSRT were 30.9% and 15.4%, respectively. The all-or-none compliance with applicable goals of resuscitation improved from the baseline 0% to over 50% at the study period end. Overall observed/expected sepsis mortality index improved from 1.38 pre-SSRT to 0.68 post-SSRT implementation.
 Dr. Franco[/caption]
MedicalResearch.com Interview with:
Dr. Pablo Moreno Franco MD
Assistant Professor of Medicine
MAYO Clinic
Medical Research: What is the background for this study? What are the main findings?
Dr. Pablo Franco: Early alerts and prompt management of patient with severe sepsis and septic shock (SS/S) starting in the emergency department (ED) have been shown to improve mortality and other pertinent outcomes. With this in mind, we formed a multidisciplinary sepsis and shock response team (SSRT) in September 2013. Automated electronic sniffer alerted ED providers for possible sepsis and when S/SS was identified, they were encouraged to activate SSRT.
Dr. Franco[/caption]
MedicalResearch.com Interview with:
Dr. Pablo Moreno Franco MD
Assistant Professor of Medicine
MAYO Clinic
Medical Research: What is the background for this study? What are the main findings?
Dr. Pablo Franco: Early alerts and prompt management of patient with severe sepsis and septic shock (SS/S) starting in the emergency department (ED) have been shown to improve mortality and other pertinent outcomes. With this in mind, we formed a multidisciplinary sepsis and shock response team (SSRT) in September 2013. Automated electronic sniffer alerted ED providers for possible sepsis and when S/SS was identified, they were encouraged to activate SSRT.
 Two blinded reviewers retrospectively abstracted data on clinical trajectory and outcomes of all patients with sepsis and SS/S admitted at a single academic medical center between September 2013 and September 2014. Given importance of timely recognition and interventions in S/SS, we specifically focused on 2 periods: 0-4 hours and 4-12 hours after hospital admission. Additionally, we compared the compliance to “standard of care” between the SSRT pre-implementation period and the study period.
There were 167 patients admitted with sepsis, among which there were 3 SSRT activations and sepsis mortality was 3.6%. There were 176 patients with SS, SSRT was called in 42 (23%) and SS mortality was 8.5%. CCS was involved in 66 patients and mortality was 6.9% if SSRT was activated, versus 21.6% if SSRT was not activated. There were 76 patients with septic shock, SSRT was called in 44 (57%) and septic shock mortality was 25%. Critical Care Service (CCS) was involved in 68 patients and mortality rates with and without SSRT were 30.9% and 15.4%, respectively. The all-or-none compliance with applicable goals of resuscitation improved from the baseline 0% to over 50% at the study period end. Overall observed/expected sepsis mortality index improved from 1.38 pre-SSRT to 0.68 post-SSRT implementation.
Two blinded reviewers retrospectively abstracted data on clinical trajectory and outcomes of all patients with sepsis and SS/S admitted at a single academic medical center between September 2013 and September 2014. Given importance of timely recognition and interventions in S/SS, we specifically focused on 2 periods: 0-4 hours and 4-12 hours after hospital admission. Additionally, we compared the compliance to “standard of care” between the SSRT pre-implementation period and the study period.
There were 167 patients admitted with sepsis, among which there were 3 SSRT activations and sepsis mortality was 3.6%. There were 176 patients with SS, SSRT was called in 42 (23%) and SS mortality was 8.5%. CCS was involved in 66 patients and mortality was 6.9% if SSRT was activated, versus 21.6% if SSRT was not activated. There were 76 patients with septic shock, SSRT was called in 44 (57%) and septic shock mortality was 25%. Critical Care Service (CCS) was involved in 68 patients and mortality rates with and without SSRT were 30.9% and 15.4%, respectively. The all-or-none compliance with applicable goals of resuscitation improved from the baseline 0% to over 50% at the study period end. Overall observed/expected sepsis mortality index improved from 1.38 pre-SSRT to 0.68 post-SSRT implementation.

























